Macular degeneration
Many homeopaths are reluctant to treat age related macular degeneration for several reasons. First, there is a poor understanding of the pathology and its affect on the visual system. Second is the belief that only a specialist should treat this serious disorder, and lastly is the belief this condition will not respond to homeopathy-it is an incurable state.
Since there is no effective allopathic treatment, why not try homeopathy? The homeopathic treatment of macular degeneration is a unique opportunity for homeopaths. I would like to share my experiences using homeopathy in the treatment of this disorder.
Definition of Age Related Macular Degeneration (ARMD)
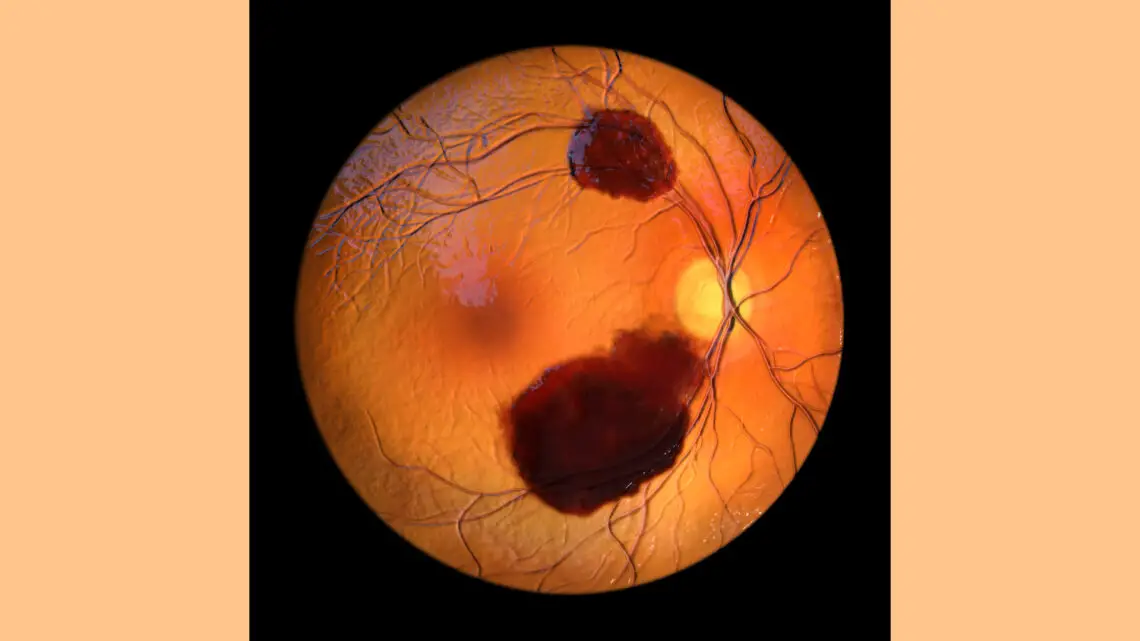
Macular degeneration (Homeopathy for Macular Dystrophy) is a pathological condition that occurs in the macular area of the retina. The macula is the area of the retina responsible for central vision or that which gives us the greatest detail in our sight. The pathological changes primarily occur in the choroid (the vascular layer of the eye which lies between the sclera and the retina) and pigmented retinal epithelium (PRE – the layer separates the choroid from the retina). These changes may lead to fluid accumulation, hemorrhage and scar tissue. Loss of central vision occurs, but this rarely produces total blindness because the peripheral vision is preserved. Macular degeneration affects thirteen million Americans. Most of them are over the age of sixty-five, but certain hereditary conditions may cause it to develop in younger individuals. Persons over the age of seventy-five have a thirty percent chance of developing it.
ARMD; it rarely affects anyone younger than fifty-five years old. Caucasians tend to develop it more than persons of pigmented skin, due to the fact they have less pigment in the retina, especially if they have blue, gray, or green eyes. It affects men and women equally. People who are nearsighted (myopic) have a greater chance of developing the condition as do people who work or spend a lot of time out of doors and are exposed to ultraviolet radiation from sunlight.
Symptoms of ARMD
When a patient has ARMD, vision in the center of the visual field gets fainter and fainter until finally there is hardly any way to see objects in the center of the visual field. The first thing most people will notice is a lessening of their sight as they look straight ahead at things, like the printed word, faces or clocks. This may be a dimming, a blurring, or actual “holes” or black spots in the vision. Extreme light sensitivity and poor night vision also precede ARMD in many cases. Light-to-dark adaptation, for example, the ability to find a seat in a movie theater, is also apt to be very slow.
