Are you looking for a homeopathic cure for slipped disk? This article discusses the homeopathy treatment of slipped disk along with the best homeopathic medicine for slipped disk treatment.
What is slipped disk?
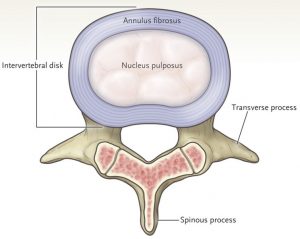 The disks are pads of tissue situated between each of the vertebrae that make up the spinal column. Each disk consists of a tough, fibrous outer ring called the annulus fibrous and a softer, jellylike inner layer called the nucleus pulpous. The function of the disk is to act as both a strong connection between the vertebrae and a cushion to absorb weight on the spinal column.
The disks are pads of tissue situated between each of the vertebrae that make up the spinal column. Each disk consists of a tough, fibrous outer ring called the annulus fibrous and a softer, jellylike inner layer called the nucleus pulpous. The function of the disk is to act as both a strong connection between the vertebrae and a cushion to absorb weight on the spinal column.
A slipped disk does not really slip; the tough outer fibrous ring (annulus) cracks open and the softer inner layer protrudes (prolapse) through the crack, like toothpaste coming out through a crack in a toothpaste tube. For this reason doctors prefer to speak of a disk prolapse rather than a slipped disk.
The disk begins to prolapse when a crack develops in its tough outer ring. This is usually the effect of wear and tear in the back as a result of normal aging. One particularly heavy or awkward lift, a fall, or even a sudden cough or sneeze may force some of the soft disk nucleus to prolapsed, leading to sudden prolapse.
The nucleus of a disk is softest and most jelly like during childhood. Over the years the nucleus gradually dries out so that by middle age it has a consistency similar to crab-meat. As someone gets older, the nucleus becomes even firmer. In elderly people the disk is mainly a section of scar tissue; this accounts for the fact that old people lose height.
Slipped disk occurs less frequently as people get older; it is a disorder affecting young adults and people in early middle age. Disk protrusion occurs where the outer layer of the disk is weakest; that is, just in front of the nerve roots, which emerge from the spinal cord at each vertebral level. There is very little free space within the spinal canal, and the protruding disk material presses on the nerve root at that level and causes the painful symptoms of a slipped disk.
The area of the spine most likely to be affected is the lowermost part of the back. Here the greatest strains occur, and it is not surprising that most disks that fail are at this level. However, it is possible for disks to prolapse at any level along the length of the spinal column – in the back or the neck.
Homeopathic treatment of slipped disk
 Homeopathy is one of the most popular holistic systems of medicine. The selection of homeopathic medicine for slipped disk is based upon the theory of individualization and symptoms similarity by using a holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathic medicine for slipped disk is not only to treat slipped disk but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to treat slipped disk that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. These are the remedies which are most often helpful in the treatment of slipped disk:
Homeopathy is one of the most popular holistic systems of medicine. The selection of homeopathic medicine for slipped disk is based upon the theory of individualization and symptoms similarity by using a holistic approach. This is the only way through which a state of complete health can be regained by removing all the sign and symptoms from which the patient is suffering. The aim of homeopathic medicine for slipped disk is not only to treat slipped disk but to address its underlying cause and individual susceptibility. As far as therapeutic medication is concerned, several remedies are available to treat slipped disk that can be selected on the basis of cause, sensations and modalities of the complaints. For individualized remedy selection and treatment, the patient should consult a qualified homeopathic doctor in person. These are the remedies which are most often helpful in the treatment of slipped disk:
Commonly indicated homeopathy medicines for Prolapsed Intervertebral Disc
- Bryonia
- Rhus tox
- Kali carb
- Phosphorus
- Sepia
- Lachesis
- Thuja occidentalis
- Ruta
- Calcarea carb
- Cimicifuga
- China officinalis
- Natrum mur
- Pulsatilla
- Kalmia
- Ledum pal
- Medorrhinum
- Calcarea phos
Bryonia
- Homeopathic medicine for slipped disk having cramp-like pain all over the back.
- Shootings pain in the loins and in the back.
- Painful stiffness in the small of the back, compelling him to walk and sit crookedly.
