My first encounter with Post traumatic Stress Disorder, or PTSD dates all the way back to the early 80’s in Moscow, USSR. I was a young family physician then. One day, during routine home visits I meet a young man who just recently came back from Afghanistan. At that time the war was between the Soviet Union and Afghan rebels. As we are learning now, the consequences to both parties involved were and remain the same. They were and are disastrous. That young man apparently witnessed a number of atrocities. He was visibly anxious to the point of sheer panic. He also complained of frequent flashbacks and night terrors he experienced almost every night. Unfortunately, at that time I was just beginning to practice homeopathy and could not fully appreciate this and adequately prescribe for the young man. Later in my life I had another opportunity to face PTSD. Lamentably, this opportunity is known worldwide as 9/11. I was in New York working at the Center for Health and Healing of the Beth Israel Medical Center. I was surprised that very few patients came. But slowly, more and more surfaced, frequently coming with seemingly unrelated complaints. I’ve seen a significant number of patients since then and as it turned out, this time I was well prepared. Homeopathy brought about amazing results of the kind that conventional (allopathic) psychiatry has not been able to achieve. The goal of this article is to share my experience with my fellow homeopaths, and anyone willing to learn and apply this miraculous healing practice of homeopathy.
Definition
Posttraumatic Stress Disorder, or PTSD, is a psychiatric disorder that can occur following the experience or witnessing of life-threatening events, such as military combat, natural disasters, terrorist incidents, serious accidents, or violent personal assault like rape. People who suffer from PTSD often relive the experience through nightmares and flashbacks, have difficulty sleeping and feel detached or estranged. These symptoms can be severe enough and last long enough to significantly impair the person’s daily life.
Data from a number of studies indicates that up to 30% of individuals of various age groups, including children and adolescents exposed to life-threatening events, present with a clinical picture of PTSD 1-4. Unfortunately, only about a fourth of victims discuss their problems. For example, despite universal health coverage and the benefits of an employee assistance program for all employees, only 28.5% of those with PTSD symptoms have talked to a health professional about the events of Hurricane Katrina or issues encountered since the storm 4.
To memorize all the key signs of PTSD, psychiatrists suggest the following mnemonic:
PTSD Mnemonic
E – Event/experience (threatening to life or physical integrity of self or others)
R – Re-experiencing (flashbacks, nightmares etc)
A – Arousal (anxiety, startle, hypervigilance, irritability)
A – Avoidance (of things, places, images etc. reminiscent of event)
D – Duration of plus one month
It is important to remember that PTSD can occur at any age, including childhood. Not surprisingly, PTSD is generally more severe or long-lasting when the trauma is of human design (e.g., torture, terrorist attack) vs. a natural disaster (e.g., earthquake)
History of PTSD
As one can easily imagine, even from such a basic fact as having had wars throughout human history, PTSD has always been there. Below are some highlights of historical development for better understanding of PTSD.
1900 B.C. – Egyptian physicians report hysterical reaction.
VIII Century B.C. – Homer in The Odyssey describes flashbacks and survivor’s guilt.
490 B.C. – Herodotus writes of a soldier going blind after witnessing the death of a comrade next to him.
1597 – Shakespeare vividly describes war sequelae in King Henry IV
1600 – Samuel Pepys describes symptoms in survivors of the great fire of London.
1879 – Rigler coins term Compensation Neurosis
1880’s – Pierre Janet studies and treats traumatic stress. He describes “hysterical and dissociative symptoms”, inability to integrate memories, by “phasic nature” of suppression and intrusion.
1899 – Helmut Oppenheim coins term Traumatic Neurosis
WW I: – “Shell Shock”
WW II: -“Battle fatigue”, “Combat exhaustion”, and, again, “Traumatic Neurosis”
1980 – PTSD becomes a diagnostic category in DSM III
Careful research and documentation of PTSD began in earnest after the Vietnam War. The National Vietnam Veterans Readjustment Study estimated in 1988 that the prevalence of PTSD in that group was 15.2% and that 30% had experienced the disorder at some point since returning from Vietnam.
