Case Study
A female aged 62 years works full time as a Ceremony Officer and keeps fit by walking but admits that she is not an active person. She lives on her own, a nonsmoker, partakes in social alcohol and keeps good general health with no past or present medical, surgical or drug history. She has not had any previous history of fracture or any other injury.
The current injury occurred when she fell off her bed in the middle of the night with excruciating pain in her leg. She does not recall how or, what happened and has poor recollection of the mechanism of injury.
She suffered an acute trauma to her lower third of the left leg with extensive soft tissue contusion, haematoma, which extended down into her foot with swelling and pain. She managed to call the emergency number and was taken to a local hospital by ambulance.
She was admitted in hospital via Accident & Emergency department after a series of plain radiographs confirmed a closed displaced oblique fracture of the tibia and fibula (Figs.1a & 1b) The following morning, she was reviewed by the Trauma & Orthopaedic team at her local hospital, who scheduled her for open reduction and internal fixation surgery (ORIFS) with tibial intramedullary nail (Figs.2a & 2b). She was discharged from the hospital after 5 days with analgesics and, was to remain non-weight bearing using 2 elbow crutches.
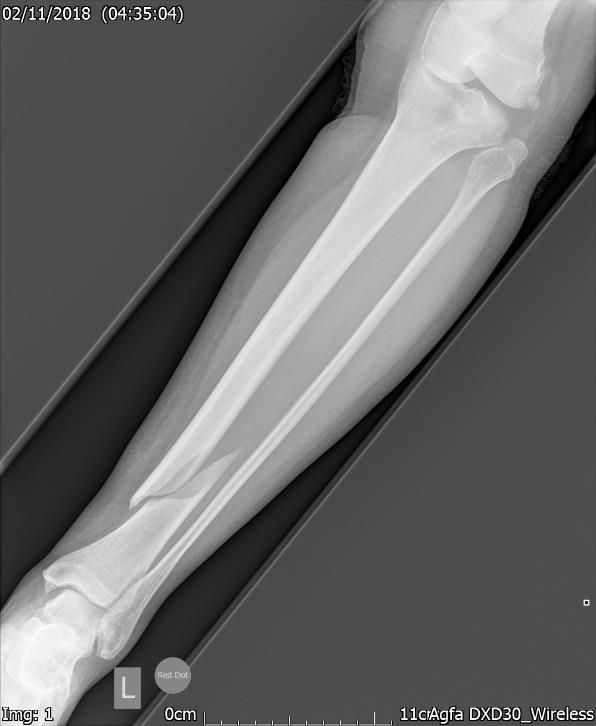
Figure.1a. Pre-surgery Xray – AP view – Closed displaced oblique fracture of the tibia.
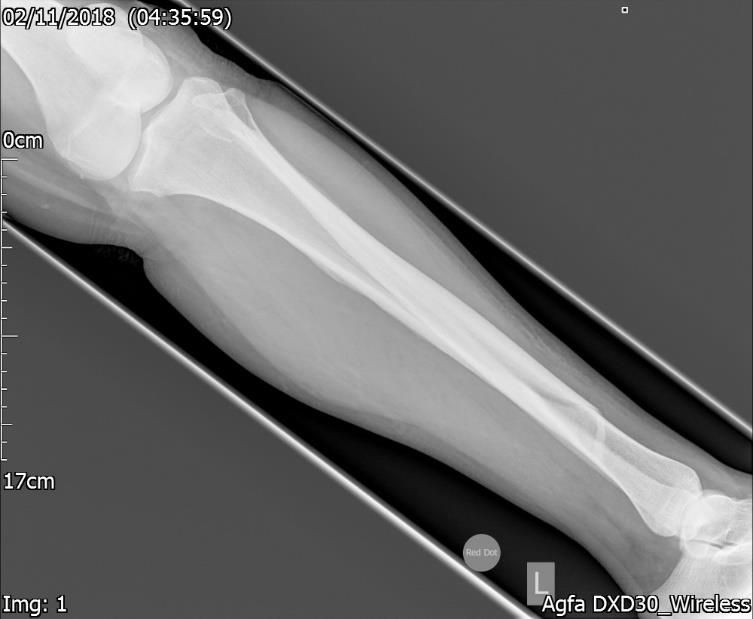
Figure.1b. Pre-surgery Xray – Lateral view – Closed oblique fracture of the tibia.
