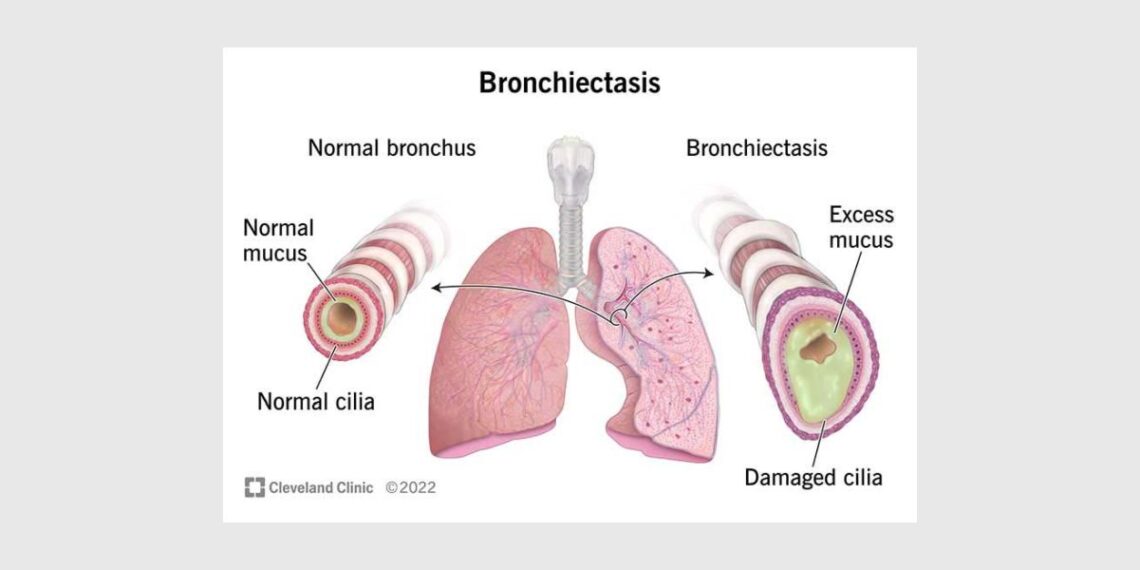
Bronchiectasis is destruction and widening of the large airways that causes the flabby and scarred lungs.
| Pathological types
|
Clinical types |
|
Dry Bronchiectasis that presents with hemoptysis but not sputum production. |
Causes of Bronchiectasis
Causes of bronchiectasis mainly include:
Focal airway obstruction
Intrinsic airway narrowing
- Tumor
- Foreign body
- Broncholith
Extrinsic airway narrowing
- Enlarged lymph nodes
- Post-surgical distortion of bronchial anatomy
Idiopathic
Post-infectious conditions
Bacteria
- Pseudomonas aeruginosa
- Haemophilus influenza
- Staphylococcus aureus
- Streptococcus pneumoniae
- Mycobacterium tuberculosis (MTB)
- Mycobacterium avaim complex (MAC) and other non-tuberculosis
- Mycobacterium species
- Bordetella pertussis (whooping cough)
Viruses
- Measles
- Adenovirus
- Influenza virus
Fungi
- Histoplasma capsulatum
- Pneumocystis carinii
Chronic obstructive pulmonary diseases (COPD)
Inhalational injury
Aspiration
Toxic gases
- Ammonia
- Chlorine
Inherited molecular and cellular defects
- Cystic fibrosis (Homeopathy for Cystic Fibrosis)
- Alpha-1 antitrypsin deficiency
Immune disorders
- Allergic bronchopulmonary aspergillosis
- Rheumatoid arthritis
- Sjogren’s syndrome
- Inflammatory bowel disease
- Polychondritis
- Lung allograft rejection
- Graft versus disease in post bone marrow transplant
Immuno-deficiencies
- HIV infection
- X-linked agammaglobulinemia
- Selective IgG deficiency
- Selective IgA, IgM or IgE deficiency
- Common variable immunodeficiency
- Chronic granulomatous disease of childhood
Primary Ciliary Dyskinesia
- Kartagener’s syndrome
Inherited bronchial structural abnormalities
- Bronchopulmonary sequestration
- Bronchial atresia
- Tracheobronchomegaly
- Congenital cartilage deficiency (Williams-Campbell syndrome)
Other
- Yellow nail syndrome
- Young’s syndrome
Traction Bronchiectasis
- Interstitial pneumonitis
- Chronic granulomatous disease infection induced fibrosis (I.E. tuberculosis)
Clinical Features
Bronchiectasis is associated with a number of abnormalities that profoundly affect respiratory function, including atelectasis, obstruction of the smaller airways, and diffuse bronchitis. Affected persons have recurrent bronchopulmonary infection; coughing; producing of copious amounts of foul-smelling, purulent sputum; and hemoptysis. Weight loss and anemia are common.
Manifestation:
The manifestations of Bronchiectasis are similar to those seen in chronic bronchitis and emphysema. As in the latter two conditions, chronic bronchial obstruction leads to marked dyspnea and cyanosis. Clubbing of the fingers, which is not usually seen in other types of obstructive lung disease, is more common in moderate to advanced Bronchiectasis.
