DEFINITION
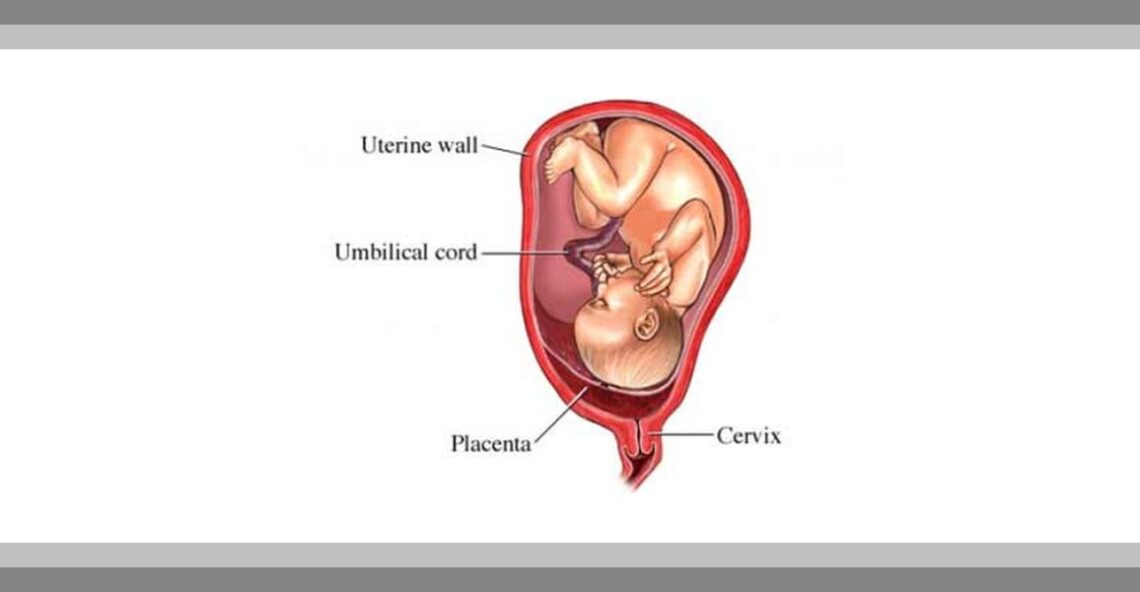
Placenta previa is the condition in which placenta implants in the lower portion of the uterus and covers all or part of the internal cervical os. It can block the cervical opening to the va-gina (birth canal). Placenta previa carries as risk of excessive bleeding, which can threaten the well-being of the mother and the baby. A low lying placenta diagnosed in early pregnancy usually self corrects as the uterus enlarges. Types of placenta previa include:
- Total placenta previa: The placenta completely covers to opening of the cervix. This type presents the most serious risk to the mother.
- Partial placenta previa: The placenta partially covers the opening of the cervix.
- Marginal placenta previa: The placenta just reaches the cervix.
Body parts involved
Uterus; placenta (the organ that transfers nourishment and oxygen from mother to fetus): cervix (opening to the uterus).
Risk increases with
- Previous uterine surgery involving the lining of the uterus. This includes dilation and curettage (D&C) and cesarean section.
- Smoking
- Prior induced abortion.
- Multiple previous pregnancies and births.
- Pregnancy with twins or other multiples.
- Pregnant women over age 35.
- Previous placenta previa.
Types of Placenta Previa
Ultrasound enables an accurate grading and localization of the placenta. The classification of placenta previa is based on the location of placenta, as described by Jauniaux and Campbell, is:
Type I -Low lying placenta with its lower margin within 5 cm of the cervical os
Type II– Marginal placenta previa, with the placenta reaching up to the margin of the os
Type III– Partial placenta previa, with the placenta partially covering the os
Type IV– Total placenta previa, with placenta completely covering the os
Types III and IV placenta previa cause much more bleeding than Types I and II and the bleeding occurs earlier in the 3rd trimester. The anterior placenta previa gets pulled up above the symphysis pubes during labour and does not compromise the fetal oxygenation to the same extent as the posterior placenta previa.