Macular degeneration rarely leads to total blindness. Instead, worsening symptoms include a loss of central vision and a diminished ability to see things straight ahead. People with ARMD will rely more and more on peripheral vision. Sometimes, in the early stages, there are holes in the vision, called scotoma. These are areas where you cannot see anything. Most people with ARMD become unable to drive and are eventually declared legally blind.
Types of ARMD
There are two main types of macular degeneration, wet and dry.
The dry or areolar type consists of degeneration of the retinal pigment cells resulting in drusen (described below) and hyper and hypopigmented areas in the retina with loss of rods and cones and generalized atrophy (Homeopathy for Optic Atrophy). Dry ARMD, which affects ninety percent of persons with ARMD, results from a buildup of cellular waste product called drusen, in the back part of the inner eyeball where the retina and macula are. Drusen is from the German word druse meaning bump or gland. It refers to the earliest changes that are observed in ARMD. A drusen or bump develops on Bruch’s membrane. This occurs when the retinal pigment epithelium becomes overloaded with undigested discs from the cones. This material collects on Bruch’s membrane producing thickened areas.
The wet type or exudative type presents as vascular leakage with exudates and a detachment of the retina with loss of vision. In addition when the retinal pigment epithelium becomes overloaded, the RPE cells begin to degenerate. Debris begins to accumulate at the base of these cells. These cells lose their attachment to Bruch’s membrane and fluid begins to accumulate under the cells. Soon there are breaks in Bruch’s membrane leading to growth and leakage of blood vessels from the choroid. This leakage and new blood vessel growth into the retina lead to the wet stage of macular degeneration. A small percentage of these cases can be treated successfully with the argon laser. There is another type of wet macular degeneration that occurs in people who are diabetic. This results from leakage of small blood vessels, which leads to fluid accumulation under the retina and loss of central vision.
Summary of the types of macular degeneration
– Dry Stage of Macular Degeneration
– Development of Drusen
– Degeneration of Retinal Pigment Epithelial Cells
– Wet stage of Macular Degeneration
– Breaks in Bruch’s Membrane Leading to Growth and Leakage of Blood Vessels
– Absorption of Blood with the Development of Scar Tissue
Traditional treatment
There have been many studies that have shown that the antioxidants, Vitamins A, C, E, Zinc and Selenium can retard the progression of this disorder. One of the treatments for wet ARMD uses laser surgery to cauterize the leaky blood vessels. This measure may preserve more vision in the long run, but usually results in worse vision in the short run because healthy tissue is almost always destroyed along with the diseased vessels. Laser treatments are only indicated for the wet type of degeneration and in fact only a small percentage of patients with the wet type will actually qualify for laser treatment.
Homeopathic approach
Macular degeneration can be treated homeopathically just like any other disease state of the body. The constitutional approach works best, the goal being to find the remedy for the totality of the case. When the remedy is not clear or the patient is not willing to undergo constitutional treatment, a more lesional approach can be used.
Rubrics for Macular degeneration:
INFLAMMATION – Choroid
EYE – INFLAMMATION – Chorio-retinitis
EYE – ATROPHY – CHORIOD, Atrophic spots
EYE – INFLAMMATION – Retina – pigmented
EYE – INFLAMMATION – Retina – punctata albescens
EYE – INFLAMMATION – Retina – syphilitic
EYE – INFLAMMATION – Retina
VISION – DIM VISION – FOGGY
VISION – LOSS OF VISION – vanishing of sight
VISION – LOSS OF VISION – colors, for
VISION – SCOTOMA VISION – SCOTOMA – central
Constitutional approach
Miasms
I first try to uncover the miasm stages in these cases to limit the remedies under consideration. The exudative type of degeneration represents the sycotic miasma. The dry or atrophic type of macular degeneration more commonly represents the syphilitic miasm. Psoric Stage – This is the earliest presentation with minimal pigmentary changes and a loss of the foveal light reflex. The foveal light reflex is produced when healthy cones reflect the light, which enters the eye. As the cells become weakened with age and disease, they loose this ability to reflect light. Sycotic Stage -There is a hyperproliferation of tissue in the macular area. This can manifest as excessive pigment which has the appearance of dark pepper like specks in the macular area. Another presentation can be that of drusen. These drusen cause a weakening of the retina and can lead to death of the photoreceptive cells. This weakness can also cause tiny blood vessels to grow into the retina. These vessels can leak fluid or bleed and cause a sudden loss of vision (wet macular degeneration). Syphilitic Stage – There is more destruction of tissue with atrophy and destruction of the retina.
