The Story of Fidgety Philip
 “Let me see if Philip can
“Let me see if Philip can
Be a little gentleman;
Let me see if he is able
To sit still for once at table.”
Thus spoke, in earnest tone,
The father to his son;
And the mother looked very grave
To see Philip so misbehave.
But Philip he did not mind
His father who was so kind.
He wriggled
And giggled,
And then, I declare,
Swung backward and forwardAnd tilted his chair,
Just like any rocking horse;-
“Philip! I am getting cross!”
 See the naughty, restless child,
See the naughty, restless child,
Growing still more rude and wild,
Till his chair falls over quite.
Philip screams with all his might,
Catches at the cloth, but then
That makes matters worse again.
Down upon the ground they fall,
Glasses, bread, knives forks and all.
How Mamma did fret and frown,
When she saw them tumbling down!
And Papa made such a face!
Philip is in sad disgrace.
 Where is Philip? Where is he?
Where is Philip? Where is he?
Fairly cover’d up, you see!
Cloth and ll are lying on him;
He has pull’d down all upon him!
What a terrible to-do!
Dishes, glasses, snapt in two!
Here a knife, and ther fork!
Philip, this is naughty work.
Table all so bare, and ah!
Poor Papa and poor Mamma
Look quite cross, and wonder how
They shall make their dinner now.
Attention-deficit hyperactivity disorder (ADHD) is considered to be a neurological syndrome that exhibits symptoms such as hyperactivity, forgetfulness, mood shifts, poor impulse control, and distractibility, when judged to be chronic, as symptoms of a neurological pathology. It is seen in both children and adults and is believed to affect between 3% to 5% of the human population.
Much controversy exists surrounding the diagnosis, such as over whether or not the diagnosis denotes a disability in its traditional sense, or simply describes a personal or neurological property of a patient. Those who believe that ADHD is a traditional disability or disorder often debate over how it should be treated, if at all. According to a majority of medical research in the United States, as well as other countries, ADHD is now generally regarded as a non-curable neurological disorder for which a wide range of effective treatments are available. Methods of treatment include the use of medication, psychotherapy, a combination of both, as well as other techniques. Many patients are able to control their symptoms over time, even without the use of medication.
ADHD is most commonly diagnosed in children. When diagnosed in adults, it is regarded as adult attention-deficit disorder (AADD). It is believed that anywhere between 30 to 70% of children diagnosed with ADHD retain the disorder as adults.
Terminology
The most appropriate designation of ADHD is currently disputed; the terms below are known to be used to describe the condition. A difficulty in the condition’s nomenclature arises when some scientific research suggests that certain behaviors are directly attributable to ADHD, while other research concludes that the same behaviors constitute disorders that need to be classified independently of ADHD. For the purposes of this article, the “Terminology” section will be used only to name ADHD and its near equivalents, while the names for its manifestations and subtypes will be listed in “Symptoms” section, below.
- Attention-deficit hyperactivity disorder (ADHD): In 1987, ADD was in effect renamed to ADHD in the DSM-III-R. In it, ADHD was broken down into three subtypes (see ‘symptoms’ for more details):
- predominantly inattentive ADHD
- predominantly hyperactive-impulsive ADHD
- combined type ADHD
- Attention deficit disorder (ADD): This term was first introduced in DSM-III, the 1980 edition. Is considered by some to be obsolete, and by others to be a synonym for the predominantly inattentive type of ADHD.
- Undifferentiated attention-deficit disorder (UADD): This term was first introduced in the DSM-III-R, the 1987 edition. This was a miscellaneous category, and no formal diagnostic criteria were provided. UADD is approximately the predominantly inattentive type of ADHD in the DSM-IV-TR. The DSM-III-R diagnosis of attention-deficit hyperactivity disorder required hyperactive-impulsive symptoms in addition to the inattentive symptoms.
- Attention-deficit syndrome (ADS): Equivalent to ADHD, but used to avoid the connotations of “disorder”.
- Hyperkinetic disorders (F90) is the ICD-10 equivalent to ADHD. The ICD-10 does not include a predominantly inattentive type of ADHD because the editors of Chapter V of the ICD-10 believe the inattentivity syndrome may constitute a nosologically distinct disorder.
- Disturbance of activity and attention (F90.0)
- Hyperkinetic conduct disorder (F90.1) is a mixed disorder involving hyperkinetic symptoms along with presence of conduct disorder
- Other hyperkinetic disorders (F90.8)
- Hyperkinetic disorder, unspecified (F90.9)
- Hyperkinetic syndrome (HKS): Equivalent to ADHD, but largely obsolete in the United States, still used in some places world wide.
- Minimal cerebral dysfunction (MCD): Equivalent to ADHD, but largely obsolete in the United States, though still commonly used internationally.
- Minimal brain dysfunction or Minimal brain damage (MBD): Similar to ADHD, now obsolete.
Formal definitions
Neurologically, the U.S. Surgeon General and ICD-10-CM, describe ADHD as a metabolic form of encephalopathy, which impairs the release and homeostasis of neurological chemicals, thereby possibly reducing the function of the limbic system.
From a developmental/behavioral standpoint, the Diagnostic and Statistical Manual of Mental Disorders-IV-TR states that ADHD is a developmental disorder that presents during childhood, in most cases before the age of seven, and is characterized by developmentally inappropriate levels of inattention and/or hyperactive-impulsive behavior. The DSM-IV also stipulates that in order to be diagnosed, the condition must also result in significant impairment of one or more major life activities, including interpersonal relations, educational or occupational goals, as well as cognitive or adaptive functioning. ADHD may be also diagnosed in adulthood, but symptoms must have been present prior to age seven, in order to yield a positive diagnosis.
Symptoms of ADHD
The symptoms of ADHD fall into the following two broad categories:
Inattention:
-
Failing to pay close attention to details or making careless mistakes when doing schoolwork or other activities
-
Trouble keeping attention focused during play or tasks
-
Appearing not to listen, when spoken to
-
Failing to follow instructions or finishing tasks
-
Avoiding tasks that require a high amount of mental effort and organization, such as school projects
-
Frequently losing items required to facilitate tasks or activities, such as school supplies
-
Excessive distractability
-
Forgetfulness
Hyperactivity-impulsive behavior
-
Fidgeting with hands or feet or squirming in seat
-
Leaving seat often, even when inappropriate
-
Running or climbing at inappropriate times
-
Difficulty in quiet play
-
Frequently feeling restless
-
Excessive speech
-
Answering a question before the speaker has finished
-
Failing to await one’s turn
-
Interrupting the activities of others at inappropriate times
A positive diagnosis is usually only made if the patient presents with at least six of the above symptoms. In addition, a positive diagnosis is made if six or more of these symptoms presented before the age of seven; the symptoms usually begin to appear between the ages of four and six.
Children who grow up with ADHD often continue to have symptoms as they grow into adulthood. Adults face some of their greatest challenges in the areas of self-control, motivation, as well as executive functioning (also known as working memory). If the patient is not treated appropriately, co-morbid conditions, such as depression and anxiety may present as well. If a patient presents with such conditions as well, the co-morbid condition is usually treated first.
Diagnosis
The Centers for Disease Control and Prevention (CDC) emphasize that a diagnosis of ADHD should only be made by trained health care providers, as many of the symptoms may also be part of other conditions, such as bodily illness or other physical disorders, such as hyperthyroidism. Further, it is not uncommon that physically and mentally nonpathological individuals exhibit at least some of the symptoms from time to time. Severity and pervasiveness of the symptoms leading to prominent functional impairment across different settings (school, work, social relationships) are major factors in a positive diagnosis.
