FROM THE HISTORY1
Goiter was first described in China in 2700 BC. Da Vinci described thyroid as a thing that is designed to fill empty spaces in the neck. According to Parry – thyroid works as a buffer to protect the brain from surges in blood flow. Roman physicians have reported thyroid enlargement as a sign of puberty. In 500 AD Abdul Kasan Kelebis Abis performed the first goiter excision in Baghdad, the procedure remained unknown. In 1200s AD advancements in goiter procedures included applying hot irons through the skin and slowly withdrawing them at right angles. The remaining mass or pedicled tissue was excised. Patients were tied to the table and held down to prevent unwanted movement, but most died from haemorrhage or sepsis. In 1646 AD Wilhelm Fabricus performed a thyroidectomy with standard surgical scalpels, for which he was imprisoned. In 1656 thyroid (Homeopathy for Thyroid Problems) was first identified by the anatomist Thomas Wharton. In 1808 AD Guillaume Dupuytren performed a total thyroidectomy, but the patient died postoperatively of “shock”. In 1820 AD Johann Straub and Francois Coindet found that use of seaweed (iodine) reduced goiter size and vascularity. In 1830 AD Graves and von Basedow describe a toxic goiter condition they referred to as “Merseburg Triad” – goiter, exopthalmos, and palpitations. In 1866, Samuel David Gross said, “If a surgeon should be so foolhardy as to undertake it [thyroidectomy] … every step of the way will be environed with difficulty, every stroke of his knife will be followed by a torrent of blood, and lucky will it be for him if his victim lives long enough to enable him to finish his horrid butchery.” In 1883, Theodor Kocher while addressing the German Medical Congress stated, “The thyroid gland in fact had a function”. In the same year Kocher’s performed a retrospective review on 5000 career thyroidectomies. The thyroxine was discovered somewhere in 19th century and a remarkable turning point started with this in management of thyroid disorders by allopathic counterparts.
REFERENCES FROM THE LITERATURE2
The homoeopathic literature is loaded with vast examples of thyroid diseases and their cure with homoeopathy. It was the insight of our great masters that they have so beautifully described thyroid related disorders and their management in Homoeopathy. In his great work, Master Samuel Hahnemann has quoted, “What action is exerted on the skin by certain diseases of the glands with an internal secretion (thyroid gland, ovaries, testicles, supra-renal capsules, pituitary gland, etc.) must remain reserved for future research. So much, however, is established to-day to prove that some of these disturbances (Addison’s disease) cause considerable alterations of the skin.” Below are some of the references from the history regarding thyroid disorders and their Homoeopathic cure.
CASE STUDIES PRESENTED SO FAR2
- Journal of Homoeopathic Clinics, Vol 3, Sep N’1, Case 458, 1869-1870: A 19 years old female with large swelling of the thyroid gland was treated with Bromine 3, several times a day following by Calc Carb 3 and was relieved in three weeks of time.
- International Hanhnemannian Association 1902: A case of thyrotoxicosis was treated by Homoeopathically chosen remedies: China, Lachesis, Sul.
- Clinical Illustrations Homoeopathician (A Journal Of Pure Homoeopathy) 1914: presented 3 cases of thyroid enlargement with thyroid dysfunction and were reported cured by Iodum and Baryta carb.
- International Hahnemannian Association 1919: “Our knowledge of the endocrine remedies is as yet in a formative stage, but the therapeutic use of the ductless glands is steadily growing. We know more of the thyroid gland and of its therapeutic applications, than of any of the other ductless glands.” There is also a case presented which was treated using 2x and 3x trituration of thyroidinum.
- International Foundation for Homoeopathy: Case Conference Proceedings 1995: A case of primary hypothyroidism aged 30 female was presented by Dr. George Guess.
- Master F. J. , 1995: A case of a lady aged 51 years with migraine of 15 years standing, hypothyroidism since 10 years and leucoderma since 5 years and a diagnosed as a case of Hypothyroidism was given Staphisgaria.
