Amoebiasis is worldwide parasitic disease that is especially prevalent in the tropical countries. More than 10% of the population of the world is estimated to be suffering from E. histolytica infection; the prevalence of infection is about 50% in the underdeveloped areas lacking facilities of basic sanitation; 90-99% of infections are asymptomatic.
Agent
E. histolytica, the agent of Amoebiasis, occurs in two stages; a motile trophozoites stage and a nonmotile cystic stage. The trophozoite is found in the intestinal and extra intestinal lesions, and in diarrhoeal stools, the cyst is mostly present in non diarrhoeal stools of patients of Amoebiasis.
The trophozoite is unicellular protozol parasite belonging to the class Rhizopoda. It ranges from 10 to 60 µ in size with an average of 25 µ. It has no definite form; it keeps on changing its shape by throwing pseudopodia that help in locomotion; its nucleus is spherical and its cytoplasm is clearly divisible into translucent ectoplasm and granular endoplasm.
The cyst is spherical in shape and is surrounded by a cyst wall. A mature cyst contains four nuclei and a clear hyaline cytoplasm. The trophozoite cannot survive outside the human host; it degenerates with minutes. The cysts can survive in moist stools for weeks or months but cannot resist desiccation. The cysts are killed readily by boiling but not by chlorination; they are, however, removed by filtration of water.
Reservoir and source
Reservoir is human, an infected person suffering from the disease or an asymptomatic carrier discharging eggs in stools. Sources are water or food contaminated by excreta of patient or carries containing the cysts of E. histolytica.
Transmission process
Amoebiasis being a fecal oral infection, the portal of exit is the fecal route and the portal of entry, the oral route. Transmission of infection can occur by contaminated food, drink or water (vehicle borne transmission); homosexual practices (contact borne transmission); or infected houseflies and cockroaches (vector borne transmission). Poverty, ignorance, unhygienic living conditions and insanitary latrines promote the transmission of excremental disease including Amoebiasis.
Incubation period
Incubation period may extend from few days to few months. It is commonly 3-4 weeks.
Clinical features
The incubation period may range from a few days to many years. Amoebiasis is one of several “tropical” diseases that can have a prolonged latent period and may be present more than a decade following exposure
Pathophysiology
Amoebiasis is a parasitic disease caused by the organism, Entamoeba histolytica. It is the second leading cause of death from parasitic disease in the world. Infection involves ingestion of cysts in focally contaminated food or water. These cysts pass through the gastrointestinal tract. These cysts may then be excreted in stool, completing the life cycle.
Amebic invasion into sub mucosal tissue is the sinequa non of amoebic colitis. Amoebiasis involves two genetically distinct organisms: Entamoeba dispar, which causes no disease or mucosal invasion, and E. histolytica, which is the pathogenic form. E. histolytica causes amebic colitis and extra intestinal Amoebiasis. Although most cases of Amoebiasis involve infection via ingestion of contaminated food or water, there is a high rate of infection among men who have sex with men, who transmit the infection via oral and anal sex, as well as via contaminated enema devices.
Diagnosis
Any exudates should be examined at once under the microscope for motile trophozoites containing red blood cells. Movements cease rapidly as the stool preparation cools. Sigmoidoscopy may reveal typical flash shaped ulcers, which should be scraped and examined immediately for E. histolytica. Several stools may need to be examined in chronic Amoebiasis before cysts are found. In endemic areas one third of the populations are symptomless passes of amoebic cysts.
Antibodies are detectable by immunofluorescence in over 95% of patients with hepatic Amoebiasis and intestinal amoeboma but in only about 60% of dysenteric Amoebiasis.
Clinical Complications
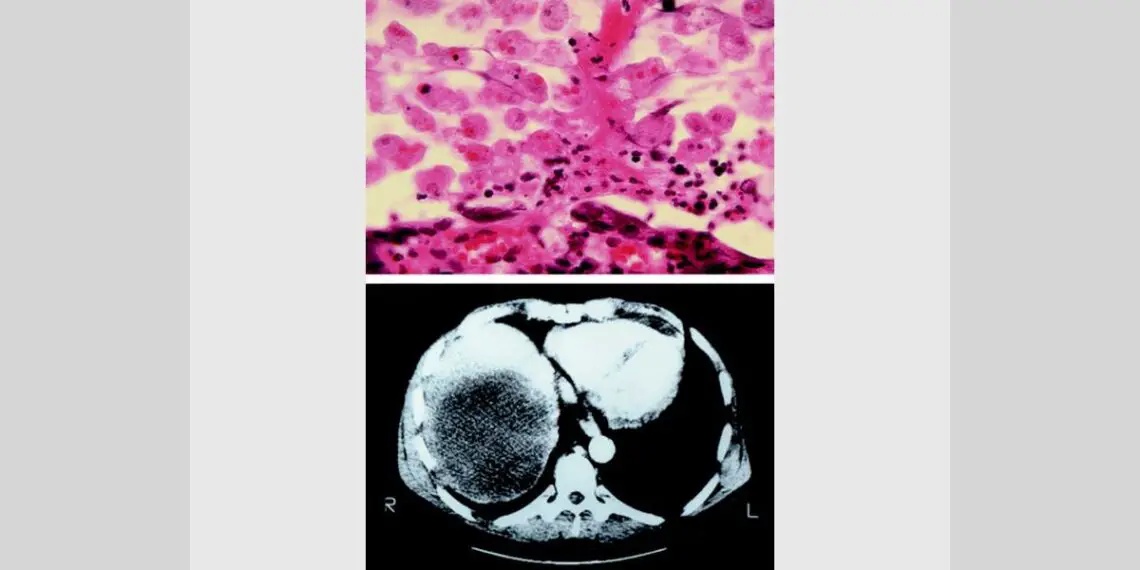
Complications include the development of intra-abdominal abscesses, liver abscess, brain abscess, amoebic liver abscess rupture through the diaphragm (causing empyema and fistulas), rectovaginal fistulas, Perianal disease, and bacterial super-infections.
Control and prevention
Control and prevention is by personal hygiene, food hygiene and the proper provision of water and sanitation. San filtration, especially if it is combined with alum flocculation, removes cysts from water supplies. A high concentration of chlorine is required to kill cysts, 3.5 parts million (ppm) residual, although they are more sensitive to iodine.
Treatment
Treatment of all stages of the disease is by metronidazole 2.4g daily in an undivided dose for 3 days or 2g daily for 5 days, or by other derivatives of the 5-nitroimidazole group of compounds (tinidazole, ornidazole and nimorazole).
Homeopathic treatment of Amoebiasis – Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathy is not only to treat Amoebiasis but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to cure Amoebiasis that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. There are following remedies which are helpful in the treatment of Amoebiasis:
Aconite, Arsenic, Lachesis, Sulphur, Baptesia, Colchicum, Podophyllum, Nux Vomica and many other medicines.
Reference:
Dhaar: Foundation of Community Medicine, 2/e; 461
Michael l. Greenberg: Greenberg’s text atlas of emergency medicine; 2005; 732
G. V. Gill: Lecture notes: Tropical medicine; 2009; 186
Nicholas A. Boon, Sir Stanley Davidson: Davidson’s principles and practice of medicine; 2006; 358
Roger Webber: Communication disease epidemiology and control: a global perspective; 2009; 89-90





Avery good and descriptive information. Thanks sarmaji