Background
I coordinate and supervise several homeopathic clinics in Eastern Province, Kenya that are staffed with graduates from ALCNM. These clinics have achieved a fee-paying patient base of 35,000 local people over that period. The homeopaths are assisted by a laboratory technician at permanent clinics and on mobile clinics in villages.
At our clinics in rural Kenya, I have found it very challenging. One one hand, no one doubts the effectiveness of single remedy prescribing. On the other hand, there is the challenge at our high volume clinics that see about 500 patients a month. For this reason, in acute diseases, I have employed a system of using nosodes and remedy complexes such as Abha Light’s “MalariX” and the Narayani mixes. This article begins an exploration of this approach.
Case-Taking Challenge
Typically, a patient enters my practice room, called from the small crowd of mainly colourfully-scarfed women in the waiting area outside. This village clinic, positioned amidst statuesque baobab trees, lies along the major and only highway that runs from the Kenyan coast all the way to Uganda and beyond. Most of the population in this semi-arid area are farmers, to some extent only as rich or poor as the rains allow the crops to grow. People in their shambas (homesteads), on dusty plains, in small markets, hear about the homeopathy clinics and they come in.
Several times a day, I take a case something like this: the patient will have medley of symptoms such as headache, heaviness between shoulders, abnormal heat and sweat, joint pains, lumbar pain, biting pains in stomach, burning in hypogastrium, goat-like ball-stools, dreams of dead people she knows. Quite a usual case for a village in Africa. Even though I press for modalities and generals, a past history of illness, and time allowing, a bit of delving into emotional/mentals, the specificity of symptoms may not be easy to glean. Kikamba, the local mother tongue, or the national language, Swahili, do not possess the intricacy of the English vocabulary.
From experience, one knows that the parasitic and bacterial infections common in rural Kenya such as malaria, typhoid, brucella, amoeba, hookworm, etc. have overlapping symptom pictures. So, whilst taking the case and thinking of treatment in a homeopathic, holistic way, I’ll equally be pondering on identifying the illness. In other words, I’ll send the patient for lab tests, but which ones? Having selected possible tests, I need to negotiate with the patient about which tests can actually be done, according to the patient’s finances. While the lab tests are going on, I will look for the simillimum. Often however, the case analysis will be put aside to await test results, and another patient is called in to be seen in the meantime.
The test results are done within an hour. I scan them, and any intent I had of single remedy prescribing fades fast ; the results show malaria, brucella, amoeba and hookworm infections present simultaneously. With such acute infections identified, my responsibility as a health practitioner feels heightened. I need to address this individual’s complicated health problems, in the shortest possible time.
The need of lab tests in order “to cover the case”
In Kenya, people view our village clinics as any other clinic – as a primary health care centre. Often, we are a clinic of first choice for treatment. Of course, we refer cases to hospitals when they are beyond our capabilities. It is imperative to provide as many services as possible – including diagnostic tests for blood, urine and stool, which perhaps the usual homeopathic clinic in industrialized countries may not consider as important. In my practice , I have evolved an effective framework for handling a high volume of acute cases in a competent manner. Over time, from clinical experience, I have gained confidence in my ability to bring patients back to health.
After the lab tests identify the parasitical and bacterial infections, one must consider their potential risks to the patient. For example, malaria and typhoid are red-flagged. Malaria’s falciparum variety transmitted by mosquitos in our area, always threatens to complicate with cerebral symptoms, which is not treated well, causes death in a very short time. Positive tests for other ailments do not demand such immediate concern: amoebiasis and brucella, for example are almost always present in our rural community, yet with limited symptomology. Since most patients regularly get re-infected, their personal immunity builds up to the diseases causing a modified symptom picture. Only infrequently do we see these diseases as found in the text books. I found that I need to view the patient not only from the simillium, but also from the disease aspect. Infecting agents have to be identified in the patient.
In treatment therefore, one “covers the case” by including the results from the lab as well as the simillium symptoms. In this process, I employ nosodes as part of the treatment.
Given the typical case above, I would be hard pressed to select a single remedy. What I might do is give Thymol 6 for the hookworm, Brucella nosode 200c for the Brucella, MalariX (Abha Light’s malaria complex remedy containing Malaria co nos 30c,) and Amoeba nosode 30c. I would prescribe them as alternating remedies over the next few days.
Another option might be to include a Narayani remedy, which often helps. One such remedy, useful in replenishing red blood cells being destroyed by the malaria parasite, is Blood OMI 30.
This would be the initial treatment and it may sort them out completely. Or it is possible to follow the nosodes with a symptomatic simillium after the initial “boost” from the nosodes. It’s very possible that I won’t hear from the patient again for two years and they often report having been well. For others, this treatment will not be adequate for their longer term chronic states. It may get them over the danger period of acute infections, but they will need a deeper, more individualized case taking. I’ll generally know if the patient returns for a follow-up a week or two later.