Psychoanalytical Testing
Due to the lack of objectivity that surround the critical factors, many question the reliability of ADHD diagnosis. The American Academy of Pediatrics Clinical Practice publishes guidelines to aid providers in making an objective diagnosis, but even if strictly adhered to, doubt still remains among some patients, as well as providers. Other diagnostic methods, such as those involving magnetic resonance imaging (MRI), may detect the presence of ADHD by analyzing images of the patient’s brain, are usually not recommended (see brain scans). In a majority of cases, diagnosis is therefore dependent upon the observations and opinions of those who are close to the patient; in many patients, especially as they approach adulthood, self-diagnosis is not uncommon.
Publications that are designed to analyze a person’s behavior, such as the Brown Scale or the Conners Scale, for example, attempt to assist parents and providers in making a diagnosis by evaluating an individual on typical behaviors such as “Hums or makes other odd noises”, “Daydreams” and “Acts ‘smart'”; the scales rating the pervasiveness of these behaviors range from “never” to “very often”. Connors states that, based on the scale, a valid diagnosis can be achieved; critics, however, counter Connors’ proposition by pointing out the breadth with which these behaviors may be interpreted. This becomes especially relevant when family and cultural norms are taken into consideration; this premise leads to the assumption that a diagnosis based on such a scale may actually be more subjective than objective (see cultural subjectivism). The scales are further criticized, because they were originally developed to measure the effectiveness of stimulant medication, and not to detect ADHD. Therefore, the scales might merely evaluate a patient’s response to stimulant medication, such as Ritalin or Adderall, rather than the presence of ADHD.
Clinical Testing
The American Academy of Pediatrics Clinical Practice Guideline for children with ADHD emphasizes that a reliable diagnosis requires:
- The use of explicit criteria for the diagnosis using the DSM-IV-TR.
-
The importance of obtaining information about the child’s symptoms in more than one setting (especially from schools).
- The search for coexisting conditions that may make the diagnosis more difficult or complicate treatment planning.
A proper diagnosis is dependent upon a physician fulfilling all three of these criteria. The first criteria can be satisfied by using an ADHD-specific instrument such as the Conners Scale. The second criteria is best fulfilled by examining the individual’s history. This history can be obtained from parents and teachers, or a patient’s memory. The requirement that symptoms be present in more than one setting is very important because the problem may not be with the child, but instead with teachers or parents who are too demanding. The use of intelligence and psychological testing (to satisfy the third criteria) is essential in order to find or rule out other factors that might be causing or complicating the problems experienced by the patient.
Computerized tests
Computerized tests of attention are not especially helpful in providing a further independent assessment because they have a high rate of false negatives (real cases of ADHD can pass the tests in 35% or more of cases), they do not correlate well with actual behavioral problems at home or school, and are not especially helpful in determining treatments. Both the American Academy of Pediatrics and American Academy of Child and Adolescent Psychiatry have recommended against the use of such computerized tests for now in view of their lack of appropriate scientific validation as diagnostic tools. In the USA, the process of obtaining referrals for such assessments is being promoted vigorously by the President’s New Freedom Commission on Mental Health.
Brain scans
Neurometrics, PET scans, FMRI, or SPECT scans have the potential to provide a more objective diagnosis. However, these are not typically suitable for very young children, and may unnecessarily expose the patient to harmful radiation. Because the etiology of the disorder is unknown, and a complete neurological definition of this disorder is lacking, a majority of clinicians doubt the current predictive power of these objective tests to detect ADHD to be used to direct clinical treatment. Currently, the American Academy of Pediatrics and the American Academy of Child and Adolescent Psychiatry recommend against using these neuro-imaging methods for clinical diagnosis of individuals who may have ADHD. They remain, however, useful research tools when studying groups of patients with ADHD. An October 2005 meta-analysis by Alan Zametkin, M.D., with the NIMH entitled “The ADHD Report”, concluded that these diagnostic methods lack adequate scientific research on accuracy and specificity to be used as a primary diagnostic tool.
Incidence
ADHD has been found to exist in every country and culture studied to date. While it is most commonly diagnosed in the United States, rates of diagnosis are rising in most industrialized countries as they become more aware of the disorder, its diagnosis, and its management.
Nearly four million children younger than 18 in the United States had been diagnosed with attention deficit hyperactivity disorder (ADHD). In general, 5-8% of children are likely to have ADHD while 4-5% of adults do so. More than twice as many boys have been diagnosed than girls (10% vs. 4%).
The ADHD treatment rate among Caucasian children is significantly higher than among African and Hispanic Americans (4.4% Caucasian, 1.7% African, 1.5% Hispanic in 1997)
The same study notes that outpatient treatment for ADHD has grown from 0.9 children per 100 (1987) to 3.4 per 100 (1997).
Possible causes
Research indicates that the frontal lobes, their connections to the basal ganglia, and the central aspects of the cerebellum (vermis) are most likely to be involved in this disorder, as may be a region in the middle or medial aspect of the frontal lobe, known as the anterior cingulate. The cerebellum, which is believed to play important roles in “short-term memory, attention, impulse control, emotion, higher cognition, [and] the ability to schedule and plan tasks,” has been shown to be smaller in the brains of those who have ADHD.
A 1990 study at the U.S. National Institute of Mental Health correlated ADHD with a series of metabolic abnormalities in the brain, providing further evidence that ADHD is a neurological disorder.
The source of these differences is not yet known, but a couple of theories have been presented.
Hereditary dopamine deficiency
Research suggests that ADHD arises from a combination of various genes, many of which have something to do with dopamine transporters. Suspect genes include the 10-repeat allele of the DAT1 gene and the 7-repeat allele of the DRD4 gene. Other studies have documented an association between ADHD and the dopamine beta hydrozylase gene (DBH TaqI).
SPECT scans found people labeled as ADHD have reduced blood circulation, and a significantly higher concentration of dopamine transporters in the striatum which is in charge of planning ahead.
Metabolism
It has long been suggested that ADHD could be the result of a nutritional problem. Recent studies have begun to find metabolic differences in these children, indicating that an inability to handle certain elements of one’s diet might contribute to the development of ADHD, or at least ADHD-like symptoms. For example, in 1990 the English chemist N.I. Ward showed that children with ADHD lose zinc when exposed to a food dye. Waring, McFadden, and others have shown that children with autism or ADHD are low in sulfation metabolism, in particular the enzyme Phenol Sulfotransferase-P. Some studies suggest that a lack of fatty acids, specifically omega-3 fatty acids can trigger the development of ADHD. Support for this theory comes from findings that breast-fed children are less likely to have ADHD than their bottlefed counterparts and until very recently, infant formula did not contain any omega-3 fatty acids at all. Time will tell whether or not this is coincidence or a true correlation.
External Factors
There is no compelling evidence that social factors, alone, can create ADHD. The few environmental factors implicated fall in the realm of biohazards including alcohol, tobacco smoke, and lead poisoning. Allergies (including those to artificial additives) as well as complications during pregnancy and birth– including premature birth–might also play a role.
Smoking during pregnancy
It has been observed that women who smoke while pregnant are more likely to have children with ADHD. Nicotine is known to cause hypoxia (lack of oxygen) in the uterus. Hypoxia causes brain damage. Therefore it is entirely possible that smoking during pregnancy could cause the fetus to suffer brain damage.
Head injuries
It has been known for some time that head injuries can cause a person to display ADHD-like symptoms. This is possibly because of the damage done to the victim’s frontal lobes. This is also why one of the earliest names for ADHD was “Minimal Brain Damage”.