Nowadays clinical criteria characteristic to the majority of patients is best described in the Fourth Edition of the Diagnostic and Statistical Manual of Mental Disorders 5.
• Exposure to a Trauma – The person has been exposed to a trauma, in which he or she has experienced or witnessed an event involving the threat of death, serious injury, or a threat to the physical well-being of oneself or others. Note that only physical threats count in the definition of a trauma in PTSD. Situations that represent a psychological threat (e.g., a divorce, being criticized by a loved one, being teased) are not considered traumas in the definition of PTSD, even though they may lead to difficulties for the individual.
• A Response of Fear, Helplessness, or Horror – The immediate response to the trauma is one of fear, helplessness or horror (in children, it may be a response involving disorganized behavior or agitation). If an individual’s response to the trauma is primarily one of sadness or loss, rather than fear (this is often the case following the death of a loved one who was ill), PTSD would likely not be diagnosed.
• Symptoms of Re-Experiencing the Trauma – The individual persistently re-experiences the event in at least one of the following ways:
1. Recurrent and disturbing memories, images, and thoughts about the trauma.
2. Recurrent and disturbing dreams or nightmares about the trauma
3. Acting or feeling as if the trauma was occurring again (these experiences are often called flashbacks). This may include hallucinations (e.g., seeing things or hearing voices that were present during the trauma, even though they are not really there currently), misinterpreting things that are heard or seen (e.g., being convinced that the sound of fireworks in the distance is actually the sound of gunfire).
4. Becoming emotionally upset upon being exposed to reminders of the trauma, including physical sensations that were present during the trauma or situational reminders (e.g., the street where the trauma occurred, the anniversary of the trauma).
5. Becoming physically aroused (e.g., breathless, heart racing) upon being exposed to reminders of the trauma, including physical sensations that were present during the trauma or situational reminders (e.g., the street where the trauma occurred, the anniversary of the trauma).
• Symptoms of Avoidance and Emotional Numbing – The individual avoids triggers and reminders of the trauma, or experiences a sense of emotional numbing, as indicated by at least three of the following features:
1. Avoiding thoughts, feelings, or conversations that remind the individual of the trauma.
2. Avoiding activities, places or people that remind the individual of the trauma.
3. An inability to remember important aspects of the trauma.
4. A lack of interest or participation in significant activities, such as socializing, work, and hobbies.
5. Feeling detached or different from others.
6. An inability to enjoy things or to experience positive emotions (e.g., feeling “flat”).
7. A sense that one’s future will be shortened. For example, it may be difficult to imagine having a career, getting married, having children, or having a normal life span.
• Symptoms of Increased Arousal and Vigilance – The individual has symptoms of arousal and vigilance that were not present before the trauma, as indicated by at least two of the following features:
1. Difficulty falling or staying asleep.
2. Feeling irritable and grumpy, or experiencing outbursts of anger and temper tantrums.
3. Difficulty concentrating.
4. Hypervigilance (e.g., always being on guard, looking over one’s shoulder while walking down the street, etc.)
5. Becoming startled very easily (e.g., jumping when the telephone rings).
• The problem must last at least one month for a diagnosis of PTSD to be assigned.
• The individual’s fear, anxiety, avoidance, or other PTSD symptoms cause significant distress (i.e., it bothers the person that he or she has the symptoms) or significant interference in the person’s day-to-day life. For example, the difficulties may make it difficult for the person to perform important tasks at work, meet new friends, attend classes, or interact with others.
Conventional Treatments for PTSD and Acute Stress Disorder.
Most of the treatment guidelines suggest psychotropic medications (psychopharmacology) and /or various types of psychotherapy6-8. While certain types of psychotherapy have been consistently shown to be effective in treatment of PTSD7,9, the evidence of the effectiveness of psychotropic medications has been, at best inconclusive 8,9. Remarkably, one of the most frequently used prophylactic psychological tools, a brief psychological intervention (debriefing), that is conducted immediately after the exposure to a stressful event, has also been reported ineffective in preventing of development of PTSD10. A large proportion of female PTSD victims opt for psychotherapy over medication11. Most frequently cited reasons are the effectiveness (or lack thereof) of a treatment, including potential masking of symptoms with the medication and more logical, long-lasting effects with the psychotherapy.