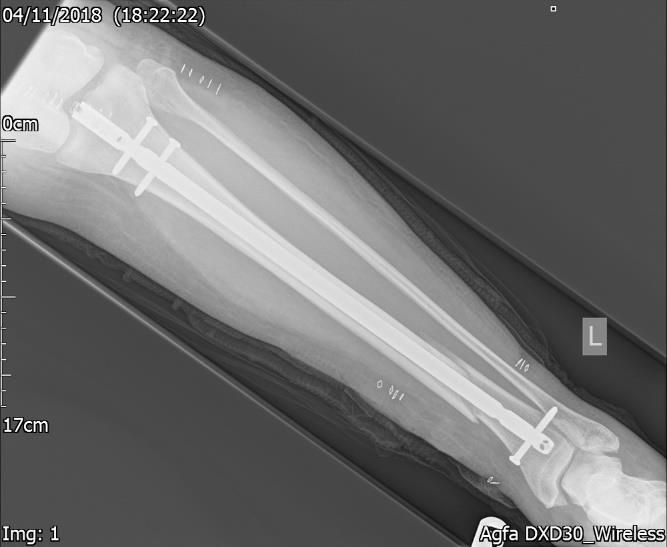
Figure.2a. 2 day post-surgery Xray – AP view – ORIF with tibial intramedullary nail.
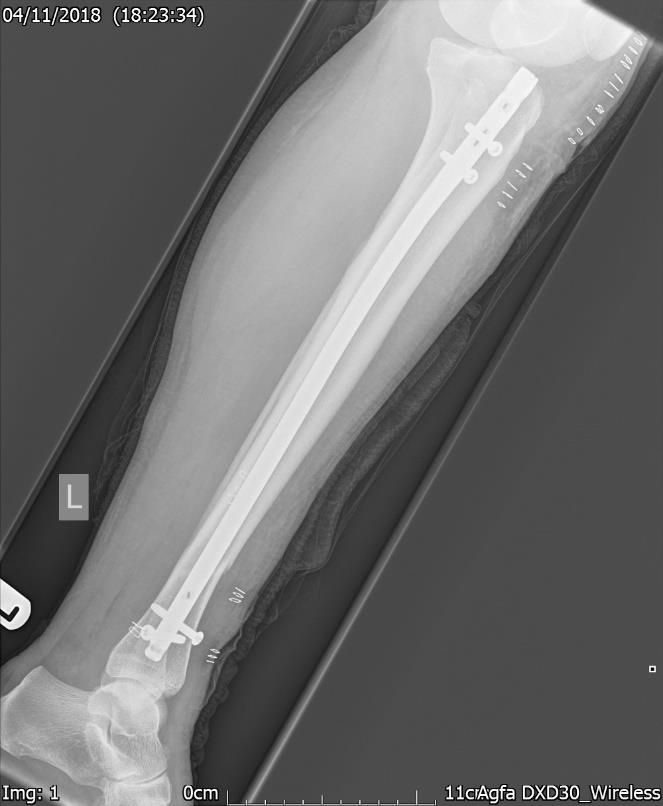
Figure.2b. 2 day post-surgery Xray – Lateral view – ORIF with tibial intramedullary nail.
She was also followed up in the out-patient physiotherapy department and remained under their care for 7 weeks. She was unable to look after herself since she lived on her own and had to stay with a family member for 5 weeks.
This along with being unable to work, had a big impact on her mental and financial health. She was experiencing bouts of anxiety, depression and was increasingly becoming frustrated and irritated.
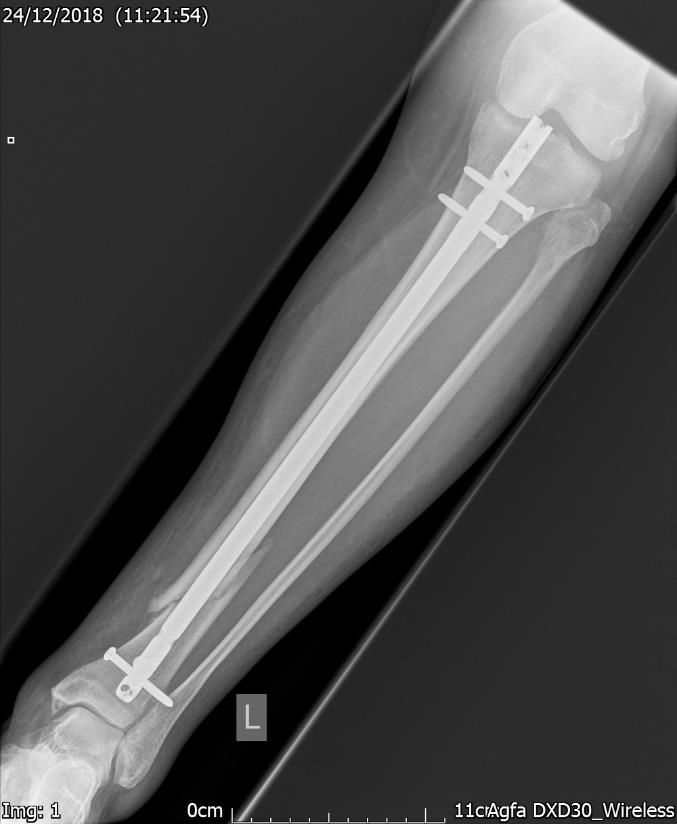
Figure.3a. 7 weeks post-surgery. Xray – AP view. Satisfactory internal fixation with fracture line clearly visible.