Dopamine deficiency caused by sleep apnea
Another theory is that ADHD is caused by brief pauses in breathing (apnea) during infancy. In October 2004, Dr. Glenda Keating and Dr. Michael Decker of Emory University presented data at the Society for Neuroscience’s annual meeting showing that repetitive drops in blood oxygen levels in newborn rats similar to that caused by apnea in some human infants is followed by a long-lasting reduction in dopamine levels, associated with ADHD. Apnea occurs in up to 85% of prematurely born human infants. It remains to be seen whether or not these findings can be replicated in human babies.
Treatment of ADHD
There are many options available to treat people diagnosed with ADHD. The options with the greatest scientific support include a variety of medications, behavior-changing therapies, and educational interventions.
Findings of a large randomized controlled trial suggest that:
-
Medication alone is superior to behavioral therapy alone.
-
The combination of behavioral therapy and medication has a small benefit over medication alone.
Mainstream treatments
The first-line medication used to treat ADHD are mostly stimulants, which work by stimulating the areas of the brain responsible for focus, attention, and impulse control. The use of stimulants to treat a syndrome often characterized by hyperactivity is sometimes referred to as a paradoxical effect. But there is no real paradox in that stimulants activate brain inhibitory and self-organizing mechanisms permitting the individual to have greater self-regulation. The stimulants used include:
- Methylphenidate – Available in:
- Regular formulation, sold as Ritalin, Metadate, Focalin, or Methylin. Duration: 4-6 hours per dose. Usually taken morning, lunchtime, and in some cases, afternoon.
-
Long acting formulation, sold as Ritalin SR, Metadate ER. Duration: 6-8 hours per dose. Usually taken twice daily.
- All-day formulation, sold as Ritalin LA, Metadate CD, Concerta (Methylphenidate Hydrochloride), Focalin XR. Duration: 10-12 hours per dose. Usually taken once a day.
-
Amphetamines —
- Dextroamphetamine – Available in:
- Regular formulation, sold as Dexedrine. Duration: 4-6 hours per dose. Usually taken 2-3 times daily.
-
Long-acting formulation, sold as Dexedrine Spansules. Duration: 8-12 hours per dose. Taken once a day.
- Adderall, a trade name for a mixture of dextroamphetamine and laevoamphetamine salts. – Available in:
- Regular formulation, Adderall. Duration: 4-6 hours a dose.
- Long-acting formulation, Adderall XR. Duration: 12 hours. Taken once a day.
- Methamphetamine – Available in:
-
Regular formulation, sold as Desoxyn by Ovation Pharmaceutical Company. Usually taken twice daily.
-
- Bupropion. A dopamine and norepinephrine reuptake inhibitor, marketed under the brand name Wellbutrin.
- Atomoxetine. A norepinephrine reuptake inhibitor (NRI) introduced in 2003, it is the newest class of drug used to treat ADHD, and the first non-stimulant medication to be used as a first-line treatment for ADHD. Available in:
- Once daily formulation, sold by Eli Lilly and Company as Strattera. This medicine doesn’t have an exact duration. It is to be taken once or twice a day, depending on the individual, every day, and takes up to 6 weeks to begin working fully. If the intake schedule is interrupted, it may take a few weeks to begin working correctly again.
Second-line medications include:
- Benzphetamine – a less powerful stimulant. Research on the effectiveness of this drug is not yet complete.
- Provigil/Alertec/Modafinil – Research on this drug is not yet complete.
- Cylert/Pemoline – a stimulant used with great success until the late 1980s when it was discovered that this medication could cause liver damage. Although some physicians do continue to prescribe Cylert, it can no longer be considered a first-line medicine. In March 2005, the makers of Cylert announced that it would discontinue the medication’s production.
- Clonidine – Initially developed as a treatment for high blood pressure, low doses in evenings and/or afternoons are sometimes used in conjunction with stimulants to help with sleep and because Clonidine sometimes helps moderate impulsive and oppositional behavior and may reduce tics.
Because most of the medications used to treat ADHD are Schedule II under the U.S. DEA schedule system, and are considered powerful stimulants with a potential for diversion and abuse, there is controversy surrounding prescribing these drugs for children and adolescents. However, research studying ADHD sufferers who either receive treatment with stimulants or go untreated has indicated that those treated with stimulants are in fact much less likely to abuse any substance than ADHD sufferers who are not treated with stimulants.
ADHD and ADD Medication Side Effects
Adderall Side Effects
The most common side effects are restlessness or tremor; anxiety or nervousness; headache or dizziness; insomnia; dryness of the mouth or an unpleasant taste in the mouth; diarrhea or constipation; or impotence or changes in sex drive.
Concerta Side Effects
In the clinical studies with patients using CONCERTA®, the most common side effects were headache, stomach pain, sleeplessness, and decreased appetite. Other side effects seen with methylphenidate, the active ingredient in CONCERTA®, include nausea, vomiting, dizziness, nervousness, tics, allergic reactions, increased blood pressure and psychosis (abnormal thinking or hallucinations).
Ritalin Side Effects
Nervousness and insomnia are the most common adverse reactions but are usually controlled by reducing dosage and omitting the drug in the afternoon or evening.
Other reactions include hypersensitivity (including skin rash, urticaria, fever, arthralgia, exfoliative dermatitis, erythema multiforme with histopathological findings of necrotizing vasculitis, and thrombocytopenic purpura); anorexia; nausea; dizziness; palpitations; headache; dyskinesia; drowsiness; blood pressure and pulse changes, both up and down; tachycardia; angina; cardiac arrhythmia; abdominal pain; weight loss during prolonged therapy.
Allergic reactions: skin rash, hives, drug fever, joint pains possible. Headache, dizziness rapid and forceful heart palpitation-infrequent.
Strattera Side Effects
Upset stomach, decreased appetite, nausea or vomiting, dizziness, tiredness, some weight loss, and mood swings were the most common side effects.
In rare cases, Strattera can cause allergic reactions, such as swelling or hives, which can be serious. Your child should stop taking Strattera. Call your doctor or healthcare professional if your child develops any of these symptoms.
Alternative treatments for ADHD
There are many alternative treatments for ADHD, most of them heavily disputed or relegated to adjunct status with medication treatment. This section attempts to deal with the most prominent of the alternative treatments. Bear in mind that the term “alternative” may mean unscientific because there are little or no credible scientific studies to support these suggested interventions, rather than there being experimental evidence against the intervention.
Nutrition
As noted above there are indications that children with ADHD are metabolically different from others, therefore it is believed that diet modification may play a major role in the management of ADHD. Perhaps the best known of the dietary alternatives is the Feingold diet which involves removing salicylates, artificial colors and flavors, and certain synthetic preservatives from children’s diets. Granted, according to a recent meta-analysis, there is little scientific evidence for the effectiveness of the Feingold diet in treating ADHD specifically, but this could be because much research has focused on food dyes, and the diet eliminates much more than that.
It has been documented since the early 1970’s that poor diet and food allergies could be related to ADHD, or that there could be improvements in an ADHD individual by putting them on a specific ADHD Diet. Often ADHD individuals have physical symptoms as well that could be due to food allergies such as, asthma, chronic ear infections, migraines, eczema, chronic infections, etc… Dr. Benjamin Feingold made the original claims that certain foods and food additives could trigger ADHD, and when he tested this diet with his patients he found success. He claimed that 30-50% of his ADHD patients benefited from his ADHD Diet (free of artificial colorings and salicylates). As the ADHD Diet Information and the word of Dr. Feingold’s success became widely known, skepticism and controversy emerged.