REFERENECES FROM MATERIA MEDICA2
- Blackwood A. L. Manual of materia medica therapeutics: “A normal thyroid has much to do with the function of the ovaries; with a hypothyroid condition, although the ovaries and uterus are normal, menstruation may not appear and the patient becomes obese, the skin dry; should the pituitary show disturbance, the skin will be moist and soft”.
- American Homoeopath described the concept of Hypothyroidism, cancer and clinical depression.
- Boericke W. Pocket manual of homoeopathic materia medica: Kali Carb: “Pain in small spot on left side Hypothyroidism”. Thryroidinum: “Marked sensitiveness to cold, Hypothyroidism after acute diseases, i.e. weakness.
- Grand George D. The spirit of homoeopathic medicines: “At times the remedy is suggested by hypertrophied glands or the beginning of goiter. Homeopathic treatment will remedy a slight disorder in the glandular system, but when the disorder is too great, hormonal treatment will be necessary.
- Lesser O. Textbook of Homoeopathic Materia Medica: “If the alkali and earthy alkali metals, Na, K, Mg, Ca, as cations determine the drug picture, then they shape it as hydrogenoid, cold, sensitive to cold, relaxed torpid lymphatic constitutional types stigmatized along the side of the parasympathetic system. Seen from an endocrine side, they tend toward the hypothyroid side, the function of the lymphocytic apparatus (thymus) is increased.”
- Master F. J. The bed side Organon of Medicine: “Never give thyroidinum as a routine or specific for all patients who come with thyroid problem.”
REFERENCES FROM REPERTORY3
There are 32 references in the forms of rubrics and subrubrics given in Synthesis treaure edition. Whereas Kent’s repertory, Murphy repertory and Complete repertory consists of 9, 13 and 37 rubrics in relation to thyroid and other rubrics and vice versa respectively.
THYROID GLAND
DEVELOPMENTAL CONSIDERATIONS4
The thyroid gland starts developing by 3-4 weeks of gestation, appearing as an epithelial proliferation in the floor of the pharynx. Follicles of the thyroid begin to make colloid in the by 12th week of gestation and thus contribute in development of physical and neurological features. Failure of synthesis of hormones and TSH by thyroid gland may result in arrested or abnormal growth of the fetus. At birth, a cold-stimulated short-lived TSH surge is observed, followed by a TSH decrease until day 3 or 4 of life by T4 feedback inhibition.
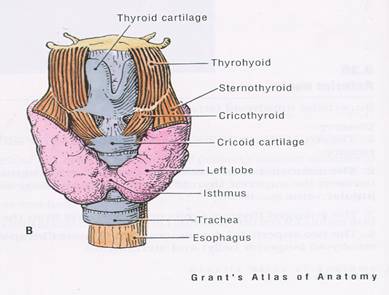
ANATOMY OF THYROID GLAND5
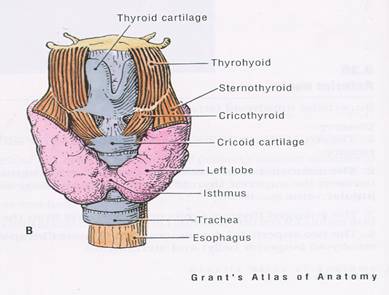
FUNCTIONS OF THYROID GLAND6
The thyroid gland is one of the most important endocrine gland which secrets two major hormones, thyroxine and triiodothyronine. It is situated in the anterior part of the neck just above the lower part of the trachea, situated in between the cricoid cartilage and suprasternal notch. Normally it is not palpable but may be palpated in conditions in which it is enlarged. Enlargement of the gland may not be a sign of its under or over functioning, but association of goiter with thyroid function status and other investigative modalities helps us to understand disease in a better term. Goiter is assessed by palpation by fingers of both hands for size, consistency and presence of nodules if any.