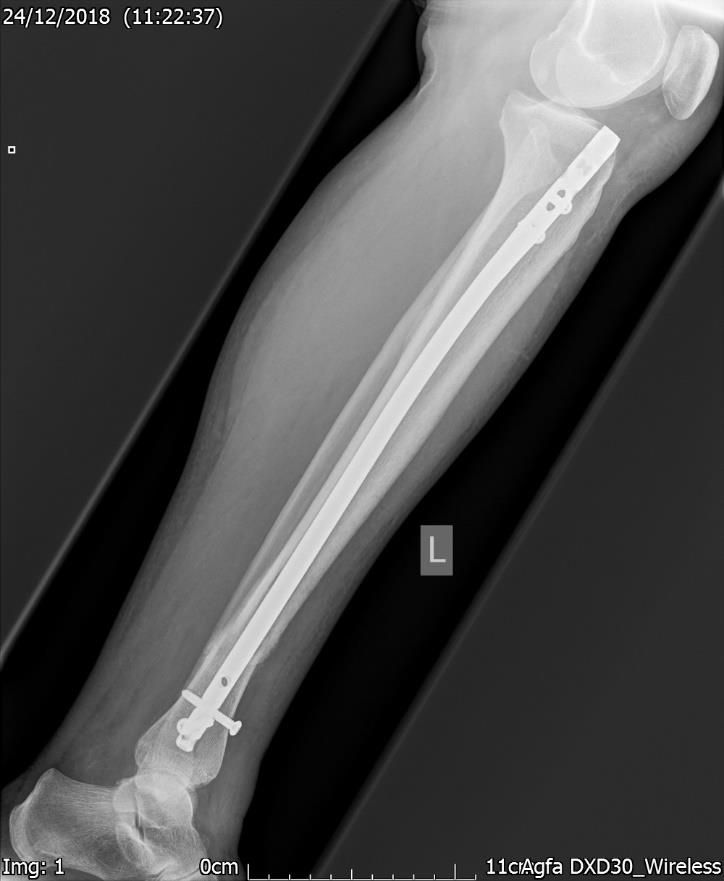
Figure.3b. 7 weeks post-surgery. Xray – Lateral view. Satisfactory internal fixation.
At 3 weeks, she was reviewed in the fracture clinic and the repeat x-ray (Figs. 3a & 3b) showed satisfactory internal fixation with good position and some callus formation. She was comfortable and happy with the management thus far with minimal swelling of the lower limb and, had intermittent pain which she controlled with reduced physical activity and analgesia.
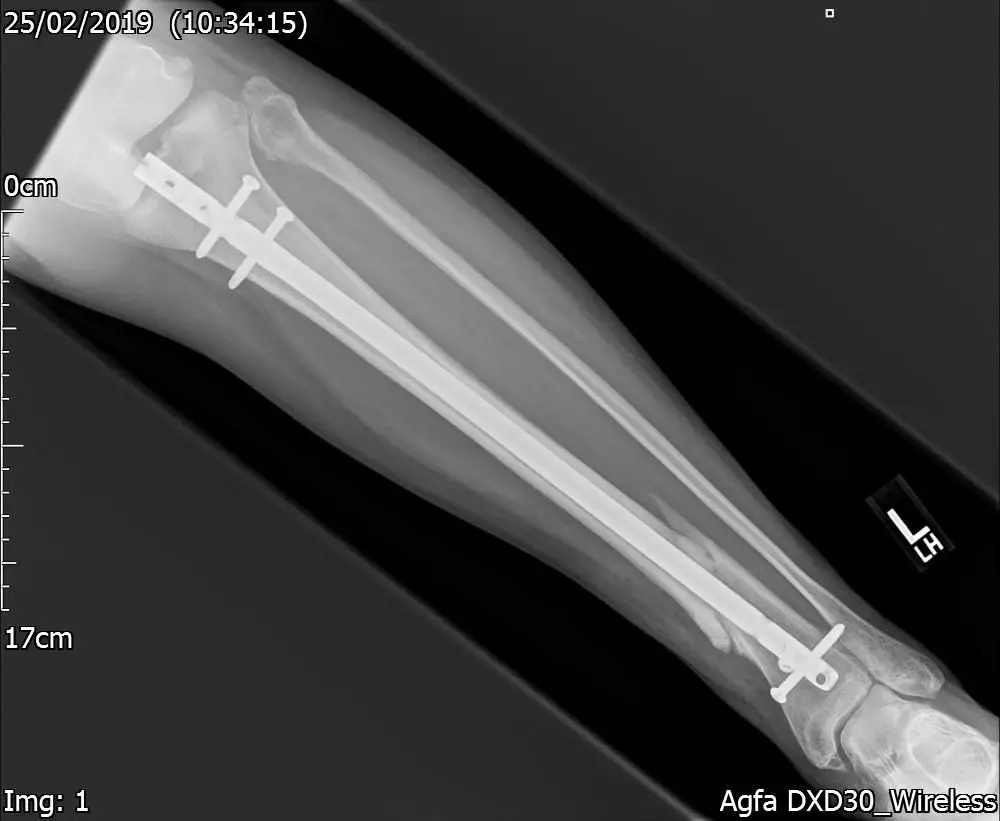
Figure.4a. 16 weeks post-surgery. Xray – Lateral view. Satisfactory internal fixation with some callus.