The first study that supported Dr. Feingold’s ADHD Diet Information in 1976 found that at least 4 out of 15 children diagnosed with ADHD improved on a diet free of artificial colors and flavors. Many breakfast cereals, candies, chips, breakfast bars, ice creams, boxed macaroni and cheese, canned ravioli’s, sodas, and pretty much everything your child loves to eat contains artificial colors and flavors.
Our Standard American Diet (SAD) consists of processed foods, red meat, refined carbohydrates, food additives, soft drinks, and fried foods. With that said, it is a good idea for the whole family to follow an ADHD Diet.
This program is recommended for every member of the family. It’s not just an ADD diet. It’s the same program that we put professional athletes and business executives on for optimized performance, with only minor changes.
We have found that it really helps about 20% of the ADHD kids that try it. The most common feedback that we get from parents is, “Well, it helped my kid somewhat, but I really feel great!” Results fall into a “Bell Curve.” A few do great, a few are completely unaffected, and most do somewhat better but it is not enough as a stand-alone intervention. Please have realistic expectations. But please try it. It just may be a big help to your family.
First, what NOT to eat for TWO WEEKS:
1) NO DAIRY PRODUCTS, especially cow’s milk. This is the single most important restriction. Instead try Almond milk, Rice milk, or Better Than Milk. Drink water instead of milk. In fact, drink lots of water. The brain is about 80% water, and increasing your water intake to 7 to 10 glasses per day might be helpful all by itself. Sodas, Gatorade, teas, ices, etc., do not count as water. Water counts as water.
2) NO YELLOW FOODS. Especially Corn or Squash. Bananas are white. Don’t eat the peel.
3) NO JUNK FOODS. If it comes in a cellophane wrapper, don’t eat it.
4) NO FRUIT JUICES. Too much sugar content. One small glass of apple juice has the sugar content of eight apples. Later on you can have juice, but dilute it with water 50/50.
5) CUT SUGAR INTAKE BY 90%. If you can, cut it down to zero. Sugar is in just about everything, but give it a try. Do your best without going crazy.
6) CUT CHOCOLATE BY 90%. No more than a single piece, once a week.
7) NO NUTRASWEET. None. Period.
8) NO PROCESSED MEATS and NO MSG. Only get meats with labels that say, “Turkey and Water,” etc. If the meat has chemicals listed that you can’t pronounce, don’t buy it.
9) CUT FRIED FOODS BY 90%.
10) AVOID FOOD COLORINGS WHENEVER POSSIBLE. See if your child is sensitive to any particular colors, such as Reds, Yellows, etc. For now, though, avoid all if possible.
SUMMARY: Just eat foods that God made for a while. Eat like people did in the 1940’s. Go to a used book store and get a Betty Crocker’s Cook Book for recipe ideas. There really are about 10,000 meals that you CAN eat. Just not much in the way of “fast foods” or “convenience” foods.
AFTER TWO WEEKS begin adding these foods back into your diet, one food every other day. Eat A LOT of that food every day for four days. If you have a problem with one of the foods, you will see some kind of a “reaction” within four days. The reaction can vary from big red splotches on the body to ears turning bright red to explosive temper outbursts. If there’s a problem, you’ll know. If there’s no problem, enjoy the food.
WHAT TO EAT TO FEED THE ADHD BRAIN:
1) FOR BREAKFAST SERVE HIGH PROTEIN, LOW CARBOHYDRATE MEALS. Say, “Good-bye,” to Breakfast cereals and milk. Serve 60% Protein and 40% Carbohydrates for Breakfast. Other meals should be 50% / 50%.
2) PROTEIN SUPPLEMENTS might be needed to get the added protein for Breakfast. They are often very helpful in the afternoon as well. Here is our favorite recipe for a Protein Shake:
a) Make a cup of coffee, using one of General Mills’ International Coffees, or something like that, with a flavor that you or your child will like (yes, I know I’m breaking my own rules here, as these coffees have dried milk and some sugar, but I’m trying to get your kid to actually drink the thing, and also get some caffeine mixed with the protein.). Pour the hot coffee into a blender with about 6 oz of ice. Turn on the blender for a bit.
b) Add a good quality protein powder. There are many good ones available. If you can’t find one that you like, ask at your local health food store. Get protein powders that are mostly protein and very little carbohydrate. Add between 15 and 20 grams of protein to the cold coffee in the blender.
c) Turn on the blender again.
d) Drink it up.
This protein shake is helpful for a lot of people. For many small kids, and many adults, this recipe works about as well as a small dose of Ritalin (100 mg of caffeine is roughly the same as 5 mg of Ritalin). So many who might just take a small dose of Ritalin might get away with just doing this.
Don’t forget, though, that even caffeine can have some side effects. Every once in a while we find someone that has problems with the caffeine in the coffee. Usually, though, the caffeine in the coffee helps the person to focus better. The protein helps to feed the brain. If you find this helpful, have one with Breakfast, and one around 3 pm. If it is not helpful, then don’t bother with it.
3) MINERAL SUPPLEMENTS may be helpful. Colloidal Minerals or fully chelated minerals are the best. We like the MinPac from VAXA, but there are several good choices. Don’t buy minerals in the grocery store. Get good minerals.
4) FLAX SEED or PRIMROSE OIL. High sources of Omega oils. Borage oils and some fish oils are good as well. Very important. Mix about a spoonful a day into foods as you prepare them, or add to salad dressings, etc.
5) EAT LOTS OF FRUITS AND VEGETABLES. Avoid Aluminum exposure. Eat in a healthy manner.
Try it out and let us know what you think. Oh, before you email back and ask, “Well, what can we eat?” please look through your Betty Crocker Cook Book and you’ll find hundreds of recipes that will fit. It’s the convenience foods that are most of the problem. Re-discover the lost art of cooking.
In the 1980s vitamin B6 was promoted as a helpful remedy for children with learning difficulties including inattentiveness. After that, zinc was promoted for ADD and autism. Multivitamins later became the claimed solution. Thus far, no reputable research has appeared to support either of these claims, except in cases of malnutrition. Currently the addition of certain fatty acids such as omega-3, is thought to be beneficial, but there is not much evidence to support this either.
It is claimed by some with ADHD that commonly available mild stimulants such as caffeine and theobromine have similar effects to the more powerful drugs commonly used in treating the disorder. Herbal supplements such as Gingko biloba are also sometimes cited. While there is no scientific evidence to support this claim, it is widely accepted by those who wish to avoid strong medication.
Technology-based alternatives
There has been a lot of interesting work done with neurofeedback and ADHD. Children are taught, using video game-like technology, how to control their brain waves. Although some clinical professionals consider the treatment promising, there is not yet sufficient evidence that it remains effective after the immediate treatment is complete. A thorough review of the scientific research by Sandra Loo, Ph.D. and Russell Barkley, Ph.D. (Developmental Neuropsychology 2005) concluded that neurofeedback does not have adequate support from appropriately conducted scientific studies to support it as an intervention at this time.
Audio visual entrainment uses light and sound stimulation to guide and change brainwave patterns. Compared to other technology based alternative treatments it is inexpensive but probably not covered by health insurance. It is safe for most but cannot be used by those suffering from photosensitive epilepsy due to the risk of triggering a seizure. There is no scientific evidence to support this treatment at this time nor does it appear to be consistent with current evidence on the causes of ADHD.