There is also evidence suggesting that in depressed patients with a history of early childhood trauma (loss of parents at an early age, physical or sexual abuse, or neglect), psychotherapy alone was superior to antidepressant monotherapy12.
Various ethical issues13 that exist around research, production, and marketing of antidepressants and other psychotropic medications also make the efficacy and safety of psychopharmacology highly questionable.
Amazingly, some allopathic physicians have suggested that there is no evidence that conventional medication, including psychotropic medications, “are likely to do more good than harm in the long term” and that “although several drug classes (and possibly some antidepressants) are known to induce psychic indifference, the utility and desirability of this effect is doubtful”15.
As a matter of fact, the authors cited above represent a group of physicians who suggest a so called “drug-centered approach,” the essence of which is an idea that conventional drugs, instead of treating the target problem create a different state in the brain or the body (i.e. sedation) that simply suppresses symptoms of the illness rather that treating them.
Homeopathic Approach to PTSD
There are also very few peer reviewed papers on homeopathic treatment of anxiety disorder available at this time16-18. They offer only very general guidelines on homeopathic treatment of this serious mental health issue. However, homeopathic literature has an almost 200 year history of clinical reports of successful application of homeopathy starting with the original proving of Aconitum described by Hahnemann19.
While the helpful presence of homeopaths during World War I is a strong possibility, the writer was not able to gain access to any records of their success. Unfortunately, all man-made catastrophic events beginning with World War II, up until September 11, 2001, probably lacked trained homeopaths due to limited access to patients and an obvious decline of the number of homeopathic practitioners per capita. India’s vast number of trained homeopathic practitioners is an exception to the rule, but again, the author has no access to reports from this part of the World.
The terrorist attack on 9/11 produced vast numbers of patients suffering from PTSD compatible to the Vietnam War or a nuclear disaster in Japan during WWII20,21.
This time a number of homeopaths (although not as large as one would desire) were able to participate in treatment of victims of this catastrophic event. Some of them, including the writer, have published case reports22-29. Despite differences in training and theoretical approaches to assessment and treatment of homeopathic patients, the results reported were uniformly impressive. Those treated with homeopathy were able to recover completely and go on with their life. Later Roger Morrison and Nancy Herrick participated in treatment of victims of the terrorist act in Bali and reported amazing results using only very basic homeopathic remedies30. Other homeopaths also participated in homeopathic treatment of victims of natural disasters and have reported overwhelming success with use of very few standard homeopathic remedies39,40. As a result, the homeopathic community has gained an insight into the practical aspects of treating PTSD.
Methodology of Homeopathic treatment of PTSD
- One should clearly understand the difference between the acute and chronic illness. Especially in the case of a massive terrorizing disaster. The latter produces a Genus Epidemicus33 type response. A few remedies will most likely be very frequently required for the majority of the population. In a case of a natural disaster, such as an earthquake or a hurricane, the majority of relatively healthy people are going to respond with the picture of a limited number of remedies. For example, victims of earthquakes in Honduras responded very well to Aconitum31, while victims of hurricane Katrina frequently presented with a clinical picture of Ignatia amara32. Roger Morrison and Nancy Herrick reported an amazingly good response by victims of the Bali terrorist attack to Aconitum and Arnica30. One should know the Materia Medica of these frequently prescribed remedies very well. In the first few hours/days after the disaster the clinical presentation of victims will be very clear. The response to the remedy is going to be very dramatic and satisfying to both the patient and the practitioner.
