This is a case of COVID in a 58-year-old surgeon. He has asthma in winter, is hypertensive since many years and had myocardial infarct last year. His wife is a homoeopath, and she treated him for the first few days.
17-10-20: The patient started experiencing boring throat pain in the evening and also fatigue.
18-10-20: Next morning he had mild discomfort and a feeling of malaise. He continued his daily professional activities. The same evening, he had fever gradually rising up to 101F and throat pain. He had very short lasting (a few seconds) chills before fever. Profound weakness during fever.
Rx: Ars Alb 30 one dose. He took Paracetamol 650 mg to bring down the fever. Azithromycin 250 mg b.i.d.
19-10-20: Fever going up to 101 F. Throat pain, difficulty swallowing food. Profound weakness. Drowsiness. O2 saturation fluctuated between 95 and 97.
RT PCR, HRCT Chest and basic blood work were done on day 2 of fever because of his co-morbidities.
Blood work was WNL including WBC total and diff. count.
HRCT chest was normal; no GGO noted.
RT PCR: Positive for COVID19. Cycle threshold was 16.
Rx: Ferrum Phos 6x dissolved in water q.4.h.. Azithromycin continued for 5 days. Paracetamol as needed.
20-10-20: Fever continued. Throat pain severity a little less. Oxygen saturation maintained at 95.
Rx: Ferrum Phos 6x dissolved water, q.4.h. and Pyrogen 30 t.d.s., Paracetamol as needed, Favipiravir 400 mg started.
21-10-20: On this day his wife consulted me in the night. Fever at 99. No chills. Extreme weakness. Thirsty as usual. A little bit of coughing started. Asking for tasty food, pav bhaji, batata poha. Has become very irritable and very drowsy. He would give short answers and when pressed for details, he would get angry. Oxygen maintained at 95. I took these rubrics:
Chill absent fever during
Heat concomitant, Exhaustion, Weakness
Heat concomitant, Sleepiness
Irritability during fever/when questioned
Hurry
Dictatorial
Irritability during fever
He was asking for tasty food. He is very impatient and domineering by nature. He has a feeling of hurry to get better very fast.
I advised Nux vomica 200, q.4.h. which he took on 22nd & 23rd October. After that he was much better. No fever, no throat pain. Weakness was much better.

Covid-19 Coronavirus SARS-CoV-2 cell pandemic virus. 3d render, 3d illustration
26-10-20: Cough with rattling in chest. Advised Nux vom 200, single dose. His wife gave him one powder dose of Nux and he finished the entire bottle of Nux in 2 days. His wife mentioned that usually his cough increases and he gets wheezing and has to use an inhaler. However, this time he did not need to use the inhaler. The Nux was working in spite of the Favipiravir.
HRCT done on 27-10-20: GGO in both lung bases, score 4/25. CRP 2.9, Ferritin 228, D-dimer 363, IL-6 2.34.
Rx: Tuberculinum Aviare 30, two doses on 27-10-20.
30-10-20: No cough. Secretions in chest decreased. No more complaints.
4-11-20: CT scan shows scattered fibrosis. RT PCR still mildly positive. Cycle threshold 33. CRP 4.2.
[In contemporary literature, Hypersensitive Pneumonitis caused by Mycobacterium Avium- “hot-lung disease”- has striking similarities with COVID19 including ground-glass opacities on CT scan.
Anshutz in “New, Old and Forgotten Remedies” summarizes anecdotal cases of influenzal bronchitis effectively treated by Tuberculinum Aviare.
Other indications of Tub Aviare are:
Recurrent tendency for cough & cold.
Rattling without expectoration
Post influenza, cough remains with weakness]
On 1-11-20 (day 16) patient went cycling for 45 mins at 5 am in the morning as he was feeling fit. On 3-11-20 (18 days after he fell sick) he started with his surgical practice. He did not have any post covid weakness. He only gets tired if he has to stand for very long during surgery. Other than that, he is feeling fine. He took Favipiravir for 9 days as opposed to 14 days as he was feeling fine.




Dt. 9.9.21
Dear Chandana
Though I am Civil Engineer ,
But I have great faith in Homeopathy treatment. There is rumer that homeopathy works slow in fact homeopathy works fastest becoz its action is on nerve system this is never brought to the notice of the public.
