In April 2020 a mother of two consulted me about her daughter Sally, one and a half years old, diagnosed with congenital bilateral urinary (vesicouretral) reflux.
The problem came to light six weeks after her birth, when Sally got a urinary tract infection (UTI) that led to a kidney infection. She was subsequently put on a daily regimen of prophylactic antibiotics.
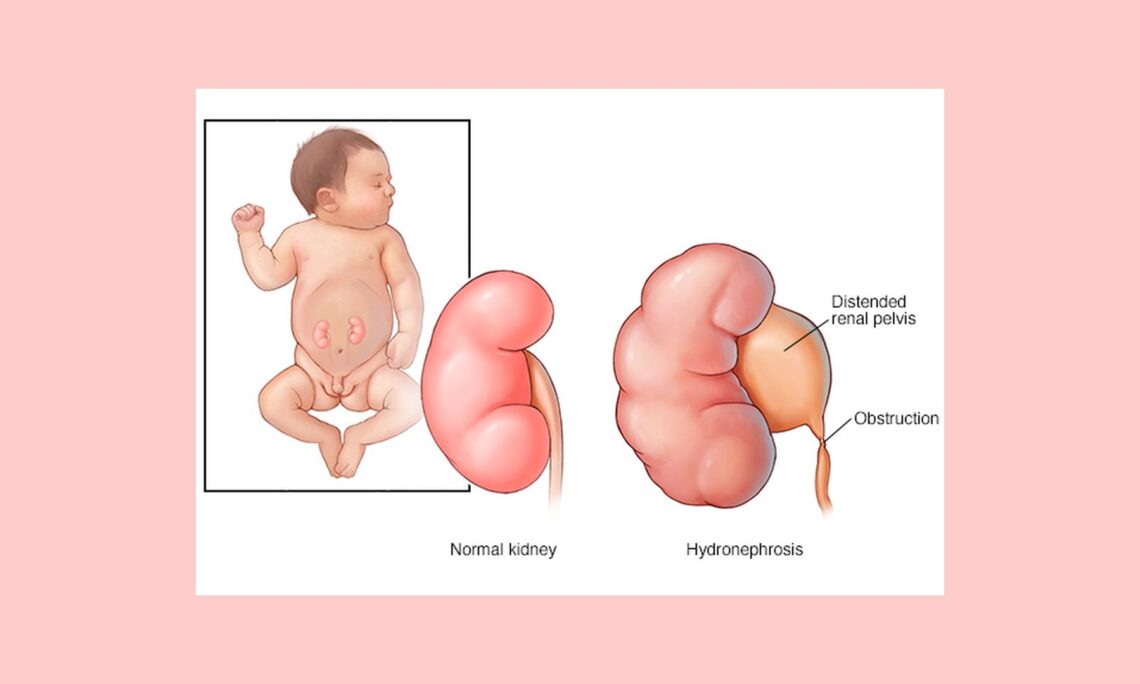
Children with primary vesicoureteral reflux are born with a defect in the valve that prevents urine from flowing backward from the bladder into the ureters. Kidney damage is the primary concern. The more severe the reflux, the more serious the complications are likely to be.
Sally has Grade V reflux (the most severe) on one side and Grade IV on the other. The nephrologist plans to correct the problem surgically when Sally reaches the age of five.
During the initial consultation I focus on Sally’s general physical and emotional traits for clues as to what remedy she needs, since there are no distinguishing features of the main pathology.
The little girl is sweet, bubbly, happy, always smiling and very independent. She loves her brother, who is two years older, and wants to do everything he does.
She loves taking a bath and splashing around.
She is warm blooded, never wants socks on, even outdoors. She throws the covers off during sleep. Her preferred sleep position is on her belly or left side. Sometimes she sleeps on her chest with her butt up in the air.
She loves activity, even if she is not feeling well. She talks a lot, especially for a child her age. She can get whiny and clingy at times. She is currently teething. She still nurses. She wants her hands clean but doesn’t like the process of having them cleaned. She is messy with her toys. She never asks for drinks. Her poops are very stinky, accompanied by a lot of gas.
Analysis
Almost any first year homeopathic student would prescribe Sulphur in this case. Sally’s buoyant, happy-go-lucky personality and stinky stools were highly characteristic, and Sulphur covered every other aspect.
Rx Sulph 30C once every two days, April 14, 2020. I also advised the mother not to give Sally any more vaccinations. (For explanation see my paper, Homeoprophylaxis, posted on my website.)
Follow-up June 25:
A new study of Sally’s urinary system was performed. On one side the reflux had disappeared, and on the other it was only Grade I. The nephrologist was extremely surprised; she couldn’t believe there was such an improvement. “I have never seen this,” she said, “and I don’t know why.”
Nevertheless, the doctor wished to continue with the daily antibiotic.
Email August 8:
Mother writes: “I see Sulphur is helping Sally; over the past two months there has been a huge improvement.”
Email Sept. 18:
“My 2 year old has had very foul smelling urine all day today. It started overnight, as I noticed it this morning, and she didn’t have it yesterday. This has happened in the past, and at least two of those times she developed a UTI after I first noticed the foul odor. Only this time she doesn’t have fever or vomiting, so I’m not sure what to do. I was reading some blog posts, and someone suggested I give her her constitutional remedy, which I assume is Sulphur. Should I do that? Or what can I give her to potentially stop the UTI from developing?”
I replied: “If your daughter is feeling fine and her only symptom is foul smelling urine I would suggest you wait. Sulphur covers foul smelling urine, so it may just be a discharge of toxins. If there are additional symptoms I would recommend that you call me.”
