A 76 year-old man presented on 27/11/2018 with chronic non-healing ulcers in both legs since 5 yrs. The ulcers had burning pain with discharge of water and blood, non-offensive. There is redness around the ulcer with swelling of both the lower limbs. Burning pain < night/ prolonged sitting> open air. He had been on regular allopathic medication and ointment with temporary improvement and then recurrence of symptoms within a week. He was diagnosed with Lipodermatosclerosis.
Past History – Hypertension since 15 years. He is on a Meta xl 50/OD.
Knee replacement surgery in 2010 of the left knee, which was not successful and now the patient walks with a stick.
Family History – No significant family history
Personal History
Appetite – Good
Thirst – Normal, 3 lit/day
Bowe l- Very hard stool, passes once in 2-3 days.
Urine – Benign Prostatic Hypertrophy since 4 years; urine flow is increased at night with urgency and residual urine.
Sleep-disturbed due to frequent urination.
Dreams- of dead people
Perspiration- Normal
Thermals – likes cold weather, cannot stand heat and wants fanning in all seasons.
Mentals – Retired after 16 years from a government job. He had been very active in his work. He was always smiling and very friendly with people around. Loves talking to people. Very dictatorial as a person. He says that he loves himself the most. No fears and phobias, he is very courageous.
As stated by his daughters, he is very suspicious about his wife. He keeps tormenting her that she is having an affair with the young tenant boys in their house. He is always watchful and is very abusive towards her.
Analysis of the Case
Mentals
Suspicious
Dictatorial
Dreams of the dead
Loquacity
Abusive
Active
Physical Generals
Hot patient
Desires chicken
Particulars
Venous ulcers
Discharge blood
Discharge water
Repertorisation Chart
| Remedy Name | Lach | Phos | Lyc | Caust | Ars | Nux-v | Sulph | Rhus-t | Bell | Merc | Bry | Dulc |
| Totality | 19 | 19 | 19 | 17 | 16 | 16 | 16 | 16 | 15 | 15 | 14 | 14 |
| Symptoms Covered | 6 | 6 | 5 | 6 | 5 | 5 | 5 | 4 | 5 | 5 | 4 | 4 |
| Kingdom | ||||||||||||
| [Complete ] [Skin]Ulcers:Burning: | 3 | 3 | 4 | 4 | 4 | 3 | 4 | 4 | 2 | 4 | 2 | |
| [Complete ] [Mind]Loquacity: | 4 | 3 | 3 | 2 | 3 | 3 | 3 | 4 | 4 | 1 | 4 | 4 |
| [Complete ] [Mind]Suspiciousness, mistrustfulness: | 4 | 3 | 4 | 4 | 4 | 3 | 4 | 4 | 4 | 3 | 4 | 3 |
| [Complete ] [Mind]Dictatorial: | 3 | 3 | 4 | 3 | 1 | 3 | 1 | 1 | 3 | 3 | ||
| [Complete ] [Generalities]Food and drinks:Chicken:Desires: | 1 | 3 | 1 | |||||||||
| [Complete ] [Generalities]Discharges, secretions:Bloody: | 4 | 4 | 4 | 3 | 4 | 4 | 4 | 4 | 4 | 4 | 4 | 4 |
As per the Organon of Medicine- 6th Aphorism
- 6 Sixth Edition
The unprejudiced observer – well aware of the futility of transcendental speculations which can receive no confirmation from experience – be his powers of penetration ever so great, takes note of nothing in every individual disease, except the changes in the health of the body and of the mind (morbid phenomena, accidents, symptoms) which can be perceived externally by means of the senses; that is to say, he notices only the deviations from the former healthy state of the now diseased individual, which are felt by the patient himself, remarked by those around him and observed by the physician. All these perceptible signs represent the disease in its whole extent, that is, together they form the true and only conceivable portrait of the disease.
In this case apart from the totality of symptoms, information given by the daughter (which was never shared by the patient himself) helped to select the simillimum and get good results within a short time.
