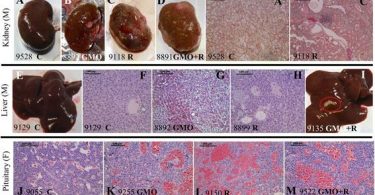
FURUNCLE (BOIL)
A furuncle is an infection of the pilosebaceous unit, therefore is more extensive than a folliculitis because the infection also involves the sebaceous gland. It is an infection of the hair follicle with Staphylococcus aureus. It may be associated with perifolliculitis, which may proceed to suppuration.
A furuncle frequently occurs on the neck, face, armpits, and buttocks. It begins as a small, tender, red nodule that becomes painful and fluctuant. After a couple of days, there will be softening at the centre on the summit of which a small pustule appears.
Frequently, pus will spontaneously drain, and often the furuncle will resolve on its own. Perianal boils when ruptured form sinuses. In persons whose immunity is very low furuncles may lead to cellulitis. Constitutional symptoms like fever, malaise and pain are usually present. Factors that contribute to the development of furuncles include:
- Obesity
- Blood disorders
- Taking oral steroid medications
- Diabetes
Homoeopathic Approach:
Patients present to us either during acutes or with recurrent tendency to develop furuncles. Here the tendency can be reduced by maintaining good hygiene, with changes in lifestyle along with homoeopathic medicines.
Among the remedies for the condition are Bell, Apis, Anthracinum, Hep S, Arsenicum alb, Sil, Phyt, Bry, etc.
Anthracinum: There is a tendency to develop a succession of boils. The boils have an angry look.
Hepar Sulph: In the early stage of pus formation. Excessive sensitiveness of part with sharp sticking pains.
Arsenicum. alb: The affected part burns like a coal fire
CARBUNCLE
Definition:
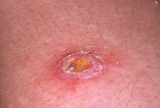
An acute, circumscribed, cutaneous and subcutaneous inflammation characterized by multiple foci of necrosis and sloughing of the superficial tissues. It is infective gangrene of subcutaneous tissue due to staphylococcal infection. As there is more accumulation of pus and slough and a major portion is hidden, the condition can be classified under the sycosyphilitic miasm.
Pathology: The carbuncle is formed as the staphylococci penetrate the deeper layers of the skin and the subcutaneous fat. There are many small abscesses which communicate with each other and get discharged by separate openings which give a sieve-like appearance to the surface.
Due to the persistence of facial attachment to the skin, individual compartments in the carbuncle are maintained. Carbuncles may be more extensive than they appear.
FEATURES
- Middle or old age.
- Extensive infection of a group of contagious vesicles which are painful that change to stiff swelling and spreads rapidly with marked induration. Later these vesicles transform into pustules. ( Apis M, Amm M,)
- These pustules burst out subsequently in several openings in the skin giving sieve like appearance, which is the characteristic of carbuncle. (Hepar S, Bufo, Petro)
- A large deep ulcer is formed ultimately due to aggregation of the multiple openings. At the floor of the ulcer lies ashy – grey slough. (Ars alb, Graph, Anthracinum,)
- As the slough gets separated eventually, the ulcer heals by itself as there is excavated granulation tissue underlying. In some individuals, like diabetic persons, the sloughing process may increase and may extend to deeper tissues like muscles or even bones. ( Ac Fluor )

Homoeopathic Approach:
The suppurating tendencies that one frequently observes in homoeopathic practice is seen as incurable, since they have a strong tendency to recur if inadequately treated. Hence, proper selection and administration of acute, chronic and intercurrent medicines should be undertaken.
The remedies for the condition are:
Anthracinum: There is a tendency to develop a succession of carbuncles. The carbuncles have an angry look.
Hepar Sulph: In the early stage of pus formation. Excessive sensitiveness of part with sharp sticking pains.
Silicea: Helps in suppuration and healing of the infected parts.