There was no further trouble.
Email Oct. 12
“We are travelling in Central America. Sally has diarrhea. She doesn’t want to eat that much, but she is very thirsty and drinking a bunch. Her brother threw up this morning. His stools look a little liquidy. My husband has diarrhea today and is nauseous.
I have my kits with me. What can I give them?”
Analysis
It appears the whole family got food poisoning except the mother.
Rx Arsenicum 30C prn
Email Oct. 13:
“Sally feels warm but has no fever so far.
Her brother is complaining very loudly of belly aches. My husband threw up last night. He is better this morning but still has very loose stools and no energy.
No one wants to eat anything. We have all been taking small sips of Gatorade.”
Email Oct. 14:
“Everyone slept just fine. Sally’s fever was gone by the evening last night. No one has a fever this morning, so that’s good. We were all feeling a bit better last night and were able to eat a tiny amount of chicken broth. Sally was just very low energy this morning. She reluctantly drank a little of an electrolyte drink and felt better.”
She fully recovered by the next day.
Email Feb. 5, 2021:
“My little one fell down the stairs, and I saw her tumbling down violently and couldn’t help her at all! She seems okay, but it was horrible. She says her head hurts and her legs. What can I give her? I’m afraid of a concussion.”
Rx Arnica prn
Later the same day the mother wrote back: “Thank you! She seems to be fine. She hit her head pretty hard.”
Email March 20:
“Sally caught a cold from her brother. She has watery, droopy eyes, a constant runny nose, and she freaks out every time boogies come out and just bursts into tears. It’s been all day of this! Super clingy and irritable.”
Rx Gelsemium 30c prn
Email March 21:
“Gelsemium worked great, actually! She woke up a couple times for a few seconds and went right back to sleep. A much better night than I expected. She has been great today too.
Thank you so very much for your help! Wish I could hug you and thank you in person! I’m so thankful for your help and for your patience with me.”
Email March 23:
“The Gelsemium is not holding. Sally still has a lingering cough. It sounds dry, but when she talks sometimes I can hear something in her chest.
She coughed a bunch before falling asleep and woke up a few times for a few seconds during the night, then woke up at 5 am and coughed for an hour and a half. Poor baby. It’s just a silly dry cough. Once she’s walking around, she’s good. It’s the lying down part that aggravates.”
I talked to the mother on the phone and found that Sally is more clingy and irritable than usual. She can breathe through her nose. She is not thirsty and does not ask for drinks. Based on these details I suggested two doses of Pulsatilla 30C three hours apart, and if no improvement then Drosera 30C.
Email March 24:
“The Drosera worked really well. No coughing going to sleep. In the middle of the night she had a coughing fit, so I gave Pulsatilla. The cough didn’t stop right away, but she didn’t cough the rest of the night. She has coughed a few times this morning, but very sporadic.”
Plan: continue with Drosera
Email in the evening:
“So far Sally’s cough is gone. No cough at bedtime either. I’m praying she has a smooth cough-free night.”
She did.
On May 27 Sally had another upper respiratory tract infection with a runny nose and dry cough. She got a number of remedies, some prescribed by the mother and some by me, including Aconite, Gelsemium, Nux vomica, Phosphorus and Pulsatilla. The last helped the most, and by May 31 she was reportedly much better.
On June 27 she developed a minor fever with no other symptoms.
Rx Puls 200 tid
The fever disappeared after three doses.
On July 1 Sally developed a dry cough again, which kept her from sleeping. The mother tried Pulsatilla again, but it had no effect.
The cough became less dry and more phlegmy. I prescribed Kali bichromicum, which ended the trouble.
Email Aug. 3:
Another study was performed by the nephrologist. The mother wrote:
“NO REFLUX!!! They were stunned! They want to double check with a different doctor just to make sure and want me to keep doing the prophylaxis antibiotic until then. They’ll confirm after that conversation but didn’t say when that’ll be.
They still want to monitor her with ultrasounds going forward.
We are praising God for this and absolutely 100 percent thankful for you, Dr Finne. In His Sovereignty He has used you to help our family. So thank you!”
The mother decided to stop Sally’s antibiotics even without the go-ahead from the nephrologist. She also stopped the protocol of Sulphur every two days.
Sally continues to thrive.
Discussion
It could be argued that Sulphur was not Sally’s true simillimum, as she required a variety of other remedies for various acute problems. Such an argument is a bit theoretical, as Sulphur was the best remedy I could find and accomplished a healing miracle. The case did not suffer any setbacks from the use of the acute remedies.
In fact, I was quite surprized that Sally did not suffer any apparent side effects of the daily antibiotic she took. I could find no evidence of candida overgrowth, for example, which is often encountered.
In my experience (and that of many others) almost all young children go through a period of frequent infections, usually of the upper respiratory tract. If these episodes are treated homeopathically the child naturally develops a robust immune system that is resistant to all diseases, even those to which the child has never been previously exposed.
Hopefully this case will be an inspiration to all parents of children with urinary reflux.


Beautiful case!
I love that you allowed yourself to stay simple with it. Good old Sulphur.
Thanks for sharing Diderik.
Hi, I am interested in helping my newborn daughter with kidney inflammation/ possibly kidney reflux. We aren’t sure yet what has caused our daughters left kidney to be mildly enlarged but I want to help her heal naturally. Please email me or let me know how I can contact you. Thank you!
Hi, I am interested in helping my newborn daughter with kidney inflammation/ possibly kidney reflux. We aren’t sure yet what has caused our daughters left kidney to be mildly enlarged but I want to help her heal naturally. Please email me or let me know how I can contact you. Thank you so much!