Homeopathy has been used with humans for more than 200 years, and domesticated animals for almost as long. The extensive use of homeopathy with wild animals, on the other hand, has been considerably shorter. As the use of homeopathy with wildlife has grown, it has become clear there are some key differences from treating domestic animals. After a brief overview about wildlife rehabilitation, some of the key differences will be described, followed by some specific wildlife cases.
ABOUT WILDLIFE REHABILITATION
Wildlife rehabilitation is the temporary care of injured, orphaned, or otherwise distressed native wildlife, so that healthy animals may be released back to their native habitat. While there are a growing number of wildlife rehabilitation centers across North America, the majority of wildlife rehabilitators operate out of home-based rehabilitation facilities. They use areas of their homes and yards that are isolated from other family activities.
Rehabilitation operations are often funded by the individual rehabilitator or through a non-profit, tax-exempt organization status. Less than one percent of the rehabilitators are paid for their wildlife rehabilitation work. Wildlife rehabilitation has professional associations, publications, educational opportunities and increasingly professional standards of care and husbandry. Both state (or provincial) and/or federal permits are required to rehabilitate wildlife, including birds, mammals and herptiles. There are an estimated 12,000 licensed wildlife rehabilitators in North America (for more info, visit www.ewildagain.org/ColoRecBooklet.pdf).
Wildlife rehabilitators must perform a variety of duties. They spend considerable time talking with the public on the phone to prevent human-wildlife conflicts, resolve any problems that have already occurred, and arrange for the public to surrender wild animals that need care. Rehabilitators admit wildlife to their facilities, collect information about the reasons the animal is delivered for rehabilitation (e.g., hit by vehicle, attacked by pet, fell out of nest), and initiate case records. After conducting a basic assessment of the animal, they initiate first aid care based on standard protocols (e.g., place in a secure container, provide heat and quiet). They acquire and prepare diets needed for the species, age, and condition of the animal, which can range from milk replacers to insects to small rodents. They must feed the necessary amount at the appropriate frequency with the correct technique.
Rehabilitators must have a variety of effective and safe cages and housing for the different species, ages and conditions to be rehabilitated. They need adequate space to meet the needs of the species (e.g., quarantine, not having prey species near predators, allowing flock species to be near others of their kind). Facilities must be cleaned regularly and kept sanitary. They need to maintain a variety of supplies, such as heat sources, feeding instruments, gloves, nets, and so forth.
The wild animals must be released back to the appropriate habitat when they are capable of surviving independently.
Rehabilitators consult with veterinarians to ensure that the animals get appropriate medical care, and as required by their state and federal permits. Their veterinarians perform diagnostic and treatment protocols, such as radiographs and surgery. Many veterinarians, however, instruct rehabilitators to perform a basic assessment and initiate first aid protocols and supportive care (e.g., heat, fluids, cleaning minor wounds), as well as to administer medications on their instruction. Rehabilitators discuss euthanasia decisions with the veterinarian. Some conditions that would be considered minor for a domestic animal that is cared for in a home may prevent the animal from living independently in the wild, and prompt a possible euthanasia decision.
REASONS REHABILITATORS CONSIDER HOMEOPATHY
Wildlife rehabilitators want to provide high quality care for the animals so that they may achieve good health and be released back to the wild. They want to reduce invasive and costly procedures that stress animals already compromised by captivity, handling, and often injury. They want to reduce possible side effects from administering conventional medications (e.g., diarrhea after use of antibiotics; joint damage from corticosteroids). Rehabilitators want to accelerate the animal’s recovery and release to the wild. Some rehabilitators have voiced concerns about the use of allopathic medicines with wildlife due to the uncertainty of the medications overall effectiveness with wild animals and difficulty with calculating dosages to very young or small animals (e.g., an 8 gram weasel or finch). They also want to reduce or eliminate antibiotic resistance in the animal or the environment.
Since the early 1990s, wildlife rehabilitators have become increasingly interested in holistic modalities. Some rehabilitators have attended training programs and conference sessions on the topics, read publications, purchased medicinal herbs and homeopathic medicines, and begun working with holistic veterinarians. With the help of holistic veterinarians, wildlife rehabilitators have had acupuncture, chiropractic, botanical medicine, nutritional supplements, flower essences, and homeopathy used with a wide range of species.
Homeopathy is considered to be a very attractive modality for wildlife for a variety of reasons. It has been safe and effective with humans and animals around the world for more than 200 years. It has treated diverse physical, emotional, and mental conditions – including some that are either difficult or unable to be treated allopathically. Homeopathy helps the animal heal itself, instead of suppressing or palliating symptoms. It is relatively easy to administer homeopathic medicine to wildlife, at times without handling. Plus by applying the principle of the minimum dose, frequent capture and handling to administer medications is unnecessary. Less capture and handling translates to reduced stress and risk for the animal and handler. Homeopathic medicines are relatively easily accessible and more cost effective than conventional medications. Plus, rehabilitators are hearing about a growing number of successful cases where homeopathy has helped wildlife recovery at an accelerated rate.
Thus, it is not surprising that an increasing number of wildlife rehabilitators are turning to homeopathy. More than 600 wildlife rehabilitators have attended one and two-day seminars on the use of homeopathy for first aid and trauma care with wildlife presented by WildAgain Wildlife Rehabilitation (a team of rehabilitators and homeopathic veterinarians) since 1997. These seminars have been held around North America as independent programs or in conjunction with regional or national rehabilitation conferences. Articles and papers on homeopathy with wildlife have been published in rehabilitation publications, as well as in veterinary and homeopathic journals.
As a result, wildlife rehabilitators are increasingly contacting homeopathic veterinarians and asking for advice with acute wildlife trauma. Some will be relatively unfamiliar with homeopathy and seek help just as clients would with domestic animals. Others may have been to homeopathy seminars, taken the basic case, repertorized, and be seeking clarity on which of several remedies might best follow an initial remedy. The following information is offered to help support veterinarians treating wild animals or working with wildlife rehabilitators.
