My parents understood early on in my life that I would likely present them with challenges which might force them to reconsider some of their basic beliefs. What I eventually came to qualify as the Tubercular miasm in myself had found expression in all of my own important life choices. Having emigrated to Russia from the US with my two small children during the turbulent post-perestroika early 90’s, my mother had long ago resigned herself to the possibility that my never-ending search for the sacred homeland would conflict with her desire to have me and my children in close proximity. She had accepted, as well, my vocation as homeopath, even if she couldn’t quite understand what homeopathy is.
And so when she informed me that she had recently been diagnosed with essential thrombocythemia, neither of us doubted that I would insist on treating her with homeopathy. Her physician – a doctor of internal medicine with whom I was well acquainted – had accidentally discovered her platelets to be high on a routine blood test. She had sent her to the oncology department at the local university hospitals and clinics and the diagnosis was confirmed after further testing.
Essential Thrombocythemia (ET) is a chronic myeloproliferative neoplasm (MPN) characterized by an increased number of platelets in the blood. Most commonly diagnosed in women over the age of 50, ET is associated with a proliferation of platelet precursors in the bone marrow (Homeopathy for Bone Marrow Transplant) and complications frequently include blood clotting and/or bleeding. Less common consequences in the later stages of ET include a transformation to myelofibrosis (marrow scarring) or acute leukemia.
With this disease, as with many others, traditional (allopathic) medicine explains: “No one knows what causes the onset of ET”. One of the greatest contributions to early homeopathic medicine, and certainly one its philosophical foundations, is the understanding of miasms. Miasms don’t point a finger at a single causative agent or a defective gene. Rather they provide an understanding of a specific context, echoed in space and time both within the individual and across generations, that represents latent or explicit expression of form patterns in disease and health. When we grasp the context, the dominant miasm of the individual and the family, we are able to better understand why a particular illness develops in a particular individual. We are also able to make prognoses about potential future illness. And, of course, we then have a far more precise understanding of the nature of the person’s condition. This understanding of the nature of the condition is absolutely essential for effective homeopathic prescribing. Without knowing this we are stabbing at thin air, choosing remedies not based on a totality, but only on surface symptoms.
Allopathic medicine concentrates on the details. It searches for faulty parts and then goes about trying to fix them. Alas, people are not automobiles. Parts don’t have meaning on their own, apart from a totality. Therefore any one symptom, separated from its overall condition, or any one disease entity, separated from the sick person, can’t be understood with any depth of insight. It is an entity floating in space, not attached to anything. This concentration on the parts misleads doctors into making incorrect diagnoses. No disease appears out of thin air. There is a prerequisite inherent in the future patient, a prepared soil. How much wider could traditional medical diagnostics become were it to adopt an understanding of the law of similars!
Having learned of my mother’s diagnosis of ET, the first thing I needed to investigate was the accuracy of the diagnosis. Did it fit into the totality of my mother? Did it represent a particular expression of her dominant miasm, and the family’s miasmatic patterns? Any particular condition has an inherent logic built into it, and that is the logic of the vital force. The vital force always does only what it can with what it has. It can’t be “strong” or “weak”, but it can be forced to go around obstacles. It runs like a river, and rivers can be full of boulders or garbage, beaver dams or boats.
Beyond accurate diagnosis, the homeopath, regardless of his or her medical background, is obligated to study the disease condition in question. We need to understand a disease entity from both the allopathic and homeopathic perspectives. Such an understanding seeks answers to the questions:
- what is the typical course of the disease?
- what are the risk factors of the disease?
- what are the usual treatments? Have there been any documented cases of cure of the disease with homeopathic treatment? What is the experience of treating such a patient with homeopathy?
- what is the mortality rate, with and without regular allopathic treatment?
Familial occurrence of MPNs has long been known. Hereditary predisposition was supported by an epidemiological study from Sweden showing an increased occurrence of these diseases among relatives of MPN patients.[1] Recently, molecular support for these clinical observations was provided by the discovery of an increased frequency of a special haplotype of the JAK2 gene, the 46/1 haplotype, in MPN patients and their first-degree relatives.[2] What allopathic medicine calls “hereditary predisposition”, homeopathy calls miasmatic tendencies. Heredity is more narrow and often involves finding a gene. Miasms are broader and include an entire spectrum of potential disorders.