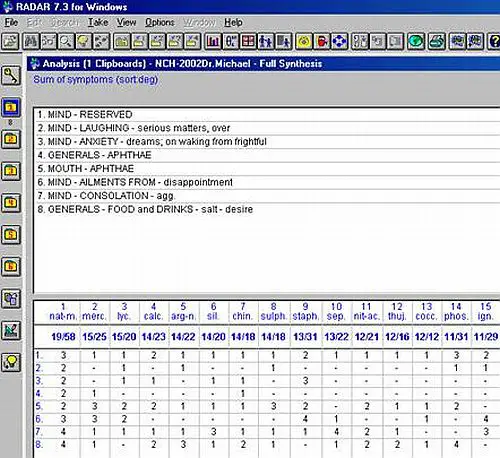
- There are going to be individuals who are constitutionally predisposed to be sensitive to stressors characteristic to terror inducing events. For example, a patient whose constitutional remedy is Natrum Muriaticum, will most likely respond with a clinical picture that indicates this remedy. Shortly after 9/11 I saw a young cardiologist, whom I’ll call Dr. Michael. His main complaint was large painful aphthae deep in the mouth that did not allow him to eat any solid food. Visual: Very quiet, reserved. Neat. Laughs while talking about serious problems. Complaints: 1.Wakes very anxious from scary dreams 2. Large aphthae in the mouth – unable to eat. 3. These problems since 9-11: felt “very disappointed”, “abandoned”. Some Hx: Responsible, serious since young age. Does not tolerate abandonment too well. When upset, needs to stay alone. Recently started craving salt “like crazy.” His girlfriend says, “he would eat it with tablespoons, if he could.”
Below is a pretty straightforward repertorization.
Here are Dr. Michael’s e-mails after I gave him one dose of Natrum Muriaticum 200C:
2 days later: ” Ed, I can eat now. I think I’m 50% better”. Had my first normal meal today. First time in almost 3 weeks. Thank you very much. This small pill really worked.
5 days later: “I’m 90% better. Going to a steak house tonight”
6 months follow up: Remains well. No anxiety. No aphthae. Now realizes that he was “quite depressed too.” That is better too. “The depression is gone.”
- Even when the Genus Epidemicus has been clearly identified, one must remain alert and conduct thorough evaluations, as different people will still react differently to the same stressor. Mitch Fleisher24 described a case of Acute Stress Disorder when two people both exposed to the events of 9/11 developed two different clinical pictures. One required Aconitum ( in my observation, a leading remedy after 9/11; another – Gelsemium). I reported a similar situation that happened with two experienced homeopaths during our trip to the International Academy of Homeopathy (Alonisos, Greece)33. They were riding on the same motorbike and fell rather suddenly. Both were shaken up. They were evaluated and treated by Paul Herscu. One presented with a clear picture of Pulsatilla, another – Arsenicum album. A “typical” fall with psychological sequealea. Actually, the homeopath who needed Arsenicum album stated that he was fine. But Arnica still was not indicated. Automatic. “protocol” prescribing should never be a part of homeopathic practice. This principle does not exclude consideration of remedies that are most likely to be effective in a particular situation. But there always has to be differentiation of presenting symptoms. In another paper23 I presented a case of two people who slept in the same house when a part of the fuselage of the airplane that crashed in Bell Harbor on November 12, 2001 landed in the garage of their house. One required Stramonium, the other – Opium. Both were morbidly scared and both went into a state of their constitutional remedy bypassing the Aconitum state.
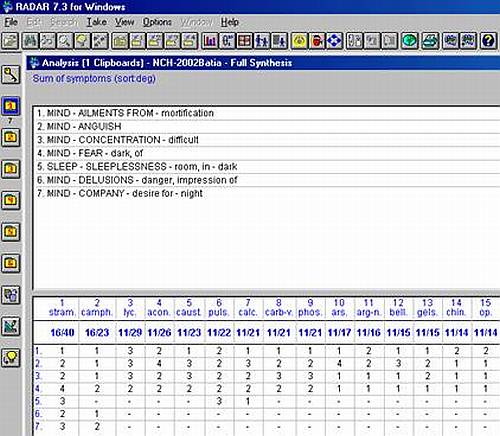
Below is a detailed description of their cases.