Description of lesion
Characteristics of the macula can be very useful in remedy differentiation. Is the lesion wet or dry? Is there hyperpigmentation or hypopigmentation? What color is the exudate? Yellow, white, or orange? Is there blood present? What color is the blood? As an ophthalmologist I have the unique ability to observe the changes inside the eye and to use these physical findings to help select the remedy, but you can ask the patient to bring in retinal photos of the macular degeneration so you can study these characteristic features. I often will look at the Skin and Generalities sections as well. Some rubrics that I have found to be helpful in treating macular degeneration are:
SKIN – CICATRICES
SKIN – DISCOLORATION
SKIN – EXCRESCENCES
SKIN – ERUPTIONS
SKIN – FRECKLES
SKIN – INFLAMMATION
SKIN – WARTS
GENERALS – ARTERIOSCLEROSIS
GENERALS – ATROPHY
GENERALS – HEMORRHAGE
GENERALS – INDURATIONS
GENERALS – INFLAMMATION
GENERALS – STASIS of the venous system
GENERALS – TUMORS
Remedies that have an affinity to the eye
Retinal Atrophy
Carboneum sulphuratum
Cina maritima
Haliaeetus leucocephalus
Kalium chloricum
Phosphorous
Santoninum
Sanicula
Tabacum
Vanadium
Choroidal Atrophy
Cina maritima
Kalium chloricum
Kali iodatum
Santoninum
Veratrum viride
Lesional approach
Some prescribers have had experience with a more lesional approach to this disease. I use this approach when the patient is not interested in undergoing constitutional treatment.
Tissue salts
Tissue salts can also be useful in the treatment of macular degeneration. The following salts have been helpful in the treatment of ARMD:
Calc flourica 8X – The tissue strengthener.
Calc phosphorica 6X – The cell builder.
Kali phosphorica 6X – Nerve nutrient.
Natrum muriaticum 6X – The fluid distributor. Dryness or excessive moisture in any parts of the body. Can be helpful in cases of wet macular degeneration.
Carboneum sulphuratum – Andrew Lange, ND, has reported success in early macular degeneration using Carboneum sulphuratum. He uses 30C everyday and has seen resolution of drusen and pigmentary changes.
Secale – Dr. Johann A. Miller has had good success with Secale in the treatment of macular degeneration. Secale is used in low potency when the patients have some general signs compatible with Secale such as, being worse from heat and better from cold.
Sanicula and Vanadium – Dr. A. U. Ramakrishnan has used Sanicula in cases of macular degeneration with the symptom of wavy vision. He has also used Vanadium 200C every month for the treatment of macular degeneration.
Sarcode – Human retina 5C: Max Tetau has reported the affects of 5C, 7C and 9C sarcodes on the tissue that was prepared. 5C Stimulates activity of the tissue from which it was derived. 7C normalizes tissue activity and 9C suppresses tissue activity.
Human retina 5C has been used with some success in stimulating the activity of the failing macula.
Case 1
DS 76 year old female
Prominent look of suffering on her face during the interview.
Recent episode of a hypertensive crisis with a reading of 220/146, she is very anxious about getting her vision back and has had over ten laser treatments in both eyes. She is worried about the future and what will happen. She needs more information. She needs the information so she can do whatever will help her. She has to be sold on this approach; she is a skeptical person.
She sleeps with the light on all night. She was robbed as a child and has a fear of robbers. She is afraid that a man will come up through a trap door. Her parents’ home was large with fourteen rooms. She and her sister would take turns staying up at night. She has a fear that someone is in the room. She is on guard all the time. She sleeps facing the door on her left side. She also has a gun; a small ladies gun which is loaded. She will sleep for a couple of hours and then wake at 2:00 to 3:00 AM. The fears are worse when she is alone. She stayed up all night when her husband was in the hospital. She could solve this problem if she had a dog. The dog would be on guard instead of her.