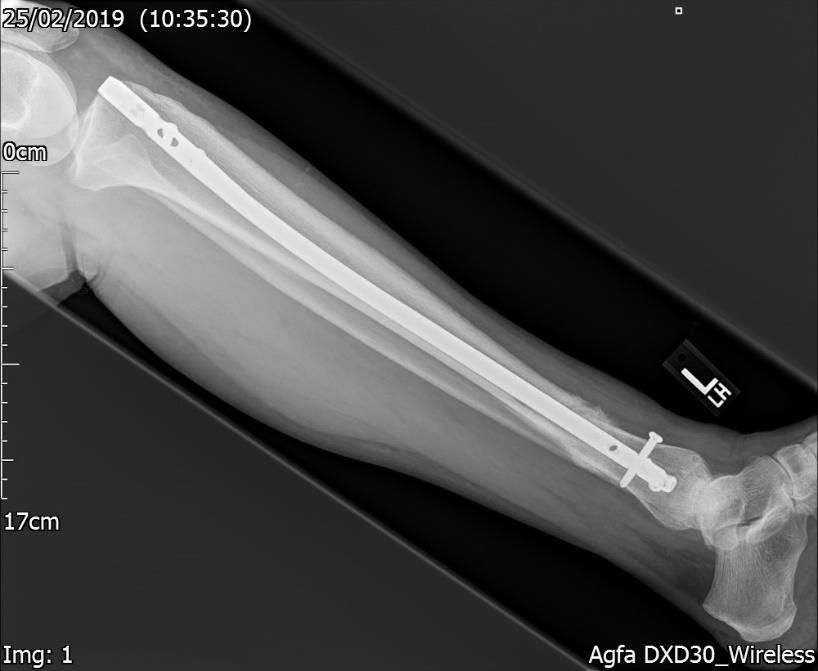
Figure.4b. 16 weeks post-surgery. Xray – Lateral view. Satisfactory internal fixation with some callus.
She was to be reviewed by the Trauma & Orthopaedic team in 8 weeks’ time. At her next review investigations showed the fracture line still clearly visible with some callus formation (Figs. 4a & 4b). The consultant advised that if this did not show any improvement at her next visit, she may need further revision surgery.
She was also under supervised exercise program with the next review in 6 weeks’ time. Unfortunately, she did not take this news well and her bouts of anxiety, depression, frustration due to lack of physical activity, got worse.
In order to attempt to promote healing, she searched the internet with an open mind for options, both medical and non-medical. She came across use of homeopathic medicine and contacted LC for advice and had her first consultation a week after the last x-rays (Figs 4a & 4b).
At this stage, the bone was showing no real sign of healing; there was mild swelling, manageable pain in the lower third of her left leg, surgical wounds had healed well and she was cautiously full weight bearing and relatively mobile.
Having considered all the ‘pros and cons’ of homeopathic treatment including benefits, minimal side effects and ‘nothing to lose’ attitude, patient gave informed consent to try classical homeopathy as a non-interventional alternative.

Figure.5. Symphytum officinale.
Symphytum officinale (Fig.5.) 200C* was given in water over 21 days with a break of 7 days after the first week. In addition, she was also given Calcarea Phosphate (15)(16) (phosphate of lime) 6X Tissue salts (cell salt, calcium phosphate), 4 tablets 4 times a day.
There are no known side effects, but the patient was to contact the clinic if anything untoward should happen. She was also given a Class 1 compression sock, exerting 18 -21 mmHg of pressure. This was to be worn daily to stimulate the micro-circulation and reduce any swelling.