WORKING WITH WILDLIFE IS DIFFERENT FROM DOMESTICATED ANIMALS
Most homeopathic veterinarians work primarily with domestic animals, such as cats, dogs, horses and livestock. The human companions or owners of these animals provide food, shelter, water and arrange for veterinary care. They often provide considerable history on the animal. The cases are usually chronic. Wildlife cases are generally very different as discussed below:
Reason Wild Animals Arrive for Care
While most domestic animals may arrive at the homeopathic veterinarian clinic for a general ‘wellness’ examination or treatment of a chronic condition (or an acute flair-up of a chronic condition), wild animals do not. Wild animals stay in the wild unless something severe happens that they cannot resolve on their own, allowing people to capture and restrain them. Wild animals often arrive with serious acute conditions. Research into the relative frequency of occurrence of twenty-eight major categories of conditions presenting in wildlife cases is shown in Figure 1. 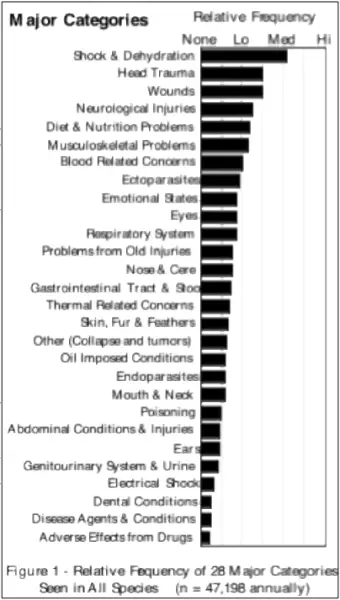 The relative frequency of occurrence of specific conditions seen in wildlife is shown at the end of this paper in Figures 2-4.
The relative frequency of occurrence of specific conditions seen in wildlife is shown at the end of this paper in Figures 2-4.
Anatomy and Physiology
Wild animals arriving for rehabilitation could be from hundreds of species of birds, mammals and herptiles – and may have different anatomy and physiology. They may have wings, a cloaca, multiple stomach chambers, prehensile tails, talons, shells, and heads that are supposed to turn 180 degrees. They may chew cud, unhinge their jaws to consume prey, or eat cecotrophs. Their temperature and respiration rates may be considerably different. It is critical to know these differences in order to notice and assess problems, and provide effective care. For example, a shattered jaw in a raccoon may heal just fine, whereas the teeth of a squirrel with a fractured jaw are unlikely to align correctly and most often results in a non-releasable animal. A robin missing two toes may be releasable, whereas a red tailed hawk missing two talons on a single foot may not.
Natural History
The amount and accuracy of knowledge of the natural history of a species vary widely, but is often limited. The history of family units or individual animals tend to be even more limited. This requires the caregiver to have considerable knowledge of not only the species in general, but specific knowledge of what to expect with the individual. It is critical to know what is normal for the species, age, and time of year. For example, the caregiver must know when the animal is normally active and its typical behavior, including mating season, nesting, rearing young, migration, and hibernation. Caregivers need to know the types of problems that may occur, such as fawns or seals that might be kidnapped, ground squirrels that get into poison targeted for mice, gulls that swallow fish hooks, and porcupines with fractured limbs. They need to be aware of development stages and needs, such as when a fledgling would normally leave the nest, a duckling would be swimming, and a fox is weaned.
Stress Considerations
Wild animals are part of the natural food chain – predator and prey. Weakness or signs of weakness make them more susceptible to predation. Being chased, captured or handled by a predator is not only stressful, it can be fatal. Humans are generally predators, or considered predators – regardless of their potentially helpful intentions. This means that many wild animals will be very stressed by capture and handling, as well as restraint by or even proximity to humans. They will also hide or show symptoms differently – such as the ‘kidnapped’ rabbit that dies when picked up for an examination or the turkey vulture that regurgitates all food from the stress of being in captivity. To the person unfamiliar with a species, it may look “fine” – and then it dies unexpectedly since the symptoms were hidden. It is critical to reduce stress by minimizing handling and sounds, using such things as towels to cover the animal (especially eyes), and reducing proximity to anything that might be considered a predator (people, domestic animals, etc.).
The behavior of wild animals is considerably different from domesticated animals. They live and move freely in the wild and in all types of weather. They may migrate, hibernate, or estivate.
They make or take shelter, breed and raise their offspring – as they choose. They rely on their senses to find food, water and others of their species, and to avoid predators. Depending on the species, they may have stronger vision, hearing, or smell. They tend to be very alert and sensitive to their environment. Minimizing their exposure to sounds, sights and smells that are found in a veterinary clinic or other human setting helps reduce stress.
Diet and Nutritional Needs
Wild animals eat their choice of fresh, raw foods at the time they want. The amount of time a species is dependent on parents for food varies widely. The type of food eaten by the adults and young of a species may also vary. In the wild, young mammals first nurse from their mothers, young finches are fed insects, young mourning doves are fed a mixture of seed and crop liquid (not at all like mammal milk), and owls are fed mice. Each of these diets may change over time. The diets that these animals are fed in a rehabilitation setting are designed to meet their nutritional and caloric needs, and resemble their natural diet. The dietary and feeding needs (foods, amounts, feeding frequency, and methods) are very specific, and if not met can result in serious problems, even fatalities. Information from a knowledgeable rehabilitator can make a significant difference in the effectiveness of feeding wild animals, such as getting a baby bird to gape, the method to tube feed a young opossum, the formula for a hummingbird, or the correct amount to feed a rabbit.
Orphaned Wildlife
Healthy animals that are doing well in the wild are rarely admitted for rehabilitation, although there are a few unnecessary ‘kidnaps’ each year, especially of rabbits, fawns, sealsand fledgling birds. A majority of animals arriving for rehabilitation are juveniles. Some have lost a parent or something happened to the nest (fell down, destroyed), some were harmed by a pet or humans; others were just the victim of unfortunate circumstances (trapped in garage, caught in fence). Juveniles may have minor or major health problems, such as shock, dehydration, and an assortment of injuries, ranging from bruises, wounds, fractures, or head or neurological trauma.
