Definition
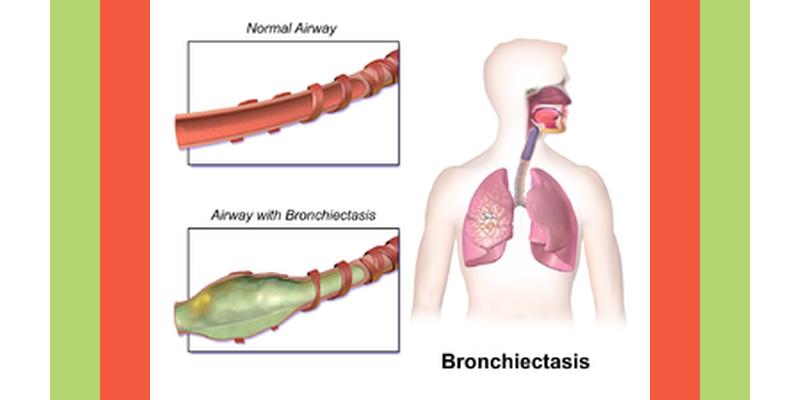
Bronchiectasis is localized irreversible dilatation of the bronchi. The disease runs a chronic course, characterized by repeated bronchial infection and haemoptysis.
Aetiopathogensis of bronchiectasis
| A. | Bronchial obstruction by | |
| • | Foreign body | |
| • | Tumour | |
| • | Stenosis | |
| • | Secretions | |
| • | Pressure from lymph nodes | |
| B. | Bronchial infection | |
| • | Childhood pneumonias in measles, whooping cough | |
| • | Pulmonary tuberculosis | |
| • | Bronchial asthma complicated by allergic bronchopulmonary aspergillosis | |
| • | Repeated chest infections of any type in immunodeficient persons | |
| C. | Miscellaneous | |
| • | Fibrocystic disease | |
| • | Kartagener’s syndrome | |
| • | Immotile cilia syndrome | |
PATHOLOGY
Bronchiectasis (Homeopathy Treatment for Bronchiectasis) commonly affects lower lobe bronchi, the left side being affected more frequently than the right. The right middle lobe and lingula are next in frequency of involvement. Upper lobe bronchiectasis is usually secondary to apical fibrotic tuberculosis.
Three morphological forms of bronchiectasis have been recognised, namely, cylindrical, fusiform, and saccular or cystic. In the cylindrical type, there is uniform dilatation of all the segmental and subsegmental bronchi. Bronchial dilatation in the fusiform variety is irregular with tapering of the lumen at either end. Cystic bronchiectasis is characterised by the presence of multiple cavities of bronchial origin which may resemble cavities produced by parenchymal destruction or alveolar dilatation. The bronchial epithelium may be ulcerated with prominent thin-walled capillaries in the submucosa which are responsible for frequent haemoptysis.
CLINICAL FEATURES
A typical patient is a young adult having a history of respiratory symptoms for several years. Symptoms may date back to a childhood exanthematous illness or whooping cough. The chief complaint is cough with copious purulent expectoration and this has a postural relationship. The sputum is frequently blood-tinged, and occasionally foul-smelling. Fever and other constitutional symptoms may occur during episodes of bronchial infection. Patients generally show evidence of chronic malnutrition and if the disease has been acquired in childhood, the growth and development of the child may be affected.
Some patients present with recurrent episodes of haemoptysis with almost asymptomatic periods in between (bronchiectasis sicca).
Haemoptysis may occasionally be very large and life-threatening. It results from erosion of abnormal bronchial artery-pulmonary artery communications which may develop in bronchiectasis.
Physical findings include evidence of malnutrition in long-standing cases, and digital clubbing. Examination of the chest reveals persistent coarse crepitations over a localised region of the lung, usually at the base. The affected side of the chest may be retracted, with wasting of the overlying muscles on account of associated pulmonary fibrosis (Homeopathy Treatment for Pulmonary Fibrosis). In the presence of large bronchiectatic cavities, bronchial breath sounds may be heard. Patients with extensive bilateral disease may have evidence of pulmonary hypertension, cor pulmonale and chronic airways obstruction. In some patients, particularly those with bronchiectasis sicca, there may be no positive finding on clinical examination.
DIAGNOSIS
A skiagram of the chest may show cystic lesions looking like a bunch of grapes, which are typical of cystic bronchiectasis. X-ray of the chest, however, may be entirely normal in patients with limited disease, particularly of the cylindrical variety. Only an area of pneumonitis may be seen and underlying bronchial abnormality may be invisible. Bronchography may be done to show cystic lesions.