BATIA:
“I could not believe it! I wake up and the airplane is sitting in my garage! They even found airplane parts in the bedroom! My enemies should be that lucky!”
- Anguish
- Cannot concentrate
- Fear of the dark
- Cannot sleep in the dark room
- Night terrors
- Needs company
- Feels “in danger”
Cured after one dose of Stramonium 30C
Ari, a 23 year old macho-man, Batia’s nephew. He was in the same house when the airplane hit the house.
ARI
No symptoms right away. But in course of a few weeks became progressively sleepy. Reported feeling “kind of dreamy”, absent-minded, had anxious dreams. Started thinking about death a lot. “The weirdest thing, doc, is that I sometimes feel like somebody is lying in bed with me.” He also did not care for girls, became very lazy and constipated.
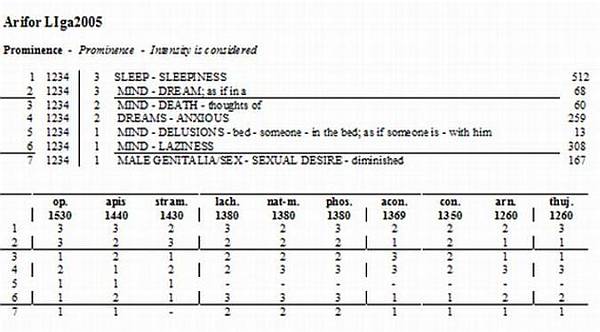
- There is a continued argument between firm believers in one, and only one constitutional remedy that “works” for each and every occasion for a particular person, and homeopaths who believe in prescribing different remedies to the same person depending on a particular acute situation. It has been my experience that even in cases when long-term follow up reveals that the initially prescribed remedy was not constitutional, one still can see significant improvement after accurate acute prescribing. For example, one of the first patients a saw after 9/11 was in both the 1993 and 2001 Twin Tower bombings. On the morning of 9/11 Richard (that is his alias, of course) was on a subway station under the WTC when the first airplanes hit the building. Evacuated with everyone else he realized that his attaché case was left at the subway station. He went back, and crawling in the dark, retrieved the case and went to his office in the building right across from the WTC. He stayed glued to the window and watched the bodies flying through the air. These pictures stayed with him day and night ever since. He became progressively more withdrawn. He was morbidly afraid of the dark. Had terrible nightmares and flash-backs. Usually a mild-mannered man, he became extremely argumentative. At one point two young men attempted to mug him at the parking lot. He bit them viciously until the police came. Even then he had to be pulled away from the criminals. He was literally unable to sleep because of constant nightmares. He also felt very guilty that he was alive while his colleagues and friends from the WTC were dead. He lost all his concentration. A very prominent computer analyst, he was paid a high salary, but was unable to perform. Richard had all the symptoms of PTSD.
Below is a simple repertorization of the case:
Follow up two weeks after one dose of Stramonium 200C. No nightmares for the last 5 days.
4 weeks later:
In the course of a total of 6 weeks since the remedy, only two nightmares, mood is much better, significantly less irritable.
An apparent success? Actually Richard continued to complain of feelings of guilt and poor concentration. Although significantly improved, he still suffered from some consequences of PTSD. It took two re-takes using the Sensation method until I arrived to his constitutional remedy. It has been over 1.5 years since he presented with no complaints after a few doses of Aurum Bromatum. It’s a rare remedy and involved a long process of finding it. Even the first relatively superficial prescription changed Richard’s life rather dramatically.
Homeopathic approach to PTSD in children
Children are more and more frequently exposed to physical and sexual abuse. They also silently watch their parents argue, getting divorced, behave violently towards each other. It also has been my experience that violent, terrifying events that occur in a mother’s life during pregnancy may affect the fetus rather dramatically. On more than one occasion, I found a correct remedy based on a history of the pregnancy.
