The condition called mesial temporal sclerosis is closely related to temporal lobe epilepsy, a type of partial (focal) epilepsy in which the seizure initiation point can be identified within the temporal lobe of the brain. Mesial temporal sclerosis is the loss of neurons and scarring of the deepest portion of the temporal lobe and is associated with certain brain injuries. In this patient it was a left sided temporal sclerosis.
Brain damage from traumatic injury, infection, a brain tumor, a lack of oxygen to the brain, or uncontrolled seizures is thought to cause the scar tissue to form, particularly in the hippocampus, a region of the temporal lobe. The region begins to atrophy; neurons die and scar tissue forms. This damage is thought to be a significant cause of temporal lobe epilepsy. In fact, 70 percent of temporal lobe epilepsy patients have some degree of mesial temporal sclerosis. It also appears that the mesial temporal sclerosis can be worsened by additional seizures.
POSSIBLE CAUSES
- Aging
- Although the hippocampal sclerosis is commonly found among elderly people (≈10% of individuals over the age of 85 years), association between this disease and ageing remains unknown.
VASCULAR RISK FACTORS
There were also observations that hippocampal sclerosis was associated with vascular risk factors. Hippocampal sclerosis cases were more likely than Alzheimer’s disease to have had a history of stroke or hypertension, (evidence of small vessel disease) but less likely to have had diabetes mellitus.
SYMPTOMS
Mesial temporal sclerosis usually results in partial (focal) epilepsy. This seizure disorder can cause a variety of symptoms such as strange sensations, changes in behaviour or emotions, muscle spasms, or convulsions and memory loss. The seizures usually are localized in the brain, but they may spread to become generalized seizures, which involve the entire brain and may cause a sudden loss of awareness or consciousness. Apart from the chronic nature of epilepsy, hippocampal sclerosis was shown to have an important role in internal cardiac autonomic dysfunction. Patients with left hippocampal sclerosis had more severe parasympathetic dysfunction as compared with those with right hippocampal sclerosis. In young individuals, it is commonly recognized as Mesial temporal sclerosis with Temporal Lobe Epilepsy (TLE). On the other hand, it is an often unrecognized cause of cognitive decline, typically presenting with severe memory loss.
DIAGNOSIS
The changes associated with mesial temporal sclerosis are usually identifiable on a magnetic resonance imaging (MRI) scan.
THERAPY BY THE ALLOPATHIC SCHOOL
-ANTI EPILEPTIC DRUGS
-SURGERY-The assessment of the extent of mesial temporal sclerosis is important because it can be a good indicator of the outcome for patients undergoing temporal lobectomy to control seizures. For this procedure, the part of the brain containing the point at which the seizures start is removed.
Case Report: A 38 yr old male who was overweight had been seeing me for the past 10 years off and on for his health issues, mainly ureteric calculi, and pain in the renal region, at times left and other times right. Had been excreting calculi from the urinary tract until one year ago. For the past year he has been healthy otherwise. He has been in the habit of chewing gutka, (tobacco product) and paan masala (contains Betel leaf) for the past 6-8 yrs and also takes alcohol daily, for the past 3-4 years. He eats rich food and is a non vegetarian. He gets no exercise and has a fatty liver.
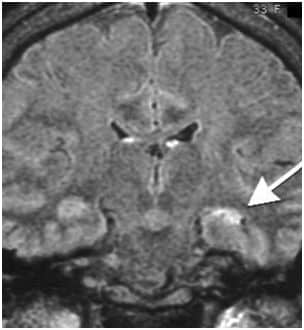
On 15th July 2014, it was a hot summer day, and at noon he was riding his bike when he experienced some abnormal sensation of fluttering in the left side of his chest. He immediately stopped his bike and stood up. He went on having the sensation for about 2-5 minutes and then it subsided , only to reoccur every 20- 30 minutes. He was rushed the same night to a nearby hospital for fear of a heart attack and was admitted for observation for the night to look for any cardiac cause. The next day he was discharged from the hospital and told that the ECG was normal and his symptoms were not related to cardiac cause. After paying the bill of 15000/- Rs he went back home only to realise now that he also had a slur in his speech for those 2- 5 minutes when the abnormal sensations in his chest were experienced. He subsequently consulted a neurology specialist in the town. The neurophysician ordered an MRI which revealed that there was scar/atrophic tissue/dead neuronal tissue, in the deepest part of the left temporal lobe/hippocampus.
The area where the arrow points is the scarring of the neuronal tissue
MRI Report On 17th July 2014 after which antiepileptics were given.
The neurophysician prescribed anti epileptic drugs. For about 6 days the patient took those drugs only to realise that there was no reduction in those uncomfortable symptoms, and now some new symptoms had also come up. He came to me on the 22nd of July 2014 and I asked him to explain in detail what he exactly felt in those 2 -5 minutes.