First prescription
Lachesis 200/ 3 doses
Sac lac daily 2 doses for 15 days
Follow up:
12/12/2018 Ulcers have healed up. But he has developed 2 small ones over the left big toe. Sac lac for 15 days
25/12/2018 Ulcers have healed up. No blood or watery discharge. Redness in the lower leg++ Sac Lac for 15 days
09/01/2019 ulcers have healed+
severe pain in the knees < rising from sleep
gas formation, distension of abdomen since 2 days
hard stool
appetite good
appetite – eating very little quantity
has lost his son in law, feeling sad about it
28/01/2019 mild redness and swelling of legs
no pain or burning
pain in knees is slightly better
gas formation is better
Lachesis 200/ 3 doses
Sac Lac for 15 days
11/02/2019 not much change in pain in knees
sob < walking
no cough or cold
no palpitation+
lots of flatus+
occ burning in stomach+
constipation+,
sleeps good
Appetite good
o/e redness of the rt leg+ Sac Lac for 15 days
28/02/2019 redness of the leg is better
now he has constipation and gas formation
pain in knees slightly better
he is able to walk at home Sac Lac for 15 days
15/03/2019 reddish discolouration around the ankle region.
No much pain.
pain in knees slightly better
constipated+ Sac Lac for 30 days
16/04/2019 mild redness of rt lower limb
pain in the knees is slightly better
no change in constipation
bowels – once in 2 days , has to be mechanically removed. associated with bloating of abdomen and tenderness.
urine output is good
urgency+
Rx: Lycopodium 200/3doses
Sac Lac for 30 days
22/05/2019 constipated, has to be mechanically removed
urine output is good
he has residual urine++
urine frequent – 4 times
no urgency at night
pain in knee no much change Sac Lac for 15 days
08/06/2019 Bowel is better now.
pain in knees < walking ,but is able to walk at home
no problem with skin now Sac Lac for 15 days
Before Treatment
Before Treatment
After Treatment
About the disease:
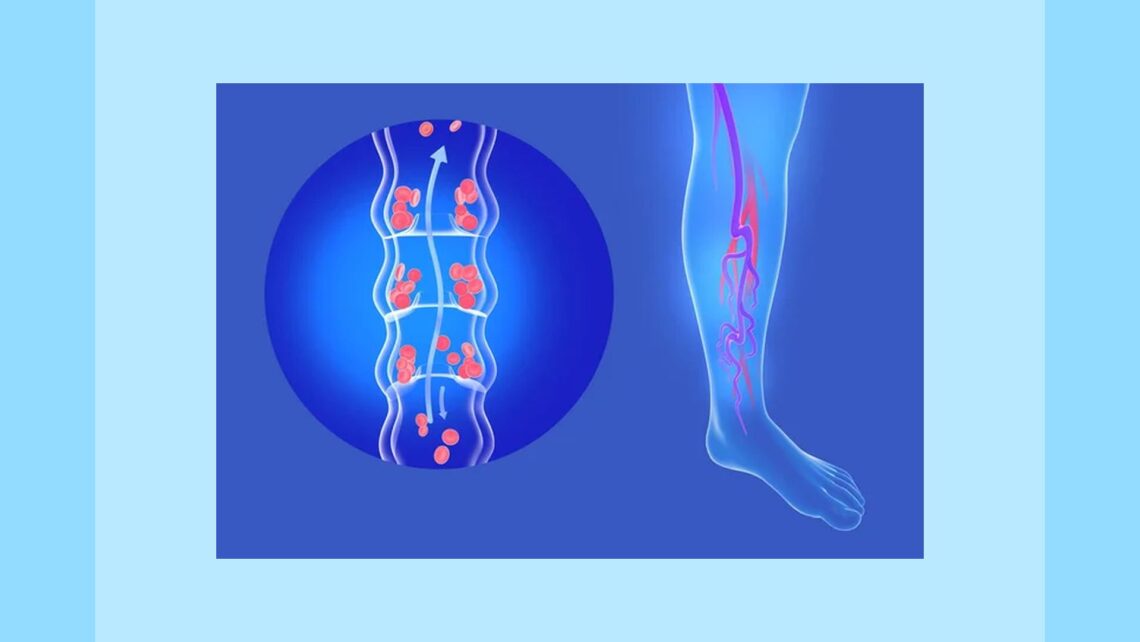
Lipodermatosclerosis is a chronic inflammatory condition characterised by subcutaneous fibrosis and hardening of the skin on the lower legs. Lipodermatosclerosis is also known as sclerosing panniculitis and hypodermitis sclerodermaformis. Lipodermatosclerosis is common, affecting middle-aged or older people. It is more common in women and is associated with immobility and a high body mass index (obesity).
This is caused by:
- Incompetent venous valves
- Venous outflow obstruction
- Dysfunction of the calf muscle pump [2].
The resulting venous hypertension causes an increase of leukocytes within the veins, which then migrate into surrounding tissue. The leukocytes become activated, attracting and releasing proinflammatory cells and cytokines, inducing a chronic inflammatory state. Increased collagen production leads to the fibrosis of subcutaneous fat.