CT scanning of the chest is now the preferred method for diagnosis. Since bronchiectasis is frequently produced by underlying bronchial obstruction (foreign body or adenoma), bronchoscopic examination is required.
Pulmonary function tests show a mixed pattern of restrictive and obstructive ventilatory dysfunction. Airway obstruction is produced as a result of retention of secretions and bronchial inflammation, whereas the restrictive changes are due to atelectasis and scarring of the lung parenchyma. Patients with extensive disease may develop severe respiratory failure. In a large majority of patients, however, only mild hypoxaemia is present.
MANAGEMENT
Bronchiectasis is largely a preventable disease. Prompt treatment of childhood respiratory infections reduces its incidence. Early and adequate management of foreign body inhalation or empyema should reduce the risk of subsequent bronchiectasis.
HOMOEOPATHIC MANAGEMENT
The selection of remedy is based upon the theory of individualization and symptom similarity. This is the only way through which a state of complete health can be regained by removing all the signs and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat bronchiectasis but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, many remedies are available to treat bronchiectasis that can be selected on the basis of symptoms, cause, sensations and modalities of the complaints.
Some pathology rubrics are:
- Complete dynamic 2015
Chest; emphysema, bronchiectasis:
absin acet-ac ACON agar agarin agav-t alco all-s alumn AM-C aml-n ANT-AR ANT-C ant-s ANT-T apom arg-n ARS ars-i astra-e aur BAC BALS-P bani-c bar-ar bar-c BELL benz-ac beryl blatta-a BROM bry cadm CALC calc-f CALC-P calc-s CAMPH CANTH CAPS CARB-V carbn-o carbn-s chel CHIN chin-ar CHLOL CHLOR chlorpr COCA CON CONV COP cortico crat crot-h CUPR CUPR-AR CUR DIG dinitrob DROS dulc EPHE-V eucal euon-a ferr-i glon grat GRIN hall hed helia HEP hist ichth impa-w iod IP just KALI-BI kali-c kali-i kreos kres lac-d LACH led leon lepro LOB LYC LYCPS malv marr med MERC merc-v morg myos myrt-c myrt-ch NAPHTIN NAT-M nit-ac nux-v op per PHEL PHOS plb pneu poly-a psor PULS queb sabal SANG sanguin-n saroth SARS SEC SENEG SEP SIL silphu SOL-N spong STANN stry stry-m SULO-AC SULPH tell ter thal THUJ tity-s TRIG-F-G tub tub-r VERAT
- Phatak Repertory
BRONCHIECTASIS, BRONCHORRHOEA (17)
1 all-s, 2 ars, 1 bac, 2 calc, 1 all-c, 1 cop, 1 eucal, 1 grin, 2 hep, 1 kali-bi, 1 kali-c, 2 lyc, 1 phel, 2 puls, 1 sil, 3 STANN, 1 tub
- Boericke Repertory
BRONCHIECTASIS, BRONCHORRHEA, DILATATION (23)
2 acet-ac, 2 all-s, 2 alumn, 2 ant-t, 2 benz-ac, 3 CALC, 2 eucal, 2 ferr-i, 2 grin, 3 HEP, 3 KALI-BI, 3 KALI-C, 2 kreos, 2 lyc, 2 myos, 3 PULS, 2 sang, 3 SIL, 3 STANN, 2 sulph, 2 tub, 3 BAC, 2 ichth
Here are some keynotes of a handful of remedies often indicated in bronchiectasis:
HEPAR SULPHURIS CALCAREUM: Hahnemann’s calcium sulphide. Locally, it has special affinity to the respiratory mucus membrane, producing croupous catarrhal inflammation, profuse secretion; also easy perspiration. In nose smell like old cheese. Hay-fever. (Hepar 1x will often start secretions and profuse drainage in stuffy colds.) Loses voice and coughs when exposed to dry, cold wind. Hoarseness, with loss of voice. Cough troublesome when walking. Dry, hoarse cough. Cough excited whenever any part of the body gets cold or uncovered, or from eating anything cold. Croup with loose, rattling cough; worse in morning. Choking cough. Rattling, croaking cough; suffocative attacks; has to rise up and bend head backwards. Anxious, wheezing, moist breathing, asthma worse in dry cold air; better in damp. Palpitation of heart.