Cerebellar Stimulation
There exist several exercise programs based on cerebellar stimulation that are used to treat ADHD, Asperger’s syndrome and many learning difficulties like dyslexia, dyspraxia, etc. Most prominent are the DORE program, the Learning Breakthrough Programâ„¢ and the Brain Gym®, based on Educational Kinesiology.
These programs include balance, coordination, eye and sensory exercises that specifically stimulate the cerebellum. As noted above several studies have shown that the cerebellums of children with ADHD are notably smaller than their non-ADHD counterparts. Cerebellar stimulation assumes that by improving the patient’s cerebellar function many of the symptoms can be reduced or even eliminated permanently.
ADD Coaching
ADD Coaches work with AD/HD individuals, helping them prioritize, organize, and work on other important life skills. They also help clients to learn about their specific challenges and gifts, thus helping clients to be more realistic in setting goals for themselves. Most coaches give emphasis to finding their client’s strengths and arranging for them to spend more time in areas of strength, while minimizing time spent dealing with areas of difficulty that will not likely be helped by coaching or other interventions. While certain things may always be a challenge, ADD Coaching provides structure and support for helping individuals deal with those difficult tasks as well.
Controversy
While ADD/ADHD is a known psychiatric condition, there are various theories about the cause and some controversy over the number of persons diagnosed and the cost of medications. Some denial in families may also relate to the negative perception of the condition as a hereditary brain disorder.
The ADHD diagnosis is controversial and has been questioned by some professionals, adults diagnosed with ADHD, and parents of diagnosed children. They point out the positive traits that children with ADD have, such as “hyperfocusing.” Others believe ADHD is a divergent or normal-variant human behavior, and use the term neurodiversity to describe it. See below for further elaboration of the many controversies concerning this disorder.
Skepticism towards ADHD as a diagnosis
Many have wondered why the number of children diagnosed with ADHD in the U.S. and UK has grown so dramatically over a short period of time. However, doctors often claim that improving methods of diagnosis and greater awareness are probably in part, if not mostly the reason for this increase. Critics have complained that the ADHD diagnostic criteria are sufficiently general or vague to allow virtually any child with persistent unwanted behaviors to be classified as having ADHD of one type or another.
One critic points out that most children with ADHD have no difficulties concentrating when they are doing activities that are fun, such as playing video games which they can do for hours completely focused. This critic argues that the symptoms of ADHD describe children when they are bored and unconnected to a task.
Lack of definitive evidence
The biological evidence, though repeated and repeated, when scrutinized more closely is not what it seems. For example Zametkin’s impressive looking brain image at the beginning of this article, contrasting differences in brain activity in those with the diagnosis is a picture of those with and without the diagnosis while doing an assigned task. Thus a person (with ADHD) who is not doing the assigned task will have a different looking picture of the brain’s activity on that basis alone. If brain imaging is done while one person moves their arm and another doesn’t there will also be a demonstrable difference. In this particular case the so-called biological evidence may turn out to be inconclusive.
In 1998 NIH called together most of the experts in this field. They issued a consensus statement. This is the next to last sentence of that report: “Finally, after years of clinical research and experience with ADHD, our knowledge about the cause or causes of ADHD remains largely speculative. Consequently, we have no documented strategies for the prevention of ADHD.”
While a believer that ADHD is a biological condition Xavier Castellanos M.D.,then head of ADHD research at the National Institute of Mental Health (NIMH) (interviewed October 10, 2000 on Frontline was very explicit about the extent of our biological information
Workshop
This is a small workshop for those who wants to understand what is the internal feeling of persons who suffer from ADHD syndrome
- One of the basic things in ADHD syndrome is the disability of giving priority, ranking the information which is coming from the external world.
- It means that all information and attraction which come from outside are ofs the same intensity.
- ADHD person have great difficulties in classifying them; to give priority, determine on which more attention should be paid..
- All this creates great confusion, great pressure which, in the end, produces impulsiveness, behavior disorder, hyperactivity …
This is a small exercise to give an example of that feeling, sensation of confusion, that specific state of an ADHD person.
Description of exercise
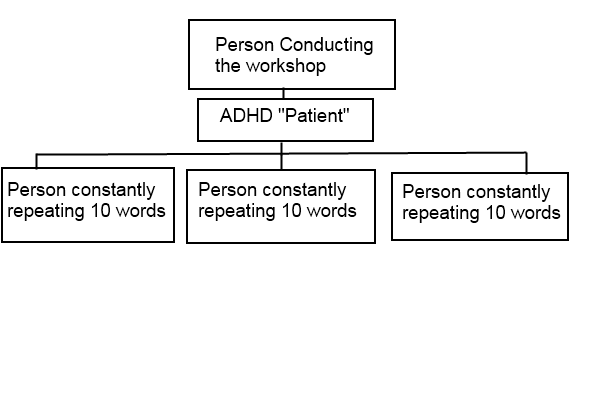
- For this workshop we need five persons. One of them, who will act ADHD should stand in the middle.
- In front of her stands a person who conducts this exercise. His or her task is to vituperate with yowling on ADHD for 2 minutes, and then next 2 minutes of reproaching without yowling. All this is happening continuously.
- The other 3 persons are standing behind the ADHD person and their task is to say over 10 words, randomly chosen, monotonously for 4 minutes
- The reaction which is produced in the person who acts as an ADHD person, is the reaction which we can see during the interview.
- This is a very powerful and shocking exercise but gives a strong sensation and clear picture of what is happening in the head and soul of those who suffer from ADHD syndrome.
Common theme
These are some general common themes which help us make a good diagnosis of ADHD disorder. Alongside them, I give some suggested rubrics from repertory as a direction for finding remedies.
Inattention:
- Failing to pay close attention to details or making careless mistakes when doing schoolwork or other activities
- Mind; concentration – difficult, reading
- Mind; concentration – difficult, studying
- Trouble keeping attention focused during play or tasks
- Mind; concentration – difficult, attention cannot fix
- Mind; concentration – difficult, children in
- Appearing not to listen, when you spoken to
- Mind; concentration – difficult, talking while
- Failing to follow instructions or finishing tasks
- Mind; concentration – difficult, one subject, on
- Avoiding tasks that require a high amount of mental effort and organization, such as school projects
- Mind; mental power – loss of
- Mind; ailments from – mental exertion
- Frequently losing items required to facilitate tasks or activities, such as school supplies
- Mind; concentration – difficult
- Excessive distractibility
- Mind; distraction
- Mind; confusion
- Forgetfulness
- Mind; forgetful
Hyperactivity-impulsive behavior
- Fidgeting with hands or feet or squirming in seat
- Mind; restlessness; children in
- Mind; restlessness; sitting, while-work, while
- Leaving seat often, even when inappropriate
- Mind; restlessness¸diner; drives him from place to place
- Running or climbing at appropriate times
- Extremities; motion – constant
- Difficulty in quiet play
- Frequently feeling restless
- Mind; restlessness; motion, amelioration
- Generals; restlessness
Excessive speech
- Mind; speech -wild
- Mind; speech – foolish
- Mind; speech – hasty
Answering a question before the speaker has finished
- Mind; answering – hastily
- Mind; answering – disconnected
- Failing to await one’s turn
- Interrupting the activities of others at inappropriate times
Specific themes
These are some specific themes on mental-emotional level, which can help us to better understand internal sensation, deep feelings of persons who have ADHD
- Self-control
- Focusing – attention – totality of attention
- concentration on individual attraction
- Sense of time – sense that a lot of time has past, time is passing very fast
– no sense for time
- No self-experience in continuum
- Repeating mistakes
- Sensation that he/she is “OK” – you have to accept me as I am
- basic need to be accepted, to be loved
- manifestly, he is not good, because of disorder of behavior, but without any evil intention
“I am ok, but you are not”:
This is an attitude that occurs in later states and progresses with delinquency, serious disorders of behavior.