Adult Wildlife
Adult wild animals presented for rehabilitation tend to have much more severe health problems or they would not have been captured. The large majority of adult wild animal cases are presented with acute conditions, since those with chronic conditions and weakness tend to quickly become part of the natural food chain.
Absence of Chemicals or Medications
An extremely small number of wild animals have ever been medicated or vaccinated. While a few states have distributed oral rabies vaccines for coyotes, foxes, and raccoons, this is still very rare. As a result, the systems of most wild animals are considered very “clean” from a homeopathic perspective.
Diseases and Parasites
Wild animals may also have some diseases and parasites that may not be common in domestic animals. Some of these are natural for the species and not considered a problem for the host. However, such parasites as baylisascaris may be a problem for other species of animals, including humans. In other cases, diseases may be transmittable, whether to others of the same species, other species, or even to humans. Thus, it is critical for anyone providing care for wildlife to be familiar with these conditions and take appropriate precautions. In some areas, local regulatory agencies place restrictions on the rehabilitation and release of certain species due to such issues.
Regulatory Considerations
Native wild animals arriving from the wild are not “owned”, although their possession is, for the most part, regulated by various government agencies (federal, state, and local). For example, federal permits are required to work with migratory birds, marine mammals, and threatened or endangered species. Ninety percent of the states require rehabilitation permits for mammals, birds and herptiles. Some local governments also have regulations affecting wildlife rehabilitation. While most state and federal agencies allow veterinarians to provide ‘good Samaritan’ services to wildlife, veterinarians without their own wildlife rehabilitation permits are usually expected to transfer wildlife to a permitted rehabilitator within 24 hours or to arrange for an exception.
Independent Survivability
Another key difference in working with wild animals is that they are to be released, preferably in a minimum amount of time and be able to survive independently in the wild. Not only could it be extremely stressful for many of these animals to be kept indefinitely in captivity, it could violate state and federal regulations. Wildlife needs to be released – which is very different from the domestic animal that is dependent on the care of humans. This also suggests that some treatments that might be considered for domestic animals not be performed on wildlife, such as the amputation of wings.
HOMEOPATHY WITH WILDLIFE IS DIFFERENT
In addition to differences between working with domesticated animals and wildlife, there are also differences in how homeopathy is used with wildlife versus domestics.
Case-taking
Taking a homeopathic case with a wild animal requires knowledge of what is normal for the species. This means understanding the natural history, typical problems, and how to recognize differences from normal health and behavior. For example, it is normal for nestling finches to gape, but not mourning doves. It is normal for neonate woodchucks to twitch gently in their sleep, but not to move convulsively when eating.
It is critical to know what is normal in order to effectively take the whole case, including physical, mental and emotional symptoms. Granted, it may be difficult to assess many symptoms, but it may be possible by working with a rehabilitator experienced and knowledgeable with that species. Rehabilitators knowledgeable about a species can provide information about whether behavior is normal territoriality or aggressive, active or restless, staying still to avoid notice or dull, or vocalizing normally. If a person does not have extensive knowledge of and experience with various ages of a species, it can be even more difficult to collect information about the whole creature.
Limited History
In most cases, there is also extremely limited history about the individual wild animal. History before the rescuer became involved is often unavailable. The rescuer, however, may provide information on where, when and how the animal was found. The rescuer may even describe the etiology or the reason for the rescue (e.g., dug up nest when gardening, found on the cement sidewalk, discovered in insulation in wall when remodeling, brought in by cat). In many cases, the rescuer just “finds” the animal and delivers it for help, without knowing or providing any background information (e.g., location found, care by rescuer). This lack of information makes it more difficult to provide care, but also can affect release location and the ability to meet regulatory requirements. It is not unusual for the history of the case to be built from knowledge of natural history, the rescuer, the location found, and the animal’s condition.
Display of Symptoms
While domestic animals do not verbalize their symptoms, their human companion or owner often notices and describes them. Wild animals tend to hide their symptoms or show them differently. Some people will be able to effectively notice and describe what is happening, others may not. Plus, the symptoms may be very different from what would be seen with humans or domestic animals. For example, a human infant or puppy may cry when hungry, whereas a young squirrel would not make a sound when hungry since that could attract predators.
There may be a variety of rubrics that may not be able to be used with wildlife, such as descriptions of pain, perceptions of temperature, some mental symptoms and “sensations as if”. It is possible, however, to draw inferences on some of the modalities based on knowledge of the species and observation. A cedar waxwing drinking considerable water (they get most of their needed moisture from the berries in their diet) or a gray fox leaning an injured shoulder against a cool wall of a cage are demonstrations of this.
Urgency
Another difference is the limited of amount of time available to take a case. The time available to collect information may be limited due to the potential for stressing the animal with too long or close an observation. It can also be difficult to collect information on the animal’s behavior due to the restrictions of captivity. That said, it is still critical to take the whole case and include as much of it as possible in the repertorizing and remedy selection. Again, a person who is very knowledgeable of the species may be able to help add insight, particularly about natural history, what is normal behavior, and so forth. For example, the person unfamiliar with porcupines may interpret their slow movement and poor vision to be related to head trauma, while they normally move slowly and have limited sight.
Repertorization
Since the largest and most detailed repertories reflect human conditions, finding some rubrics for other species can be challenging. For example, feathers, air sac, crop, and antlers are not listed as such in human repertories; nor are functions such as laying eggs or unhinging jaws; or behaviors such as flying, migrationor hibernation. It may be necessary to use related or combined rubrics in order to repertorize the case.
In some situations, it may be necessary to extrapolate and use etiology to develop the basic repertorization.For example, a bird that hits the window and ruptures air sacs may be repertorized as [GENERALITIES; INJURIES, blows, falls and bruises; general] since [RESPIRATION; DIFFICULT; injury, from] and [CHEST; INJURIES; lungs] do not have enough remedies to be very useful. Hopefully future repertories will be expanded to include rubrics such as flying (birds, bats), torpor (hummingbirds, jumping mice), cecotrophy (rabbits), cracked shells (turtles), throwing pellets (owls, grebes), and shedding skin (snakes) in order to be more useful for a wider range of species.
