Part I- Regarding Hemangioendothelioma
Summary
The term hemangioendothelioma describes several types of vascular neoplasms and includes both non-cancerous (benign) and cancerous (malignant) growths. The term has also been applied to those that show “borderline” behavior, intermediate between entirely benign hemangiomas and highly malignant angiosarcomas.
Hemangioendotheliomas are caused by abnormal growth of blood vessel cells, although the exact underlying cause for the abnormal growth is unknown. They can also develop in an organ, such as the liver or lung. They usually grow slowly and can sometimes spread to other tissues in the body (metastasize).
Examples of types of hemangioendotheliomas include spindle cell hemangioma; papillary intralymphatic (Dabska tumor); retiform; kaposiform; epithelioid; pseudomyogenic (epithelioid sarcoma-like hemangioendothelioma); and composite. Treatment depends on the type of hemangioendothelioma present but typically includes surgical excision (removal).
Conventional Treatment
Treatment for hemangioendothelioma may depend on the type of hemangioendothelioma present in the affected individual and the risk of recurrence or metastases. In most reported cases, surgical excision (removal) of the mass has been the only treatment.
For spindle cell hemangioma, simple excision is reportedly curative; however, new growths develop in adjacent skin and soft tissues in 60% of affected individuals. For individuals with papillary intralymphatic angioendothelioma (PILA), excision of the involved lymph nodes, as well as the mass, has been recommended.
Surgical excision is reportedly also the usual treatment for individuals with retiform hemangioendothelioma (although local recurrence with this type is common), epithelioid hemangioendothelioma, and composite hemangioendothelioma (with the exception of 1 case treated with interferon).
Most individuals with pseudomyogenic hemangioendothelioma have been treated with simple excision, but a few individuals have also received post-surgical radiotherapy (RT).
With regard to kaposiform hemangioendothelioma, some large lesions cannot be completely removed and may cause fatal complications due to the associated Kasabach–Merritt syndrome. In these cases, several medical therapies have been used, including systemic corticosteroids; alfa interferon; RT; embolization; and several other therapies, both alone and in various combinations.
Prognosis
The long-term outlook (prognosis) for individuals with hemangioendothelioma is not predictable and differs among affected individuals. The prognosis in each case depends on the type of hemangioendothelioma present, the risk of recurrence and whether the condition has metastasized (spread) to nearby tissues or other parts of the body.
For example, although surgical removal of lesions of spindle cell hemangioendothelioma is considered curative, new masses develop in adjacent skin and soft tissues in 60% of the cases. Likewise, for individuals with retiform hemangioendothelioma, local recurrence is common but metastatic disease is rare.
On the other hand, a follow-up study of 30 patients with cutaneous epithelioid hemangioendothelioma showed that 21% of the affected individuals developed systemic metastases, and 17% of these patients died as a consequence. Survival rates in the literature for individuals with hemangioendothelioma generally range from 62% to 83% and local control rates (stopping cancer growth at the site of origin) range from 80% to 100%.
Epidemiology
- Wide age range (0 – 93 years)
- Usually adults, 60% women)
Sites
- Any location
- Most commonly: soft tissue, bone, lung, skin and liver
- Often multifocal: bone and visceral lesions
- In up to 50% of cases, closely associated with or arising from a vein
Pathophysiology
- Gene fusion driven.
- Unclear
Clinical features
- Clinical presentation depends on the tumor location, most frequently pain
- If arising from a vein, occurring symptoms caused by vascular occlusion, such as edema or thrombophlebitis
- Recurs locally, may metastasize (usually to lymph nodes and lungs)
Diagnosis
Diagnostic workup includes radiology, histology (biopsy, resection) with immunohistochemistry and molecular analysis
* https://rarediseases.info.nih.gov/diseases/6557/hemangioendothelioma
PART II- DETAILS OF THE CASE.
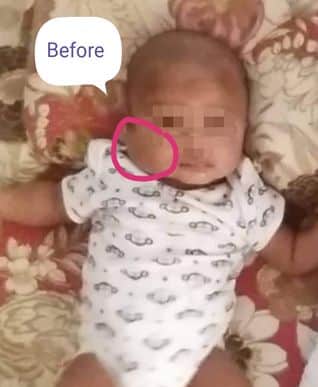
Introduction. A relative of mine stays in London, UK. They have two issues, one girl 6 years of age and a boy of 6 months. The parents and near relatives were anxious about the boy’s health, because a swelling/ tumour appeared in the second week of his birth; on the right side of his face, (parotid swelling type), which was increasing in size gradually.