The posterior, on the other hand, can be compressed by the presenting part and this will cause severe fetal asphyxia and sometimes fetal death. Because of this, posterior placenta previa is described as a “dangerous placenta previa”. Lately, placenta is called “low lying” if its lower margin is more than 2 cm from the internal os, and placenta previa if the distance is less.
Pathology of placenta previa
- The placenta may be large, thinned out and infracted at places. Since the lower uterine segment is thin with poor decidual lining, adherent placenta with accrete, increta and percreta is common. The risk of accrete increase with increase in number of the uterine scars.
- The fetal malformation is reported in 7% cases, which is attributed to abnormal placentation and perfusion. IUGR may also occur.
- Mal-presentation such as breech or transverse lie is common, caused by an abnormal uterine shape due to the placenta occupying the lower segment.
- A high level of Alfa-fetoprotein reported in a few cases suggests abnormal placentation.
Etiology of placenta previa
The exact etiology of placenta previa is unknown. The condition may be multifactorial and is postulated to be related to multiparty (four fold increase in grand multiparous patients), multiple gestations (two fold increase), advanced maternal age, previous cesarean deliver (three fold increase), previous abortion, and possibly, smoking (two fold increase).
Thus, possible etiologic factors include a scarred or poorly vascularized endometrium in the corpus, a large placenta, and abnormal forms of placentation.
Symptoms of placenta previa
The symptoms of placenta previa are bleeding that is spontaneous and causeless, unless it follows intercourse. The bleeding is often painless unless it occurs with the onset of labour. The bleeding is recurrent and occurs at intervals and progressively becomes severe. The first bleed, called a warning bleed, is slight and is noticed by the woman as bright blood. The causeless, painless and recurrent bleeding in the third trimester is typical of placenta previa. It is not rare for the patient with Types I and II placenta previa to bleed just once near term or at the onset of labour.
Diagnosis for placenta previa
- History: – Classically, placenta previa is diagnosed after painless bleeding in the second or third trimester. A higher than normal rate of placenta previa is associated with previous cesarean section, previous induced or spontaneous abortion, advanced maternal age, and smoking .Accordingly, placenta previa is associated with placenta accrete, an abnormally adherent placenta that commonly causes excessive bleeding in the third stage of labor due to incomplete separation. This is especially noted in patients with repeated cesarean sections, indicating that both conditions may be related to endometrial defects. The rate of accrete may be as high as 65% after multiple cesarean sections.
- Examination:- In modern obstetrics, there is no reason to perform a cervical examination in suspected previa before performing an ultrasound examination, due to the risk of perforating the portion of placenta that is palpable through the os. Prior to the widespread availability of ultrasound on obstetric units, cervical examination at term was often performed after the patient was prepared for possible cesarean delivery (“double setup”). Nowadays a double setup examination is done only when the localization of a low lying placenta is not clear from the ultrasound.
- Blood tests are generally normal in the absence of anemia due to massive hemorrhage.
- Imaging
- a. Ultrasound: – an ultrasound should be performed with the onset of painless bleeding in pregnancy. False-positive and false negative rates may each approach 5%. Bladder over-distention is associated with false positives, and consideration should be made to catheterizing the bladder before performing an ultrasound. Clinical judgment is important. Heavy bleeding, especially when coexisting with signs of fetal distress, should lead to an immediately delivery.
- b. Incidentally discovered placenta previa: – In this age of “routine” obstetric ultrasound, previa is frequently diagnosed prior to any bleeding and commonly over-diagnosed
- c. MRI: – can clearly outline the location of a placenta previa, but it is much more expensive and less readily available.
Possible complications of placenta previa
- Poor fetal growth, due to an abnormal placenta providing a decrease in blood flow and oxygen delivery.
- Premature delivery or (possibly) fetal death.
- Rarely, blood loss could lead to maternal shock and death.
