ABSTRACT: A case of Hyperhidrosis in a paediatric patient treated with homoeopathiccConstitutional remedy based on symptom similarity.
KEY WORDS: Hyperhidrosis, Paediatric, Constitution
INTRODUCTION: Hyperhidrosis is defined as abnormally excessive sweating involving the extremities, underarms and face, usually unrelated to body temperature or exercise. It is the excessive secretion of the eccrine sweat glands in response to stimuli like heat.
Hyperhidrosis is classified into primary, which is idiopathic essential and secondary which is in response to several other diseases and drugs. Primary or essential hyperhidrosis affects around 0.6% to 1.0% population. Primary hyperhidrosis may be inherited and its symptoms may manifest during adolescence.
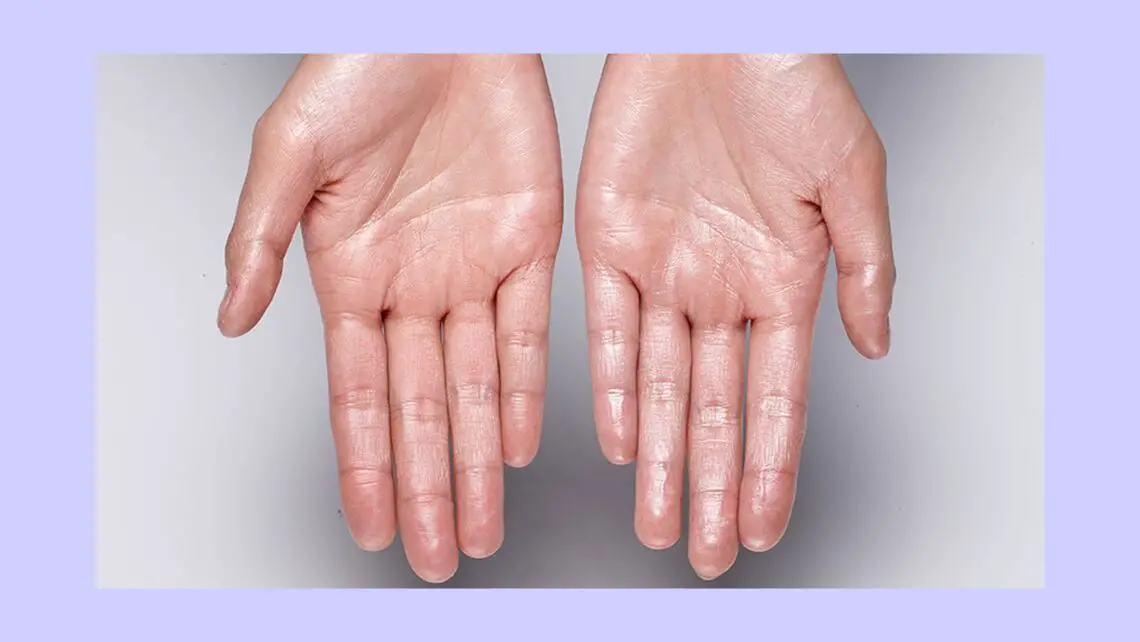
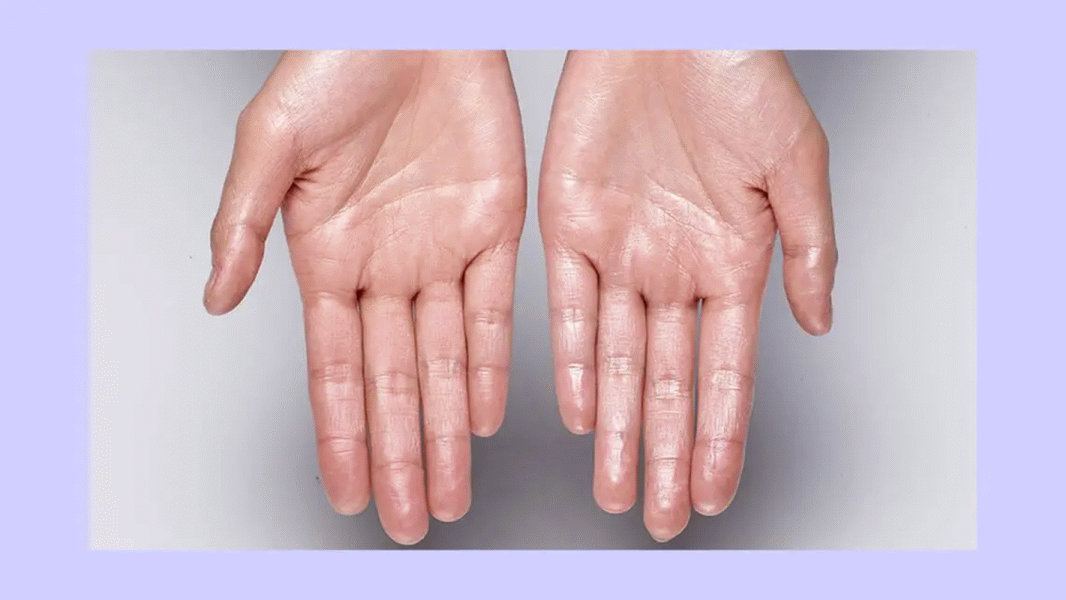
The main mechanism behind primary hyperhidrosis is the excessive stimulation of the sweat centres of the hypothalamus in response to emotion leading to increased secretory activity of the eccrine sweat glands of the palms and soles. The patient presents with excessive perspiration of palms, feet and sometimes axilla, pale or bluish appearance of the palms and feet, unusual softening of the skin and feet may become cracked or scaly, occasionally staining of garments.