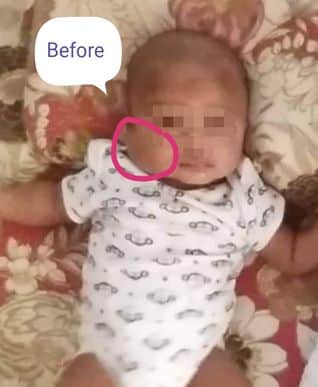
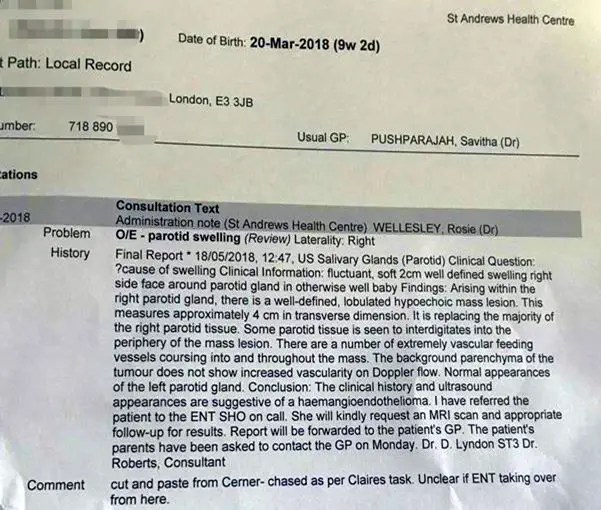
The boy was shown to local health centre, “St. Andrew, Health Centre. London”; who gave him treatment with medicine by injection. They diagnosed the case to be “Epithelioid hemangioendothelioma”.
They visited Bangladesh when the boy was 6 months old. The parents did not have any confidence in homeopathic treatment. I had to convince the father, showing the complicated cases cured by homeopathy. Ultimately he agreed to try remedies for a month only.
CASE TAKING
The following information were collected:
Master. Rahman
Age – 05 months.
Family H/O of disease:
Father – Sycotic.
Mother – Syphilitic. Cold allergy
Sister – Tubercular. Cold allergy
Maternal Grand Mother: Asthma.
P/ Grand Father- Died of stroke.
Maternal Grand Father: Heart Disease.
P/ Grand Mother – Arthritis
The boy only suffers from occasional cold affection. Did not have any other remarkable difficulties/ symptoms.
The following symptoms were considered:
- Disease Tumours general, haemangioma of face.
- Irritable
- Obstinate
- Alternating moods
- Family history of sycotic, syphilis and tubercular miasm.
Result of Repertorization:
- Kreos . 2. Abrot 3. Cham. 4. Cina. 5. Ant C. 6. Sanic
Rxs:
Abrotanum
In order to counter the miasmatics, Medorrhinum and Thuja were considered. To counter any malignancy and the metastatic character of the hemangioendothelioma, Carcinosin was considered.
As the patient was staying at Dinajpur then, I suggested the father buy the remedies in centesimal potency.
25/09/2018
Abrotanum 30. 2 pills 4 times a day. For 7 days.
Result: Size of the tumour seems to be reducing, moods also improving.
- Thuja 2 pills, 4 times a day for next 5 days.
Result: size of the tumour has reduced, moods improved further.
- Medorrhinum Twice a day for next 5 days.
Result: Size of the tumour seems to be reduced by 40%, moods much better.
- Carcinosin 200. Twice for next 5 days.
Result: Size of the tumour seems to be reduced by 60%, moods also improving.
19/10/2018 The same course was repeated, when the face became normal in size.
12/11/2018 Then, a course of increased potency was given.
RESULT: The boy got rid of the tumour 100% by the end of the 2nd course i.e before 12, Nov. 2018. Only one course was repeated later. No follow up was done because they went back to London in mid-November 2018. Moreover, there was no return of the tumour to this day.