Pain was monitored using Visual Analog Scale (VAS where zero (0) denotes no pain and 10 denotes excruciating pain) along with subjective review of her mental state which she tried to grade on a similar scale with zero (0) being very happy and 10 being no improvement or worse.
The main monitoring tool was going to be x-ray evidence of callus formation which will be the indication that the fracture was healing. Her VAS for pain was 4/10 and Mental state 5/10 before homeopathic treatment.
* C means that a substance is diluted in a ratio of 1:100 and the number preceding the letter indicates the number of times a substance has been both diluted and agitated – homeopathic word is succussed.
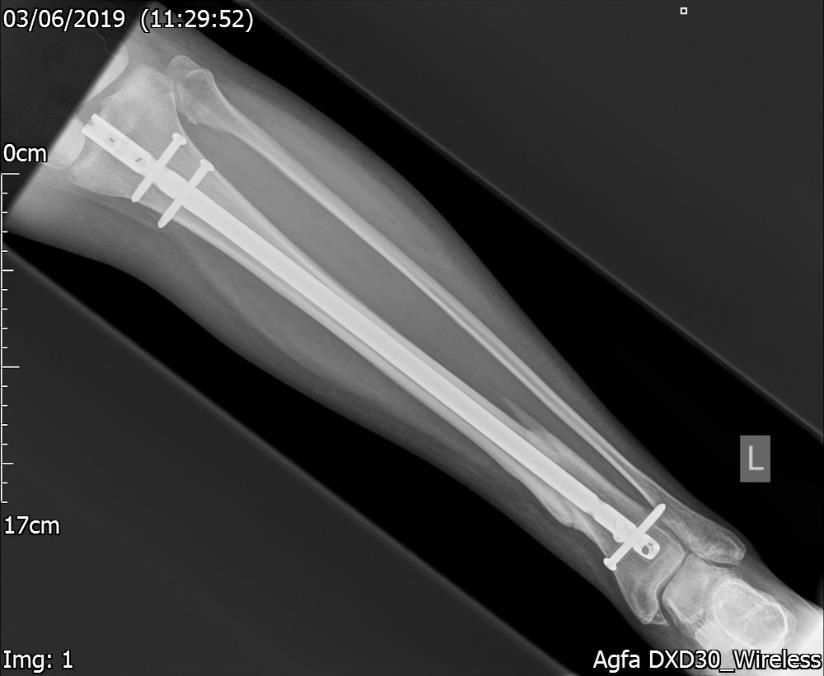
Figure.6a. 28 weeks post-surgery & 12 weeks post-homeopathy.
Xray – Lateral AP. Good callus formation with further evidence of non-union.
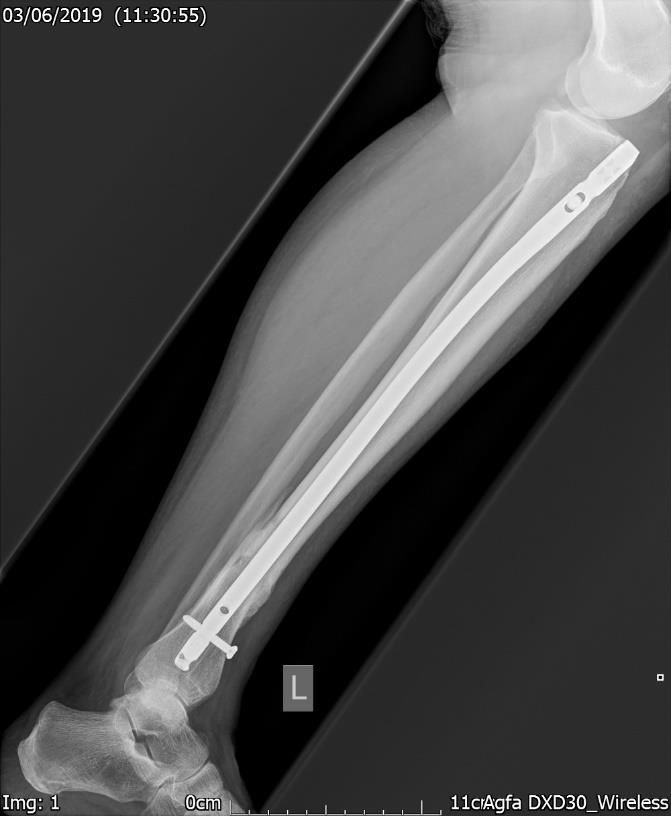
Figure.6b. 28 weeks post-surgery & 12 weeks post-homeopathy.
Xray – Lateral view. Good callus formation with further evidence of non-union.