Physical exam 5/100 right eye, 5/10 left eye Cataracts Central scarring in right eye from laser treatment Retinal pigmentary changes with large drusen (Tumors/Warts) in left eye
Diagnosis: ARMD Cataracts Hypertension Anxiety
Rubrics
FACE – EXPRESSION – suffering
MIND – FEAR – alone, of being
MIND – ANXIETY – health; about – own health; her/his
MIND – ANXIETY – night
GENERALS – TUMORS
She escapes by reading books about the simple life. Small town, a quite place, the neighbors visiting each other. She likes the feel of soft clothes. Desires creature comforts. She wants a simple dog, a dog to stay on guard at night. There are many aspects of Calcarea carbonica in her story with issues of security in the home, enjoying the simple pleasures of life. There is also the fear and anxiety element of Arsenicum album.
Plan: Calcarea arsenicosum LM1
Follow up one year later: It took her 2 months before she started the remedy because she had a strong fears of an aggravation. She feels good. Lots of energy. She can relax easily. She has a lot more energy in her business. She is getting a lot of compliments on her skin since taking the medication. Her fears are greatly improved. She does not have the fear of being robbed. Her fears at night have greatly improved. Happier and more relaxed. Her vision has improved two lines on the chart. Physical Exam: 5/100 in the right eye, 5/10 in the left eye.
Case 2
RR 78 year old female
Chief complaint is macular degeneration, cataracts and a balance problem.
She has noticed her vision decreasing since her last eye exam when she was told that she had macular degeneration and cataracts. Vision is very dim and she has trouble reading. The vertigo comes on suddenly and she then goes down like a rock. Room spins from left to right. She is debilitated. She is like a quivering old lady. She is so weak that her arms and legs shake. Twice it happened at 7:00AM when she woke up from bed. She pulled herself up with great effort. She lives in fear that this attack will come back again when she is under stress. She works as a real estate broker. When she is in a stressful conversation she can feel her balance leave her. She feels that the bottom is dropping out of her stomach and she experiences light-headedness. She has also developed ringing in her ears associated with the vertigo.
An important aspect of her life was ballroom dancing which she did with great dedication. She is very depressed because now she can’t compete. She feels hopeless and withdrawn. Her sexual drive was never very high and she is not in a relationship. She states there is a lot of sexuality in dancing. She enjoys the provocative aspects of the Latin dancing.
Physical exam: 20/300 right eye, 3/100 left eye. Advanced cataracts in both eyes. Myopic degeneration with atrophic changes in her retina.
Diagnosis: ARMD, Vertigo, Cataracts.
Rubrics
EYE – CATARACT
VERTIGO – ACCOMPANIED by – staggering
VERTIGO – SUDDEN
EAR – NOISES in – ringing
MIND – DANCING
FEMALE GENITALIA/SEX – SEXUAL DESIRE – diminished
According to A. B. Norton in his article “The Homeopathic Treatment of Incipient Senile Cataract, with Tabulated Results of One Hundred Cases“, Sepia is the number one remedy to think of in females with advanced cataracts.
Plan: Sepia LM1
Eight month follow up: She can read the menu. She’s had a seventy percent improvement in her vision. Street signs are becoming clearer – colors are vivid. No more dizziness – stronger and confident walking. No more ringing in her ears. PE – vision is now 20/200 OU.
Case 3
EA 78 year old female
Two years ago, she developed cloudy vision in the left eye where her vision became very dim and letters began to run together while she was reading. One of the biggest difficulties in her life has been her relationship with her daughter. “She has cut me off from the family. She will not return my letters and she will hang up the phone when I call. It is such a big disappointment in my life.” “She has told lies about my husband and I. You know mother, you are a slob. I wanted to cry but I could not cry. How could she be so hurtful? We could go for hours not talking to each other.
My daughter would not appreciate anything that I did. I wanted to tell them to ‘go to hell’ but I did not because I did not want to exacerbate it.” “I blow and get angry very quickly. Sometimes a silly little thing will irritate me. I was eating my salad and they brought out the main course. It was cold and I became extremely upset.”