In many cases, the conditions presented are serious and time sensitive. There may be limited time to analyze the data and make a decision. For example, a scrub jay fledgling that collapsed after being accidentally drenched with a herbicide needs immediate action (washing off the herbicide) as well as giving a remedy. Nestling swallows found dehydrated, in shock, and overheated on hot cement need prompt action giving hydration fluids – as well as homeopathic remedies). It helps for the care-giver to be knowledgeable of general conditions (e.g., how to recognize shock, dehydration, fractures; common locations for wounds on a species; typical problems) and treatments before a crisis or condition arrives.
Selecting Homeopathic Medicines
While the process of remedy selection for wildlife is similar to domestics, the remedies selected generally emphasize the acuteness of the situation. The remedies are then reviewed in a complete materia medica, such as Materia Medica with Repertory (Boericke), Materia Medica of Homeopathic Medicines (Phatak), Lotus Materia Medica (Murphy), and The Concordant Materia Medica (Vermeulen),
Research into the most common conditions of wildlife admitted to rehabilitation shows a variety of conditions, as shown in Figures 2-4. Rehabilitators who have been repertorizing these conditions have identified a variety of homeopathic medicines that are commonly used. Homeopathic medicines frequently considered for acute wildlife trauma include Aconitum napellis, Arnica montana, Hypericum, Natrum sulphuricum, China, Arsenicum album, Phosphorus, Carbo vegetabilis, Veratrum album, Belladona, Ruta graveleons, Rhus toxicodendron, Symphytum, Ledum, Lachesis, Hepar sulphuris, Silicea terra, Gelsemium, Bryonia, Cantharis, Calendula, and Hamamelis.
What may be surprising for some is the frequency with which remedies not commonly considered for acute situations are used, such as Ignatia, Nux vomica, Lycopodium, Podophyllum, Cicuta virosa, Conium, Calcarea carbonica, Calcarea phosphorium, Sulphur, and Gunpowder.
Aconitum napellus is often the first remedy given to a wild animal due to its fear from being captured, handled and in the possession of humans. Aconitum napellus may also help those animals that are in shock from fear. Arnica may then follow a short while later if the animal has undergone some kind of blunt force trauma (e.g., falling from a nest, being stepped on) or in shock from injury. Arnica may also be given when traumatic circumstances, while unspecific, may have caused the problem (e.g., wild animal found by a side of a road or a found bird below a window), or an old trauma from which the animal has not fully recovered.
Ignatia is one of the more commonly used homeopathic medicines due to its effectiveness with grief and loss, and lack of appetite due to fear. This is frequently considered with young animals that have been separated from the mother or siblings (e.g., rabbits, raccoons), or flock (e.g., crows, ravens) or herd animals (e.g., deer), or those who mate for life (e.g., geese, eagles). Rehabilitators working with these species have said that Ignatia helps these animals stabilize faster, eat better and recover much faster.
Some of the homeopathic medicines used are not for the trauma, but for potentially serious problems resulting from ‘help’ by the well-intentioned rescuer. For example, improper feeding of a baby bird or mammal may result in aspiration – of which infants may die quickly if not treated aggressively (Phosphorus has been used effectively with sudden onset respiratory difficulties such as aspiration). Rescuers often feed an improper diet, resulting in severe diarrhea, bloat, or in some cases, if it has gone on long enough, nutritional deficiencies and delayed growth. In such cases, medicines such as Arsenicum album, Nux vomica, Podophyllum, Lycopodium, Calcarea carbonica, Silicea, or Calcaria phosphorium may work if they match the symptoms.
Potency Selection
As mentioned previously, if a wild animal arrives for rehabilitation it is most likely a result of an acute condition, since if it had been weak for a significant time it would have returned to the food chain. Adult wild animals are often admitted with very serious conditions (e.g., fractures, head trauma, toxins) since they would not have been captured by humans if there were only minor problems (scratches, minor bruises). The cause of these problems was generally a result of a significant insult (e.g., being hit by a car, major puncture wounds, electrocution). In many cases, the wild animals arrive with a very strong vital force (good, fresh diet, physically active (exercise) and absence of chronic conditions).
It is the author’s experience, as well as a growing number of homeopathic veterinarians and rehabilitators, that an animal with a high vital force that has sustained an acute condition from a serious insult often has needed a single dose of a higher potency homeopathic medicine, such as a 200c or 1m. If a 30c potency is used, the remedy may need to be repeated several times in a short time (3 to 24 hrs) to see the results otherwise obtained with a single dose of a 200c or 1m. Higher potencies, such as 200c or 1m, have been used effectively when there has been a strong emotional component, such as fear or grief. Effectively matching the potency to the animal’s need follows the concept of the minimum dose.
While lower potencies, such as 6x, 12x or 30x have been used by some rehabilitators, there have been concerns that the frequent repetition of the remedy increases stress due to regular handling. Additionally, they seem to have limited affect on acute, life-threatening conditions that need a strong healing message.
Repeating and Changing Homeopathic Medicines
As is consistent with classical homeopathy, the decision of when to repeat or change the homeopathic remedy is based on symptoms. Symptoms do, however, change far more quickly with acute traumas than with chronic conditions. As a result, the wildlife caregiver must stay very alert to symptoms, including the often subtle signs that show that a condition has changed. It may also be necessary to repeat or change a remedy more quickly if the symptoms change, like in minutes (e.g., breathing difficulty, severe bleeding), hours (e.g., convulsions, severe and deteriorating infection), or a couple of days (e.g., tendon damage). For example, a young woodchuck with bloat and soft yellow stool (after being fed the correct diet but too much of it by a caregiver) may be given Nux vomica 200c. However, if a few hours later, the animal has blasting, green liquid diarrhea, it may be appropriate to change the remedy at that time since the condition has worsened. Concurrent to using the homeopathic medicine in this case, the caregiver would place the animal on oral Lactated Ringer Solution and give some probiotics (such as Probiacin®). A fecal examination may also be performed.