- Shootings under the left shoulder-blade, extending to the heart, greatly aggravated by cough and respiration.
- Bryonia patients are irritable, inclined to be vehement and angry
- Pains: stitching, tearing, worse at night, by motion, inspiration, coughing and better by absolute rest, lying on painful side.
- Excessive dryness of mucous membranes of entire body.
Calc carb.
- Pain in the back. Intolerable pain in the back.
- The spine pains on bending backward.
- Painful stiffness in the spine, with dullness and heaviness in the legs, in the morning on waking, and after rising.
- Pain as if wrenched in both sides of the back. Stitches in the back.
- Bruised pain in the back and chest.
- Spasmodic, jerking pain, extending from the left side of the back to the anus. Painful jerks in the right side of the back, on breathing, with chilliness, and cold.
- Pressive pain in the spine, between the shoulder-blades, with short breath and aggravated by breathing, with painfulness in the bones of the spine on touch.
Kali carb.
- Homeopathic medicine for slipped disk having stiffness in the back, unable to stoop.
- Stiffness and lameness in the back, and small of the back.
- Rheumatic pains in the back, chest, shoulders and arms, worse on moving them.
- Attack of pain in the back, during rest, after physical effort. Violent backache. Pressure in the spine when swallowing.
- Pain in the back as from a sprain.
- Stitches in the right side of the back, extending through the chest.
- Burning tearing near the right side of the spine.
- Bruised pain in the back, during rest, not during motion.
Lachesis
 Burning in back. Spasms in muscles of back.
Burning in back. Spasms in muscles of back.
- Painful stiffness from loins to hip, as if muscles were too short.
- Insupportable nocturnal pains in back, in loins, hip and knee.
- Pain in the small of back, with constipation, intermittent fever, palpitation of the heart or dyspnoea.
- Pain in the coccyx, when sitting down patient feels as if sitting on something sharp.
- Want of strength in back and knees, which forces patient to stoop when walking.
- Pain, as from dislocation, in loins, as after great exertion.
Phosphorus
- Homeopathic medicine for slipped disk having paralyzed sensation in upper sacrum and lower lumbar vertebrae.
- Contusive pain in loins and back (as if back were broken), especially after having been seated a long time, hindering walking, rising up, or making the least movement.
- Pain and burning in small of the back when rising from stooping position.
- Pain in coccyx impeding easy motion, can find no comfortable position, followed by painful stiffness of nape.
- Oversensitiveness of all the senses to external impressions, light, noise, odors, touch.
- Restless, fidgety; moves continually, cannot sit or stand still a moment.
- Burning in spots along the spine, between the scapulae or intense heat running up the back.
Rhus tox
- Rheumatic tearing between shoulders, not affected by movement, worse by cold, better by heat.

- Pain in small of back when sitting still or when lying: better when lying on something hard or from exercise.
- Complaints from spraining or straining a single part, muscle or tendon, overlifting, particularly damp ground; too much summer bathing in lake or river.
- Affects the fibrous tissue, especially the right side more than the left.
- Pains: as if sprained; as if a muscle or tendon was torn from its attachment; as if bones were scraped with a knife;
- Worse after midnight and in wet, rainy weather; affected parts sore to touch.
- Lameness, stiffness and pain on first moving after rest, or on getting up in the morning better by walking or continued motion.
- Great restlessness, anxiety, apprehension, cannot remain in bed, must change position often to obtain relief from pain.
Ruta
- Pressure on inside of right scapula. Pricking itching between shoulders, not better by rubbing. Contusive pains in back and loins, often with oppressed respiration.
- Pain in loins and sacrum as from contusion.
- Pain in loins when walking and when stooping, or only when seated, better by pressure and when lying down.
- Backache better lying on back.
- Pain in lumbar vertebrae as if bruised. Bruised pain in spine.
Thuja
- Cracking in cervical vertebrae on making certain movements with head.
- Painful drawing in sacrum, coccyx, and thighs, while sitting, after long sitting prevents standing erect.
- Pain, as of a fracture, and stiffness in loins, back, and nape, especially in morning, after rising.
- Ailments from bad effects of vaccination, from suppressed or maltreated gonorrhoea.