Treatment of Bronchiectasis
Antibiotics
Where modern medicine is concerned, antibiotics may be helpful in the management of Bronchiectasis. Treatment is usually started when there is an exacerbation that produces shortness of breath, blood-spitting, fever, or increased cough and sputum production. Some patients may benefit from continuous or regular administrations of antibiotics but run the risk developing drug resistance.
Chest Physiotherapy
Chest physiotherapy is a time honored procedure that utilizes gravity to promote drainage of thick mucus from the damaged bronchial tubes. This simple technique reduces the opportunity for bacteria to cause recurrent infection.
Treat the Underlying condition
When Bronchiectasis results from another condition, such as sinusitis, it is essential to correct the contributing disorder.
Sinusitis is often associated with Bronchiectasis. Antibiotics may be necessary here as well to eradicate infection that drains into the airways. Sinus drainage may be facilitated by the use of anti-inflammatory sprays that shrink swollen mucous membranes.
Gastroesophegeal reflux can be treated by elevating the head of one’s bed and by not eating for two hours before bedtime. Alcohol and caffeine should also be avoided. What is the role of surgery in the treatment of Bronchiectasis?
In patients with Bronchiectasis localized to one portion of the lung, surgery is another treatment option. Before considering surgery, a chest CAT scan must be done to determine if multiple areas of lung are damaged. If only one segment of lung is found to be involved, pulmonary function test are performed to determine if there is adequate reserve to permit removal of the lung. It is also important to evaluate the patient’s general health and nutritional status prior to considering surgery.
Diagnostic testing
Chest radiograph can be normal in 7 to 20% of patients with established Bronchiectasis. Radiographic abnormalities are rarely distinctive or diagnostic. The diagnosis is supported by increased or crowded lung markings, tubular or ring shadows (produced by thickened dilated bronchial walls), gloved finger shadows, and, especially cystic air-containing areas with or without fluid levels.
High resolution CT has become the most reliable modality in the evaluation and non-invasive diagnosis of Bronchiectasis. An airway diameter of more than 1.5 times the adjacent blood vessel is indicative of cylindrical Bronchiectasis. Other anatomic forms are even easier to diagnose on CT.
The diagnostic approach to a patient where Bronchiectasis is strongly suggested on the basis of chronic cough, sputum, recurrent focal infection, or hemoptysis includes chest x-ray study, sputum smear and culture, pulmonary function testing (which should show a picture of airflow limitation), immunologic evaluation, especially quantitation or IgG and its subclasses, IgA and IgM, sweat chloride test, chest CT and possibly, bronchography. A presumptive diagnosis can usually be made on the basis of the clinical history, examination, and the aforementioned tests, although chronic bronchitis may be indistinguishable on purely clinical grounds.
Complications of Bronchiectasis are as follows:
Hemoptysis amyloidosis
Pneumonia brain abscess
Lung abscess aspergilloma
Empyema cor-pulmonale
Septicemia respiratory failure
Osteomyelitis hypoproteinuria
Homeopathic treatment of bronchiectasis – Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat bronchiectasis but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to treat bronchiectasis that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. There are following remedies which are helpful in the treatment of bronchiectasis:
Spongia, Sulphur, Arsenic Iod, Kali Iod, Stannum Met, Ipecac, Antim Tart, Dulcamara, Ammonium Carb, Kali Bi, Hepar Sulph, Carbo Veg, Nitric acid, Silicea and many other medicines.
References:
Exam Zone- Zone Comprehensive Guide to Pgmee, Volume 3; 58
Phillip M. Boiselle, David A. Lynch- CT of the airways; 2008; 218
Carol Mattson Porth, Glenn Matfin-Essential of Pathophysiology: Concepts of Altered Health States; 2010; 584
Richard A. Bordow, Andrew L. Ries, Timothy A. Morris- Manual of clinical problems in pulmonary medicine; 2005; 309
Francis V. Adams- The breathing Disorders Sourcebook; 1998; 111



dear alls,
i have restrictive lungs problems, i am also using damiana 30 for batter sex result. is any relations/side effects for using this medicion when i am using elophatic medicine ? pls gide me.
b. regards,
yousuf
Bronchiectasis with collapse right upper lobe.
Have bronchiectasis for years. Am holistic. Last summer was on cipro 500mg 2xday for 3 weeks and another round of same for another 3weeks for pseudamonas infection of r lobe mid sternum. Have had lingulaectomy, 28 years ago. Doing well however, sputum hadn’t changed much from the summer and was taking sulphur 30x for almost a month to see if that would change from very light green to white or clear., after taking it for 3 weeks about 3xaday was taking it diluted 1 tablet in small amount of water, taking 1 to 2 tbs per day and then 1 per day..Yesterday noticed rusty sputum, had not seen rusty sputum at all last summer while on the Cipro. Have seen rusty sputum many times off and on througout the years. Just want to know what my next step should be. There is no fever, only the inflamed feeling. It seems is as if the sulphur has taken the inner portion off of the infected area and now needs to have something to heal that. Appreciate your help.
Carol