The WHO diagnostic criteria (as of 2016) for ET include all four of the following:
- Sustained platelet count >450 x 109/L;
- Bone marrow biopsy showing increased number of enlarged, mature megakaryocytic; no significant increase or left-shift of granulopoiesis or erythropoiesis;
- Not meeting WHO criteria for BCR-ABL+CML, PV, PMF, MDS or other myeloid neoplasm;
- Presence of JAK2, CALR or MPL mutation;
- Presence of a clonal marker or absence of evidence for reactive thrombocytosis (for example due to iron-deficiency anaemia).
Risk factors associated with ET include:
- Gender: Women are 1.5 times more likely than men to develop essential thrombocythemia.
- Age: People older than 60 are most likely to develop the condition, although 20% of ET sufferers are under the age of 40.
- JAK2 Mutation: Approximately half of all ET patients have a mutation of the JAK2 gene in their blood-forming cells. This mutation leads to hyperactive JAK (Janus kinase) signaling, causing the body to make the wrong number of blood cells.
- CALR mutation: Nearly a quarter (23.5%) of those diagnosed with MF and ET have a mutation called Calreticulin, or CALR. Discovered in 2013 by two independent laboratories, the identification of the CALR genetic marker has potential implications for treatments and prognosis for those with ET.
The calreticulin gene (CALR) is mutated in about 20-25% of cases of primary myelofibrosis and 20-25% of cases of essential thrombocythemia. The most common mutations (>90%) are caused by either a 52 bp deletion or a 5bp insertion in exon 9 of CALR; both result in a frameshift and premature truncation of the protein. The combination of thrombocytosis and either the JAK2 p.V617F, an MPL exon 10 mutation, or a CALR exon 9 mutation in the absence of bone marrow fibrosis and erythrocytosis may be considered as diagnostic of essential thrombocythemia. Patients with a CALR exon 9 mutation have very high platelet counts but a relatively low risk of thrombosis. Patients with myelofibrosis carrying a CALR exon 9 mutation have an indolent clinical course with better survival than those carrying JAK2 p.V617F or an MPL mutation. The survival is especially superior compared to patients with nonmutated JAK2, CALR, and MPL, who have a very poor prognosis and a particularly high risk of leukemic transformation.
My mother’s test results for the CALR mutation were positive. The lab report reads: A 5 bp insertion, c.1154_1155insTTGTC, or type 2 mutation was detected in the calreticulin gene (CALR), resulting in a frameshift with premature truncation.
ET evolves to myelofibrosis in a minority of cases, whereas transformation to acute leukemia is rare and increases in association with the use of certain therapies. Survival of ET patients does not substantially differ from that of the general population. However, important morbidity is derived from vascular complications, including thrombosis, microvascular disturbances, and bleeding. Because of this, treatment of ET must be aimed at preventing thrombosis and bleeding without increasing the risk of transformation of the disease.[3]
Patients are considered at high risk of thrombosis if they are older than 60 years or have a previous history of thrombosis and at high risk of bleeding if platelet counts are > 1500 × 109/L. Patients with low-risk ET are usually managed with low-dose aspirin, whereas treatment of high-risk ET is based on the use of cytoreductive therapy, with hydroxyurea as the drug of choice and IFN-α being reserved for young patients or pregnant women. For patients resistant or intolerant to hydroxyurea, anagrelide is recommended as second-line therapy. Strict control of coexistent cardiovascular risk factors is mandatory for all patients. The role in ET therapy of new drugs such as pegylated IFN or the JAK2 inhibitors is currently under investigation.[4]
My mother’s oncologist at the university hospitals and clinics in her town was a young woman from India. She immediately prescribed hydroxyurea. This care decision was made despite my mother’s low risk factors. Her platelet count had never exceeded 1,000,000 x 109/L. She never suffered from hypertension and she was not overweight. She did not have diabetes or a history of thrombotic events. These factors alone were sufficient, in my mind, for her doctor to choose an “expectant” path. Yet she was adamant about the chemotherapy.