One of the amazing things about using homeopathy with wildlife trauma is the potential speed of the response when the correct remedy is given. There have been numerous cases where the caregiver is astounded with the speed with which the wild animal responds to the homeopathic medicine. For example, a red-tail hawk that had been treated conventionally for a head trauma and unable to stand for two months and then promptly stood upright 10 minutes after getting a single dose of Arnica montana 200c. While a second dose of Arnica was required in this case, the animal recovered completely.
A Mountain bluebird in seizure after organo-phosphate poisoning stopped convulsing within several minutes of Cicuta virosa 30c. After two repetitions when symptoms returned (30 minutes interludes), the bird stabilized and recovered completely. A rehabilitator gave 4 nestling finches that hit the ground in a storm a single dose of Arnica 200c; within 1 hour they were covered with bruises; 3 hours after that the bruises were gone. As a result, it is critical to monitor results, exercise caution with handling and caging since the animal may recover faster than might be expected, and not expect to repeat the remedy unless the symptoms demonstrate the need.
Administration
Giving a homeopathic medicine in pellet or liquid form to a domestic animal that is accustomed to being handled is very different from wildlife. Since it can be difficult, and possibly dangerous, to put a pellet or liquid in a wild animal’s mouth, administration needs to be considered carefully. Rehabilitators have found that administering the number 10 size pellets (poppy seed size) works effectively with many species of wildlife, whether the animals are small or large.
In many cases, particularly with young or small animals, it is possible to dissolve the homeopathic medicine in water, pull that liquid into a small syringe (1 cc), and carefully put a drop in or on the mouth or beak. If the animal is difficult or risky to capture and handle, the dissolved homeopathic medicine may be sprinkled on food, placed in a pole syringe and placed in the animal’s mouth, or placed in water for the animal to drink (or walk or swim through). Or the dissolved homeopathic medicine may be lightly misted or sprayed toward the animal’s face, allowing the homeopathic mist to contact the mucus membranes of mouth, nose or eyes. If the animal is unconscious, it may be possible to put the pellets directly in the mouth. As always, it is essential to exercise caution in order to prevent injury to the caregiver.
Other Considerations
While homeopathy can address many of the conditions with which wildlife are admitted, other supportive care treatments are often necessary. An animal in shock from an injury can benefit from Arnica, but also needs to be placed in a quiet, secure, and warm place (with the exception of species that would find heat problematic). A severely dehydrated animal needs fluids as well as China. A wound may benefit from Hypericum or a variety of other remedies, but also need to be thoroughly cleaned, then possibly sutured and wrapped. Homeopathy is certainly used concurrently with some of these other treatments, and as such is highly complementary.
While homeopathy has certainly been shown to help in a variety of wildlife cases, it cannot help an animal recover from all medical problems, such as when the physical pathology may be too severe for the animal to recover (e.g., a crushed skull, a severed wing). Plus, for homeopathy to be effective with wildlife, it has to be used in conjunction with appropriate rehabilitation husbandry practices, such as diet, caging, reduced stress environment, appropriate socialization for the species, and so forth. If homeopathy is used without these other things, the wild animal may not recover and be released.
CASES
The following cases demonstrate some of the differences in using homeopathy with wildlife, including a summary of the repertorization as produced by MacRepertory©.
Fawn Hit by Car
A mule deer fawn (Odocoileus hemionus) was hit by a car traveling at a low rate of speed. The fawn was making high pitched noises that sounded like a combination of screams and cries when the rehabilitator arrived. It was breathing very rapidly, seemed extremely sensitive to noise, and had its eyes wide open. Knowing that fawns (a prey species) have died of fright, the rehabilitator immediately covered the fawn with a blanket.
Having previously repertorized these symptoms, the rehabilitator gave the fawn an Aconitum napellus 1m. 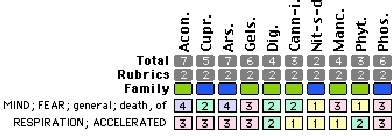 Within minutes, the fawn stopped screaming and was significantly calmer. The fawn was transported to a veterinarian who said that there were no apparent physical injuries and sent her to the rehabilitation facility for care. No problems occurred during her rehabilitation and release.
Within minutes, the fawn stopped screaming and was significantly calmer. The fawn was transported to a veterinarian who said that there were no apparent physical injuries and sent her to the rehabilitation facility for care. No problems occurred during her rehabilitation and release.
Squirrel with Urine Retention
A fox squirrel (Sciurus niger) was carrying her young offspring across a lawn when a dog lunged at them. The mother dropped the youngster and stood between it and the dog. The dog killed the mother squirrel before being pulled away by its owners. The juvenile squirrel, untouched by the dog, was put in a box and taken to a rehabilitator. While the rehabilitator found no obvious injuries, the young squirrel had rapid breathing, eyes wide open, and did not urinate when stimulated. The rehabilitator put the squirrel in a quiet, secure, and warm cage. A little while later, the rehabilitator gave her some Lactated Ringer Solution with a small syringe.
A few hours after that, the animal was given a dissolved squirrel milk replacer. The juvenile squirrel ate reluctantly, but that was normal for a wild animal just arriving in captivity. What was abnormal was that her bladder was distended but the squirrel still had barely urinated. Also, while wild animals in captivity may avoid human touch, this young squirrel seemed more frightened than normal when touched.
New to homeopathy, the rehabilitator contacted a homeopathic veterinarian who repertorized:
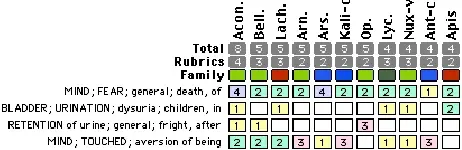

After reading the remedies in a materia medica, they selected and administered a single dose of Aconitum napellus 1m. The squirrel did not seem to be as afraid of touch and urinated normally when stimulated one hour later. No other problems occurred during her rehabilitation and she was released at the appropriate age.
Robin Hit the Window
While a woman was having lunch, a robin (Turdus migratorus) flew into the window in front of her and fell to the deck, 10 feet below. The woman placed the robin in a box and took the bird directly to a rehabilitation center. A quick examination by the veterinarian on duty found the bird in shock, to have a drop of blood on the beak that seemed related to head trauma.