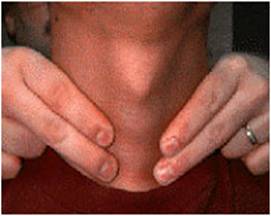
Thyroid palpation method
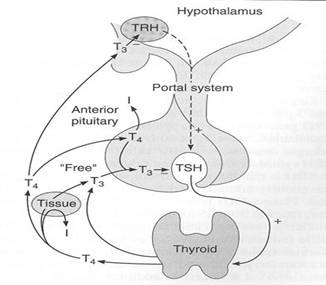
Thyroxine (T4) and tri-iodothyronine (T3) are two major hormones that are secreted in pulsatile manner under feedback mechanism controlled by hypothalamic-pituitary-thyroid-pituitary axis.
DIAGNOSING VARIOUS THYROID DISORDERS
The diagnosis of thyroid disorder is primarily done on following points:
- Complete homoeopathic case taking.
- Family history of systemic disorders particularly thyroid and autoimmune disorders. It is seen that the individuals who have family history positive of thyroid dysfunction are at greater risk of developing thyroid disorders.
- Consistancy and size of thyroid gland, as it may give us some hint about the underlying pathology, e.g. firm gland are suggestive of Hashimoto’s thyroiditis, goiter in high grades can induce pressure symptoms on trachea and other adjacent tissues, painful gland suggests acute or subacute inflammatory condition.
- Presence of anti thyroid antibodies, may suggest some of the thyroid dysfunction.
- Other investigations also help in arriving at diagnosis of thyroid disorders. Some of the investigations are: Radioactive iodine uptake (RAIU), Technetium scan (Tc Scan), Fine needle biopsy (FNB). These investigations are condition specific and are to be advised as per requirement of the case. The detailed description of these investigative modalities is described later in the following text.
The ultimate and ground level workers in thyroid-body axis are the two hormones secreted by thyroid gland. These hormones are responsible for various activities in almost the entire body. Every organ and tissue thus needs these hormones (particulary T3) for proper functioning. Thyroid hormones acts by crossing the cell membrane and binding to intracellular receptors (?1, ?2, ?1 and ?2), which act alone, in pairs or together with the retinoid X-receptor as transcription factors to modulate DNA transcription and thus various metabolic and other functions are performed. There are two variants of thyroid hormones circulating in body; free and bounded hormones, as hormones are circulated along the body in protein-bound form. These proteins are majorly thyroid binding globulins (TBG) and less commonly albumin. According to extensive research studies done on this reveals that free hormone assay is more reliable as bound hormones level may vary in conditions in which there is pooling of TBG in body eg.,
- Pregnancy
- Estrogen therapy
- Oral contraceptive pills
- Acute viral hepatitis
- Primary biliary cirrhosis
- Hepatocellular cancer
- Collagen vascular disease
On the other hand TBG in decreased in
- Glucocorticoids
- Androgens
- Nephrotic syndrome
- Protein-losing enteropathy
- Cirrhosis
- Critical illness/starvation
T4 (thyroxine) is the major circulating hormone whereas T3 is more biologically active. Both T3 and T4 give a feedback to pituitary to release or suppress secretion of TSH. TSH is ultrasensitive to even smaller amouts of circulating T3 and T4 levels, this phenomenon is to be understood at the ground level to understand the diagnosing and follow up cases of thyroid disorders. This can be understood by the following simple yet informative flow chart:
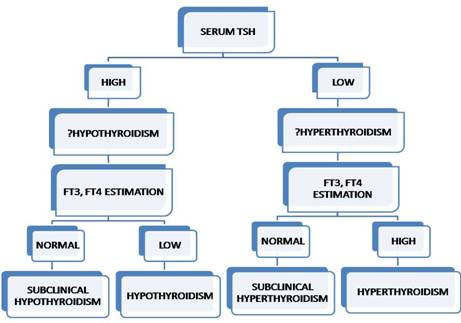
TSH is one of the most reliable marker of thyroid disorders along with FT4 estimation. Other diagnostic modalities used to diagnose various thyroid dysfunctions are given below with their advantages and description:
| MARKER/INVESTIGATION | BRIEF UTILITY |
| TSH | Most reliable marker to assess thyroid dysfunction with FT4 as TSH is the precursor of release of FT3 & FT4 |
| Free T3, T4 | Circulating un-bound hormone assays depicts the actual level of thyroid hormones thus prognosis can further be made along with the clinical and confirmed diagnosis. |
| Antibodies: Anti-TPO, Anti-TSHr | Presence of antibodies may sometime help us to understand the natural history of thyroid functions, as their presence confirms the undergoing pathological conditions. |
| Thyroid ultrasonography | Thyroid Ultrasonography is done to see the consistency of thyroid gland. It is also done to rule out the presence of nodules. Ultrasonography can also be suggestive of congenital anomalies e.g. absence of one or both lobes of thyroid gland. |
| RAIU | Scintillation counter measures radioactivity after I123 administration. Uptake varies greatly by iodine status, e.g. indigenous diet (normal uptake 10%).