The homeopath is in a very difficult dilemma when it comes to treating patients for what are considered incurable disease entities, the traditional treatment of which involves severely suppressive drugs. Oncological conditions present especially challenging situations. Under usual circumstances when faced with chronic disease we have an expectation – indeed a prerequisite – that the patient take his or her share of responsibility in regard to treatment decisions. We work from the “informed consent” mentality; it is our job to explain the treatment options, their probable success rates (or lack thereof), the side effects of traditional treatments, as well as what we predict can be achieved with homeopathy. It’s one thing when the patient suffers from degenerative disease, with which he will have to live the rest of his life, and which can most probably be improved. It’s quite another thing when the person has a diagnosis of cancer. Cancer brings out a person’s most significant emotional and mental symptoms, expressed in the very way in which the person reacts to the diagnosis. For most it is akin to reacting to a sentence of execution. Most patients react by “scrambling”: fear activates the fight or flight mode and they are ready to do anything and everything to just be rid of the cancer monster. They tend to become irrational and irresolute. They want someone else to take responsibility for their condition, to tell them what to do. And so those cancer patients who come to the homeopath tend to be either wanting the best of all worlds (a misnomer that can never be achieved), or they want to be saved by what they view as a powerful alternative to the evils of modern medicine. It is a rare person who is not in “fight or flight”.
Young homeopaths often fall into the trap offered by such patients. They are easily drawn into a codependent healer-patient relationship because it gives a sense of being needed, being indispensable. Like in any codependent relationship, the interaction is not based in love, but in dependence; it does not engender free will and the self-actualising potential entailed therein, but leads to self-loathing and resentment of the Other.
We nourish a loving, mature healer-patient relationship in part by being honest (first and foremost with ourselves) about our fallibility. Then it’s equally important to admit that homeopathy has limits, even when masterfully practiced – because life has limits. This is what the “fear of God” means: it’s not actually being afraid of God, but rather an acute awareness of our utter mortality, the finite nature of our earthly existence, the greater destiny for each soul according to God’s providence.
ET and all myeloproliferative neoplasms are considered by some to be a slowly-progressing form of blood cancer, since they fit into the definition of “cells growing without control”. Others don’t consider them cancer at all, since they generally affect life expectancy minimally. From the homeopathic standpoint, one can say that myeloproliferative diseases are an expression of the cancer miasm, insofar as one discrete area of the organism is dominating the organism as a whole. The particular nature of Essential Thrombocythemia can be considered an expression of the tubercular miasm, since the condition centers in the blood, marrow, and bones. Metaphorically, the overproduction of blood cell precursors leading to the overproduction of platelets can be seen as a the organism wanting to stop what it perceives as a massive hemorrhage, a threatened departure of one’s blood as the life-giving principle.
My mother and I discussed her condition at length. She has not been one to take medicine her whole life, but since she has great respect for her internal physician, she was inclined to “try” the chemotherapy, knowing that her doctor recommended it strongly. My arguments against chemotherapy at this point were, for her, rather insufficient. She wanted to do what the doctors recommended, out of politeness and respect. While I accepted her initial decision, I sensed deep anxiety at the prospect of her starting chemotherapy, since I was already closely familiar with the context of my mother.
Homeopaths with a soft spot for the miasms love a good detective story and the story of my mother’s family provides endless homeopathic intrigue. Without delving too deeply into family history, the following points have definite relevance for my mother’s case:
- Her father had died of tuberculosis of the bones, having contracted it via BCG having been administered as treatment for bladder cancer. The bladder cancer had been very slow growing and he would not have died from it, and as it was, he was already 87. After suffering excruciating back pain it was discovered he had a fractured spine, and a bit later the diagnosis of TB was confirmed. He nevertheless lived until the age of 94 – albeit in constant pain.
- My mother’s older sister had died of leukaemia at the age of 37. She developed a leukaemia transformation from the chemotherapy she was given for the treatment of multiple myeloma (a blood/bone cancer) – which had started at age 27.
- My mother’s aunt (grandfather’s sister) had died of leukemia, also as a transformation effect after chemotherapy for breast cancer.
- My mother’s grandmother on her mother’s side had suffered from what later came to be considered manic-depressive psychosis, which began when she was a young woman. Her twins had been taken away from her to be raised by their grandmother. She was an emotional, creative woman who corresponded with a few writers of the early twentieth century. She committed suicide by hanging at the age of 54 during a psychotic depression.
My deepest concern about my mother taking chemotherapy was the risk of her condition transforming into leukemia. With our family history, her advanced age (78), and lack of concomitant risk factors for thrombotic events, the risk from chemotherapy was unwarranted. Yet my mother had made up her mind to listen to the doctors, and she started taking the Hyroxyurea.