The robin was placed in a quiet, warm cage and a drop of Arnica 1m that had been dissolved in water was placed in her beak. When the robin was checked 30 minutes later, she was standing and alert. Food and water was put in the cage. After another hour, she was found eating and trying to escape. She was placed in a flight cage and was flying normally. She was released the following morning back to where she had been found and to her waiting mate.
House Sparrow with a Slow to Empty Crop
A rescuer found a nestling house sparrow (Passer domesticus) on the ground and took it to a rehabilitator. Other than being slightly dehydrated, it had no obvious injuries and gaped normally. After being placed on heat and rehydrated, it was started on an appropriate diet. A little while later the rehabilitator noticed that the bird’s crop was slow to empty. The time between feedings was lengthened and amount of food decreased. The crop was sluggish and abdomen distended. The bird seemed to ‘get full’ quickly and was slightly constipated. Even with further changes in amount of food and feeding frequency, there was still no improvement.
A rehabilitator skilled in homeopathy was asked to help. She took the full case. While she was somewhat unsure to how to repertorize slow to empty crop, she repertorized:
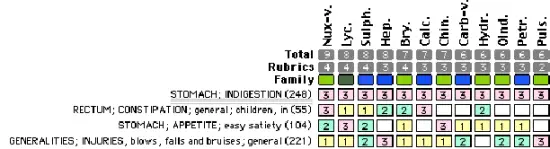
After reviewing the materia medica, she felt that Lycopodium was the closest match since it included symptoms of weak digestion, bloat, getting ‘full’ quickly, and constipation. Thirty minutes after she gave a Lycopodium 30c, the bird’s digestive system had returned to normal. The bird was placed back on the 20 to 30 minute feeding schedule. The bird developed normally, had no further problems, and was released in the normal time frame.
Red Squirrel with Head Trauma
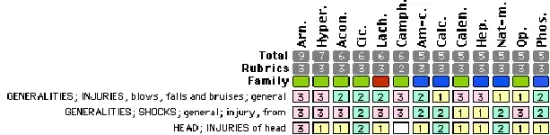
A homeowner found his twin toddlers playing with a juvenile red squirrel (Tamiasciurus hudsonicus) on his porch. He drove the terrified squirrel to a rehabilitator. Her veterinarian had previously approved her giving homeopathic remedies according to classical homeopathic protocols, and if she had questions to contact the veterinarian. She believed that the squirrel’s symptoms matched Aconitum napellus (e.g., eyes wide open, rapid breathing, adverse to touch, in a terrorizing situation with fear for his life). She gave him a drop of Aconitum napellus 1m dissolved in water. She placed him on heat in a quiet place. Thirty minutes later, he was much calmer so she conducted an assessment of his condition. He had a bump on his head, bloody nose, and general bruising on the body, but no other wounds. She repertorized (GENERALITIES; INJURIES, blows, falls and bruises; general; HEAD; INJURIES of head) and gave him a single dose of Arnica 1m. After hydrating him, she placed him on the appropriate diet. He developed with no apparent problems.
Three weeks later, however, the rehabilitator heard loud shrieks coming from his cage. She found him trying to attack the cage with jerky, rigid movements. His pupils were widely dilated and he seemed to have some vertigo. He seemed to be more frantic when she made any noise or turned on additional lights. She believed the problem was a result of the initial head trauma and not disease. She repertorized and then read the top remedies in the materia medica.
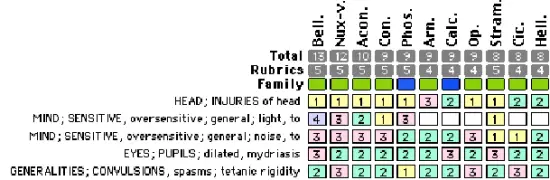
She felt Belladonna matched his symptoms but wanted to consult with her veterinarian. The veterinarian confirmed that it was likely head trauma and said that the risk of a disease such as rabies was extremely low in rodents. He agreed with the decision about Belladonna and said to let him know if the Belladonna did not immediately correct the situation.
She carefully gave the agitated animal a drop of dissolved Belladonna 1m from a syringe, covered the cage with a towel, turned out the lights and left the room. She checked him again in 30 minutes. He was sitting quietly on the floor of his cage and the light did not seem to bother him. His movements remained jerky and his pupils were still somewhat dilated. She decided to wait to monitor his movements. An hour later, his pupils and movements were normal, and he was not irritated by light or noise. She continued to monitor him, but the rest of his recovery was normal. He was released at the appropriate age and time for his species.
Owls Not Producing Pellets
A feedstore owner found three young barn owls (Tyto alba) when he was unloading a truckload of hay that had been in transport for several days. The owls were immediately delivered to a rehabilitator. Other than mild dehydration, the birds seemed fine. She put them on heat in a quiet area and hydrated them. After they were hydrated, they each ate three mice as if ravenous. Their voracious appetite continued but they did not produce or ‘throw’ any pellets, to get rid of the bones they had consumed. Six days later, they had still not thrown any pellets and she was very concerned. She was unsure how to repertorize producing pellets since humans do not ‘throw pellets’ after eating bones. She repertorized:
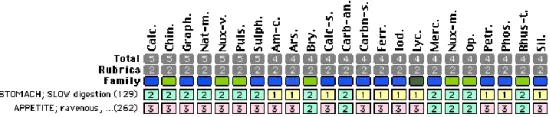
While she was uncertain about the match, she gave Lycopodium 30c since it covered the slow digestion and former dehydration (she would have preferred a higher potency but only had the 30c). She returned to feed them one hour later. They had each produced a huge, well-formed pellet. They continued to produce pellets and develop normally. They were released after fledging and hunting mice on their own.
Turtle with Hemorrhage
A snapping turtle (Chelydridae sepentina) was taken to a rehabilitator after being found by the side of a road. There were no signs of injury. A few days later, the turtle started hemorrhaging from his rectum. The rehabilitator took the turtle to a veterinarian who treated exotics. The veterinarian agreed that there were no external injuries and did not know if the turtle was bleeding due to injury or some other problem. Other than monitoring and keeping him on a good diet, the veterinarian was unable to offer other suggestions. He said he hoped the turtle would improve, but was not optimistic. In response to a question about trying homeopathy, the veterinarian said he was fine with trying it but could not offer suggestions about what to do.