Elevated RAIU with hyperthyroid symptoms may be presented in:
Low RAIU with hyperthyroid symptoms is used to distinguish:
(Jod-Basedow effect)
The RAIU technique is also used as a therapy to suppress the hyperactive gland in thyrotoxicosis and hyperthyroidism. |
| Technetium scan (Tc Scan) | Technetium scan is also based on the uptake phenomenon of Tc by thyroid gland that is then use to differentiate various nodules and hyper functioning and hyperactive thyroid gland. |
| Final Needle Biopsy (FNB) | FNB is used to study the morphological and pathophysiology of glandular tissue. By this technique we can differentiate various types of carcinomas, dysplasia, and chronic lymphatic infiltration. |
SUMMARY
- TSH is a good screening test to assess thyroid function in an outpatient setting.
- If TSH is abnormal, the diagnosis is confirmed with thyroid hormone levels.
- Change in thyroid binding proteins could alter total thyroid hormone levels.
- 99% of thyroid hormones are protein bound.
- In order to assess the thyroid hormone levels unaffected by the binding proteins, free thyroid hormone levels assessment is more reliable.
- T4 is the major thyroid hormone in circulation; therefore assessing T4 status alone is usually sufficient to assess the thyroid hormone status.
- In certain situations, T3 level becomes abnormal without changes in T4, as in T3 thyrotoxicosis where there are elevated levels of T3 along with normal T4 levels and low TSH level.
- Acute illnesses can alter thyroid function tests without thyroid disease as they tend to increase binding proteins, also TSH can also be influenced by stress and anxiety.
- Thyroglobulin is a good cancer marker for papillary and follicular cancer after total thyroidectomy.
- Thyroid antibodies can assess the risk of developing autoimmune thyroid diseases.
SPECTRUM OF THYROID DISORDERS7
GOITER
Chronic enlargement of the thyroid gland not due to neoplasm is called as goiter.
- Endemic goiter-Areas where > 5% of children of 6-12 years of age have goiter, very common in China and central Africa.
- Sporadic goiter –Areas where < 5% of children 6-12 years of age have goiter. Multinodular goiter in sporadic areas often denotes the presence of multiple nodules rather than gross gland enlargement.
- Familial
Etiology:
- Hashimoto’s thyroiditis
- Early stages only, late stages show atrophic changes
- May present with hypo, hyper or euthyroid states
- Graves’ disease – Due to chronic stimulation of TSH receptor
- Diet – Brassica (cabbage, turnips, cauliflower, broccoli), Cassava, Lithium prevents release of hormone, causes goiter in 6% of chronic users
- Neoplasm
- Chronic Iodine excess – Iodine excess leads to increased colloid formation and can prevent hormone release. If a patient does not develop iodine leak, excess iodine can lead to goiter.