Conclusion
Laboratory tests provide important diagnostic tools in rural Africa. The identification of specific infecting agents impacts on the homeopathic approach to case analysis and prescribing. The homeopath has the option to act using symptomatically similar remedies, polypharmacy and nosodes. This practical application of homeopathy works well!
A CASE:
Below is a case from one of our mobile homeopathic clinics. The patient was of the Masaai tribe, who are mostly herders. The Mission clinic runs monthly and the usual allopathic treatment is suspended when we are present. The Mission nurses interpret for us. As it’s a mobile clinic, we keep the patient on hand until we are certain the treatment is helping.
A Masaai woman (of 40 yrs) was helped in by a friend. She was very weak, and on sitting doubled over, resting her head on her knees. She couldn’t describe her problem at all, only saying there was a headache. She was panting. Blood pressure was low at 90/60. No Fever. Abdominal cramping was evident, > doubling up. No vomit or diarrhoea. Her mind was out of sorts, she was confused, unable to explain herself properly.
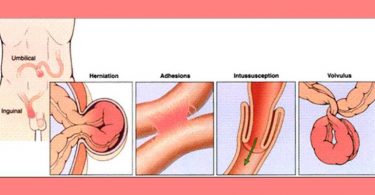
A visiting volunteer Naturopath examined her. A small palpable mass below the umbilicus was felt, maybe a pregnancy in early stages? Could this be threatened miscarriage (she later said she had missed her last period), or ectopic pregnancy, or ovarian cyst or PID.. ..or appendicitis? Her abdomen was checked for rebound pain, there was none.
I had given the patient Colocynthus 200c whilst she sat on the bench. Fifteen minutes later without much effect, I followed with Cimicifuga 200c. After having noted the few symptoms above and the little we could glean from the patient, we sent her to a clinic room to lie down. She said she was OK, “just coming to pay a visit” (whilst obviously in pain). She quickly went to sleep after the Cimicifuga 200c.
She was not responding to the remedies as I would have expected in such an acute attack. However there was some slight amelioration, enough to observe a few more characteristic symptoms. We confirmed her pregnancy and took a few more tests. She had some mental disturbances and confusion along with abdominal pain and headache.
She was confused and wasn’t expressing herself with the right words. She had dyspnea and was very sleepy. Her headache seemed to be over the temples, though it was difficult for her to describe. Her stomach was distended beyond the pregnancy itself.
I did repertorisation and Nux moschata was a remedy that came up. The patient stirred from sleep, I gave her Nux-m 30c, and she returned to sleep.
One and a half hours later we spoke with the patient. Clarity of mind had returned, She was able to explain that the abdominal cramps had started before she went to bed last evening, and now in the clinic they had gone. All that remained was the headache, as a sharp pain, left side of the head. We observed that her breathing had become regular. At this point we took a blood sample to test for malaria, typhoid and brucellosis. She continued resting on the couch. Soon after, lab test results showed: (1) No malaria seen. (2) Brucella highly reactive. (3) Typhoid highly reactive. I expected the headache to be due to the Brucella and Typhoid. I decided to let the Nux-m, as the indicated remedy, run its course.
One hour later, the patient said the headache persisted but was less painful. I repeated Nux-m 30c. Fifteen minutes later, I gave Brucella nosode 200c, single dose, and the patient continued lying down.
One hour later, the headache had improved and the patient sat up. I repeated the Brucella 200c. The patient waited outside, sitting in the shade. I also gave a dose of MalariX. This was to protect her in case the malaria test was a false negative, as it often can be, when malarial parasites are not circulating in the blood when the sample is taken. Despite the fact that Malaria is so endemic, the tests are not always foolproof.
Two hours later the patient wanted to go home. The headache was “mild”. I sent her off with Nux-M 30c, Brucella 200c and MalariX, one pillule to be taken that evening, (one has to be very wary of the possibility of malaria and its consequences).
Next day at 2 pm the patient reported back “doing good”. The headache was 20% of what it was. No further sign of the abdominal pains. She was communicating normally. The weakness still persisted. I prescribed 2 Narayani remedies to help strengthen her during the pregnancy Blood OM1 30 1×3 (2weeks) + Calcium mix 67 30 1×3 (3 weeks).





Wow – so lovely to see more practical multi prescribing. And to see the use of lab tests of part of your work too.
Hello Dr.
Where can I buy the MalariX and other homeopathic remedies for malaria and typhoid, amoebas? I spend most of the year in Nigeria and am tired of being in the clinic every month for one thing or the other. My liver and kidneys are not going to last forever. I’m currently in the U.S., where can I buy these remedies?
Thank you!
There are many homeopathic remedies for malaria it’s not one pill fits all.A classical homeopath needs to do a full case taking on you prior to prescribing a proper well indicated remedy.If you search the database on remedies and malaria you will find that there are at least 10 that might fit the symptoms.Only one of these homeopathic remedies will work the other 9 will not.