The rehabilitator returned home and offered him food, but he did not seem to be as interested as he should have been. She then repertorized the case, believing it was likely that he had been hit by a vehicle.
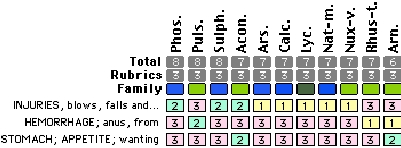
She read the remedies in the materia medica and selected Phosphorus since she felt it was the best match. She selected a 30c potency since that is a mid-range potency and she was uncertain about the potency for a rather slow-moving species. She administered the dissolved Phosphorus 30c to the turtle with a syringe. Within 24 hours, the turtle had stopped hemorrhaging (which is considered very rapid for a turtle). She kept the turtle for several months to make sure that there was no relapse. He was released back to the exact area where he was found.
Nestling Sparrow Injured by Cat
A day after being rescued from a cat, a nestling house sparrow (Passer domesticus) was delivered to a rehabilitator. Recognizing the bird’s extreme fear, the rehabilitator gave the bird Aconitum napellus 1m and placed her on heat in a quiet basket. She immediately offered the bird some food and found it not to be gaping as much as it should. Examination found several small lacerations and minor punctures which she cleaned thoroughly.
While infection was not yet visible, she was well aware that cat teeth and claws are a reservoir of bacteria. Such wounds could quickly become infected and the bird could die of septicemia. Her allopathic veterinarian said that wildlife injured by cats needed treatment to prevent the development of infection and had provided her with antibiotics in case she wanted to use them. The rehabilitator, however, preferred using homeopathic remedies because the unwanted affects of antibiotics (decrease of appetite, gastrointestinal upset, and chance of antibiotic resistance). She also felt that by time the antibiotics took eaffect, the young bird might die. After offering it more food, she repertorized the case.
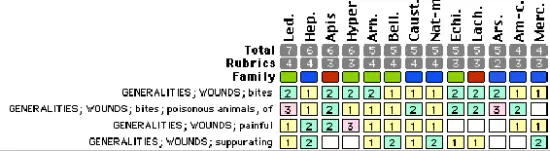
She read the remedies with the highest rating, as she had with many other cases of cat bites. The remedies listed most high had often not been effective with cat bites. She reviewed the description of Gunpowder offered by Clark in “Gunpowder as a War Remedy”.
“The great sphere of action of gunpowder is in cases of septic suppuration – or, in other words – of wounds that have become poisoned with the germs of putrefaction. … But Gunpowder my [may] also be used as a prophylactic.
That is to say, it will not only cure septic suppuration when present, but it will afford such protection to the organism against harmful germs, that wounds will be less likely to become septic in one who is under its influence….
Now the great point about Gunpowder is that it has a broad and clear indication that hardly anyone can miss – blood – poisoning. …
The poison quickly finds its way into the blood – boils, carbuncles, eruptions, abscesses, or other manifestations appear, showing unmistakably that the blood has been poisoned. To all these conditions Gunpowder acts as an antidote.”
She selected Gunpowder due to its effectiveness with exposure to severe infection, even if symptoms were not visible. The rehabilitator administered a single dose of homeopathic Gunpowder 200c dissolved in water. Within a couple of hours, the nestling was more alert and eating eagerly. No infection developed. The sparrow developed normally with no further problems. He was released at the normal time for his species.
CONCLUSION
People using homeopathy with wild animals have noted significant variations from working with domesticated animals. Case-taking can be quite different since there is less history, symptoms may be shown in very different ways if noticeable at all, and there may be little knowledge of what is ‘normal’ for the species and individual animal. Finding rubrics in the repertory that may be used to describe variations in anatomy, functions, behavior and diet can be challenging. The speed with which one needs to take the case, repertorize and select a remedy is also different with trauma cases where the animal may die if not treated promptly. Being able to select an appropriate potency to ‘jump start’ the desired response in species with very different energy levels (turtles versus hummingbirds), not cause an aggravation, and minimize handling is another challenge. Administration may be quite different, especially if the animal cannot be captured or handled easily. Then there are the challenges of monitoring the changes in the case without increasing stress and being able to identify the changes that would show the remedy was correct and healing is well underway, or that a remedy needs to be repeated or changed.
One of the most significant differences is how the wild animals respond to the remedy. It is not unusual for the response to the correct homeopathic medicine to occur within minutes. While this may not result in the animal’s immediate release back to the wild (it may need to be weaned, rebuild its strength, grow feathers, or develop waterproofing), it is rewarding to see the animal healthy again and on its way toward release back to the wild.
It is well appreciated that homeopathic veterinarians often have very busy practices with domestic animals. However, working with wildlife cases offers the chance to learn about some different species, treat different types of conditions, and experience some very rapid and complete recoveries. The time a homeopathic veterinarian works on wildlife cases may be limited as wildlife rehabilitators who are knowledgeable in the use of homeopathy for trauma care provide a written case and repertorization – and just contact the veterinarian on special consultations. It can be very rewarding for the homeopathic veterinarian to see rapid and complete recoveries – and have the opportunity to participate in the wild animal’s release back to its natural habitat. Rehabilitators are very grateful for the help of homeopathic veterinarians and homeopathy to help the wild animals that they rehabilitate.
The author expresses sincere appreciation to the many rehabilitators and veterinarians who work with wildlife and provided information for this paper, particularly Therese Bush (CA) and Nancy Kelly (CO).
© 2011. Shirley J. Casey. Originally published in the Academy of Veterinary Homeopathy for the Conference Proceedings, 2002. Republished with permission of the author. Similar articles are available at www.ewildagain.org.
REFERENCES
Blackmer, R.; A. Casey; and S. Casey. 1997. Beyond Conventional Allopathic Medicine: Options Considered by Wildlife Rehabilitators, Journal of Wildlife Rehabilitation, Winter: 7-13.
