November
Sherry, (not real name) age 50, previously diagnosed by her physician with COPD, was referred to my office by a D.O.M. for both homeopathy and psychotherapy. My colleague gently referred to her as a “nervous wreck.” Retrospectively, I think the patient may have been making my colleague a nervous wreck. (Allied professionals will often refer to me when a patient is making excessive demands on them or they don’t want to deal with mental health issues.)
November
She came in with an oxygen tank wheeled behind her and a friend to lean on. She could not drive on her own. She could barely walk and talk.
When she sat down and caught her breath, she presented her complaints like a semi-automatic: bam- bam-bam-bam-bam-bam-bam.
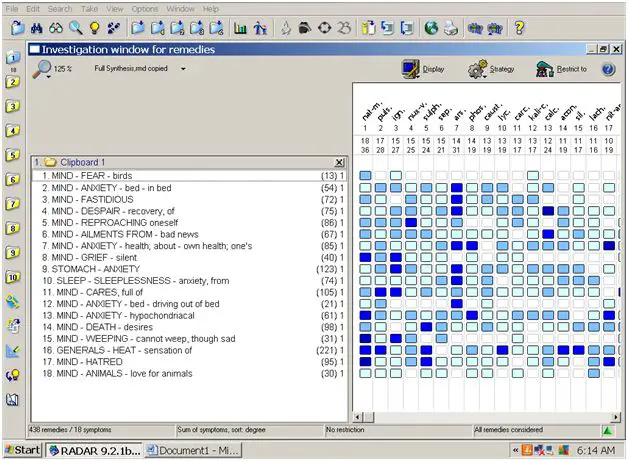
She told me she had anxiety—all the time. She was afraid of many things, including birds. She hated chickens, in particular. She even hated feathers. She shuddered as she mentioned them. I noted this carefully.
She complained that her heart beat constantly (I wryly thought to myself, “That’s probably a good thing,” but asked if she meant that it was rapid, and she said it was). Her pulse rate was approximately 110 while she was seated. She had no appetite and was quite emaciated. Her skin was wrinkled around muscle and bone. She felt most of her anxiety in her chest and solar plexus. She said the worst started when she received “bad news” about her blood pressure from an MD about two years ago. One year ago, she got an infection and couldn’t breathe. She was—even with an oxygen tank—still a smoker. She hyperventilated easily, was worried about her health, fastidious (3X), and woke at night from anxiety. She had spasms in the throat that felt like a lump and couldn’t swallow easily. Swallowing usually aggravated the lump in her throat. Generally, she was ameliorated by fresh air, open windows, being held by her husband and burping. She was generally worse for heat, for a dirty house and fatty foods.
She was born in town and lived in boarding schools. Her father was a “mean alcoholic and military man.” Her mother was a mild-mannered school teacher. Both she and her mother were beaten by her father. She used to throw up from anxiety when he came home. She used to re-iron clothes and re-make the beds to make sure everything was good enough for her father. Everything had “to be in the right place.”
She was married to a good, patient man, who, she smiled, was a “neat, orderly person, too.” As she’s speaking, my mind is flowing to Arsenicum, of course. But as usual, that’s not where this case goes. She goes on to describe a very interesting life—married five times, mother of two kids with whom she is close, drove a truck for a living, smoked and drank, was a bit addictive, tended bar, married a cowboy, got down and dirty with the best of them. She may have been fastidious and anxious, but this was no Arsenicum.
As she spoke of her divorces and disappointments, what began to emerge was a picture of a woman who needed love but had no idea how to go about getting it. There was a great deal of grief in her history (loss of parents, pets, lovers, friends). She was doubtful of recovery. Like an Ignatia patient (which also came to mind), she had melancholy, sadness and weeping. Unlike Ignatia, however, she eventually (second visit) wept in front of me. Mentally, she was much relieved by activity (like cleaning while she listened to music) and physically she was ameliorated by open air.
More importantly—she had received bad news, feared something terrible happening, and felt the same way as a little girl when she had to hide from her raging, drunk father—breathless with anxiety and fear. She longed for consolation (a rescue, of sorts).
Her ailments came into their fullness after her husband wrecked their car. Then one thing piled after on top of the other—their credit card was stolen, they had terrible doctors, and her worry for him blossomed into a full blown anxiety disorder. She fretted, “Where’s the love, the protection, the food?” She felt forsaken and prayed often for God’s support.