This is what he said: –“While in this episode I started to shiver with a feeling of coldness and almost shuddering of only the left side of the body. The hair on my left arm stands up (piloerection), and then a wave like sensation of fluttering originating from left side of chest and moving both up and down on left lower limb and left upper limb and towards the face, also left sided and lacrimation from left eye, and during this time I get that slurred speech if I try to speak. After about 2 to 5 minutes these sensations/episode passes off on its own, only to return aft 20 minutes. During this period, I have a feeling of anxiety and fear also.
During this time the feeling of coldness is so great that I have to cover the left side of my body with a blanket, even though it is the heat of summer, and the right side I leave uncovered. But I am not even able to use the fan, because if I do so, this episode comes earlier than 20 minutes. I used to take alcohol and tobacco products daily but since the day this has started to occur, I have stopped taking them. Also since I am taking these anti-epileptic drugs, that neurologist has given me, now even if a dog barks, I get startled and fearful. I don’t want to hear the sound of T.V. I feel sleepy and miserable after these drugs. My family and I are in great distress, since I have been told by the neurologist that I am not supposed to drive, since I may black out and fall from a scooter or my car may meet an accident under the influence of these anti epileptics drugs.
I told him not to worry and to stop those antiepileptics right away. I started to analyse the case to pick out the characteristic totality which would form the basis of my prescription.
- Chilliness on left side of the body
- Wave-like sensation which travels upwards and downwards to the left upper and lower limbs from the chest.
- Slurring of speech
- Fearful and anxious
- Lacrimation left eye during the episode.
- Now also lethargic and dull after 6 days of anti-epileptic therapy.
Now the perfect match must be found
Gelsemium is the perfect match (coldness, shivering, wave like sensation which travels up and down, slurring of speech, dull and lethargic). It just fit every bit of the puzzle.
Now a dose of Gelsemium 200 was given, and the patient was asked to wait in my clinic. After about 40 minutes he got that conglomeration of signs and symptoms again, so the 1st improvement noticed was the time lag, instead of 20 minutes, it came aft 40 minutes. With no further repetition, I sent him away with placebo for 2 days. Aft 2 days he came back and said, “Now the gap in between the episodes has increased, and also the intensity of symptoms is much less. I don’t feel that fearful now, the piloerection also comes in a mild manner, the chilliness is there, but less, the slurring speech is also there but less.”
Certainly the medicine had worked but the patient was still suffering, so now I decided to use the LM scale of potencies. Gelsemium LM2 was given twice a day, and on the 4th day he said- “I was feeling a lot better, the whole episode has almost vanished; there are no such symptoms of chilliness, wave etc, but now since the last dose I feel more lethargic and dull and tired , even though I felt better earlier.”
He was again put on placebo, and he went on improving steadily till November 2014. In Nov 2014, there was a change of symptom picture. He now complained of a headache whenever he woke up from sleep, on the left side of the head, dull aching and it would go off after about 1-2 hrs. The peculiarity was that he would get this left sided headache even after he woke up from an afternoon nap.
Now his symptoms were demanding another perfect match/simillimum. It was Lachesis. Lachesis LM2 was given twice a day for 4 days, after which he reported complete relief of the headache.
As of Jan 2015 he has got his job back and the last MRI done to see the vascularity of his brain was normal. There is no blood flow obstruction, but the plain MRI still shows that atrophic scar in the deepest part of left temporal lobe. All the symptoms have gone, and health is restored.
What is to be learnt here?
A simple medicine can initiate cure even of a complicated disorder. Miasm consideration is not necessary, when the totality is characteristic and speaks for the remedy. Remove from your own thinking disease/remedy relations, like for viral/ seasonal flus, Gels, Ars, Acon, or for joint pains, Rhus tox, Bry etc. Who knew that reversal of neuronal damage manifestations could be initiated by Yellow Jasmine? Even a homoeopath can bungle a case if totality is not considered (or if miasm is considered in lieu of totality). Atrophy/scar in brain remains but the symptoms vanish.
Homoeopathy is the science of symptoms. If you can rationally think and catch the symptoms, you catch the remedy. If you neglect that approach, you can lose the match!






Your selection of medicine is very accurate. Gelsemium and Lachesis are wonderful drugs
Dr. Aparna Singh
It is a nice case well presented. However I want to ask you from which source book did you get the information on Gelsemium. Checked Clarks Dictionary of Practical Materia Medica and could not find much. As well as Murpheys Materia Medica.
Hi Madam,
my daughter(7 year old) was diagnosed that she as F/S/O Left mesial temporal sclerosis.
Please suggest us medicines which can cure it.
Hi mam, my son 13 yrs old boy. I took MRI and test mentioned as follows “features are suggestive of right mesial temporal sclerosis”
Can u guide me. He is not speaking.
Hello mam,
My wife is 33 yr. Old. On 16.04.17, she reported acute pain in lower left abdominal region and than fainted with biting of lips etc. Seizures. MRI Scan suggest MTS, EEG is normal.
Pl suggest.
Please give me your contact details for your medical advice