Physical exam: Retinal pigment atrophy in the left eye. Vision 10/10 right, 1/70 left eye
Diagnosis: ARMD Hypertension
Rubrics
MIND – CONTRADICTION – intolerant of contradiction
MIND – ANGER – trifles; at
MIND – ANGER – violent
CHEST – PALPITATION of heart – anger
VISION – RUN together – letters
Plan: Staphysagria LM1
Seven month follow up: Peripheral vision is better on left eye – the right she has noticed an overall improvement. Colors are much brighter, she has a dress that she thought was gray and now it looks lavender! She is not getting angry as easily or as often. She called her daughter and asked her if she wanted to meet her-she said yes. It was a good meeting, at the end she said that they had wasted three years. Vision has improved three lines in the left eye: 10/10 in the right eye 1/40 in the left eye Homeopaths should not view macular degeneration as an incurable disease. I hope that all homeopaths will welcome the opportunity to help people who are suffering from the effects of macular degeneration. Do not tell them what so many eye doctors have told them: “Nothing can be done.” Homeopathy can help, so begin to look for the simillimum that will improve their vision and their life.
———————————————-
Dr. Edward Kondrot, MD(H),CCH, a board certified opthalmologist, is recognized as a pioneer in the use of homeopathy for eye conditions and is director of the Healing the Eye and Wellness Center in Arizona. He is author of “Healing the Eye the Natural Way: Alternative Medicine and Macular Degneration” , “Microcurrent Stimulation: Miracle Eye Cure”, and Homeopathy and Eye Disease (Audio Tape).
Visit him at his website at http://www. homeopathiceye.com



Dr. Kondrot , I am an internist practicing internal and integrative medicine in costa rica and have an 80 yeat pacient with we macular degeneration and bleeding and inflamation of the optic nerve. What suggestions of homeopathic meds do you have . Thank you very much
Edward, I find what you wrote fascinating. I believe my own experience with macular degeneration occurred as a result of cooking with all the seed oils (canola, vegetable, etc.) – I have read a lot about this and it made sense to me as my family believed it was healthier. Needless to say, we all suffer now from this. *Before my eyesight was fantastic!!
Would you say that homeopathy would still help in this case? Even if MD was the result of using the heated veggie cooking oils? There is a lot of research about how these oils when heated actually affected millions of people in this way (started in the 80’s).
Your comments appreciated. Thank you!
Robin,
Where di d you find out about the seed oils causing problems at? I would love to read more about that.
Thank you
My clinical confirms the observations of Robin { see comments posted above} }
I hope, for the askers’ sake, that the questions have been answered. I would really love to see more discussion about this particular subject here (even in the shape of comments), so that I could perhaps find some help myself. You see, I live in a country where there are no reliable homeopaths at hand and even homeopathic remedies are not sold (except for the odd combo “remedy” which I would not use, of course).
I have had astigmatism and myopia since early adolescence. (I’ve been using contact lenses all this time).
Recently my right eye has started to deteriorate rapidly. Judging by the symptoms, I would say it looks like macular degeneration, even though I am not “old” (I am fifty.) I have no other “conditions” that I know of. I don’t even get colds. But I do believe I have congenital connective tissue debility.
The thought of vision loss is very distressing, and I would love to hear some suggestions, so that – in absence of a homeopath – I could thoroughly study the homeopathic options available myself. I am not exactly a beginner in homeopathy (self-taught, of course), and I have read all of Hahnemann’s texts plus many others, but I would love to hear some suggestions from a person who has actual experience with homeopathy and eyesight.
Hello Mariwb,
I am 48 years and just found out after extensive testing by Retina Specialist Dr. WALD M.D. of New York EYE and EAR. Very depressing. I see swiggly lines and have darkening central vision in my right eye. Left eye also has many Drusen but in peripheral vision area. Have you found anything from your research that can help me. Kindly share.
You are absolutely right Mr Mariwb,I too will appreciate the comments of some one who had macular degeneration is cured with homeopathy. I have this problem in my left eye last more than 20 years I am 71 now.My doctor who is my nearest relative as well confirm that till today there no any kind of treatment for this ailment.
Dear sir thanks for that.I get injury when i was traveling in train… one stone heated from out side that stone cover eyebrow and maxilla, now problem is macular hole, told by doctor my age 27 only. ñow left eye6/6 and right eye 6/24. i am afraid of operation. please suggest to me homeopathic treatment.