THYROID NODULES
- Prevalence
– Palpable: 4-7%
– Non-Palpable: >50%
– Cancer in nodules: 5%
- Women affected more than men
- Most subjects are euthyroid and/or asymptomatic
- Prevalence is less than 1% with thyrotoxicosis
- Historical Red Flags are defined as:
– Male
– Extremes of age (<20 or >65)
– Rapid Growth
– Symptoms of local invasion (hoarseness, dysphagia, neck pain)
– History of radiation to the head or neck dispose an individual to develop nodules
– Family history of Thyroid Cancer or Polyposis
SOLITARY THYROID NODULE
- More likely to be malignant in men, patients over 60 and patients with a h/o head or neck irradiation are at more risk.
- No growth for years almost always indicative of benign nodule as it is not a nodule that appears suddenly (likely a cyst or adenoma hemorrhage)
- Malignant nodule develops in weeks to months.
- Virtually all patients with thyroid carcinoma are euthyroid as are those with benign nodules. Nodule of >1.5 cms., are usually detectable on examination and are confirmed in the Ultrasonography. Lifetime risk for developing a nodule is 5-10%. Studies show 50% of people during autopsy have either single or multiple nodules. 5-10% of clinically detectable hypofunctioning (cold) nodules can be malignant. The laboratory/imaging techniques used are: TSH, Calcitonin, Ultrasound, FNB for characterization of Nodules, Nuclear Scan to see whether nodule is “Hot” or “Cold.” If FNB is suggestive of malignancy then surgery is advised, and if it is suspicious or negative then a follow up of few months is given to the patient with repeat investigations. In case there are indeterminant reports then FNB is repeated, if still indeterminant, surgery is recommended.
PRIMARY HYPOTHYROIDISM
Definition – disorder of the thyroid gland causing decreased thyroid hormone production and secretion. It is the most common disorder of thyroid dysfunction. The factors attributed to these are:
- Worldwide – iodine deficiency is most common cause.
- Iodine depleted areas – chronic autoimmune thyroiditis is commonly present in these areas.
- Associated with elevated serum cholesterol, CPK, AST and LDH
SECONDARY HYPOTHYROIDISM
Definition – It is caused by decreased thyroidal stimulation by TSH.
- Also referred to as central or hypothyrotropic hypothyroidism.
- Caused by either pituitary or hypothalamic diseases.
- Very uncommon.
- TSH is usually low or inappropriately normal.
Symptoms of hypothyroidism
It includes – Fatigue, lethargy, mental impairment, depression, cold intolerance, hoarseness, dry skin, decreased perspiration, weight gain, decreased appetite, constipation, menstrual irregularities, arthralgias and parasthesias.
Signs
Slow movements, slow speech, hoarseness, bradycardia, dry skin, non-pitting edema, hyporeflexia, delayed relaxation of reflexes are some of the signs of hypothyroidism.
N. B.: Older patients tend to have fewer signs and symptoms of hypothyroidism and those they have tend to be less specific.
Diagnosis
- Low FT4, High TSH (Primary, antibodies estimation suggested)
- Low FT4, Low TSH (Secondary or Tertiary, TRH stimulation test, MRI)
HASHIMOTO’S THYROIDITIS
- It is the most common cause of hypothyroidism.
- It is due to action of auto- antibodies to TPO, TBG thus by inhibiting/diminishing the production and secretion of thyroid hormones.
- Commonly presents in subjects from 30-50 yrs, female affected more than males.
- It is usually non-tender and asymptomatic.
- Lab values
- High TSH
- Low T4
- Anti-TPO Ab, Anti-TBG Ab
SILENT THYROIDITIS (POST-PARTUM THYROIDITIS)
Silent thyroiditis is termed post-partum thyroiditis if it occurs within one year of delivery. Patient comes with hyperthyroid symptoms. Soon there is progression to euthyroidism followed by hypothyroidism for up to 1 year. Later on hypothyroidism generally resolves.
SUBACUTE THYROIDITIS (DEQUERVAIN’S, GRANULOMATOUS)
It is the most common cause of painful thyroiditis. It often follows a URI. FNA may reveal multinuleated giant cells or granulomatous change.
Course
– It starts with pain and thyrotoxicosis (3-6 weeks) followed by asymptomatic euthyroidism.
– Then there is period of hypothyroid state(weeks to months).