Not 6 weeks had passed, when I received a call from my father. “Don’t worry – yet,” he began. “Your mother got very sick over the weekend and is in the hospital.” She had expended an extra amount of energy that weekend on a relative’s wedding. When Monday rolled around, she was feeling extremely weak, short of breath, and had developed a fever. She collapsed onto the floor and my father called the ambulance. Later I learned that she had been put on oxygen by mask and they were investigating the possibility of sepsis. Her temperature was 104° when they brought her in.
In hindsight, this dreadfully frightening episode ended up being a blessing in disguise. When my mother finally gained some of her strength back and was discharged from the hospital, she readily agreed to never take chemotherapy again. Any doctor, homeopaths included, is constantly faced with situations requiring the sharpest of analytic skills. Homeopathic case analysis requires recreating the chronology of events leading up to the present symptom picture. We know that no disease appears accidentally; there is a logic to the vital force, which came to the present expression based on the way in which it was “directed”. The involvement of allopaths in our patients’ care does not presuppose correct diagnosis or correct assessment of what’s really going on. Allopathic doctors are not trained to analyse the chronology of symptoms the same way homeopaths are. They do not know about Hering’s most important law – the one about former, suppressed symptoms reappearing briefly in the course of recovery. This law underscores in reverse the relevance of chronology of the case. It’s easy to forget that regular doctors don’t take into consideration the effects of suppression from medications, for example. They tend to regard all symptoms as either part of the person’s disease process, or part of a new diagnosis which seems to have fallen from the sky. There is no logic, no rhyme or reason, no red thread binding a case together from beginning to end. As frustrating as this may be, it becomes an interesting and vital challenge for us to unravel the picture and make our own conclusions.
In my mother’s case, for example, the numerous doctors who examined her during her two days at the university hospital had finally diagnosed her with “community acquired pneumonia.” In spite of this diagnosis and the fact that she was on oxygen for two days due to dyspnea and poor oxygen saturation, she was nevertheless discharged on day 3. Nothing was mentioned about this being a side effect of chemotherapy, even tough her leukocyte count was below normal and her blood chemistry had gone haywire.
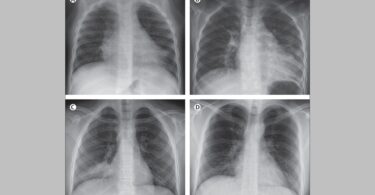
My analysis of her illness and subsequent collapse was that her condition had been suppressed by the Hydrea, and under emotional and physical stress her vital force was not able to maintain status quo. Her vital force had now shifted its center of expression to the lungs. But it was clearly not a “pneumonia”. Even speaking with her on the phone was enough for me to make different conclusions. Her voice was weak and she barely had strength to speak. Her level of consciousness was altered, she reacted slowly to questions, didn’t always understand what was being asked. She did not have a cough! Her temperature remained elevated to 103°, despite fever-reducers and antibiotics. She did not perspire. Her only complaint was, “I’m having a hard time breathing”. And, finally, there was the chest X-ray result: “Findings and impression: Grossly normal study without any acute cardiopulmonary or pleural findings.”
Notwithstanding the absence of any objective findings other than shortness of breath and fever, the university hospital held fast to the pneumonia diagnosis – and then sent her home! This is an excellent example of why the homeopath needs to absolutely question everything, as well as being an example of how allopathic and homeopathic medicine differ in their interpretations of what’s happening in the course of an illness. The first assumption of university hospital doctors, when my mother was brought in to the emergency room, was that her present symptoms represented a complication of her “main” disease (ET). Therefore they suspected a pulmonary embolism when they observed her shortness of breath. Pulmonary embolisms can happen to people with ET. Yet there was no logic, no grounds for suspecting such a diagnosis, when her platelet count had been suppressed down to normal by the Hydrea a this point. Moreover, they weren’t taking all her symptoms into account. And the most significant bit of information from her history which they completely ignored was the fact of her being on Hydrea. They ignored this information because they don’t have an understanding of the vital force, nor of the danger of suppression. There wasn’t a name, a diagnosis, for her condition – so they had to choose the next-best name in the book.