I am detected with macular degeneration. I stay in Kolkata, India. How can i get in touch with Dr. Edward Kondrot? Please help!
my relative is 4.5yrs old he is suffering from macular digeration eye deases so please give me some suggestion so that he could be treated and could see everything and could go to school
hello,
i am suffering from low vision due to macular dystrophy since 14 years. now i am 20. can anybody suggest what to do? any remedies pls?
Dear sir
I have been detected wet amd since last three months. Allopathic doctors have suggested operation . Please help
SK Singhal
I am suffering from low vision due to macular dystrophy since now I am 42. can anybody suggest what to do? any remedies pls?
very impressive article ,want to how can i contact or reach dr. kondrot
,i am in medical practice and use homeopathy for certain conditions.
Dear Dr.Kondrot,
Am 74,and a patient of hypertension,which is under control,anfd have been diagnosed as suffering from Macular Degeneration,early stages…Luckily as soon as I noticed wavy vission I approached my Opthalmologist who immediately referred me to a Retinologist,who afte conducting a few tests diagnosed my condition as Macular Degeneration,and gave me AVASTIN Injection,at intervals of 4 weeks…I have just taken the 4th injection…but so far the improvement has been only slight/marginal…
What homeopathic Treatment would you advise me to follow ?
Dear Mr Yogesh Lajmi,
My father, 86 yrs, has been diagnosed with Age Related Macular Degeneration (ARMD). He has taken two injections of Avastin, but improvement is marginal. Can you please share your experience with homeopathic treatment and the medicines prescribed.
Thank you
Rakesh Kapoor
Dear Doctor
My son aged 23 has developed macular dystrophy, alopathic doctors have given up any treatment. I am a national of Nepal. I need your advice and help. Please do me favor so my son may get better.
Dear Andy,
I have sent you an email with contact information for a homeopath in Nepal. He may be able to help you find a homeopath near you in Nepal. I hope you and your son find the help you need.
Sincerely
Alan V. Schmukler
Editor
Hello, Alan,
Any referrals for a good practitioner to deal with macular degeneration in New York City area?
Thank you.
Dear Sir,
I am 53. I have been suffering from ARMD for 3 years. I have been under a retina specialist. He says there are RPE changes in both eyes. Recently, I have developed a complication: When I see an object above 10 feet I see it bent 40 degrees to right . I notice letter jump to above line. A homeo practitioner has given me calcaria fluor to take 4 tabs a day. I have started taking it. Can I expect any recovery?
RAma Krishna
Hello Rama,
Did the Homeopathy tablets work? Any other treatment works?
Hello,
I am facing Heredomacular Degeneration, My age 28 years old
few week back I know the disease
and Doctor say it is not Genetic disease
any kind of treatment for this disease in Homeopatic or other
please guide me
Thank you
My wife is 43 years old and has been detected with AMD.
She has started seeing distortion of straight lines. She is a resident of Kolkata , India.
What is the suggested homeopathic treatment for this.
Can you pls suggest. We are in great tension.
What about a macular cyst? You haven’t mentioned a remedy for that?!
Hello,
I have noticed the wavy vision in my left eye along with some black spots in retina.
may age is 33years.
can you please suggest me the medicines?
I am detected with macular degeneration. I stay in Dhaka, Bangladesh. How can i get in touch with Dr. Edward Kondrot? Please help!
My wife is 40 years old . After the cataract surgery we found the vision is not proper . After diagnose doctor told that is resolved CSR . Some little scars are also there and thinning of retina too . Now the vision is 6/9 with glasses. But some time blurred .. can it be cured or can we stop the further lose. How can I get touch with DR. EDWARD KONDROT. SUGGEST SOME HOMEOPATHIC MEDICINE
Dear Sir,
My daughter aged 26 has been suffering from Macular Distrophy. How can I contact the doctor for Homoeopathic treatment? Please help me.
Thank You,
Dr. A. H. Baqui
Sir i have heredomacular degeneration problem iam finished B.f.sc degree nxt i want to do master but reading of book is very difficult.i gone 5/6hospital this is birth probem there is no solution in Karnataka. India at to do sir help me
Dr. Kondrot, I am a 70+ year old man from Kolkata, India.
In early November 2015 I noticed central vision problem on both eyes. Searching the internet I found that my problem exactly matched the phenomenon of AMD described and illustrated in
Wikipedia ( https://en.wikipedia.org/wiki/Macular_degeneration#Age-related).
Immediately, I got my eyes examined at a leading eye hospital of my city. I was diagnosed to be in an early stage of Macular RPE. I was advised to get an angiography of eyes done, which I did not do.