– It is followed by phase of recovery (complete in 95% after 4-6 months).
Diagnosis
– Elevated ESR
– Anemia (normochromic, normocytic)
– Low TSH, Elevated T4 > T3, Low anti-TPO/Tgb
– Low RAI uptake (same as silent thyroiditis)
– Graves’ disease may occasionally develop as a late sequellae
ACUTE THYROIDITIS
Causes:
– 68% Bacterial (S. aureus, S. pyogenes)
– 15% Fungal
– 9% Mycobacterial
It may occur secondary to Pyriform sinus fistulae, Pharyngeal space infections, Persistent Thyroglossal remnants, Thyroid surgery wound infections (rare) and in HIV.
Diagnosis:
– Warm, tender, enlarged thyroid
– FNA to drain abscess, obtain culture
– RAIU normal (versus decreased in DeQuervain’s)
– CT or US if infected TGDC suspected
Recovery is usually complete.
RIEDEL’S THYROIDITIS
It is a rare disease involving fibrosis of the thyroid gland.
Diagnosis:
– Thyroid antibodies are present in 2/3
– Painless goiter “woody”
– Open biopsy often needed to diagnose
– Associated with focal sclerosis syndromes (retroperitoneal, mediastinal, retroorbital, and sclerosing cholangitis)
THYROTOXICOSIS
Definition – refers to clinical syndrome of hyper metabolism resulting from increased serum concentration of T4 and/or T3, regardless of cause. Not synonymous with hyperthyroidism. Hyperthyroidism – increased thyroid hormone biosynthesis and secretion by the thyroid gland.
Symptoms – nervousness, fatigue, weakness, increased perspiration, heat intolerance, tremor, hyperactivity, palpitation, change in appetite, weight change, menstrual irregularities.
Signs – hyperactivity, tachycardia, atrial arrhythmia, systolic hypertension, stare, eyelid retraction, tremor, hyperreflexia, muscle weakness.
*Older patients – have fewer signs and symptoms of sympathetic activation and more cardiovascular dysfunction.
GRAVES’ DISEASE
It is the most common cause of thyrotoxicosis in the industrialized world. It is an autoimmune condition with anti-TSHr antibodies. Onset of disease may be related to severe stress which alters the immune response.
Diagnosis:
– TSH, T4, T3 to establish toxicosis
– RAIU scan to differentiate toxic conditions
– Anti-TPO, Anti-TSAb, FT3 if indicated
| RAIU in Hyperthyroid States | |
| High Uptake | Low Uptake |
| Graves’ | Sub acute Thyroiditis |
| Toxic MNG | Iodine Toxicosis |
| Toxic Adenoma | Thyrotoxicosis factitia |
HOMOEOPATHIC MANAGEMENT
There are various types of thyroid disorders which we commonly encounter in our day to day practice. These disorders are attributed at different levels, viz:-
- Dynamic- Euthyroid autoimmune thyroiditis.
- Functional- initial stages of autoimmune/Hashimoto thyroiditis, Subclinical hypothyroidism and Subclinical hyperthyroidism.
- Patho-physiological- Goitre, Hashitoxicosis, Chronic lymphocytic infiltration of thyroid, Non-malignant Nodules.
- Pathological- Hypothyroidism, Graves’ disease, Thyrotoxicosis.
- Destructive- Malignancies, toxic nodules.
The understanding of these levels helps us to define the prognostic and management plan for the individual. Also it helps us to define the therapeutic guidelines to treat a case of thyroid dysfunction. If we clearly perceive this concept we can avoid claiming false cures, as we cannot go against nature’s law of cure. If destruction has started we can only stop its progression, but cannot revive new cells. Once destruction has set in and the functional units of gland are non functional, no medicine can revive it or grow it, but on the other hand medicine will save rest of the cells. This is the reason why we encounter many patients in our practise who do not respond to well-selected homoeopathic remedies according to Homoeopathic principles. This occurs in cases where there is either disease that has progressed to non revertible changes or there is/are some other obstacles to cure. These obstacles to cure can be:
- Other systemic disorders e.g. Diabetes mellitus, Hypertension, Metabolic syndrome, dyslipidemia etc
- Autoimmune disorders e.g. SLE, vitiligo
- Any history of previous thyroid disorders e.g. Hashimoto thyroiditis, thyroid nodules, autoimmune thyroiditis, etc.
