WHAT IS HEART ATTACK
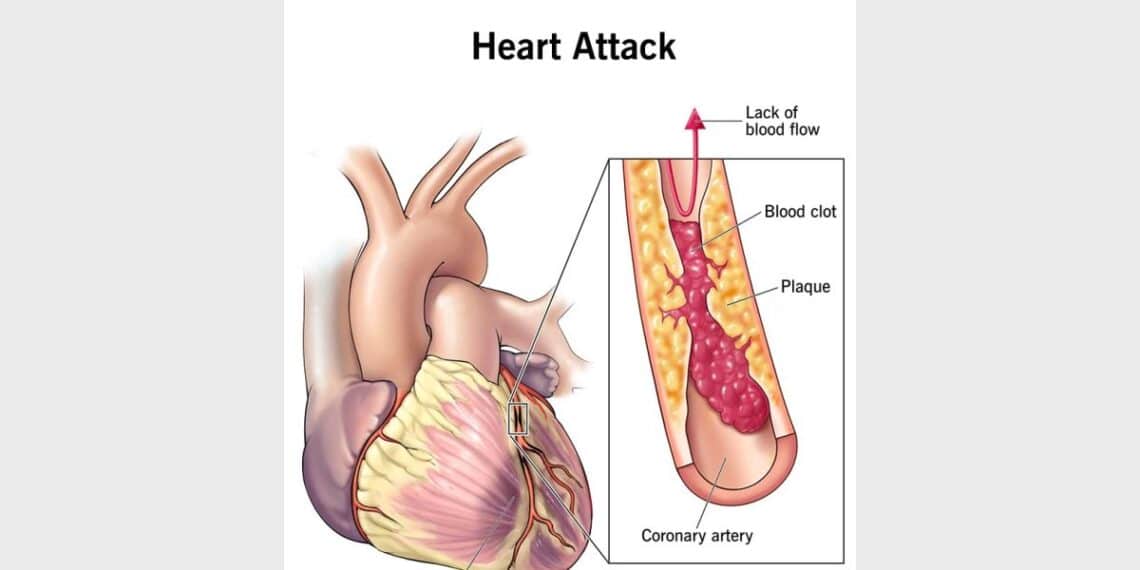
Heart attack or myocardial infarction (medically called MI or Coronary Thrombosis) is the consequence of complete obstruction of blood supply to a part of the heart muscles. This occurs due to 100% blockage in any of the coronary arteries or their branches. The heart muscles are completely deprived of their blood and oxygen supply which leads to its death.
WHAT IS THE CAUSE OF HEART ATTACK?
Almost all heart attacks are sudden in onset and the cause is rupture of growing blockages. The blockages are usually covered by a thin membrane called intimal membrane, which also keeps the deposits intact. This elastic membrane gets more and more stretched as more and more fatty deposits occur. But if the fatty deposits continue below this permeable membrane, one day a time will come when the membrane cannot stretch further and breaks off. This leads to the formation of a clot or thrombus inside the tube, closing the lumen completely. This completes the process of heart attack. The area of the myocardium (heart muscles) which gets the blood through the closed artery, dies – in the event of no blood supply.
Heart attack often occurs after a heavy meal full of fat, after sudden anger or excessive sorrow or grief or excessive stress. Heart attacks occur more frequently in the early mornings. Heart attacks also occur during the process of angiography and Angioplasty when the catheter or balloon is inflated and completely blocks the lumen of the coronary artery or breaks off the blockage by mechanical means.
Diagnosis of Heart Attack
Heart attacks do not respect time, place or circumstances. These can happen to anyone, anytime, and apparently out of the blue, perhaps even depriving the unsuspecting victim of life.
Pain
The first symptom of heart attack, in a majority of the cases, is a severe and prolonged pain in the middle of the front of the chest. In some, the pain may be severe enough to be described as the worst pain the patient has ever experienced. The pain is often accompanied by weakness, sweating, nausea, vomiting, giddiness and anxiety.
Shock
While pain is the most prominent symptom in most of the cases of heart attack, there are cases in which this is not so. The first and the most prominent symptom may be a state of shock in which the patient at once passes.
He suddenly experiences weakness which slowly or rapidly may develop into intense prostration or collapse. He may unexpectedly slump if he is standing or walking. He may lose consciousness because of less blood going to the brain.
Pulmonary Oedema
A sudden onset of pulmonary oedema a may be the first and is often the dominant manifestation of heart attack. Pulmonary oedema is the sudden out pouring of blood serum into the lung alveoli from the lung capillaries whose walls become more permeable because of lack of oxygen. The attack may appear suddenly and without warning, causing oppression in the chest and intense suffocating breathlessness.