The homeopath must always take into account any medications the patient may have taken previous to the developing of symptoms. Medications all have “side effects”, which are nothing more than symptoms of their “provings”! If we prescribe based on symptoms which are “not the patient’s own”, but are rather the result of a medication, we will confuse the case. In a similar situation the medication becomes the “acute etiology” of the present symptoms. Etiologies always must be addressed. In my practice I antidote medications when it is apparent that they have created what I term a “medication-miasm”. A miasm is, after all, nothing more than a barrier to healing, a blockage which the vital force cannot overcome. Anyone can make an antidote. It is just a potentized form of the medication itself. I usually recommend one drop, or one of the tiniest possible grains, of the medicine mixed with at least 500 ml. of water, shaken at least 20-50 times, and taken by the teaspoonful every morning on an empty stomach, 5 days in a row. The mixture must be shaken before each succeeding dose. If an aggravation starts at any point, the antidote is to be discontinued. Of course, the antidote is an isopathic remedy. Antidoting medications and vaccines has proven itself to be, in my experience, an indispensable part of homeopathy practice.
We mustn’t allow ourselves to be led astray from our philosophical grounds. Philosophy is everything in medicine. It determines the way in which we understand every case. No doctor has the ethical right to treat a person without understanding the nature of the condition. When my students can’t provide me with an accurate analysis of the nature of the condition of a patient, I send them back to square one. No further speculation and certainly no repertorization is encouraged until the nature is understood. And so in order to most competently understand exactly what was happening with my mother the day she collapsed, we need to know about Hydrea.
Hydrea (hydroxyurea) is an antimetabolite. An antimetabolite is a drug that is similar enough to a natural chemical to participate in a normal biochemical reaction in cells but different enough to interfere with the normal division and functions of cells. So named because the drug inhibits a normal metabolic process. Examples of antimetabolites include 6-mercaptopurine (6MP), methotrexate, and hydroxyurea.[5] Hydrea’s list of possible side effects covers many pages. I list the most general ones here:
- Malignancies
- Embryo-fetal toxicity
- Vasculitic toxicities
- Risks with concomitant use of antiretroviral drugs
- Macrocytosis
- Reproductive System and Breast disorders: azoospermia, and oligospermia
- Gastrointestinal disorders: stomatitis, nausea, vomiting, diarrhea, and constipation
- Metabolism and Nutrition disorders: anorexia, tumor lysis syndrome
- Skin and subcutaneous tissue disorders: maculopapular rash, skin ulceration, dermatomyositis-like skin changes, peripheral and facial erythema, hyperpigmentation, atrophy of skin and nails, scaling, violet papules, and alopecia
- Renal and urinary disorders: dysuria, elevations in serum uric acid, blood urea nitrogen (BUN), and creatinine levels
- Nervous system disorders: headache, dizziness, drowsiness, disorientation, hallucinations, and convulsions
- General Disorders: fever, chills, malaise, edema, and asthenia
- Hepatobiliary disorders: elevation of hepatic enzymes, cholestasis, and hepatitis
- Respiratory disorders: diffuse pulmonary infiltrates, dyspnea, and pulmonary fibrosis. The drug is described as potentially causing cancer:
Hydroxyurea is a human carcinogen. In patients receiving long-term hydroxyurea for myeloproliferative disorders, secondary leukemia has been reported. Skin cancer has also been reported in patients receiving long-term hydroxyurea. Advise protection from sun exposure and monitor for the development of secondary malignancies.
It probably seems strange that an anti-cancer drug could be a carcinogen. From the homeopathic point of view, however, it is obvious. What can bring about healing in a minimal dose can, in high dose, causes the very symptoms one is hoping to treat. (The analogy is not entirely appropriate in relation to chemotherapy drugs, because in any case they do not cure, but only suppress symptoms). Because I studied the pathogenesis of Hydrea (i.e. possible side effects), I postulated that my mother’s shortness of breath had been brought on by the drug. What I didn’t yet know, at that moment, was the results of her computerised tomography of her lungs. In searching for a pulmonary embolism, the doctors had stumbled upon lung nodules, which had been discovered ten years previously and had hitherto not significantly changed. Now, after the Hydrea, they had changed significantly enough that the oncologist ordered another CT scan in several months to check for further changes. I knew one thing: had my mother gone back to the Hydrea, I feel certain she would have soon met her demise from one or another side effect.
The first week home she began having odd shifting pains here and there, concentrated in her upper back, and the dyspnea and tightness in her chest was still present. The physician’s assistant at her internist’s office diagnosed her with “myalgia” and sent her home. She was reminded several times that she should return to her oncologist as soon as possible, in order to resume the Hydrea. By this time my mother herself was acknowledging the absurdity of the medical system and the complete denial of reality it seemed to perpetrate. She had started talking with her doctors about homeopathy. Her oncologist fondly recalled childhood memories of growing up on homeopathy in India. “My parents treated me with remedies all the time,” she recounted. “But then when I grew up, I found science.”