- Other endocrinal disorders e.g. PCOS, prolactinoma, Cushing syndrome, etc.
Association of thyroid dysfunction with these disorders make the condition what we read in Organon as “Complex diseases”. The treament plan of these cases is done according the laws embedded in Organon of Medicine8.
In aphorism 3 of Organon of Medicine8 fifth edition, Hahnemann states that, “If the physician clearly perceives what is to be cured in diseases, that is to say, in every individual case of disease (knowledge of disease, indication),……” the first homework to be done by a physician is to understand the disease and its component, then only can he see the finer shades of individualization, difference between common and uncommon symptoms, understanding an individual as a whole and not a diseased part or organ, diagnosis and prognosis of this state, etc. The natural history of any disease helps us to manage a disease and to intervene in it with judicial employment of medicines. For example, cases in which irreversible pathological changes have occurred, remedies having specific actions in low to moderate doses are usually advised. In cases where there are dynamic or functional abnormalities, remedies with moderate to high potency are advised.
LEVELS OF PREVENTION OF THYROID DISORDERS:
PRIMORDIAL PREVENTION
Health promotion:
Educate the family regarding lifestyle measures, good food habits, positive attitude to be inculcated in young child
Specific protection:
- Regular exercise
- Desirable BMI
- Health promotive measures and attitude
- Identifications and elimination of exciting or precipitating factors, if any.
PRIMARY PREVENTION
- Early diagnosis and treatment.
- Reinforce primary and preventive measures.
- Identifications and elimination of exciting or precipitating factors, if any.
SECONDARY PREVENTION
Aggressive reinforcement of:
- Primary and secondary risk intervention.
- Secondary prevention: lipid profile within normal limits
- Aggressive and effective control of disease.
TERTIARY PREVENTION
- Disability limitation
- Rehabilitation
TREATMENT GUIDELINES FOR PHYSICIANS
Although it has been a matter of debate regarding the exact guidelines to treat various thyroid disoders especially diseases which are in their subclinical states, a general line of treatment can be sought out if one knows the basic facts about thyroid disorders. Moreover one needs to be updated regarding the latest techniques and research going on. For a very long period of time subclinical hypothyroidism and subclinical hyperthyroidism were treated as full blown cases of hypo or hyper thyroidism. As the studies in these areas advanced, it was seen that one needs to clearly define the line and justification of treatment. Treatment only upon biochemical anomaly and in absence or minimal symptoms needs to be justified and scientfically reasoned. Also the term subclinical sometime seems arbitrary when there are symptoms but biochemically anomalies are minimal and vice versa. Thus a physician’s discretion at this point of time should be critical and justified.
As Hahnemann has rightly said that there are patients in disease and not the disease in patient. Therefore, a holistic approach is needed to treat the patients. A detailed case taking with psycosomatic approach should be adapted during the case taking. It should include investigation of emotional and psychological factors such as stress, repressed emotions, mental shock, grief, anger, dreams, delusions, and all other factors affecting the mind along with past, family history and intellectual and physical aspects of the patient. Hahnemann in aphorism 2nd has stated that, “The highest ideal of cure is rapid, gentle and permanent restoration of the health, or removal and annihilation of the disease in its whole extent.” Such a chosen remedy on the basis of individualization as stated in aphorism 7 works at deeper levels especially on pituitary-hypothalamic axis and sets right the basic imbalance of hormones in the body.