In May 2016 I discovered this post of yours. I selected Calc fluorica 6X, Calc phosphorica 6x, Kali phosphorica 6X and Natrum muriaticum 6X and started taking these regularly ( 4 tablets of each 4 times a day). I have got positive results of this medication – the problem of central blurred vision is no longer there.
Now my question: how long should I continue to take these medicines and how should the dosage be adjusted?
Hi, how you doing now with your problem ? I am really curious to know your results
The cell salts, bio chemic medicines may have to be taken regularly. It is not like homeopathic remedy, which have to be stopped after the result is achieved. Please consult experienced homeopath in your area. Kolkata is known for best homeopaths.
You may contact Bharat Sevashram Sangh, originally known as Hindu Milan Mandir institution. Many monks are from Bengal and they will greatly help you.
If you come across any one among them, please inform me. We can pass on information to other patients for benefit, which is generally not available as permanent cure, allopathy is very costly treatment for eyes also.
HI Dipankor
Are the following homoeo medicines available in India:
Calc fluorica 6X, Calc phosphorica 6x, Kali phosphorica 6X and Natrum muriaticum 6X.
If so I shall also try for myself taking these regularly.
Thanks
RAVIKUMAR
Hello, I am Sujoy Dasgupta aged 83 years having dry macular degeneration for 2 years. I am taking I Site AF capsules . I read your letter few weeks back and have started taking bio chemic medicines . I would be grateful if you kindly inform after how many days you started getting results and whether this treatment is to be continued lifelong for the eyes. your answer to my query will be highly appreciated. thank you.
Hello Dr. Edward Kondrot / Alan V. Schmukler,
I’m aged 38, Male from Chennai, India diagnosed with retinal dystrophy in both the eyes. I humbly requesting to give me details to contact Dr. Edward on this or would suggest me a good homeopathic in my city in and around. Thanks.
Hi, I have a 12 year old son who has a drusen in both optic nerves and would like to proceed with homeopathy, would you have any suggestions on a doctor near Toronto? Or how can I get in touch with you?
My left eye has been diagnosed as IPCV(idiopathic polypoidal choroidal vasculopathy.Is there any homeopathic remedy ?please advice me.
I have now diagnosed with retinal scar following the retinal bleeding took place in the month of june,2017 which was earlier diagnosed ss IPCV.May I get homeopathic remedy for retinal scar.
what does the cherry red spot signifies?
i am 40 year old. in 2011 i got injury in left eye by plastic pellet filled with liquid during training. my central vision is completely lost. i can only get apparent blurry picture from left eye. i spot blind spot in left eye. my right eye is good . is any remedy in homeopathy. pls help
with regard
There has been some queries about Dr. Edward Kondrot’s contact. I am pleased to give it: [email protected]
Since I also have macular degeneration related edema, I am taking “accentrix” injections in ere at an interval of 3 months.
I am trying to find homeopathetic medicine for treating “RETINAL DRUSEN”, any information on the subject will be useful. email me.
Dear Sir
I am 47 years old IT Manager. I have center vision loss in my left eye. I have had 3 injection in my eye (Evastin) but no considerable improvement. having problem in my right eye. vision is decreasing now but center vision is ok.
I had tests like FFA and OCT. Doctors say that there is leakage in vein due to which this had happened. Doctor said it is not AMD.
Is there any homeopathic medicine for this problem.
Waiting for any useful response please
Muhammad Nasim Akhtar Siddiqui
i have same situation and doing same job as we user computer and mobile all the times we need to get rid of this problem, please let me know if you have got any helpful treatment other than injection. My email id [email protected]
my father is above 85years ,he is not able to see the frontal view and has very less peripheral view because of scars . is there any kind of treatment?
Do you have any suggestions for retinal pucker? I cannot find any remedies for that condition.
Thanks
My mother is 84 yrs old..She has ARMD Dry… Is there any homeopathic medicine available for this? She also has BP, Diabetes and low heart rate. Pls advise.
My retina burn with q switch laser and mocular scar come
I suffer severe vision loss due to Macular Degeneration. I have finished the 10 day course with Ruta 6 for 10 days bur not much help. Please advise what I should do next.
I am 83 and suffering from dry armd. Shall be grateful if you inform that how long to continue treatment as suggested by you.