Management of placenta previa
The goal of therapy is to prolong the pregnancy as long as possible, anticipating planned delivery at term or when fetal pulmonary maturity can be documented by amniocentesis. Earlier delivery should be carried out in the face of severe maternal hemorrhage, fetal distress, or unstoppable preterm labor. Even if the initial maternal hemorrhage exceeds 500 ml, the pregnancy can usually be significantly prolonged. We emphasize that this conservative goal applies only to the patient who is hemodynamically stable and in whom the bleeding stops within a reasonable period of time.
The patient should be hospitalized if she has an episode of bleeding after 24 weeks. Although out patient management can be allowed under certain strict conditions for patients who are reliable, there is evidence that, with inpatient management: (1) the gestational age at birth will be more advanced: (2) the birth weight will be greater; (3) the neonatal mortality will be lower; and (4) neonatal hospitalization will be of shorter duration.
Stool softness is important; a diet high in fiber should be prescribed. Oral iron therapy should be started. Weekly or twice weekly biophysical profile tests should be undertaken to assure fetal well-being.
Two to four units or red cells must be continuously available for transfusion. If active bleeding subsides and the maternal hematocrit remains greater than 34%, then she is a candidate for autologous blood transfusion, which has been shown to be very safe for both the mother and the fetus. In the face of active bleeding or if the hematocrit drops to less than 30% red cell transfusions should be administered.
Glucocorticoides should be administered at least once between 28 and 32 weeks’ gestation. The rationale for administration is that (1) infants of mothers with previa tend to have delayed pulmonary maturation; (2) Glucocorticoides need at least 12-24 h to be effective; and (3) the obstetrician has no way of predicting when emergency delivery may become necessary.
Preterm contractions are not common among patients with previa, particularly with marginal and partial placenta previa. Although controversy surrounds the use of tocolytic agents in this situation, tocolytic therapy may prevent further shearing of the placenta from the lower uterine segment and prolong gestation.
If fetal lung maturity can be documented, delivery should be carried out electively within 24 h. At 39 weeks or more, delivery can be carried out without amniocentesis.
Emergency delivery should be carried out in the face of (1) excessive maternal hemorrhage; (2) fetal distress; or (3) uterine contractions unresponsive to tocolytic therapy. If central placenta previa is diagnosed, delivery must be by Cesarean. If there is a question of a marginal placenta previa, a double set-up examination should be performed in the Cesarean room before delivery. Occasionally, the obstetrician is surprised to find that no placenta can be palpated through the cervix, in which case the membranes may be ruptured and Labor induced in anticipation of a vaginal delivery.
Finally, an alternative method of management of symptomatic placenta previa before 30 weeks gestation may be placement of a cervical cerclage.
Homeopathic treatment of placenta previa – Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat placenta previa but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to treat placenta previa that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. There are following remedies which are helpful in the treatment of symptoms related to placenta previa:
Nux Vomica, Sabina, Sepia, Secale Core, Ferrum met, Veratrum Album, Erigeron, Phosphorous, Ipecauc and many other medicines.
Reference:
T. Murphy Goodwin, Martin N. Montoro, Laila Muderspach, Subir R; Management of Common Problems in Obstetrics and Gynecology; 2010; 57
H. Winter Griffith, Stephen Moore, KENNETH YODER- Complete Guide to Symptoms, illness & Surgery; 2006; 518
Daftary & Desai- Selected Topics in Obstetrics and Gynaecology-4: For Postgraduate and; 2008; 109
Padubidri & Anand, V. Padubidri, Ela Anand- Textbook of obstetrics; 2006; 108-09
Robert B. Taylor- Manual of family practice; 2002; 465
Hung N. Winn, John C. Hobbins- Clinical maternal- fetal medicine; 2000; 51-52
Placenta Previa Cases Cured with Homeopathic Medicine
Blessed Events! Everyday Miracles in the Delivery Room – by Susan Vaughen




My wife completed 5 months of pregnancy ultrasound report shows placenta is attached on posterior wall lower edge of the placenta about 2.3 cm from internal is.
I too have a low lying placenta about 1.6 cm from internal OS. It was diagnosed in my 5th month and now my 6th month is running. Will it go up?
Nice article