- suffering – neglected, does not belong anywhere
- anger – cannot control
- molestation of animals, or those weaker than he is
- difficulty with authorities
- harden on punishment
“I am not OK, anymore”:
- withdrawal
- failure, on every field
- narcomania, other types of delinquency
- depression
- violent behavior
- sense of guilt
- suicide
7. Impatience
Homeopathic Remedies
Aconite
Indicated especially for those who often have strange and irrational fears, fears and sweating at night, a tendency to fevers, croup, and thirst.
Anacardium
Indicated especially for those who feel put down, isolated, and separated from the world; for those who feel pathological inferiority; those who feel need to prove themselves; test-taking anxiety in which the person goes blank.
Argentum nitricum
Indicated when there is antagonism within the self, the mind is of two wills, the person imagines devils speaking in one ear and angels in the other, like Jekyl and Hyde. It is indicated for people who can be cruel and malicious, often after a history of being abused or belittled; for those who swear; and for those who act as if they lack a conscience.
Aranea ixabola
Indicated for excessive teasing, especially teasing and manipulating by acting cute; for those who act as a mischievous leader, inducing others to disobey; and for those who are fascinated with spiders.
Arnica
Used for children in shock, or who have never been well since a shock or trauma, even trauma from a difficult birth. It is often confused with Sulphur.
Aurum metallicum
Used for children who act like little adults; who want affection, but don’t know how to express emotional needs; for those who can be cold to their family, and have a hard time making friends. It is indicated for those who are perfectionist, and who can be bitter and negative; for those who try hard and don’t want to fail; for those who tend to sinus problems, nasal congestion, and moaning in sleep; and for those who feel better from music.
Baryta carbonica
Used for those who can be sweet, timid and fearful or be the class clown, acting goofy and acting out. It is indicated for apparent arrested or delayed mental, physical or social development; for children who are shy, self-conscious, with self-limitation, feeling defective. It is used for those with the fear of looking bad, being laughed at, and criticized; for those who feel incompetent and incapable. It is indicated for those who feel that they are being laughed at, mocked, or criticized; and for those who are timid due to fears, especially the fear of making a mistake. It is used for those who feel that they are being watched; for those who dare not look up; for those who act childish and immature; for those who have difficulty with schoolwork. It is used for those who are backward or behind; for those who are often the teacher’s pet; and for those who tend to tics and glandular swellings.
Baryta iodatum
Used for those who are irritable, hurried, restless, and nervous; who have difficulty concentrating; and who have a canine-like appetite.
Belladonna
Used for those who are forgetful, slow, and have a poor learning ability; sensitive to noise and light; have night terrors and fear of ghosts; look wild when angry; have large heads, with bright red cheeks. The belladonna person often looks well, even when sick; tends to otitis media; complains of hot and throbbing discomfort; and often craves cold drinks, especially made from lemons and oranges.
Bismuthum subnitricum
Indicated for children who cling desperately to their mothers and are terrified when alone and who tend to be thirsty for cold water, but can have acute stomach pain in which even water is vomited as soon as it reaches the stomach.
Bufo
Used for those who have difficulty relating well to others; have narrow focus; don’t understand danger; have seizures or autism; have a slow, coarse appearance; can hug or bite you; mast-urbate or show a premature interest in sex. These children rely on basic instincts and need instant gratification; are upset when not understood; cannot tolerate music or bright objects; often present with eczema, nail biting, and may have protruded tongue or a gaunt face with stupid expression.
Calcarea bromatum
Indicated for restlessness in flaccid, chubby children.
Calcarea carb
Indicated for those who feel unsafe; are afraid of robbers, dogs, heights, and airplanes — any situation with potential risk to physical safety; are cautious and protective; fear that others will perceive their confusion and think them insane; feel as if everything is horrible; are stubborn and methodical; are obstinate and strong-willed; can be slow, hesitating; and of a chunky build; and sweat on the head as infants.
Calcarea phosphorica
Indicated for those who feel frustrated and dissatisfied; act fussy and peevish; for young children who are restless, shy, and fearful, but who love to take chances and play tricks, even act like daredevils. These children feel as if they are away from home and must get home; are athletic; love travel, change, and new experiences; complain of growing pains, especially in the bones; desire smoked meats; tend to have abdominal gas, colic, slightly swollen abdomen; and often have tonsillar hypertrophy.
Cannabis indica
Used for those who feel isolated, disconnected, anguished, terrified, and even sometimes ecstatic. This remedy is indicated for those who feel spacey, confused, and inattentive; have time and space disorientation; fear going insane; feel like everything is a dream with even familiar things which seem strange or unreal (derealization); act as if in a dream or off in space; can’t pay attention for long; but are good at science projects until theorizing causes them to lose touch with reality; are absent-minded; can be obsessive-compulsive; appear as if on drugs with a “stoned” look in eyes; and have parents who used marijuana excessively. There are three common behavioral variations of this remedy: (1) presenting as laughing, giggling, and clowning around; (2) presenting as ethereal and airy; and (3) presenting as brassy, loquacious, and liking to dress up in olden-day clothes.
Capsicum
Indicated for those who are intensely homesick, discontented, brooding, irritable, absent-minded, disobedient, and angry; who appear extremely obstinate; who are contrary, even against something they want if suggested by someone else. Capsicum is prescribed for those who fear being censured and are easily offended; who are restless, clumsy, and run into things; who have difficulty sleeping at night, but yawn during the day. It is used for those who can wake in a fright, screaming, or full of fear and who are worse form any draft, even warm air. Capsicum children are often seen in daycare with frequent otitis and bright red ears. They can have a pale face and puffiness under the eyes, as well as rashes.
Carcinosinum
Indicated for those who are fearful, timid, unhappy, worried, and obstinate, yet sensitive to reprimand and music; appear dull of mind, disinterested, and averse to conversation. They can be very sympathetic to others; can be very tidy or very messy; love to travel and will over-extend themselves; frequently suffer from insomnia; and strongly crave or dislike salt, milk, eggs, fat meat, and/or fruit. The onset of symptoms often occurs after a severe reaction to a vaccination. Frequently there is a family history of cancer. These individuals may have brownish cafe-au-lait complexion with many pigmented moles, bizarre tics, or blinking eyes.
Chamomilla
Indicated for those with bad temper, who are very irritable and impatient; who are complaining, frustrated, restless, and thirsty; who are contrary, not knowing what they want; who demand one thing and then want something else. The chamomilla child is fidgety and quiets down once he has attracted attention. He wants to be carried everywhere, but will whine and scream. He will settle down if carried, jiggled, or rocked. These children show aversion to being touched with hypersensitivity to pain, feel pain is unbearable, feel that everything is intolerable, and can become so hyperactive that he will get exhausted and begin to cry. The child shows dullness of the senses with a diminished power of comprehension, as if they were hard of hearing. All symptoms are worse at night
Cina
Indicated for children who are cross, contrary, and disobedient with very difficult behavior. These children do not want to be touched or looked at and turn away when approached. Nothing satisfies them for long. They are restless, fidgety and fretful, especially during sleep. They grind their teeth at night and wet the bed, and may have parasites, such as pinworms. Their sleep is restless, accompanied by jerking, frequent swallowing and coughing. They often sleep on their abdomen or the hands and knees (Medorrhinum).