December
I took her case over the course of a few weeks in two separate repertorizations, both of which included Arsenicum, Natrum Muriaticum and Ignatia, as well as another, which turned out to be the one I chose:
December
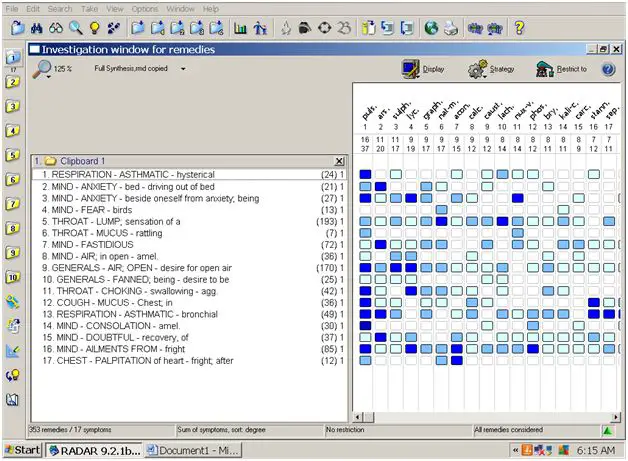
There were a few changes between the first case-taking and the second, which is why I appreciate the luxury of taking a case over time. First and most importantly, her description of her symptoms changed up a bit. This in itself would indicate a more “changeable” remedy. Second, while initially she would occasionally gripe, “I wish I was dead already. I can’t take this anymore,” she denied feeling that way at the next interview. I eliminated it as a symptom. Instead, I began to see her as more hysterical and dramatic. Instead of taking the rubric, MIND-Ailments From – bad news, I took MIND-Ailments From- fright, which seemed more accurate in the etiology of the entire case. Third, she originally stated that she didn’t cry. By the second interview, she was weeping openly and appreciated any reassurance given. She craved, more than anything, my support and assurance. Even though I didn’t take the rubric “forsaken” because it’s so large, I knew whatever remedy we chose, that had to be fundamental to its essence.
Interestingly, evidence for Natrum Muriaticum and Pulsatilla were in the same person. It made me think of an expression in AA: “Scratch an addict and you get a co-dependent.” I thought there was some truth to that, in that people may initially present with a Natrum “cover” or persona. But, after you get to know them, or they begin to recover, other aspects of their personality begin to reveal.
Because of the patient’s changeable moods, her tremendous anxiety, her thermals and craving for fresh air, her bronchial asthma, her palpitations from fright, and the desire for consolation, and her incredible fastidiousness, I chose Pulsatilla. Because of the precariousness of her physical state, I chose LM potencies.
January
I saw her after a month. She reported feeling better and looked like a different person—revivified, ruddier, less emaciated. The mucus in her chest and throat were going away. The throat spasms and the sensation of a lump were gone. Curiously, she started feeding birds in her neighborhood (homeopathy never ceases to amaze and surprise me!) even though the materia medica makes no reference to poultry (!) phobia in Pulsatilla. She started to talk about her anxiety and her childhood in a way that suggested she was less buffeted by the memories and more the master of them.
February
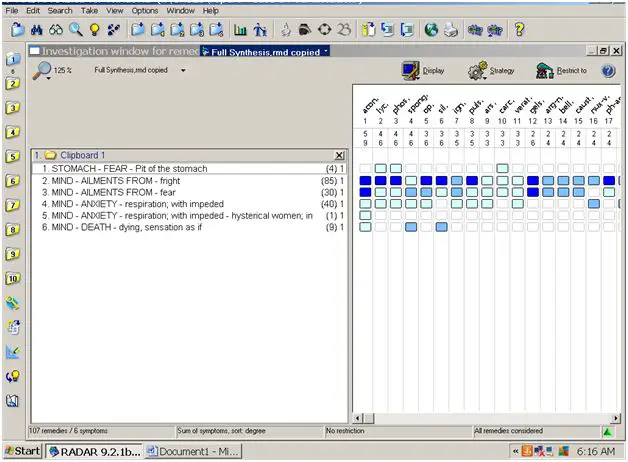
Very shortly thereafter, she began to have the symptoms of her initial visit: an impending doom, a superficial hysteria (“what if it doesn’t work?!!”), impeded respiration in a more acute presentation so that she clung to her oxygen. When she called, she’d had the symptoms for about three days. After clarifying that she’d been seen by a doctor (she’d gone to the Emergency Department), I took her symptoms to see if she needed an intercurrent.
Aconite came up first and made good sense to me. That could certainly be the layer of fright presenting itself.
However, after reviewing the nature of her symptoms (which were moving backwards in time), the relatively brief exacerbation, and the fact that all medical indicators (blood oxygen, etc…) were stable, I concluded that she was having an aggravation and that in due time it would stop if we stayed the course and I provided support for her instead of a remedy. This was an opportune time to teach her self-hypnosis and deep relaxation, which we did. I considered a placebo, but I opted for a technique that enhanced her sense of resourcefulness and self-reliance.
February
We continued on Pulsatilla LM potencies for the next few months with bi-weekly therapy sessions, as well. We moved her up LM levels every two to three weeks or so.
June
By the time she got up to LM6, she was eating well, gaining weight, had no heart symptoms, had stopped smoking, and had stopped all allopathic pharmaceuticals. She was not using oxygen.
October
She stayed on Pulsatilla for approximately 1 year. I saw her once after she got to LM10, when she said she felt fine and needed no further appointments for the time being. I have not heard anything since, but have heard from the referral source that she is doing “blessedly well.”
www.JudithAcostaLISW.com