CALCAREA CARBONICA-OSTREARUM.(Carbonate of Lime): Tickling cough troublesome at night, dry and free expectoration in morning; cough when playing piano, or by eating. Persistent, irritating cough from arsenical wall paper. (Clarke.) Extreme dyspnoea. Painless hoarseness; worse in the morning. Expectoration only during the day; thick, yellow, sour mucus. Bloody expectoration; with sour sensation in chest. Suffocating spells; tightness, burning and soreness in chest; worse going upstairs or slightest ascent, must sit down. Sharp pains in chest from before backwards. Chest very sensitive to touch, percussion, or pressure. Longing for fresh air. Scanty, salty expectoration. [Lyc.]
STANNUM: Debility is very marked when Stannum is the remedy, especially the debility of chronic bronchial and pulmonary conditions, characterized by profuse muco-purulent discharges upon tuberculosis basis. Much adhesive mucus, difficult to detach; efforts to detach cause nausea. Throat dry and stings. Hoarse; mucus expelled by forcible cough. Violent, dry cough in evening until midnight. Cough excited by laughing, singing, talking; worse lying on right side. During day, with copious green, sweetish, expectoration. Chest feels sore. Chest feels weak; can hardly talk. Influenzal cough from noon to midnight with scanty expectoration. Respiration short, oppressive; stitches in left side when breathing and lying on same side. Phthisis mucosa. Hectic fever. Much mucus in trachea. Expectoration; easy; quantities of sweets saltish sour putrid or bright yellow pus or ball of mucus. Short breath from every effort; must loosen clothes. Takes deep breath. Chest feels raw or hollow. Haemoptysis; with copious expectoration. Stitches; in left side of chest when breathing or lying side; knife like below left axilla. Catarrhal phthisis. Bronchiectasis. Retching with coughing. Can not walk can not do anything without coughing.
BACILLINUM: A Maceration of a Typical Tuberculous Lung Introduced by Dr. Burnett. Has been employed successfully in the treatment of tuberculosis; its good effects seen in the change of the sputum, which becomes decreased and more aerated and less purulent. Many forms of chronic non-tubercular disease are influenced favorably by Bacillinum, especially when bronchorrhoea and dyspnoea are present. Respiratory pyorrhoea. The patient expectorates less. Bacillinum is especially indicated for lungs of old people, with chronic catarrhal condition and enfeebled pulmonary circulation, attacks of suffocation at night with difficult cough. Suffucative catarrh. Tubercular meningitis. Favors falling off of tartar of teeth. Constant disposition to take cold. Oppression. Catarrhal dyspnoea. Humid asthma. Bubbling rales and muco-purulent expectoration. Note. This muco-purulent expectoration of bronchitic patients is equally poly-bacillary; it is a mixture of diverse species and hence Bacillinum is truly indicated. (Cartier.) Often relieves congestion of the lungs, thus paving way for other remedies in Tuberculosis.
LYCOPODIUM: Tickling cough. Dyspnoea. Tensive, constrictive, burning pain in chest. Cough worse going down hill. Cough deep, hollow. Expectorations gray, thick, bloody, purulent, salty. [Ars.; Phos.; Puls.] Night cough, tickling as from Sulphur fumes. Catarrh of the chest in infants, seems full of mucus rattling. Neglected pneumonia, with great dyspnoea, flaying of alae nasae and presence of mucus rales. Feeling of a hard body in oesophagus. A ball rises and sticks in throat. Sore throat; < cold drinks. Swellings and suppuration of tonsils. Chronic enlargement of the tonsils. Diphtheria-deposits spread from right to left. Food and drinks come through nose; on swallowing. Throat cold. As of a ball rose up in. Feeling of contraction provoking constant swallowing. Brown yellow spots on chest. Abscess of the lungs tuberculosis. Difficult respiration due to hydrothorax or/and hydropericardium with flapping of alae nasi. Feeling of tightness in chest with burning.
PULSATILLA: On account of its CHANGING; SHIFTING SYMPTOMS this remedy is known as a weather cock remedy. It affects the MINDS; VEINS; MUCOUS MEMBRANES; respiration and one side. THIRSTLESSNESS; CHILLINESS AND SHORTNESS OF BREATH; with digestive or menstrual disorders. Capricious hoarseness; comes and goes. Dry cough in evening and at night; must sit up in bed to get relief; and loose cough in the morning, with copious mucus expectoration. Pressure upon the chest and soreness. Great soreness of epigastrium. Urine emitted with cough. [Caust.] Pain as from ulcer in middle of chest. Expectoration bland, thick, bitter, greenish. Short breath, anxiety, and palpitation when lying on left side. [Phos.] Smothering sensation on lying down. Cough dry hacking from tickling in epigastrium. Chest oppressed; as by a load. Soreness or stitch beneath clavicles Hoarseness comes and goes. Asthma from suppressions. Cough after measles.