Primary hyperhidrosis is usually clinically diagnosed after ruling out other possible disorders related to secondary hyperhidrosis.
CASE HISTORY:
A 17 year-old female presented with the complaint of profuse offensive perspiration of the bilateral palms and soles since childhood, which was worse the last 3 years. The complaints started gradually and progressed slowly. The complaints increased when meeting new people and during the evenings. She also had cough with scanty whitish expectoration the last month which started after having cold food. Cough increased during the evening.
PAST HISTORY: Nothing significant
FAMLIY HISTORY: Nothing Significant
TREATMENT HISTORY: None taken
PATIENT AS A PERSON:
Appearance: lean, fair, moderately nourished
Appetite: Good
Thirst: Less – 1 litre /day, warm water
Desire: Sweets2+ Chicken1+
Bowel: Once/day, normal
Bladder: 4 times/ day
Sleep: Good, 10pm- 6am
Thermal: Chilly
MENSTRUAL HISTORY: F.M.P: 15years of age L.M.P: 10/11/19
Regular cycle, 5/28 days, abdominal cramps before menses.
LIFE SPACE INVESIGATION:
Patient hails from a middle socioeconomic family. She is in her pre-university (12th grade in Karnataka). She is a very timid person who is also anxious meeting strangers. At home she has a good relationship with her family. She is afraid of performing on the stage and has participated only in 1 group dance, during which she refused to go on stage and then was convinced and did it. She gets angry if people don’t consider her opinion and she will stop talking to them.
GENERAL PHYSICAL EXAMINATION:
Moderately built and moderately nourished.
Well oriented with time, place and person.
No signs of pallor, icterus, cyanosis, clubbing, lymphadenopathy or oedema.
RESPIRATORY SYSTEM:
Left turbinate hypertrophied. Normal vesicular breath sounds.
LOCAL EXAMINATION OF PALMS AND SOLES:
Skin is soft and moist, palms are cold to touch.
DIAGNOSIS: 1. Primary Palmoplantar Hyperhidrosis with a score of 4 according to Hyperhidrosis Disease Severity Score (HDSS).
2. Upper respiratory tract infection
HOMOEOPATHIC MANAGEMENT:
Constitutional totality:
Anger easily
Nervous on meeting strangers
Craving sweets and chicken
Increased perspiration of bilateral palms and soles
Chilly patient
Offensive perspiration
< evening
< strangers with
Cough with whitish expectoration
< Evening
PRESCRIPTION: 3/12/2019
- Silicea 200 – 2P – weekly at bedtime
- 2 pills – 4-4-4 for 2 weeks
| S.NO | DATE | FOLLOW UP | PRESCRIPTION |
| 1. | 17/12/2019 | C/o profuse perspiration slightly better on the palms, on the soles – same.
Offensiveness- better C/o Cough absent. All other generals good |
1. Silicea 1M (1P) HS
2. No.2 pills 4-0-4 for 2 weeks |
| 2. | 7/01/2020 | C/o profuse in B/l palms better, soles- same. All other generals good | 1. SL (1P) HS
2. No.2 pills 4-0-4 for 2 weeks |
| 3. | 28/01/2020 | C/o Profuse perspiration on B/l soles – better
C/o Coldness of extremities All other generals good |
1. Silicea 1M (2P)
1P HS alternate weekly 2. No.2 pills 4-0-4 for 1 month |
| 4. | 25/02/2020 | C/o perspiration of B/l palms and soles – 80% better
Hyperhidrosis Disease Severity Score – 1 C/o coldness of extremities – reduced All other generals are good |
1. Silicea 1M(1P) HS
2. No.2 pills 4-0-4 for 2 weeks |
The patient was contacted on by phone on 11/01/2021 and she said that her perspiration had completely reduced on her bilateral palms and soles. Coldness of extremities was absent and the score according to hyperhidrosis disease severity is 1. She is able to do her day to day activities.
CONCLUSION: Patient Ms. K came with the complaint of profuse perspiration of B/l palms and soles. The case was diagnosed as primary palmoplantar hyperhidrosis. Silicea 200 was prescribed as her constitutional remedy and potency was raised from 200 to 1M. Patient was better by 80% with the medicine as observed through the follow ups.
ACKNOWLEDGEMENT: I would like to express my gratitude to Dr Jolly D’Mello, Assisstant Professor of Department of Physiology and Biochemistry and Unit- II physician of the Paediatric OPD, Father Muller Homoeopathic Medical College and Hospital for her constant support and encouragement.
BIBLIOGRAPHY:
- Stolman L. TREATMENT OF HYPERHIDROSIS. Dermatologic Clinics. 1998;16(4):863-869.
- Lakraj AA, Moghimi N, Jabbari B. Hyperhidrosis: anatomy, pathophysiology and treatment with emphasis on the role of botulinum toxins. Toxins. 2013 Apr;5(4):821-40.
- Hahnemann S, Boericke W, Dudgeon R. Organon of medicine. New Delhi: B. Jain Publishers; 2011.
- Dhawale M.L. Principles and Practice of Homoeopathy part 1. 2nd Bombay. Institute of Clinical Research. 1994.
- Solish N, Bertucci V, Dansereau A, HONG HC, Lynde C, Lupin M, Smith KC, Storwick G. A comprehensive approach to the recognition, diagnosis, and severity‐based treatment of focal hyperhidrosis: recommendations of the Canadian Hyperhidrosis Advisory Committee. Dermatologic Surgery. 2007 Aug;33(8):908-23.