Introduction
Brain neoplasms are sometimes seen in cases referred to the medical examiner, and they generally fall into the following circumstances: sudden unexpected death, diagnostic failure (oversight), therapeutic misadventure, failure to recognize postoperative complications, and patient’s refusal of therapy, among other unusual special situations. Some tumors are incidental findings, for example, small meningiomas, lipomas, and subependymomas.
Clinical presentation of brain tumor
The presenting symptoms of a primary brain tumor are typically classified as generalized or focal. Headache is more prevalent in patients with faster growing, high grade tumors. Seizures are a more common presenting feature in lower grade tumors. Focal neurologic deficits such as weakness, language dysfunction, or sensory loss are seen with low-grade tumors, a consequence of their slower rate of growth. Acute events such as hemorrhage markedly alter the tempo of symptom onset regardless of tumor grade, summarizes common clinical presentations of the more common CNS tumors.
Because brain parenchyma is anesthetic, headaches associated with brain tumors may be due to increased intracranial pressure or to local pressure on sensitive intracranial structures (mainly dura and vessels). Characteristically headaches associated with increased intracranial pressure occur in the morning. Associated findings may include focal neurologic deficits, motor deficits behavior changes, and papilledema. Cushing’s triad is classically associated with increased intracranial pressure, but the full triad (hypertension, bradycardia, respiratory irregularity) is seen in only one third of the cases of increased intracranial pressure. Long standing increases in intracranial pressure may lead to optic atrophy and blindness because of transmission of the pressure to the optic nerves.
Seizures are common in patients with brain tumors, especially those with low grade neoplasms. Seizure foci most likely originate from the brain adjacent to tumor nidus. Seizures may be partial (simple, complex, or secondarily generalized) or generalized (tonic clonic, absence).
CSF dissemination of tumor cells should be suspected in patients with neurologic deficits that cannot be attributed to the primary tumor. Lumbar back pain or bowel or bladder dysfunction, for example, may suggest CSF metastasis in the lumbar eastern with involvement of the cauda equina.
What causes a brain tumor?
Because there are so many different types of brain tumors, each originating from the different types of cells within the brain, spinal cord, or meninges, it is impossible to determine a cause for most brain tumors. There are, however, known risk factors for the development of some types of tumors.
Cigarette smoking has not been clearly associated with an increased risk for the development of primary brain tumors, but smoking is an important cause of metastatic brain tumors, particularly those that originate from lung cancer. Of the 213,000 lung cancer patients diagnosed each year in the United States, about one third—more than, 70,000 people! — will develop one or more tumors in the brain.
Some primary brain tumors affect men more commonly than women and vice versa, but the reasons for these differences are not known. Some studies suggest that workers in certain occupations have a highest incidence of brain tumors. It has been known for several years that workers in the petrochemical industry have a higher incidence of brain tumors, and exposure to vinyl chloride has been recognized as CNS carcinogen; however, for many of the occupations reported to have an increased risk of CNS tumors, such as business managers and messengers, no known environmental exposure has been identified.
Patients who have previously had radiation therapy to the brain, skull, or scalp are at risk for developing brain tumors many years later. This is particularly important because of the risk of developing a second tumor after successful treatment for a brain tumor in childhood. There is no known intervention that can reduce the risk of developing a radiation-related tumor. Several studies have investigated other sources of radiation, such as electromagnetic fields, power lines, and cell phones; however, studies have not yet proven that these sources cause brain tumors.
Head injury, hair dye, and drug use have also been studied, but it has not been shown conclusively that these factors cause primary brain tumors. Food additives and preservatives and chemicals in drinking water have been studied in a number of countries. For example, eating preserved, smoked, or pickled meat and fish appears to correlate with an increased risk of brain tumors. In addition, two studies have shown that the risk of brain tumor decrease when individuals eat more fruits and vegetables; however, other studies of dietary influence on the development of brain tumors have been inconclusive.
In summary, although many factors have been studied for a possible link to the development of primary brain tumors, few are considered definite risk factors.
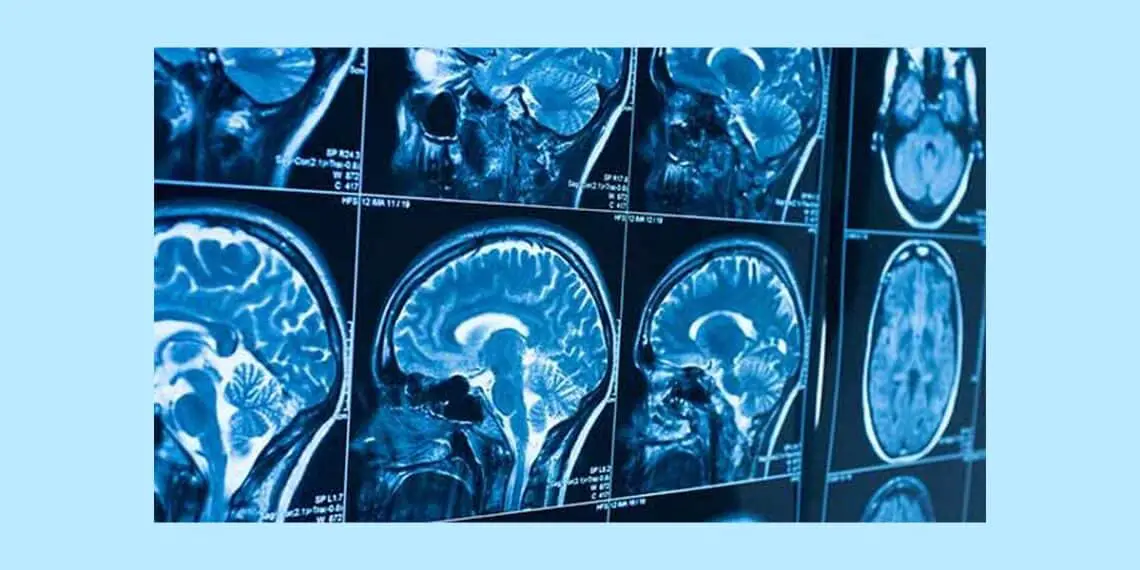
Diagnosis of brain tumor
In order to locate the tumor and determine its extent, physicians use ANGIOGRAPHY together with various types of BRAIN SCANS: CAT SCAN, MAGNETIC RESONANCE IMAGING (MRI), AND X-ray studies.