She was followed up at 8 weeks after starting the homeopathic and compression treatment and it was shown on x-ray (Figs 6a & 6b) that there was significant callus formation and she was informed by the Trauma & Orthopaedic team that there was no further need for revision surgery.
She was allowed all privileges and discharged from the clinic on an SOS basis. There was no swelling, her pain was now 0/10 on a VAS and her Mental state 8/10. In her own words ‘I am relieved and feel positive that I can now get back to my active normal life’.
Discussion
In the United Kingdom there are approximately 850,000 new fractures every year, the rates of non-union have been between 5-10%. The cost to the NHS is £7,000 – £79,000 per patient. There is extraordinarily little published data, looking at the cost implications and overall results of treatments (1). Main risk factors include smoking, age, high oestrogen levels in post-menopausal women, diabetes, low Vitamin D levels, poor diet/nutrition, lack of exercise, certain medication including NSAIDs.
Local causes can include infection, mechanical instability and poor circulation. Most common bones to be affected are the tibia, humerus, talus and 5th metatarsal (1, 2). In addition, biological or mechanical factors can lead to non-union.
There is an increase in using therapeutic agents to treat skeletal injuries. The natural process of callus formation in bone healing, includes formation of Haematoma, soft callus, hard callus, remodeling . In order to achieve this, the body has naturally occurring chemicals in the body, growth factors such as bone morphogenetic protein, transforming growth factor beta, fibroblast growth factor, platelet derived growth factors and insulin-like growth factor.
These are proteins that are secreted by cells to carry out a specific action. In the case of bone healing, if these are impaired or lacking, this will result in delayed or nonunion. Growth factors in bone repair are usually stored in the extra cellular matrix (3, 4).
Conventional management of delayed or non-union fractures.
Current treatment includes bone stimulators. These can be expensive and have to be used daily by the patient. In some patients it may not be an option dependent on the position and site of the fracture. Bone stimulators give low level pulses of electromagnetic energy (PEMF), which activates bone growth signaling pathways and increasing the number of bone cells.
It must be used for a minimum of 2 hours daily dependent on fracture, and it is single patient use and expensive, current cost £2,407 per patient. It is also only available for certain fractures under NICE guidelines (5).
PEMF offers a conservative management of delayed or non-union of long bone fractures but has its limitations. It may offer some benefit but the outcome remains inconclusive and insufficient to inform current practice (6).
Various surgical techniques are described in literature and external fixators are popularly used to provide support for the long bones offering early weight bearing and stability for bone healing (7). As with all surgical procedures especially revision surgery there are complications including a lengthy surgery, significant bone defect following excision of diaphyseal atrophic bone and there is risk of wound infection (8). However, there are techniques which can be employed to reduce this risk as shown in short series involving non-union fracture of the femur (9).
Cell Therapies are used to restore and improve tissue function; this can be from human bone marrow cells injected directly into the site of non-union (4, 10). With bone grafts, either allograft or autologous, there is a risk of infection and they can be painful and time consuming (8).
Bone grafts are normally harvested from the patient’s Iliac crest which means another site of trauma and can take up to 3 months or longer to heal. All surgery carries a risk of deep vein thrombosis (DVT), bleeding, infection, nerve damage and not all patients are suitable for this type of surgery. Patients are normally non weight bearing post operatively until wound healing is achieved (8).
Homeopathic treatment
Homeopathy is a branch of complementary medicine based on scientific evidence that the body’s own defence mechanisms can be stimulated into healing (11, 12). It is based on the basic principle of ‘like cures like’ which dates back to Hippocrates (460-377BC). Homeopathy is a therapeutic system founded in 1755 by the German medical doctor Samuel Hahnemann (12).
He discovered that if he took regular doses of Cinchona bark it produced symptoms of Malaria. He believed that giving a patient a homeopathic dose of medicine which, if given to a healthy person would produce similar symptoms of that same illness, it would trigger a healing response.
Symphytum Officinale is a homeopathic remedy made from Comfrey root (Fig.5.), a native plant to Britain. It is also known as ‘knit bone plant’ which was traditionally used in ancient Britain to help heal bones and treat wounds (11, 12, 14, 15, 16, 17).
Symphytum Officinale has been used as a traditional medical plant for joint complaints. Allen’s Materia Medica states it is an excellent remedy for fractures, mechanical injuries, facilitating union of fractured bones and favours production of callus. There are many scientific studies showing the effectiveness of Homeopathic treatment (12, 14, 15, 16, 17, 18, 19). Tsintzas & Vithoulkas (14) published four cases of non-union fractures showing the successful use of Symphytum Officinale homeopathically. In the paper it was shown how Symphytum Officinale was used to speed up the healing process of fractures. In all cases the protocol was a 30C once daily for 10 days and after that 200C once a week for three weeks.