In the first days after her discharge my mother antidoted the antibiotics she had been given in the emergency department and then the Hydrea – one after the other, with a break of 10 days in between; medication antidotes are always given in reverse order of that by which they were taken. A month had passed and she began taking the homeopathic remedies I had prescribed for her.
Based on the fact that ET is a cancerous or near-cancerous condition, I decided to approach her treatment the same way I do cancer cases. My approach to cancer patients – and some other cases as well – is modeled after the approach of Dr. Ramakrishnan. Two remedies are prescribed; one is a cancer nosode, and the other either covers the symptom totality of the patient (i.e. constitutional remedy), or is chosen based on the organ-specific pathogenicity of the remedy matched with that of the patient. In my mother’s case I chose Carcinosinum 200C as the cancer nosode, and Phosphorus 200C as the remedy which best covers both the totality of the disease entity and the dominant family miasm. Phosphorus is the ultimate polychrest for bone (including marrow), blood, liver (where erythropoietin and thrombopoietin are made), and lungs. Phosphorus is also a great tubercular remedy. She took the remedies in the following manner: at the beginning of the week she dissolved three pellets of one of the remedies in 200 ml. of water, and took one teaspoonful per day, three days in a row. Before each one she shook the container 20-30 times. The next week she followed the same procedure for the second remedy and so on.
My mother started feeling better immediately and her wandering aches and pains disappeared within the first two weeks of the homeopathic treatment. Her doctor checked her platelet level monthly. The level had gone up to over 800,000 x 109/L after the hospital stay when she discontinued the Hydrea. She continued taking the remedies week after week, and every month her platelet count dropped by approximately 25,000. She continued seeing her oncologist at university hospitals and clinics once a month, and at each visit she discussed her homeopathic treatment, and at each visit the oncologist urged her to return to the Hydrea, the improvement in her platelet count notwithstanding. After a few months I persuaded her to change oncologists. The new oncologist, from a different hospital, agreed with my assessment that her risk factors did not warrant taking Hydrea. By the time the platelet count had dropped to 600,000, she was told she was nearly cured, and wouldn’t need to check the level so frequently.
My mother stopped taking the remedies after about 10 months. She continues to feel well. This case taught me a lot. Treating your loved ones is not usually recommended because we tend to feel too strongly. Our judgment can be clouded by our emotions. On the other hand, our emotions – also products of the vital force – can be a healing factor in themselves and can aid us in our work. Being my mother’s homeopath initiated a group process since homeopathy is controversial for most and every family member participated in the treatment. All of my siblings and my father took a deep interest in understanding the case from a homeopathic point of view. We achieved complete family consensus about my mother’s treatment thanks to the determination of each person. Ultimately, I feel the family as a whole was made healthier through the experience, and it confirmed how important the principle of interconnectedness is, not only within the patient herself, but between the patient and her loved ones.
When my mother’s platelet levels had come down and her oncologist pronounced her “nearly cured”, she decided – unbeknownst to me – to stop taking the remedies. When she returned to her oncologist for her platelet count check after three months, the level had once again shot up to over 800,000. At this point she called me and reported with an ironic kind of ecstasy that she has good news. She exclaimed joyfully, “Homeopathy works!” She was also absolutely thrilled that her oncologist’s only recommendation was to “go back to doing whatever it was you were doing, because it was working!” She once again started taking the remedies as prescribed. Three weeks passed and she had another platelet count check. After just three weeks on the remedies the count had gone down by 20,000. Her oncologist was satisfied and recommended she just “stay on the homeopathy.”
Second malignancies in patients with essential thrombocythaemia treated with busulphan and hydroxyurea: long-term follow-up of a randomized clinical trial.Br J Haematol. 2000 Sep;110(3):577-83.https://www.ncbi.nlm.nih.gov/pubmed/10997967
Efficacy and safety of hydroxyurea in patients with essential thrombocythemia.Pathol Biol (Paris). 2001 Mar;49(2):167-9.https://www.ncbi.nlm.nih.gov/pubmed/11317964
[1] Landgren O, Goldin LR, Kristinsson SY, Helgadottir EA, Samuelsson J, and Björkholm M (2008) Increased risk of polycythemia vera, essential thrombocythemia, and myelofibrosis among 24,577 first-degree relatives of 11,039 patients with myeloproliferative neoplasms in Sweden. Blood 112:2199–2204.