- Fixed ideas: as if a strange person were at his side; as if soul and body were separated; as if a living animal were in abdomen; of being under the influence of a superior power.
Causes of slipped disk
-
- Herniation of intervertebral disc.
- Senile degeneration of disc.
- Obesity
- Sudden jerk.
- Over-straining of lumber spine.
- Lifting weight.
- Violent coughing.Sudden stooping or twisting.
- Sprain
- Trauma to spine.
- Commonly affected discs: L4-L5, L5-S1.
Symptoms of slipped disk
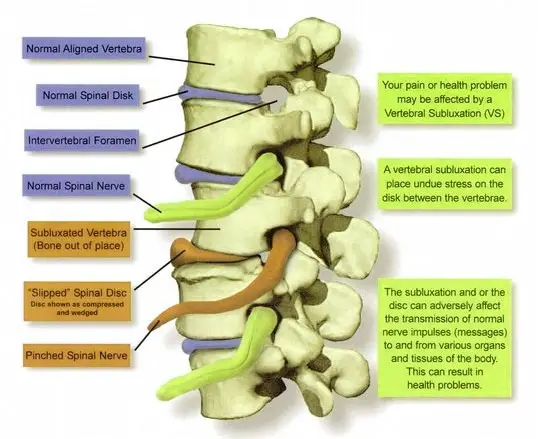
When a prolapsing disk presses on a nerve root, symptoms occur both in the back and in the area that the nerve root supplies. For example, a slipped disk in the lower back can cause pain in the legs.
Symptoms in the back can include severe backache. Often the sufferer will not be able to localize the pain with any accuracy. He or she may also develop painful spasms in the muscles that lie along each side of the spine, particularly in the early stages.
The patient will feel more pain when moving about and some relief when lying flat. Coughing or sneezing can cause the prolapsing disk material to bulge out suddenly, causing a sharp pain in the back or legs. In addition there may be a curvature of the spine, the patient unconsciously leans away from the side of the disk prolapse to try to relieve the pressure from the nerve root that is involved.
If the pressure on the nerve root is not too severe, the nerve will continue to work but will be painful. The brain cannot tell that the painful pressure is coming from the area of the disk, but instead interprets the information as pain originating in the nerve end. In a lower back disk protrusion the sciatic nerve can be irritated, and the individual may feel pain in the thigh, calf, ankle, or foot. This pain can shoot down a leg and is then called sciatica.
More severe pressure on the nerve root may cause the nerve to stop functioning altogether. Areas of skin that the nerve supplies will become numb, so that a light touch or even a pinprick cannot be felt, Muscles supplied by the nerve will become weak or even completely paralyzed. Reflexes such as the knee jerk reflex may disappear.
If only one nerve root is involved this is not too serious, because each nerve supplies only a small area of skin, or a limited number of muscles. If the nerves to the bladder or genitals are affected, however, their function can be permanently lost. Urgent medical attention is needed to relieve the pressure on these nerves.
Diagnosis of the slipped disk
Obtaining a careful patient history is vital because the events that intensify disk pain are diagnostically significant. The straight leg raising test and its variants are perhaps the best tests for slipped disk, but may still be negative.
For the straight leg raising test, the patient lies in a supine position while the examiner places one hand on the patient’s ilium, to stabilize the pelvis, and the other hand under the ankle, and then slowly raises the patient’s leg. The test is positive only if the patient complains of posterior leg (sciatic) pain, not back pain.
Video for straight leg raising test or Lasegue test:
In Lasegue test, the patient lies flat while the thigh and knee are flexed to a 90 degree angle. Resistance and pain as well as loss of ankle or knee jerk reflex indicate spinal root compression.
X-rays of the spine are essential to rule out other abnormalities but may not diagnose slipped disk because marked disk prolapse can be present despite a normal X-ray.
A thorough check of the patient’s peripheral vascular status—including posterior tibial and dorsalis pedis pulses and skin temperature of limbs—helps rule out ischemic disease, another cause of leg pain or numbness.
After physical examination and X-rays, myelography, computed tomography scans, and magnetic resonance imaging (MRI) provide the most specific diagnostic information, showing spinal canal compression by herniated disk material.
MRI is the method of choice to confirm the diagnosis and determine the exact level of herniation. A myelogram can define the size and location of disk herniation. An electro-myogram can determine the exact nerve root involved. A nerve conduction velocity test may also be performed.