They may have an irritated nose causing a constant desire to rub, pick, or bore into it until it bleeds. Their ears can be itchy. They often show twitching of the face muscles and eyelids, and are even inclined to seizures. Their appetite can be ravenous with strong thirst, and craving for sweets. These children often have large bellies.
Colocynthis
Indicated for those who are easily offended, especially by feeling unappreciated, by insults, or humiliations. They are moody and overly sensitive, and want to be alone. They tend to have abdominal cramps and sciatic pain, and may bend forward for relief.
Cornus circinatus
Indicated for those who don’t want to think, read or work. They have an inability to concentrate on thoughts, don’t understand what they are reading, and tend to aphthous stomatitis, flatulence, and weakness upon waking.
Crot. horridus
Indicated for those who are intense, animated, hurried, restless, and talkative. They have many fears, especially that someone might be following them or that they hear footsteps behind them. They fear being alone, spirits, ghosts, snakes; and can strike out in fits of rage. They resent and blame other children for getting them into trouble, report dreams of hairy spiders, and tend to have hives and epistaxis.
Cuprum metallicum
Indicated for those with anxiety at night, fears of kidnappers or the house catching fire, and are known for sticking their tongues out.
Ferrum metallicum
Indicated for those who are strong-willed and persistent, fight for their beliefs, have a sluggish mind with difficulty collecting their thoughts, tend to anemia and headaches, are often obese, with an aversion to eggs, and crave or detest tomatoes
Gallic acidum
Indicated for those who will hurt their loved ones.
Helleborus
Indicated for those who feel stupid, that they cannot cope with life’s challenges, and that their mind is sluggish. They appear dull and unresponsive; often have a history of encephalitis or head injury, and have difficulty memorizing or articulating thoughts. They have a tendency to despair and a strong aversion to making any effort, yet are easily angered. They have been observed to bite their spoon when eating without being aware of it, have a history of fever and/or head injury. One often needs to follow quickly with Hyoscyamus. This remedy picture is often easily confused with Sulphur and Medorrhinum
Hyoscyamus
Indicated for difficult children with poor impulse control, even though engaged in premeditated actions; talk excessively with episodes of mania and rage that might include hitting and screaming, also inclined to depression after manic phase; can be manipulative, lying, and violent; seem unable to think; unresponsive to questions or cannot bear anyone talking to them; intense and violent excitability with fear, delirium, and the delusion of being poisoned; feelings of abandonment, jealousy, suspicion; fears of dark, dogs, water; delirious; delusions of animals, of being pursued by enemies, as if s/he might be injured by surroundings; sees ghosts, specters; very animated, seeming silly and foolish; smiling and laughing at everything, often inappropriately; talks nonsense; acts out ridiculous gestures like a dancing clown or monkeys, trying to be center of attention, often with sexual overtones; giddy; love to run around naked, can be a totally shameless exhibitionist with bizarre behaviors for shock value, including cursing; tries to embarrass parents; jealous of their siblings, often may injure them; cannot tolerate being covered up.
Kali bromatum
Indicated for restless children, who always have to be doing something, especially with the hands, including activities like throwing.
Lachesis
Indicated for those who are loquacious, agitated and hyperactive, and restless and moody with strong emotions. They may be very jealous of siblings, or even of the same sex parent, and tend to be vengeful, sarcastic and nasty. They can be especially hurtful (and intuitively accurate) with insults; and can have a self-destructive personality, with a marked lack of confidence and a tendency to severe depression, withdrawal, and hopelessness. They hate any kind of physical or behavioral restriction, like tight clothing or being “grounded”; and cannot bear authority and run away from home. They tend to self-criticism and irritability; often reproach themselves severely; and may also show aggression which surfaces easily and makes them difficult to live and work with. They are known for suspicion with a marked preoccupation about others; and frequently feel that others are often criticizing them and putting them on the defensive. All symptoms are worse upon waking, when they typically feel unrefreshed and even more agitated, often complaining of a suffocative feeling.
Lycopodium
Indicated for those who are insecure, who act like bullies, and are cocky and boastful, often with overcompensation. They may show a marked lack of confidence and many fears, with underlying cowardice; can be dictatorial and bossy at home where they feel safe; and may have delusions of being a great person. They fear looking bad, need to cover up; are afraid of failure; are afraid to try anything new or to try again having failed once.
They fear being injured; may see phantoms and other images; display both fear and bravado; are usually intelligent and may look older than their years, but often suffer from dyslexia, confusing words or letters. They may show performance anxiety, prefer younger friends, want to please authority figures, tend to have abdominal gas; get more tired, restless, and irritable between 4 and 8 p.m. These children don’t want to sit down at the dinner table, but prefer to run around.
Lyssinum
Indicated for those who bite, growl, snarl, scratch, and act rabid. They are easily enraged; angry, but repent quickly, have remorse. They feel tormented and abandoned, as if they have suffered some wrong. These children feel as if they have been injured or abused. They often have a history of abuse, and may be children of violent parents. They strike out at presumed tormentors; and are self-destructive, with an impulse to cut his or her self. They can be defensive, as if being attacked or insulted. They may have a history of dog bite; animal-like behavior; aggravated by sound of running water; may have fears of water or reflected water, dogs, small rooms. They may crave chocolate and salt and have enuresis.
Mancinella
Indicated for those who fear evil, devils, and being possessed; may develop fears or obsession with evil after seeing a scary movie; and may have delusions that his or her soul has been surgically removed. The child says someone is taking things away. They may have asthma or bronchitis.
Medorrhinum
Indicated for those who are irritable, agitated, and in a hurry. They may have a racing mind and lust for experience, especially sensual. They may feel a need to hide her/himself, because s/he has a defect or is somehow flawed. They have anticipatory anxiety; delusions that someone is behind him or her or that someone is touching their head; fear that something dreadful has happened; a sense that everything is strange or unreal; a fear of going insane; a terrible memory, and may be forget. They may be mentally dull, unstable emotionally, have fits, can be reckless and impulsive; obsessive-compulsive, rigid; may be cruel or loving to animals; want to stay up late at night, feels better at night, yet can fear dark and monsters. They may have a history of diaper rash as a baby, and later skin rashes and asthma; nail biting; hot feet; and may sleep with their knees to the chest.
Natrum muriaticum
Indicated for children who act like “little adults,” display extreme watchfulness; sit in their mother’s laps during the interview; are often tidy, not wanting to lose control; and are sweet, except with their family. They may show silent grief or may have shrieking tantrums; may be confidante to one parent and nasty to other; may have concomitant anorexia; may display shyness with urination, especially in a public place; may crave salt, worsened by the sun; and may dislike slimy foods and fat.
Natrum sulphuricum
A specific remedy for depression after head injury. It is often seen with grief after parents’ divorce. Children who want this remedy have a strong sense of duty to family; can be suicidal; suffer existential anxiety and may have a nihilistic attitude toward life; have sadness relieved by music; often experiment with drugs; are born older; and tend to have asthma and warts.
Nux moschata
Indicated for children who pass out with the slightest injury or no obvious provocation; are giddy, spacey, and mentally confused. These children can be the perfect child – cooperating with parents, sharing, doing chores, going to bed on time; and tend to sleepiness, constipation and dryness of eyes, mouth and tongue.
Opium
Indicated for children with difficulty concentrating; spaciness; painlessness of an obviously painful complaint; being out of touch; having complaints from fright or after head injury; having constipation; having sleep apnea; and the mother often having been given drugs during pregnancy or labor.