Clinical features of lipodermatosclerosis:
Acute phase
Acute lipodermatosclerosis may mimic cellulitis, with induration, erythema, pain, itch, aching, and a feeling of swelling or heaviness in one or, more often, both lower limbs [2]. In the acute phase, signs may be localised to a single plaque but are usually more widespread. The most commonly affected areas are the pretibial or medial aspect of the leg.
Acute lipodermatosclerosis
Chronic phase
Induration, erythema, and pain continue in the chronic phase of lipodermatosclerosis. Subcutaneous fibrosis may result in significant narrowing of the distal lower limb, causing the leg to have an ‘upside-down champagne bottle’ appearance. Other clinical features of chronic venous insufficiency may be present, including hyperpigmentation of the skin from haemosiderin deposition, atrophie blanche, varicose veins, venous eczema, and venous ulcers.
Chronic lipodermatosclerosis
What are the complications of lipodermatosclerosis?
Lipodermatosclerosis is associated with poor wound healing because of the chronic inflammatory state and fibrosis. Venous ulcers commonly co-exist and may be difficult to treat.
How is lipodermatosclerosis diagnosed?
Lipodermatosclerosis is usually diagnosed clinically. Underlying venous insufficiency may be confirmed using Doppler studies.
A biopsy is helpful but should be performed with caution because of the likelihood of poor wound healing [3]. Any biopsy also needs to include the panniculus. The characteristic features seen upon biopsy are dependent on the stage of disease but include subcutaneous lobular and septal changes including:
- Adipocyte necrosis
- Pseudocyst formation
- Lipomembranous (fatty tissue) change
- Macrophage collections forming lipogranulomas (a nodule of inflamed fat cells around a foreign body)
- Iron deposition [4,5].
What is the differential diagnosis for lipodermatosclerosis?
Differential diagnoses for lipodermatosclerosis can include:
- Cellulitis
- Erythema nodosum
- Other causes of panniculitis
- Morphoea (localised scleroderma)
- Cutaneous vasculitis
- Necrobiosis lipoidica.
What is the treatment for lipodermatosclerosis?
General measures
Physical activity (walking) should be encouraged to increase the functionality of the calf muscle pump. Weight reduction is effective if obesity is a factor.
Compression therapy and elevation
Mechanical compression therapy using compression stockings or socks is the mainstay of treatment, encouraging venous return and assisting with symptom control, but may be poorly tolerated in some individuals.
Elevation of the legs can help reduce oedema and pain.
Allopathic Medical treatment
- Stanozolol can be effective for pain relief and has also shown to reduce dermal thickness [6].
- Pentoxifylline has been shown to be useful in venous ulcers in conjunction with compression or in patients who cannot tolerate compression.
- Combination therapy with hydroxychloroquine may reduce symptoms that are refractory to other treatments [7,8].
- Intralesional steroid injection of triamcinolone has proven to be effective at alleviating symptoms [9].
- Tetracyclines, such as doxycycline or minocycline, have anti-inflammatory and anti-angiogenic properties that may provide benefit [10–12].
- Phlebotonic drugs that modify the tone of the vein wall, including diosmin, hydroxyethylrutoside, or horse chestnut seed extract (escin), may reduce oedema and other symptoms [13].
- Ultrasound therapy may offer symptomatic benefit, relief of erythema, hardness and pain [14, 15].
- Ultraviolet radiation (UVA1) has been reported to be effective [16].
- Emollients and topical steroids are useful in the management of associated venous eczema.
Surgical treatment
Treatment of underlying venous insufficiency can improve symptoms and may reduce the risk of ulcer recurrence. Referral to a vascular surgeon should be considered. Leg vein therapies include:
- Endovenous ablation by laser, radiofrequency (RF) catheter, steam, cyanoacrylate and mechanical occlusion with chemical assistance (MOCA)
- Sclerotherapy
- Vein surgery [17].
What is the outcome for lipodermatosclerosis?
Venous insufficiency is a progressive disease. Although treatment can improve symptoms or slow progression, its associated conditions such as lipodermatosclerosis are usually chronic and recurring.








A very nice illustration of the complementary relation between Lachesis and Lycopodium and a demonstration that Lachesis is not always a remedy for women.
Do you know if the behavior of the patient with his wife is better now ?
In before treatment picture you have shown front side of leg while in after treatment it seems back side of leg????