MANAGEMENT of Prolapsed Intervertebral Disc (Slipped Disc)
• Rest to spine for at least 6-12 weeks.
• Use of hard bed.
• In severe cases- traction is applied to leg or pelvis, provided there is no cord compression.
• Regain mobility gradually.
• Restrict jerky movements.
• Avoid- forward bending, lifting weight.
• Reduce weight if obese.
Complications of slipped disk
- Neurologic deficits (most common)
- Bowel and bladder problems (with the sacral S1 and S2] nerve root area affected.
Treatment and prevention of slipped disk
About 88% of cases of recent onset of low back pain will resolve in six weeks, while 98% will resolve by 24 weeks. Even in extreme cases in which the patient is unable to stand up straight after an episode of pain, reduced activity coupled with motions that aid in reducing complaints can resolve the problem and return the person to his or her pre-injury activities.
Treatment of the condition should be directed at decreasing the person’s complaint or radiating symptoms. This often involves exercises and activities that are encouraged or avoided as they relate to improving or worsening of the complaint. Most programs involve some form of stretching, muscle strengthening and education, and gentle aerobic exercise. It is not uncommon to have successful resolution of the symptoms without changing the disk injury or location as seen on the MRI.
In spite of many unknowns about the relationships among the disks, nerves, and the patient’s overall complaints, both surgical and nonsurgical options exist. In the case of loss of control of the bowel or bladder, surgery can be immediate; otherwise, surgery is never a first choice.
Surgeons can remove the areas of the extruded disk, remove the disk completely and fuse the two adjacent vertebrae, or increase the space available for the compressed nerve, or both. Consideration for surgery first requires failure of nonsurgical options.
The above information about homeopathy treatment of slipped disk is only for information purpose. Please consult a professional homeopath before taking any homeopathic medicine for slipped disk.
Slipped Disk Cases Cured with Homeopathic Medicine
An Illustration of Integrating The Sensation Method with Traditional Homoeopathy – by Meghna Shah
A Case of Stramonium -Aspergers – by Carla Beharry
Case of Egotrophy of 1st Degree: He Re-adjusts – by SML Fayeton
Homoeopathy – A Ray of Hope for Infertility – by Jayesh Shah



 Burning in back. Spasms in muscles of back.
Burning in back. Spasms in muscles of back.


it is worth to read. good article good information it can batter if some homoeopathically treated case also given . thanks
no treated cases given
my mother suffring from S1 is disk prablem is it cure with out operation
Halo sir.h r u,
I m working in a pak university.in sep tember 2016 i face disk slip problm.
after MRI L5,L4 and S1 has been pointed out.
Now in march 2017 the pain remained 20% but numness is stil there in left foot fingres and in heel.
Would u like to tel me the homeo medicine that can i get from my country(pak).i shal b vry thankful to u sir.
hello brother
im also suffering from same problem is there any proper medicine to cure
please reply me
L3 to s1 some of them are hernited sliped disc and some of narrow down bone…..is that will cure homeopathic. Please help me. Suffering seatica pain in right side of leg. I am working in factory and lift a havy objects and causing of this happen to my health. Please with information. 35 years of old male.
Are you in India? If so, email Dr. Firuzi Mehta:
[email protected]
I have disc herniated problem from L3, L4, L5, and S1. Right side sietica pain wile standing and running. Suffering almost year. Is there any cute for this problem through Homeopathic. Please help [email protected]
Dear sir,
According my MIR report it shows herniated disc at l3 s1. I wanted to show u my reports. I feel pain at morning. I cannot stand easily for left leg pain .
Sir,
I want to cure by taking homeo.
I have L4/L5 disc herniated problem since 1 month also Left Leg pain just above the Ankle sietica pain while standing and walking. I can not stand & Walk not more than 1/2 hr. When I’m resting I feel some time mild pain.
Is there any cute for this problem through Homeopathic. Please
Good information thanks
Hello Sir/Madam,
Can you please prescribe me the medicine for L4 L5 disc issue. I feel numbness in entire left area of my body. Mostly pain thru out the day. My work nature is cont. monitoring computer.
Please help.