CELLULITIS
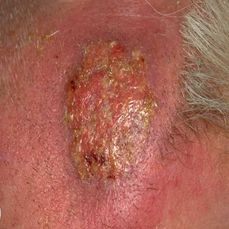
Cellulitis is a localized or diffuse inflammation of connective tissue with severe inflammation of dermal and subcutaneous layers of the skin. Or, it is a non – suppurative inflammation spreading along the subcutaneous tissues and connective tissue planes and across intercellular spaces.
It is generally subcutaneous but the term may also be applied to pelvic, perinephric, pharyngeal and other connective tissue infections. The commonest causative agent is the B-Haemolytic Streptococcus, staphylococci, and C. perfringens. The invasiveness of this organism is due to the production of hyaluronidase and streptokinase, which dissolve the intercellular matrix and the fibrin inflammatory barrier respectively.
Pathology: The organism usually gains access through a wound or scratch or following surgical incision. There is wide spread swelling and redness at the area of inflammation, but without definite localization. Initially the site of inoculation becomes red. Gradually the skin swells and becomes shiny. In severe infections blebs and bullae form on the skin. Central necrosis may occur at a later stage.
Common risk factors include:
- A weakened immune system
- Skin conditions that cause breaks in the skin, such as eczema and athlete’s foot.
- Intravenous (IV) drug use
- Diabetes
- A history of cellulitis
FEATURES:
- Fever, toxicity (tachycardia, hypotension).
- Swelling is diffuse and spreading in nature.
- Pain and tenderness, red, shiny area with stretched warm skin. (Cantharis, Apis Mellifica)
- Cellulitis will progress rapidly in diabetic and immunosuppressed individuals. (Lachesis, Rhus tox)
- Tender regional lymph nodes may be palpable which signify severity of the infection.
- No edge; no pus; no fluctuation; no limit.
CELLULITIS IN SPECIAL AREAS
- Orbital Cellulitis
- Cellulitis in orbit causes proptosis, leading to impairment of ocular movements and blindness.
- It can spread through ophthalmic veins into the cavernous sinus causing cavernous sinus thrombosis.
- It requires admission and immediate aggressive treatment with higher-generation antibiotics (penicillin, cephalosporin).
Symptoms such as the following could signal that cellulitis is spreading:
- Drowsiness
- Lethargy
- Blistering
- Red streaks.
POSSIBLE COMPLICATIONS OF CELLULITIS:
- Sometimes cellulitis can spread throughout the body, entering the lymph nodes and bloodstream.
- In rare cases, it can enter into deeper layers of tissue.
- Blood infection
- Bone infection
- Inflammation of lymph vessels
- Tissue death, or Gangrene.
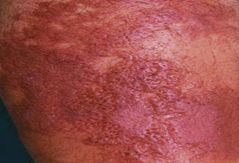
Erysipelas:
- Erysipelas is a bacterial skin infection involving the upper dermis that characteristically extends into the superficial cutaneous lymphatics. OR
- Erysipelas is a bacterial skin infection that usually affects the top layer of the skin.
- Erysipelas is very rare but requires immediate treatment.
- Erysipelas is often associated with another skin infection known as cellulitis, which affects the lower layers of the skin.
- Erysipelas is a tender, intensely erythematous indurated plaque with a sharply demarcated border. Its well-defined margin can help differentiate it from other skin infections (eg, cellulitis).
- In the middle ages, it was referred to as St. Anthony’s fire.
- Historically, erysipelas occurred on the face, but cases today most often involve the legs.
Aetiology:
- Idiopathic
- Congenital/Genetic
- Traumatic
- Infections /Infestation
- Autoimmune
- Neoplastic (Benign/Malignant)
- Degenerative
- Iatrogenic
- The bacteria Streptococcus is generally responsible for erysipelas.
- This bacteria lives on the skin and causes no harm, but can enter deep layers of the skin through a cut or wound and develops into an infection.
Other possible causes:
- Insect bites
- Ulcers in the skin
- Other skin conditions such as psoriasis
- Cardiac problems
- Diabetes
- Overdose of illegal drugs
- Surgical incisions
- Weakened immune system
Pathophysiology:
- Bacterial inoculation into an area of skin trauma is the initial event in developing erysipelas.