Case 1 was a two week old, comminuted fracture of right clavicle showing no callus formation in an athlete who was also a heavy smoker. He was offered surgical intervention but chose the homeopathic route. Three 3 weeks after starting on the Symphytum treatment the radiological pictures showed defined and solid callus bridging of the bone fragments.
The patient level of pain was reduced and there was increased mobilisation of the shoulder joint. He returned to sports in 8 weeks post injury. Case 2 was a footballer with minimally displaced fracture of distal right radius, immobilised in full plaster, whilst using the homeopathic treatment Symphytum Officinale with the same dose as in case 1.
After 3 weeks, x-rays showed solid callus formation in the fracture site and he was back to full training in 6 weeks after injury. Case 3 was a 43 year old man with minimally displaced intraarticular fracture of the distal radius which was immobilised and given the same dose of Symphytum Officinale. 3 weeks post injury the x-rays showed solid callus formation and the patient had minimal pain and almost full function of his hand.
Case 4 was a comminuted fracture of the fifth metatarsal after inversion injury. He was put in a weight bearing cast with Symphytum Officinale and 19 days post injury showed excellent union with improved function.
The literature is replete with studies and publications outlining the positive benefits of compression garments on ergogenic and physiological factors during exercise (20, 21, 22). Traditionally compression, either in a form of stocking or anti-gravitational bandaging, has been used in patients with venous insufficiency and venous ulcers. In sport they are widely used to enhance exercise performance, improved recovery, improved muscle tissue oxygenation, ameliorate venous circulation, reduce orthostatic intolerance, and generally change the hemodynamics (blood flow distribution) (23, 24, 25, 26).
There are very few specific studies assessing the usefulness of compression in either the management of fracture or non-union. In a randomised controlled trail in 90 patients presenting with ankle fracture showed that AOFAS (American Orthopaedic Foot & Ankle Society score) was significantly improved with the compression in 59 patients who were treated conservatively in comparison to 31 who underwent surgery.
Compression also improved functional outcome and quality of life following fracture of the ankle even though large number of patients (86) developed deep vein thrombosis (27). Another systematic review involving 16 studies showed that intermittent compression appears to be an effective modality to enhance fracture and soft-tissue healing. However, the number of subjects in human studies was small, and adequately powered and, that randomised controlled trials in humans were required to produce stronger clinically relevant evidence.
Conclusion
This case study demonstrates that using homeopathic medicine has a part to play in the management of non-union or delayed union fractures. There are case controlled studies which provide evidence that a combination of Symphytum Officinale, Tissue Salts and compression hosiery is an effective conservative treatment for non-union or delayed union of fractures. There is however lack of conclusive level 1 evidence in the literature.
In the final analysis it is a choice between revision surgery, which carries with it various risk factors and homeopathy, which has minimal or no adverse effects. The treatment plan described in this case offers patients a safe, gentle option with significant cost savings.
Patients Perspective
‘I was so disappointed after following the hospital advice to learn my bones weren’t healing as expected and I may have to have a further operation should this not change. I already knew that I needed to help myself and seek homeopathic advice. I followed the advice and took the medicine given. I was so pleased to learn of the major improvement it had made in 6 weeks, so no further operation and my leg is so much better in all ways.’
Corresponding author and contact details:
Ms Lucille Cowell – [email protected]
REFERENCES
1. Mills LA, Simpson RW. The relative incidence of fracture Non Union in the Scottish Population (5.17 million) a 5 year Epidemiological study. BMJ Open. 2013,Feb 8;3(2).
2. Sloan A, Hussain I, Maqsood M, Eremin O, El-Sheemy M. The effects of smoking on fracture healing. Surgeon. 2010,8:111-116.
3. Liebernam J, Daluiski A, Einhorn T. The Role of Growth Factors in the Repair of Bone. J Bone Joint Surg Am. 2002;84(6):1032-44.
4. Jain Lu Qi-Yang Wang Jia -Gen Sheng. Exosomes in the Repair of Bone Defects: Next Generation Therapeutic Tools for the Treatment of non-union. Biomed Research International. 2019,ID 1983131. https://doi.org/10.1155/2019/1983131.
5. NICE Guidelines. EXOGEN ultrasound bone healing system for long bone fractures with non-union or delayed healing. MTG12. 2019.
https://www.nice.org.uk/guidance/mtg12
6. Griffin XL, Costa ML, Parsons N, Smith N. Electromagnetic field stimulation for treating delayed union or non-union of long bone fractures in adults. Cochrane
Database Syst Rev. 2011,Apr 13;(4):CD008471.