Pain or numbness in the jaw often occurs as part of radiating chest pain, but may occur alone. It usually occurs in the lower jaw, on either or both sides. Toothaches may indeed be a dental problem, but if the aching tooth is a healthy one, the pain may be symptom of heart attack.
Atypical Symptoms
A patient may complain of a strange sense of mid-sternal uneasiness associated with apprehension, and a fast pulse. If he has had a heart attack before and develops such a sensation at some later time, he must get himself examined by his doctor. Similarly, those with a family history of heart attack and those with high level of cholesterol in the blood, must get themselves examined in such a situation.
Chest Examination
Examination with the help of a stethoscope may reveal some extra sounds coming from inside the chest. These sounds — moist rales— are due to collection of phlegm at the bases of the lungs.
Pulse
The examination of the pulse may reveal no abnormality except that it is faster than usual, 100 to 110 beats per minute. It may be low in volume. It is usually regular. When an irregularity is there or when it is beating very fast, may be over 150 beats per minute, or very slow, about 30 beasts per minute, it indicates damage to the area of the heart from where the pulse beat originates.
Fever
Within 24 to 48 hours of a heart attack, and sometimes even earlier (four to eight hours), there is moderate rise in temperature of the patient. This may go up to 100°F, and in uncomplicated cases may persist up to two to six days.
Blood Pressure
As a rule, heart attack causes a fall in the blood pressure. This fall in blood pressure is proportionately greater in patients who had high blood pressure before.
E.C.G. in Heart Attack
Each beat of the heart is associated with an electrical impulse which passes over the heart muscle. This electrical impulse originates in the right auricle (Sino-auricular node) and travels over both the auricles in wave-like fashion to reach a place in the wall between the ventricles (auriculo ventricular node) and then spreads over both the ventricles.
Increased of White Blood cells (Leucocytosis)
In a normal average person, the total number of leucocytes in the blood is about 5,000 to 7,000 per c.mm. of these 50 to 60% are Polymorphonuclear cells, 30 to 40 percent lymphocytes, 3 to 4 percent mononuclear, 3 to 4 percent eosinophils and ½ to 1% basophiles.
In a case of heart attack, the total number of leucocytes as well as the relative percentage of poly morphonuclears is increased depending, among other factors, on the extent of the heart involved.
Increased Erythrocyte Sedimentation Rate (ESR or BSR)
Rate of sedimentation of the blood cells in the plasma when unclotted blood is allowed to stand under standard test conditions is valuable diagnostic aid in cases of heart attack.
System delay: updating the ‘4 Ds’ concept
The National Heart Attack Alert Program (1994) in the United States proposed a model for reducing delay to heart attack treatment: the ‘4 Ds’:
- D1, Door– initial triage based on a rapid assessment of the patient and handover from ambulance staff if the patient came by ambulance.
- D2. Data– time from arrival to recording the first 12-lead ECG
- D3, Decision– time from arrival to an appropriate clinical interpreting ECG and other data, explaining the risks and benefits to the patient and ordering thrombolytic, and
- D4, Drug– time from decision to administer thrombolytic to actually starting the treatment, including locating and drawing up the drug.
Homeopathic management of heart attack– Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat heart disease but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to manage heart attack symptoms that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. There are following remedies which are helpful in the management of heart attack symptoms:
Bryonia, Crataegus, Nux vomica, Arsenic Album, Ferrum Met, Sulphur, Veratrum Album, Sepia, Carbo Veg, Drosera, Lachesis, kali Carb, Natrum Mur, kali Bi and many other medicines.


Cactus and Spigelia often a good adjunct therapy as well or rems on their own – sometimes Aconitum if sudden
The spider and snake remedies are interesting to check out as well to see if any fit
Aconitum and NAJA is the best remedies in Heart Attack
fatty acid degeneration,nat phos 6x care taker of fat metabolism.bengal homeo doctors say check your stool round lumps should stick each other by mucus putty,graphite is king remedy.it is not so simple if sa node av node are not fine tuned,if stools have turned pale white putty stool,kent lecture on digitalis clarifies all doubts.fatty liver, inside body fatty raj,phosphorus nat sulph may help.this is complex business catch top most qualified professional.rajasthan villages tins and tins of ghee are used,no heart block this is hereditary miasm auto control, probably their grand fathers survived on camel milk ,matter of research for american homeopaths combine with travel tour to pushkar.