[2] Jones AV, Chase A, Silver RT, et al. (2009) JAK2 haplotype is a major risk factor for the development of myeloproliferative neoplasms. Nat Genet 41:446–449.
[3] Management of essential thrombocythemia, Francisco Cervantes, Hematology Department, Hospital Clinic, University of Barcelona, Barcelona, Spain, doi: 10.1182/asheducation-2011.1.215 ASH Education Book December 10, 2011 vol. 2011 no. 1 215-221
[4] ibid.




Excellent case with excellent explanation and interpretation! Thank you, Molly!
Hello Firuzi, Can you suggest good Homeopathy support in Nashik for ET.
Many thanks
Hi Molly,
Very interesting and I’m very interested also in using homeopathy to treat my newly diagnosed ET. Do you have any connections with recommended homeopaths in Australia.
Thanks!
Dee
Hello Dee, Sorry, don’t know ant homeopaths in Australia. Wish you luck.
My 17 year old son was just diagnosed with ET. Would this protocol work for him? I am fairly familiar with homeopathy, but I feel over my head with this. He takes 1 low dose aspirin daily. Any suggestions? We are in WA state.
I hope Molly sees your comment. I’m dismayed that she has, apparently, no contact information! I can only say that the daily dose of Aspirin worries me and that you might be able to substitute one softgel a day of Vitamin E Complex, 400 I.U. as it acts as a blood thinner.
Hello Danene,
I wouldn’t recommend any particular protocol but instead it’s always vital to take the individual case. That’s what homeopathic treatment is about. If I were you, I’d recommend first finding a classical homeopath and having a conversation about it. See whether your heart resonates with his or her philosophical approach to the disease and to the person. And then you can decide whether to start treatment. All the best!
Such an interesting article! “Antidoting medications and vaccines has proven itself to be, in my experience, an indispensable part of homeopathy practice.” This is so true! As Robin Murphy always says, “We have to learn to become antidoters.”
Yes Elaine, in our medication-inundated world we can hardly do without antidoting these medicine-miasms that are formed.
Hi! And the third, the fourth, the fifth week? Did she alternately take Carcinosinum 200C and Phosphorus 200C every week, during the first three days of the week? Sorry, I don’t think I write well in English. I hope you can understand me. Regards!
Yes Juan, that is correct. One week she took one remedy for 3 days, and the next week the second remedy for three days.
Hi Molly, I just read your article. Very interesting indeed and I loved your proactive approach of finding a solution to a problem using knowledge that you had. Brilliant. As well as changing doctors. In the new Covid 19 world would you consider working with someone remotely over the net. I was diagnosed with ET Jak2 March this year and would interested in using Homeopathy to help control this disease. Many thanks B
Hello B, Thank you for your feedback. Sorry for the delayed response! Yes, all of my consultations are now online. If you need more information, please write me an email at [email protected]
Hello Molly, Just gone through the article and found it very informatic. Great explanation which is supporting to think differently. I was also diagnosed by ET in Dec 2019. Now I have been advised to take everyday Aspirin 150 mg. Regularly monitoring CBC , currently my manual platelet count is 5.25 lacs.
Interested in going for Homeopathy treatment, Pl suggest further.
Hello Dsp, classical homeopathic treatment should help you to keep your platelet counts from going too high. If you can find a homeopath in your area, I recommend consulting with them. If you need further recommendations feel free to email me. [email protected]
I have ET and i have borderline high platelets (380-490) but the number of platelets can not define the cure! Every month or even every day change in numbers. Only a bone marrow biopsy can confirm if the disease is cured or not. So, although i have just started homeopathy, i would like you to explain me what exactly do you mean please. Thank you very much
Marian, yes, you are exactly right, the number of platelets cannot define the cure. The cure must be assessed by the overall improvement in well-being. In the case of ET though I do believe that a reduction in the number of platelets should accompany the cure. In other words, if your overall condition improves (mood, energy, sleep, and so on) but meanwhile your counts go up, it might indicate a temporary aggravation. In such a situation it would be good to wait and see if the counts go down again after a few months. It’s not a simple disease to treat by any method and the person needs to consult regularly with the homeopath until long-term improvement is seen.
Dear Molly , my daughter has similar situation , diagnosed with ET ( JAK-2 mutation. Please help !!! Do you know a good homeopathic doctor in Los Angeles or nearby.