- The infection rapidly invades and spreads through the lymphatic vessels.
- This can produce overlying skin “streaking” and regional lymph node swelling and tenderness.
- Immunity does not develop to the inciting organism.
- Streptococcal toxins are thought to contribute to the brisk inflammation that is typical of this infection.
Symptoms:
- Prodromal symptoms, such as malaise, chills, and high fever.
- Pruritus, burning, tenderness, and swelling are typical complaints.
- Muscle and joint pain.
- Headache and other systemic manifestations of an infectious process.
- Associated co-morbidities in erysipelas include diabetes mellitus, as well as hypertension, chronic venous insufficiency, and other cardiovascular diseases.
Signs:
- Lower extremities in 80% of patients;
- The patient may appear healthy or toxic depending on the extent of the infection.
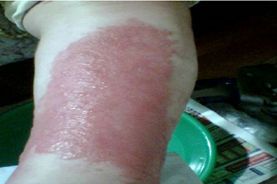
- Begins as a small erythematous patch that progresses to a fiery-red, indurated, tense, and shiny plaque.
- Step sign- classically a sharply raised border with abrupt demarcation from healthy skin.
- Warmth, Edema, and Tenderness,
- Overlying skin streaking and regional lymphadenopathy
- Vesicles and bullae, along with Petechiae and even frank necrosis.
Differential Diagnosis:
- Granuloma Faciale
- Herpes Zoster
- Necrotizing Fasciitis, Relapsing Polychondritis
- Scarlet Fever
- Stasis Dermatitis
- SLE
- Tuberculous leprosy.
Prognosis:
- Excellent.
- The mortality rate is less than 1%
- Can be fatal when associated with bacteremia in very young, elderly, or immune-compromised patients.
Complications:
- Uncommon
- Gangrene/amputation
- Chronic edema, Scarring
- Bacteremia/sepsis
- Scarlet fever, Pneumonia, Abscess, Embolism, Meningitis, etc…
- Bursitis, Osteitis,
- Arthritis and tendinitis.
- Acute glomerulo-nephritis,
- Endocarditis,
- Septicemia, and streptococcal toxic shock syndrome.
- Death
Homoeopathic Approach:
Apis Mellifica — for swelling with a puffy appearance that worsens with heat and pressure, especially in the afternoon, and is better with cold applications, open air, movement, and sitting upright. There is much swelling of the affected area along with much burning and stinging type of pains. Rosy hue of skin with much sensitivity to touch.
Cantharis — sensation of excessive burning, intense and violent inflammations that develop extremely quickly. For restless and anxious individuals; a characteristic sensation is: ulcerative pain of the skin when touched.
Lachesis — Skin yellow, green, lead-coloured, or bluish-red or blackish, Yellow, red, copper-colored spots, for symptoms that tend to be worse on the left side of the body and during and immediately after sleep.
Mercurius — for individuals who are bothered by both heat and cold, and are often trembling and impulsive. The person may have moist or greasy-looking skin, with swollen lymph nodes and offensive breath, and be very sensitive to changes in temperature. Itching, worse from warmth of the bed, round coppery red spots shining through the skin.
Rhus Toxicodendron — for individuals who are restless and anxious with itching that tends to worsen at night but is relieved by warm compresses or pressure.
Sulphur — for hot, burning skin with itching that worsens at night and with washing. Itching, burning, worse after scratching and washing. The skin becomes rough and scaly and little vesicles form. Soreness and rawness appear wherever there is a fold of skin.
Bibliography:-
- Das, Concise Text Book of Surgery 10th Edition reprinted in March 2019
- SRB’s Manual of Surgery, 6th 2019, Sriram Bhat M
- Hand Book of Surgery by S. C. Basu. 2nd Edition reprinted in 2005
- Pocket Manual of Homoeopathic Materia Medica, Boericke William, M.D
- Clinical Materia Medica. Farrington. E.A., M.D.
- A Dictionary of Practical Materia Medica Clarke Henry John, M.D.
- Homoeopathic Therapeutics. Samuel Lilienthal. M.D.