Children who suffer from PTSD experience the event over and over through strong memories, flashbacks, and nightmares. They also often worry about dying at a young age. The main psychological mechanism that young children and teenagers use is acting out. Naturally, children cannot clearly express their feelings. Observing their behavior in the office is key to successful prescribing. Oppositional and at times violent behavior in a child, should alarm health providers to a possibility of PTSD.
In my experience, the most frequently prescribed remedies for PTSD in children are Ignatia amara, Aconitum and Stramonium. Ignatia is a very important remedy in this age group. I have successfully treated numerous children of unstable argumentative parents with this remedy. Frequently, but not always, children who need Ignatia, have a hysterical component to their behavior.
Another very important remedy, especially during adolescence is Mancinella. Children who need this remedy present with a unique feeling of being controlled by some outside entity. The remedy is derived from Hippomane mancinella (Manzanillo), a euphorbiaceaous tree that grows on a territory spreading from Mexico and the West Indies through Columbia. Provers of this plant reported a feeling of “being taken by the devil” (possessed)48. The remedy state frequently first appears in adolescence. One of the adolescent boys I meat benefited greatly from Mancinella.
Jordan came to my office by accident. I met his father at a mutual friend’s party. After learning that I am a board certified psychiatrist, he asked me whether I could do anything to help his thirteen-year-old son, and he gave me the following details.
Jordan seemed to be constantly preoccupied and constantly worried. When asked what was going on, he would answer that he had the same thought going through his head. He also had to repeat certain activities every day. Before leaving to school, for example, he had to touch the door exactly five times in the exact same spot, and then he had to walk five steps forward and five steps backward. He also had to repeat certain words, many times in a row, before he felt he could sit down at the dinner table. Pretty disorganized before the problem arose, Jordan absolutely had to have certain things on his desk in a certain order now. He was also very anxious and couldn’t concentrate at school. All these problems had started cropping up about a month after the attack on 9/11. Jordan had seen the footage on TV and had got very upset.
I explained to Jordan’s father that I practice homeopathy and I’d be glad to help, but he needed to understand what I do clearly. I recommended a book to read. Soon after our conversation, he set an appointment. When Jordan and his parents came to my office, I could tell that Jordan was a quiet, timid young man. He told me that something weird was sitting inside of him and “this thing” controlled what he was doing. He couldn’t stop thinking about this problem. He was tormented by it, preoccupied with these thoughts all day and night. He felt depressed and had developed vertigo that was much worse in the morning. He also felt dull. Often he caught himself forgetting why he’d gone to the kitchen, or what he was looking for in a drawer. His concentration was terrible. Formerly happy, easygoing, and sharp, now he was constantly afraid that something bad was going to happen to him or to his family. He wanted to stay around people all the time.
The family was seriously considering heavy-duty psychiatric medications. The conventional diagnosis of this condition would be PTSD with strong elements of OCD. Preoccupation with this “thing” that was telling Jordan what to do could have been also classified as a delusion—maybe he was hallucinating. The selection of conventional medications could have been daunting, and likely would have included an antipsychotic. The Mancinella worked beautifully for him. Jordan’s symptoms gradually went away.
Conclusion.
As we all know too well in real life, finding the correct homeopathic remedy, the real Simillimum is not such an easy task as it looks in those refined descriptions of successful cases. My hope is that we are approaching the time when more and more health professionals will be able to contribute to our knowledge and skill in finding this amazing “magic” pill.
See Dr. Shalts’ biography below….





Fantasic article with some great insights, thanks very much.
repertorization of three cases here: http://www.facebook.com/photo.php?fbid=186834291349307&set=a.169326306433439.37491.100000682136934
It is wonderful to see such an in depth article today when most resort to take very strong anti depressives or similar medicines which merely suppresses the sypmtoms. A pity that more people do not seeki homeopathy for emotional problems. Thanks to Shalt for the detailed article with demostration through repertory.
It is a very interesting article in which one more time enphasis is in individualisation of the constitution, the reaction to a traumatic situation and Unicist Homeopathy . Thanks for sharing your clinical experience !