Hi Marina, personally I don’t know any homeopaths in California, but you could try checking the NASH site and speaking with a few over the phone. http://homeopathy.org/registered-homeopaths-directory/?cn-s=&cn-cat=9
I’d say you should choose someone with whom you resonate intuitively and can have an open trusting conversation. I’d look for only very experienced people. Best wishes!!!
What significance did you see in the age, nationality and gender if the doctor who prescribed your mother’s initial treatment? I’m wondering why you mentioned it .
Catherine, you ask a very pertinent question, which I hadn’t explained in the article.
This same oncologist I mention later, saying,
“She had started talking with her doctors about homeopathy. Her oncologist fondly recalled childhood memories of growing up on homeopathy in India. “My parents treated me with remedies all the time,” she recounted. “But then when I grew up, I found science.””
There are several reasons to include details like this in a case story. The first is that every case IS a story, and details are important because nothing happens by accident. Every element in a case both influences and is influenced by every other element, changing the totality.
The second reason to mention details is because none of us is removed from the law of similars. We attract specific people, situations and disease to ourselves vis this law with the help of the vital force, and all for the purpose of maximum harmony within the given constraints.
I find it profoundly interesting that my mother attracted to herself a woman doctor from India who had grown up with homeopathy but later rejected it. This combination reflected my mother’s own consciousness at that moment: she had been torn between inherent trust toward me as her daughter (and toward homeopathy by default!), and her own relatively “scientific” worldview. The next oncologist to treat her influenced the story in his own ways as well, as was no less amazing in terms of his specifics!
My husband has high platelet count of 8 lacs . We wish to go in for homeopathy treatment with dr Shankaran in India and overcome this . Feel very encouraged with ur treatment for mom . God bless u
My wife is also having ET and her platlet count was 800000 when tested in November 2019. Since then she is one capsule Hydroxy Urea 500mg. Now her TLC has started decreasing below normal count. Now how can I take homeopaathic treatment.
Dear Molly, Thanks for sharing this detailed story. Really helped me build the confidence that homeopathy has a possible cure for ET. My wife, 38yrs old, has ET with JAK2 V617F Mutation. We only diagnosed this 2 years ago in May 2021. Since then her platelets count have been in the 720k-780k range. But when we trace back her old pathology reports we could see the progression it being 500k in April 2015 and gradually progressing till 700k bracket in last 6-8 years. She has been resisting to take any allopathy medicines and only recently started taking Aspirin intermittently. We live in Delhi, India. Would you be able to refer us to a good homeopath doctor in Delhi or guide us with the treatment on this remotely ? Appreciate your help. Thanks
Hello dear Molly , I have red your article few months ago and I want to thank you for giving hopes by posting your mom story ,as I have exactly the same Disease with your ´mother, I couldn’t find myself taking the hydrea , as my immune is already super weak because of the high platelets count , now I have almost 2 months taking the homeopathy believe me i start feeling much better no pain on my bones , no pain in teeth ,no fatigue or dizziness , the only thing I’m facing is I feel sometimes little bit ache on my spleen , sooner I will be going to the doctor to check about it … all my médecine is a sort of pills only I take thrice a day .. and Beverly skipped one day ..
Hi Molly,
My mother suffers from ET and the drs are killing her with hydrea. She just went off it and feels better in a couple days so it’s definitely the hydrea. She is 86 yes old. We want to try your remedy with her. Her platelets have never been above 1,000,000 and her hemotologist has been apparently treating her very aggressively for the past 10 years. It has taking a toll on her and we need a different remedy. Her dr has taken her off the hydrea and is going to check her blood weekly so it seems the perfect time to try this. Do you agree?
Hi Tara,
Yes indeed Hydrea is quite toxic and with your mother being 86 and platelet counts under 1,000,000–I wouldn’t hesitate to take her off it. It would be ideal though if you and she could come to an agreement with her oncologist, so that her blood can continue to be monitored and it become a collaborative effort. I would predict that they won’t need to check weekly, but less frequently.
Meanwhile, while she reduces the drug over the course of a month or so, she can take the antidote daily. This should ease the side effects. That’s done by taking the tiniest grain of the drug and mixing it in 500 ml of water, storing in the refrigerator and taking one teaspoonful every morning on an empty stomach. She should shake the bottle about 20 times before each dose.
I hope this helps.