Blackmer, R.; J. Facinelli; A. Casey; and S. Casey. 1997. Exploring the Concept of the Minimum Dose: Wildlife Rehabilitators Consider Homeopathy, Journal of Wildlife Rehabilitation, Spring: 14-21.
Blackmer, R., A. Casey; S. Casey, J. Facinelli, B. Sparks. 1998. Homeopathy and Wildlife: First Aid and Trauma Care: Seminar Manual. Published by the authors, Evergreen, CO.
Blackmer, R.; A. Casey; and S. Casey. 1999. Considering Homeopathic First Aid for Wildlife. NWRA Quarterly Journal, Autumn: 14-16.
Boericke, W. 1927. Materia Medica with Repertory. Boericke and Tafel, CA.
Casey, A. 2000. A Survey of Conditions Seen in Wildlife Admitted to Rehabilitation. Wildlife Rehabilitation: Vol.18. NWRA, St. Cloud, MN: 143-160.
Casey, S. 2002. Homeopathic Gunpowder: Big Bang from a Small Remedy. .
Casey, S. 2007. Gunpowder! Little Known Remedy Packs a Wallop Against Wounds. .
Casey, S. 2006. When Wild Animals Refuse to Eat, It’s Not about Body Image. .
Casey, S. 2002. Success Using Homeopathy with Wildlife Trauma: Conference Proceedings 2002. American Holistic Veterinary Medical Association.
Casey, S. and A. Casey. 2000. Homeopathy and Wildlife Rehabilitation. Homeopathy Today. National Center for Homeopathy, Alexandria, VA: 24-25.
Casey, S. and A. Casey. 2001. Using Homeopathic First Aid with Wildlife in a Field Setting. Journal of the American Holistic Veterinary Medical Assoc., July, Vol. 20, No. 2, pp. 15-21.
Casey, S. and A. Casey. 2001. Homeopathic Success in Treating Poisoned Wildlife. Journal of the American Holistic Veterinary Medical Assoc., July, Vol. 20, No. 3., pp. 37-42.
Casey, S. and T. Bush. 2000. Homeopathic First Aid with a Sample of Wildlife Cases. Wildlife Rehabilitation: Vol.18. NWRA, St. Cloud, MN: 67-74.
Castro, M. 1990. The Complete Homeopathy Handbook. St. Martin’s Press, New York, NY.
Clarke, J. H. 1915. Gunpowder as a War Remedy. Jain Publishers, Delhi, India.
Chapman, J. and G. Feldhamer. 1992. Wild Mammals of North America. Johns Hopkins University Press, Baltimore, MD.
Engel, Cindy. 2002. Wild Health. Houghton Mifflin, New York, NY.
Facinelli, J.; A. Casey; and S. Casey. 1997. Finding and Using Holistic Veterinary Services. Journal of Wildlife Rehabilitation. Winter, pp. 14-19.
Kent, J. T. 1945. Repertory of the Homeopathic Materia Medica. Homeopathic Publications, India.
MacRepertory. Kent Homeopathic Associates.
Miller, E. 2000. Minimum Standards for Wildlife Rehabilitation, 3rd edition. National Wildlife Rehabilitators Association, St. Cloud, MN.
Murphy, R. 1995. Lotus Materia Medica. Lotus Star Academy, Pagosa Springs, CO.
Phatak, S. R. 1993. Materia Medica of Homeopathic Medicine. B. Jain Publishers, Kishan Kunj, Delhi.
Sibley, D. 2001. The Sibley Guide to Bird Life and Behavior. Chanticleer Press, New York, NY.
Sibley, D. 2000. The Sibley Guide to Birds. Chanticleer Press, New York, NY.
Vermeulen, F. 1997. Concordant Materia Medica. Emryss vy Publishers, Haarlem, Netherlands.
Van Zandvoort, Roger. 1994. The Complete Repertory. Institute for Research in Homeopathic Information and Symptomatology, Leidschendam, The Netherlands.
WildAgain Wildlife Rehabilitation. Seminars on the Use of Homeopathy with Wildlife. Information at www.Ewildagain.org.
TYPES OF CONDITIONS SEEN MOST FREQUENTLY IN WILDLIFE
A recent research study identified the most frequently seen conditions presenting in wildlife cases as observed by wildlife rehabilitators in 29 states. Forty-three respondents (a 20% response rate) were asked to indicate which of two hundred and four individual conditions listed on a survey they observed most frequently. Respondents were from a wide range of facilities, with 6 treating less than 100 animals per year, while 2 treated over 5,000 animals per year. These figures indicate the relative frequency of occurrence for all avian and all mammalian species, as well as for all wildlife species. Of special note, especially from a homeopathic perspective, is the high incidence of emotional states in wild mammals (Figure 3) as reported by the respondents.



_______________________________________________________
Wildlife rehabilitators provide temporary care to injured, orphaned, and distressed native wildlife so that those animals may survive when released back to the wild. Rehabilitators are required to have state, provincial, and often federal wildlife rehabilitation permits. The rehabilitators are trained, have special skills, use specialized diets and caging for the wildlife in rehabilitation, and work to minimize stress on these wild creatures. Rehabilitators seek to provide the highest quality of care by following professional standards, pursuing continuing education, and working closely with veterinarians. An increasing number of rehabilitators are pursuing holistic health care options for the wild animals that arrive with compromised health. For more information on wildlife rehabilitation, visit www.Ewildagain.org.
If you have found a wild animal that you believe needs help, contact a local wildlife rehabilitator for help in assessing if the animal really does need assistance and who would be available to provide effective help. If you do not know of a local rehabilitator, you can check for local rehabilitators on the internet or call animal rescue groups, veterinarians or conservation groups for a referral. Exercise caution since wild animals are just that: wild. Even small or young animals can cause serious injury or transmit diseases or parasites. Remember, wild animals need specialized care – and what actions might be appropriate for a pet may cause serious problems for a wild animal.
________________________________________________________________







Hi Shirley,
thank you so much for all your research and for sharing your experiences, much appreciated.
This is really the most interesting post I ever read about wildlife. Thanks for sharing such an informative post.