I myself suffered from following disease time to time:
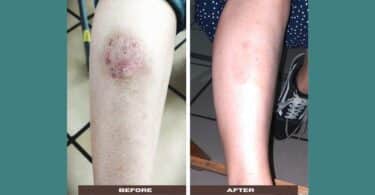
1. Wet eczema
Wet Chronic eczema from 1971 to 1986 . On 1987 I got treatment from Dr Mengai of Shahabad Je said I am Graphits patient he has been quite successful in treating eczema. I also studied Boreick’s Materia Medica. I knew about Doses acute and Chronic disease effectiveness of selection of remedy and its potencies. I say a dose of 200 potency can work for 2 months without second dose. There are follow well there are combination. So many tricks are available. I proclaim that whole word can be cured and can be eczema free by only using Homeopathic remedies Grephites, Sulphur, Silicia , Calendula , Thuza, Petroleum, Skukum Chuck, hepar sulph, myristica Lachesis, out of these mere Sulphur and petroleum and Graphitise are far enough to trat word’s 95 % population suffering from skin diseases.
2. Coughing and Chronic Bronchitis running nose stuff nose
I got treated from these ailment by Remedies nosode Tubercullinum, Medorhinum, Baccilinum high potencies one drop at 3 month interval alternatively take for few year one can be permanently be cured I proclaim this is highly effective in any patient. Care that high doses only to be take. Non veg to be avoided. Alcohol to be avoided.
3. Malaria: In 1996 I frequently suffered from malaria 4 -5 times some How I was highly distressed from Resochin tablets it mad my life hell. Fortunately I visited Banaji Homeo Pharmacy Clinic Princess street Mumbai, the Person in the shop was a Girl I asked I want some homeopathy medicine for Malaria ailment. She gave me pills with label written malaria. I took 4 pills within no time I started feeling well I continued few more days I became ok. Later on some pain comes I apprehend Malaria I used to take 4 pills 3 times a day. Now it is about 24 years I never suffered from malaria . My case is the 8th wonder after Taj.
4. Sinusitis: I suffered From sinusitis From 2005 for this I am still trying homeopathy medicine My study is on.
5. Spondylitis: I suffered from Spondylitis in 2005-2007 . I tried Kali Bich 30 potency this was given by My Homeopathic Doctor Dr. Mrityunjay Ghosh at New Alipur he was excellent young doctor highly dedicated. Frequently I took Kali Bich 6 to 30 potency as and when required I om Ok Now. This is Another Wonder after Taj.
6. From 2012 I suffered Rheumatoid Arthritis I tried so many Homeopathic remedies Angusta, Calcaria Floor, Rhus Tox , Sulphur but I say I am totally failed . Homeopathy failed . I had to rush to Rheumatologist in Pun.e The Dr. gave me Saaz , HCQS, Eterocoxib, Sompraz, Folic acid Deflaze cort I have satisfaction with these Allopathy treatment for Rheumatoid Arthritis I am some how managing till date. In Nov 2020 I tried Bryonia 200 for Rheumatoid treatment but failed it partially worked . Here I accept that I failed to overcome Rheumatoid Arthritis ailment. Some More research is required.
Conclusion:
I conclude the experimental success that after witnessing above miracles I always suggest people to try Homeopathy if they want to be permanently cured and to be healthy and happy.
My research is still on.
But I have complaint against Govt. that Govt opened Medical Colleges and the Growth of Homeopathy has suffered. Homeopathy is not for earning bread it is medical sport and to be played in sporting and fighting spirit to achieve mark.
It is well proved and settled that there is no side effect of homeopathy medicine hence non medico like me to be legally allowed to treat patients. There cannot be any better Homeopath than me for above treatments My knowledge is highly tested the time. My knowledge and growth suffered becoz I am not Registered Medical Practitioner legally I can not administer homeopathy medicine on other people suffering from disease which can be surely cured.
In fact homeopathy medicine to be made free to be administered buy any body on any body just like air water and salt.
Govt. Must make Homeopathy free from any restriction in the interest of Public interest.
I hope only a homeopath can understand what I expressed above.
Regards.
Gopal Khairwar
Mob: 9631767280 Pune