7. Hashmi MA, Ali A, Saleh M. Management of non-unions with mono-lateral external fixation. Injury. 2001,Dec;32 Suppl 4:SD30-4.
8. Ryzewicz M, Morgan SJ, Linford E, Thwing JI, de Resende GW, Smith WR. Central bone grafting for nonunion of fractures of the tibia: a retrospective series. J Bone Joint Surg Br. 2009,Apr;91(4):522-9.
9. Davda K, Heidari N, Calder P, Goodier D. ‘Rail and Nail’ bifocal management of atrophic femoral nonunion. Bone Joint J. 2018,May 1;100-B(5):634-639.
10. JF Connolly , R Guse , J Tiedeman R Dehne. Autologous marrow injection as a substitute for operative grating tibial non-union. Clinical Orthopedics and related Research. 1991,259-270.
11. Staiger C. Comfrey: ancient and modern uses. Pharm J. 2007,279: 22–29.
12. Hahnemann, Samuel; Devrient, Charles H. (tr.); Stratten, Samuel (notes) (1833).
The Homœopathic Medical Doctrine, or Organon of the Healing Art. Dublin: W.F. Wakeman. OCLC 32732625. OL 6983421M. – Full text in PDF and DjVu formats.
13. Stub T, Musial F, Kristoffersen AA, Alræk T, Liu J. Adverse effects of homeopathy, what do we know? A systematic review and meta-analysis of randomized controlled trials. Complement Ther Med. 2016,Jun;26:146-63.
14. Tsintzas D, Vithoulkas G. Fracture treatment with the aid of the homeopathic remedy Symphytum officinale. A report of four cases. Clin Case Rep Rev 1. 2016, doi: 10.15761/CCRR.1000234.
15. Oberbaum M, Yakovlev E, Kaufman D, Shoshan S. Effect of Arnica montana and Symphytum officinalis on bone healing in guinea pigs. British Homeopathic Journal. 2004,83: 90
16. Sharma S, Sharma N, Sharma R. Accelerating the healing of bone fracture using homeopathy: a prospective, randomized double-blind controlled study. BMC Complementary and Alternative Medicine. 2012,12(1):O61. PMCID: PMC3373423.
17. Sakakura CE, Neto RS, Bellucci M, Wenzel A, Scaf G, Marcantonio E Jr. Influence of homeopathic treatment with comfrey on bone density around titanium implants: a digital subtraction radiography study in rats. Clin Oral Implants Res. 2008,19(6):624-8.
18. William Boericke. Boericke’s New Manual of Homeopathic Materia Medica with
Repertory. B Jain Publishers Pvt Ltd. 2008(6). ISBN 10: 813190184X. ISBN 13: 9788131901847.
19. Allen TF. The Encyclopedia of Prue Materia Medica. New York : Boericke & Tafel, [c1874]-79;2011. http://resource.nlm.nih.gov/64240040R
20. Agu O, Baker D, Seifalian AM. Effect of graduated compression stockings on limb oxygenation and venous function during exercise in patients with venous insufficiency. Vascular. 2004;12(1):69–76.
21. Duffield R, Portus M. Comparison of three types of full-body compression garments on throwing and repeat-sprint performance in cricket players. British Journal of Sports Medicine. 2007;41(7):409–414.
22. Kraemer WJ, Volek JS, Bush JA, et al. Influence of compression hosiery on physiological responses to standing fatigue in women. Medicine and Science in Sports and Exercise. 2000;32(11):1849–1858.
23. Platts SH, Tuxhorn JA, Ribeiro LC, Stenger MB, Lee SMC, Meck JV. Compression garments as countermeasures to orthostatic intolerance. Aviation Space and Environmental Medicine. 2009;80(5):437–442.
24. Privett SE, George KP, Whyte GP, Cable NT. The effectiveness of compression garments and lower limb exercise on post-exercise blood pressure regulation in orthostatically intolerant athletes. Clinical Journal of Sport Medicine. 2010;20(5):362– 367.
25. MacRae BA, Cotter JD, Laing RM. Compression garments and exercise: garment considerations, physiology and performance. Sports Medicine. 2011;41(10):815–843. de Glanville KM, Hamlin MJ. Positive effect of lower body compression garments on subsequent 40-km cycling time trial performance. Journal of Strength and Conditioning Research. 2012;26(2):480–486.
26. Sultan MJ, Zhing T, Morris J, KurdyN, McCollum CN. Compression stockings in the management of fractures of the ankle , a randomized controlled trial. Bone Joint J. 2014 Aug;96-B(8):1062-9.
27. Khanna A, Gougoulias N, Maffulli N. Intermittent pneumatic compression in fracture and soft-tissue injuries healing. Br Med Bull. 2008;88(1):147-56.