Dear Edward,
Thank you for this article on PTSD, it is an area of great potential and promise in homeopathy and I am interested to read the references but they don’t seem to show at the end of the article. Is it possible that they could be emailed to me or included in these comments to see?
Excellent case work, doctor. I have a patient that complained of ‘adrenal shutdown’ and manic rage followed by collapse. It took 6 months of prescribing to ‘uncover’ the exciting cause: witnessing a fatal car crash which involved a driver that passed her on a mountain road only to crash head on into an oncoming vehicle within several hundred meters of her own car. I did not get this information during her initial intake or carefully working with her to get a timeline of her social and health history. Mention of this event finally emerged after prescribing Aconitum napellus.
The exciting cause was 18 years ago. My clues to PTSD were her narratives of these ‘attacks’ of fright and rage while in a car, either driving or as a passenger. Her statements were very characteristic: “I didn’t do anything wrong; It’s not my fault; I hate it when people do stupid things.”
I have suffered for almost 30 yrs from panic attacks, depression and phobias. I was involved in an accident in 1981 where I was the passenger and we got hit, and even though no one was injured, I started having what my psychiatrist termed “depersonalization” accompanied with horrible panic attacks. Have been on Zanax all these years, 2 mg. 3 times daily, the legal limit. Still have panic attacks, am very addicted to the Zanax because I don’t want those horrible feelings. I have them when I drive sometimes, and can’t ride with anyone… it’s terrible. Any suggestions please? Desparately need help!
Thank you.
Pam Benningfield
Mrs Benningfield,
As you probably read the article, the only way we can help you is by having an appointment with an homeopath to discuss your situation in lenght. Homeopathic prescribing cannot be done over the counter in this case. I strongly encourage you to seek this professionnal guidance.
Wonderful article on a much needed topic of Post Traumatic Stress Disorder in today’s frightening and dangerous world in war torn countries, broken dysfunctional and abusive families, natural disasters and shifts in the earth, shocks and accidents in our fast-paced societies. Many great stories and contributions by those who have commented here. Thanks so very much.
In gratitude, Debby
http://www.twitter.com/DebbyBruck
Dear doctor Edward shalts.
I read your piece about POST TRAUMATIC STRESS DISORDER,an excellent,informative and interesting read.Like any other disease PTSD has real causes that create a chemical imbalance.It is found that drug treatment such as antidepressents and tranquilisers appear to be less effective than homoeopathic treatment.Homoeo remedies such as IGNATIA followed by NATRUM-MUR.and bio remedy KALI.PHOS are found effective cure for psychic problems.However PSYCHO DYNAMIC and COGNITIVE BEHAVIORAL THERAPY have been found successful.Thank yoy,sir.
Thanks to the Executive director,HPATHY.COM and his team members for providing such useful health related information and promoting health service thru Homoeopathy.
Dear Dr. Shaltz, could you recommend a Homeopathic doctor in the San Diego, CA area, who has experience treating PTSD?
Thank you,
Cm
In Escondido CA: Bill Mann. http://www.williamgmann.com Phone: (760) 741-7875
You mentioned giving a patient a book, what s the name of that book please? My son is back from Afganistan and is suffering from PTSD and needs help . He lives in San Clemente ,CA and getting ready to go to training in N.C. The meds you mentioned seemed as if different ones were used according to symptoms- please direct the process to go by to direct him for help. Thank you for your info!
Dear Doctor Shultz
I am writing to you from Australia.
I suffer from complex PTSD.
IM URGENTLY SEEKING HELP.
I m sure its a long shot but would you know of any homeopaths that you could recommend in Brisbane ?
I have been under. The guidance if my teacher Dr Ursula Gehring for many years. She has done a beautiful jobbut due to our friendship uts been hard fir her to see my picture .
I would. Love to heal.
Kind regard.
Cheryl
Os if you have time could you please reply via my email address. Thank you.
Can you please provide a reference list for this article or indicate where I might find it?
Many thanks