SILICEA: Colds fail to yield; sputum persistently mucopurulent and profuse. Slow recovery after pneumonia. Cough and sore throat, with expectoration of little granules like shot, which, when broken, smell very offensive. Cough with expectoration in day, bloody or purulent. Stitches in chest through to back. Violent cough when lying down, with thick, yellow lumpy expectoration; suppurative stage of expectoration. [Bals. Peru.]. Sycotic asthma. Cold fails to yield. Slow recovery form pneumonias. Rattling in chest. Stitches in chest through the back. Shortness of breath from manual labour; walking fast. Stone- cutter’s affections. Emphysema after pleurisy. Neglected pneumonia. Painless throbbing in sternum.
KALI BICHROMICUM: Potassium bichromate specially affects the MUCOUS MEMBRANES of the air passages; NOSE; pharynx stomach and duodenum-producing ADHESIVE; STICKY; STINGY; tough lumpy or thick discharges. Diseased conditions progress slowly but deeply; causing great weakness bordering on paralysis but little fever. Plastic or fibrous exudations spread downwards. It is adapted to fat fair fleshy light complexioned persons subject to catarrhs or with syphilitic or scrofulous history. As if a hair on tongue in nostrils etc.Catarrh of pharynx, larynx, bronchi and nose, and a tough, stringy, viscid secretion is produced, which condition is a very strong guiding symptom for this drug. Perforation of the septum. Voice hoarse; worse, evening. Metallic, hacking cough. Profuse, yellow expectoration, very glutinous and sticky, coming out in long, stringy, and very tenacious mass. Tickling in larynx. Catarrhal laryngitis cough has a brassy sound. True membranous croup, extending to larynx and nares. Cough, with pain in sternum, extending to shoulders; worse when undressing. Pain at bifurcation of trachea on coughing; from mid-sternum to back. Tickling in larynx with cough < eating with eructations > heat; then vertigo. Asthma < coition. Cough > expectoration. Dry metallic hacking cough.
KALI CARBONICUM: Cutting pain in chest; worse lying on right side. Hoarseness and loss of voice. Dry, hard cough about 3 am, with stitching pains and dryness of pharynx. Bronchitis, whole chest is very sensitive. Expectoration scanty and tenacious, but increasing in morning and after eating; aggravated right lower chest and lying on painful side. Hydrothorax. Leaning forward relieves chest symptoms. Expectoration must be swallowed; cheesy taste; copious, offensive, lump. Coldness of chest. Wheezing. Cough with relaxed uvula. Tendency to tuberculosis; constant cold taking; better in warm climate. Catarrhal aphonia; with violent sneezing. Breathing difficult asthmatic < least motion or walking; walking; alternating with diarrhoea; with vertigo. Incessant hard retching or choking futile cough; then vomiting. Whooping cough. Lungs seems to stick to the ribs. Stabbing chest pains.
ALLIUM SATIVA(Garlic): It is adapted to fleshy persons used to high living who suffer from dyspepsia and catarrhal affections.Constant rattling of mucus in bronchi. Cough in the morning after leaving bedroom, with mucus expectoration, which is tenacious and difficult to raise. Sensitive to cold air. Dilated bronchi, with fetid expectoration. Darting pain in chest. Cough when smoking. Bronchiectasis with foetid sputum. Haemoptysis.
REFERENCES:
- Medicine part:
- P.I. the text book of medicine, 8th edition
- Repertory Part:
- Complete dynamic 2015 by Dr Roger Van Zandvoort
- A Concinse Repertory of Homoeopathic Medicine By Dr. S. R. Phatak
- Clinical Repertory by Dr. Oscar E. Boericke
- Materia Medica
- BOERICKE William : [Pocket Manual of Homeopathic Materia Medica], New Dehli: Jain (1927)
- PHATAK S. R. : [Materia Medica of Homoeopathic medicines], New Delhli: Indish Book and Periodicals (1977)





All wrong medicines have been administrated here , The disease has Nosode symptoms , so Tuberculinum 1 M , is well suggested .
Are the guys here are real doctors who suggested the above medicines ?