Platina
Indicated for children who are insecure, volatile, flirtatious, arrogant and contemptuous (usually girls); are forsaken and unloved with a need to reconnect to people, but have the illusion that others are physically and mentally inferior; and underneath have feelings of failure, rejection, and a lack of confidence. These children want to look good; and can be very forward with even young girls putting out a sexual message and tend to be jealous of other women. These children may be emotionally stuck, tending to live in and dwell on the past. They can have strong feelings of anger, indignation and paranoia. They may have overwhelming and aggressive impulses that provoke the most severe depression and confused states, alternately indescribably happy and laughing at the saddest thing, then insufferably sad, hopeless and terrified by any serious thought. They need excitement or melodrama; can be very restless children who cannot remain in one spot and may experience marked anxiety with trembling, as well as oppressed breathing and violent palpitations.
Phosphorus
Indicated for children with the fear of being unloved, isolated, and having lost all their friends; children who are psychic; and children who see ghosts, spirits, specters. They may have a sense of being on a distant island; are concerned that they have an incurable disease; are gregarious, bubbly, and good-natured; are sensitive, sympathetic, and kind; are sweet and compassionate; and can be spacey.
Scorpion
Scorpion is used for children who are violent if provoked or just for the fun of it, for children whose parents fear being harmed by the child; for children who lack conscience and compassion for the suffering of others. These children are detached, like solitude, can attack if bothered; and are indifferent to pain or pleasure.
Stramonium
Indicated for children who are violent or fearful; who are severely hyperactive, easily terrified, and inclined to violent agitation and fits of rage; and whose speech is loud, fast, and possibly incoherent. These children show feelings of terror and abandonment; are afraid of the dark, dogs, evil, suffocation and abandonment. Their thirst is great, yet they dread water. They have fears of death; believe s/he is always alone, and are especially afraid to be alone at night, become overly vigilant to combat these fears and become violent if controlled. They have nightmares and night terrors that become increasingly worse between midnight and 2 a.m. They often awake screaming; see ghosts, specters, spirits; have a horror of glistening objects; have delusions of animals, of danger; are clinging. They are aggressive; bite, kick, strike; use threatening language; can have seizures or personality change after a head injury, frightful episode, or trauma (especially being chased by dogs). They can be useful in autism or Tourette’s. These children can be sweet all day and have terrors at night.
Sulphur
Used for children who are egotistical; try to control feeling with mind; hate being scared; feel as if they are being scorned; have delusions that s/he has been disgraced; are messy and tattered but think they look fine. These children can be lost in thought, absent-minded, spacey; forgetful, loses things; has visions; full of theories and dreams, loves science fiction; can be a loner with limited social skills; prefers computers, reading, mechanical things
Tarentula hispania
Indicated for children who are frenzied, are worse with music; act wild and crazy; love to sing and dance; feel as if never enough time; feel as if s/he has been insulted; sense of a stranger in the room. They see faces on closing eyes; have episodes of raving delirium; are mischievous and sneaky; tease and hide; cut things; hurried, always restless.
Tuberculinum
is indicated for those who revolt against restriction and need to feel free. They always desire and seek change, travel and have new experiences; always feel dissatisfied; and feel as if there is never enough time. They are afraid of (and often torment) dogs, cats; have delusions that s/he can fly, that someone is following her/him, that he is surrounded by animals; feel everything is strange; are compulsive and uncontrollable; are destructive; throw tantrums; break things; are precocious; and are often malicious.
Tuberculinum aviare
Indicated for those who show extreme restlessness with great weakness; diminished appetite of long duration; and a tendency to otitis.
Veratrum album
Veratrum album is indicated for those who are inconsolable after fancied misfortune; have a racing mind and agitated actions; and are driven to act on impulses. They may show religious mania; are overly religious; feels s/he is in communication with God; delusions that s/he is a great person or somehow distinguished. They have delusions of animals; are always busy but often fruitlessly so; have impulses to kiss or touch others; are hurried, restless, and fidgeting, poking others; and are precocious.
Zincum metallicum
Indicated for children who are fidgety and restless, and especially known for restless feet and legs. These children have an overactive nervous system; twitch, jerking, and even have convulsions; and are sensitive, irritable, and prone to rage. They often make mistakes in writing and speaking; feel like they have committed a crime; can have tendency to lick everything; and may look like little old people.
Suggested Bach remedies which are used for treatment of ADHD
Cherry 6 – re-establishing self-control; controlling impulses
Complementary homeopathic remedies: Stram, Hyosc, Bell, Verat, Bufo, Aur, Arg Nit, Alum, Plat, Hydr, Hep Sulph
Wild Oat 36 – when person cannot choose the thing on which attention has to be focused
Complementary homeopathic remedies: Bar-C, Calc-Ph, Graph, Med, Lach, Tarent, Puls, Carb-V
Clematis 9 – difficulty with focusing; disconnected
Complementary homeopathic remedies: Olnd, Nux-M, Staph, Asar, Cann-I, Op, Chel, Lac-C, Phos, Lac-N.
Chicory 8 – Love me – as a precondition of existence
Complementary homeopathic remedies: Dulc, Ars, Chel, Lil-T, Puls, Sep, Chin, Ant-C, Ang-V
Star of Bethlehem 29 – forsaken feeling, wrongly punished; , trauma of being neglected, trauma consequences (physical and psychical)
Complementary homeopathic remedies: Ign, Aur, Ph-Ac, Caust, Op, Nat-M, Arn
Impatience 18 – impatience, hotheaded
Complementary homeopathic remedies: Ip, Cham, Ars, Lyc, Sulph-Ac, Iod, Med, Tarent
Chestnut Bud 7 – to all who are immature, to learn on their own mistakes
Complementary homeopathic remedies: Bar-C, Graph, Tarent, Med






Great, comprehensive info on ADHD. There are other non-medical approaches to ADHD, from dietary changes to education, therapy, and behavioral support like Brain Balance. It combines all these interventions for a truly drug free approach to improving brain function and reducing symptoms. Their website is worth a read… http://www.brainbalancecenters.com
Very good indepth information. Good guidance for Homeopaths and for those who are already using Bach Flower Remedies. Interlinking of the two a surprising and useful addition. Many thanks.
I wasn’t aware of low blood oxygen leading to reduced dopamine levels. I assume that it happens not only via sleep apnoea. Thank you for this information.
This is a good general article on ADD/ADHD, but what about homeopathic options? Incidentally, I have seen SOME success with chiropractic and neurofeedback. For many, after one has already explored eliminationg potential food items, such as white sugar, food dyes, preservatives and excitotoxins (such as in MSG), and psych. factors (and spinal problems, which can surely cause anxiety and lessen mental focus), stimulant meds can be very helpful. Members of my family, including myself, have found this to be dramatically true. Yet, please be aware that meds like “Ritalin” (methylphenidate) are probably over-prescribed. and frequently will produce side effects, such as lessened bone and tooth density, visual floaters, and decreased height.
I’m not suggesting one (as doctor, patient or parent) absolutely rule out the use of these meds, simply that one do consider all the factors and make an educated choice. If I had had all these facts at my disposal in the nineties, I would have lowered the dosage, addted neurofeedback to our regimen, and made sure my family members were IMMEDIATELY placed on mineral supplements, herbs which are supportive of vision (such as eyebright and watercress), and probably some special eye-drops too.
Did you read all the three pages of this article? The homeopathic options are covered on the last page.
Very short: continue with the ADD/ADHD investigation through own homeopathic practice.
Very impressive research and thoughtful insight on possible causes of ADHD, including possible treatments. A comprehensive and objective article that educates and allows the reader to draw their own conclusions. Bravo! and Well Done!