Introduction
Ascites is an accumulation of fluid in the peritoneal cavity. The predominant cause of Ascites in the United States is cirrhotic liver disease, which accounts for -80% of all cases. Ascites may also result from other systemic diseases, such as heart failure (cardiac Ascites) and nephritic syndrome, or from primary peritoneal pathology, such as peritoneal carcinomatosis or tuberculosis. The presence of Ascites is often suspected based on the history and physical examination— which will often give clues to the etiology and therefore the treatment.
Causes of Ascites
Increased portal venous pressure
- Pre-hepatic: portal vein compression or thrombosis; schistosomiasis
- Hepatic: cirrhosis; acute hepatic necrosis; viral hepatitis
- Post-hepatic; Budd-Chiari syndrome, myeloproliferative disorders, constrictive pericarditis: right heart failure, hypercoagulable states
Hypoproteinaemia
- Renal disease causing severe Proteinuria
- Malnutrition and Malabsorption
- Protein losing enteropathy
- Acute or chronic liver disease
- Severe acute or chronic illness
Chronic peritoneal inflammation and infection
- Chronic infection: tuberculosis; fungal infection
- Secondary malignant infiltration
- Post irradiation
Leakage of lymphatic fluid (chylous ascites)
- Congenital
- Surgical trauma
- Primary and secondary lymphatic malignancy
Other fluids
- Pancreatic ascites
- Bilious ascites
- Urinary ascites
Diagnostic Testing for Ascites
If the physical examination is equivocal, ultrasound confirms the diagnosis of Ascites. When the cause is in doubt, diagnostic paracentesis should be performed.
The ascitis fluid is analyzed for cell count and the differential is done before therapy because dieresis may alter fluid characteristics. Serum and ascetic fluid albumin levels are compared to assess the cause of fluid accumulation.
Ascites resulting from hydrostatic disease (portal hypertension, congestive heart failure) has serum Ascites albumin difference greater than 1.1g/dL, whereas inflammatory or neoplastic disease produces a serum Ascites albumin difference less than 1.1g/dL.
With infection, ascetic fluid exhibits increased cellularity, decreased pH, and increased lactate content as well as positive gram stains and cultures.
If malignancy is suspected, a large volume of fluid (i.e.,> 1L) must be sending for cytologic analysis. If the cytology is positive, radiographic or endoscopic studies or both are obtained to localize the sources of malignancy.
Elevated fluid triglyceride levels in chylous Ascites should prompt an evaluation for malignancy or tuberculosis. High ascetic fluid amylase levels should point to an evaluation for pancreatic disease
Ascites treatment
A. Directed toward the palliation of symptoms rather than improving the patient’s appearance.
B. Paracentesis
- Up to 1L/day may provide relief of acute respiratory symptoms; in portal hypertension, 3-4 L can be removed safely.
- Significant morbidity occurs with repeated paracentesis.
- Removal of large volumes of fluid may lead to electrolyte abnormalities and hypovolemia.
- Potential complications
- Hemorrhage
- Injury to intra abdominal structures
- Peritonitis
- Bowel obstruction
- C. Monitor weight daily
D. Encourage patient with non-malignant ascites to restrict sodium to 2 g/day.
- E. Diuretics
- Lasix, spironolactone, and amiloride are used for dieresis in ascites from benign causes.
- Goal for daily weight loss is 0.5-1.0 kg with edema and 0.25 kg without edema.
- Diuretics are not useful for malignant ascites.
- F. Systemic or intraperitoneal chemotherapy
- Aimed at the primary tumor
- Effective agents used in intraperitoneal chemotherapy
- Bleomycin
- 5-Fluorouracil
- Thiotepa
- Doxorubicin
- Cisplatin
- Mitoxantrone
G. If paracentesis is required more than once a month, a more aggressive therapy is warranted.
H. Peritoneovenous shunts (LaVeen or Denver) may be used to treat refractory cases if patient has a life expectancy of > 1 month and is without major cardiac or liver metastases, disseminated intravascular coagulation, and renal disease.
- I. Transjugular intrahepatic portosystemic shunt is non-surgical technique used to decrease the portal circulation pressure.
- J. Sclerotherapy
- May be considered using blemycin, tetracycline, or talc
- Responses rates of around 30%
- K. Supportive measures
- Positioning, elevation of lower extremities, and use of pillows
- Monitor and treat impaired bowel motility.
- Metoclopramide (Reglan) may assist with nausea and vomiting by increasing upper gastrointestinal motility. .
- Oxygen therapy, opioids, or both may help with dyspnea.
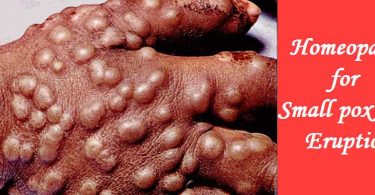
Homeopathic treatment of ascites symptoms – Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat ascites symptoms but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to cure ascites symptoms that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. There are following remedies which are helpful in the treatment of ascites symptoms:
Apis Mel, Apocynum, Ledum Pal, kali Carb, Arsenic Album, Lycopodium, kali Brom, Millefolium, Fluoric acid, Aurum Mur.
Reference:
Charles H. Griffith, Andrew R. Hoellein- First exposure to internal medicine: hospital medicine; 2007: 207
Joe Janwar Tjandra, Gordon J. A. Clunie, Andrew H. Kaye- Textbook of surgery; 2006; 597
H. David Humes- Kelley’s Essential of Internal Medicine; 2001; 187
Wendy H. Vogel, Margery A. Wilson, Michelle S. Melvin- Advanced practice oncology and palliative care guidelines; 2003; 183
Ascites Cases Cured with Homeopathic Medicine
Homeopathic Supportive Care in a Case of Advanced Cancer – by B.S. Suvarna




MY BROTHER IS SUFFERING FROM LIVER CIRROSIS WITH TUMOR IN LIVER. Every WEEK 5-6 liter water is removed from his stomach. is there any cure in homeopathic.
Pulmonary thrombosis embolism & PAH severe are the reason for my ascites. Could you prescribe specific medication
Jaipur Case- my mother 71 year is suffering from ascitis from last 1 year..we have to go hospital in every 20-25 Days for extraction of fluid aplrox 10 to 11 liter every time….but now she has got very weak ..hard to walk . plz help if any medicine in homeopathy or ayurved m 9649905446