Treatment options and outlook
Treatment of a brain tumor often depends on its classification and characteristics. For example, a medulloblastoma is usually treated with the radiation of both the brain and spinal cord because this type of tumor has a tendency to spread throughout the entire central nervous system.
Tumors are often surgically removed when possible, but too often malignant tumors are inaccessible or too extensive to be removed. In this case, survival rates are not high; less than 20% of these patients survive one year.
When a tumor cannot be totally removed, as much of the growth as possible will be cut out to relieve pressure on the brain, followed by chemotherapy or radiation therapy. Corticosteroid drugs can be used to reduce tissue swelling around the tumor.
Radiation is the second most common treatment for brain tumors after surgery, usually administered soon after surgery. The cells of many malignant brain tumors are readily killed by radiation, which is why type of treatment is almost always recommended. (One possible exception is the treatment of very young children, whose developing brains may be injured by the radiation). Most tumors do shrink from the effects of radiation, although it may take some time for swelling and dead cells to diminish so that the true size of the growth can be seen.
Another radiation technique called STEREOTACTIC RADIOSURGERY, or gamma knife, is used for patients with inoperable brain tumors. In this technique, the surgeon uses a small directed beam of radiation to treat areas that may be inaccessible by conventional surgery or for patients who may not be able to withstand an operation. The one time application is an outpatient procedure that may serve as a substitute for the 20 to 30 radiation treatments normally required.
The key is to locate the diseased tissue and program those coordinates into a linear accelerator—the unit that emits the radiation beam. The accelerator is rotated around the target area in the patient’s brain, allowing high doses of radiation to be given directly to the designated site. The procedure usually takes an entire day and is performed with a local anesthetic. A CAT scan is used to determine the exact coordinates of the diseased tissue; with that information, doctors then affix a metal ring to the head, which helps the linear accelerator focus on the target area.
At present, this type of radiation is being used for patients with various types of brain tumors, as well as brain tumors that have not responded to conventional radiation therapy. It can also be used to treat malformed blood vessels in the brain that can cause seizures and are usually inoperable under normal situations.
Chemotherapy may be used in the treatment of brain tumors, which work by interfering with various parts of the cell’s cycle. Immunotherapy is also used with brain tumors. However, most chemotherapy does not easily cross the blood-brain barrier.
Homeopathic treatment of brain tumor – Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat brain tumor but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to cure brain tumor symptoms that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. There are following remedies which are helpful in the treatment of brain tumor symptoms:
Plumbum Met, Kali Brom, Thuja, Calcaria Carb, Argentum Nitricum, Cicuta Virosa, Belladonna, and many other medicines.
Reference:
Virginia Stark- Vance, Mary Louise DuBay-100 Question & Answer about Brain Tumors 2009; 12
Edward C. Halperin, Carlos A. Perez, Luther W. Brady- Perez and brady’s principles and practice of radiation oncology; 2008; 720
Carol Turkington, Joseph Harris- The encyclopedia of the brain and brain disorders; 2009; 77-78
Brain Tumor Cases Cured with Homeopathic Medicine
How to Heal Patients with Benign and Malignant Tumors – by Seyedaghanoor Sadeghi
Mesial Temporal Sclerosis – Symptoms Reversed with Homoeopathy – by Aparna Singh
My Experience in a Case Of Brain Tumor – by A. U. Ramakrishnan
A Case of Erbium oxydatum – by Pavol Tibensky
A Case of Brain Tumour in a 23 Years Young Married Woman – by S.K.Banerjea




My one patient having suffering left temporal pariteck tumor and operated on 2005 but than developed second time and every half hourly convulsion came on face, so please suggest which medicine would help this case
you need to give more detail of your clients symptoms before a remedy can be suggested, best to see a homeopath in person but can give some recommendations if you give more details.
Has anyone treated a glomus jugulare tumour? How do i choose between plum iod, plum met or bar c?
Hello, Did you find any treatment?
Can you please provide me a mail id, so that i can send detailed description of my query along with reports.
Please post about the Dr Bannerji’s Medicine Ruta 6 and Cal Phos 3x information in the above article.
My mother is using this medicaition from Dr Bannjeri and we are hopeful she wil be fine
dear sir what about your mother with banerji protocol plz be must reply my younger brother have GBM brain tomur
Many are using & getting results
What about your mother’s case?
My sister aged 52 has been diagnosed with Acoustic neuroma as she started suffering from hearing loss in one ear. The doctor said it is a benign slow growing tumor but has now grown into a size that is affecting her hearing. Also the doctor is concerned as a part of it may be growing towards the brain. Options are radiotherapy and/or surgery both may result in complications.
we are very fearful of the consequences of surgery so want to avoid it as much as possible. Can homeopathy help? What input is required to get help from here.
Thanks,
NJ