In cases of sub clinical & mild hypothyroidism and hyperthyroidism Homoeopathic treatment has been found to be very efficacious. Homoeopathic Medicines have their impact on Hypothalamus-Pituitary Axis. Homoeopathy can delay the progression of malfunctioning of the thyroid gland. As the thyroid and its hormones affect each and every organ of the body including mental and physical growth, early detection and treatment with Homoeopathy in children can lead to prevention of complications. As homoepathic medicines are selected on the basis of constitution of the patient, it plays an important role in immuno-modulation at the cellular level and therefore helps in annihilation of auto-antibodies. Theses are the observations that authors have drawn during the past years in OPD at INMAS, NHMC & SHMC.
WHEN TO CONSULT AN ENDOCRINOLOGIST
For Patients with:
- Graves’ disease
- Multinodular goiter
- Single palpable nodule
- Central disease (pituitary or hypothalamic)
- Patients resistant to therapy
STUDIES ON HOMOEOPATHY AND THYROID DISORDERS
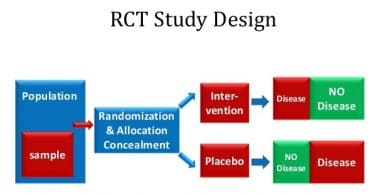
There are numerous examples of clinical and therapeutic studies done on thyroid disorders, examples of which are discussed in short in historical perspective elsewhere in this article. Following are some of the peer reviewed controlled design studies in Homoeopathy apart from clinical and therapeutic studies.
- Does a homeopathic ultramolecular dilution of Thyroidinum 30cH affect the rate of body weight reduction in fasting patients? A randomised placebo-controlled double-blind clinical trial. (Homeopathy, 2002; 91(4):197-206 (ISSN: 1475-4916) Schmidt JM; Ostermayr B, Krankenhaus für Naturheilweisen, Munich, Germany.9
- Homeopathically prepared dilution of Rana catesbeiana thyroid glands modifies its rate of metamorphosis. (Homeopathy, 2004; 93(3):132-7 (ISSN: 1475-4916) Guedes JR; Ferreira CM; Guimarães HM; Saldiva PH; Capelozzi VL
Laboratory of Molecular Pathology, University of São Paulo School of Medicine, SP, Brazil.10 - THYROIDINUM, A PROVING (HYGANTHROPHARMACOLOGY). J Am Inst Homeopath. 1964; 57:201-7 (ISSN: 0002-8967) PANOS M; ROGERS R; STEPHENSON J.11
- Pharmacologic and alternative therapies for the horse with chronic laminitis. Vet Clin North Am Equine Pract. 1999; 15(2):495-516, viii (ISSN: 0749-0739) Sumano López H; Hoyas Sepúlveda ML; Brumbaugh GW.
Departamento de FisiologÃa y Farmacologiá, Facultad de Medicina Veterinaria y Zootecnia, Universidad Nacional Autónoma de México, México DF, México.12 - To evaluate the efficacy of homoeopathic treatment in sub clinical hypothyroidism (SCH). A single blind case control 18 months follow-up pilot study at NHMC & Hospital and Institute of Nuclear Medicine & Allied Sciences, Delhi, India under Dilli Homoeopathic Anusandhan Parishad (DHAP) revealved remarkable results about management of children on subclinical hypothyroidism.13
In continuation of this scientific spirit another research study on, “Effect of Homoeopathic treatment on natural history of autoimmune thyroiditis” is undergoing at Dr. B. R. Sur Homoeopathic Medical College, Hospital & Research Centre, Nanak Pura, Moti Bagh, New Delhi (Govt of NCT of Delhi) in collaboration with Institute of Nuclear Medicine & Allied Sciences (INMAS), Timarpur, Delhi – 54 (under ministry of Defence). The project is under EMR scheme of AYUSH.
ACKNOWLEDGEMENT
The authors express their thankfulness to Maj. Gen. Dr. R. K. Marwaha, Addl. Director, Institute of Nuclear Medicine, Timarpur, Delhi, Dr. V. K. Khanna, Ex-Principal, NHMC & H, Defence colony, New Delhi and Dr. V. K. Chauhan, Principal SHMC & H, Nanak Pura, Moti Bagh, New Delhi for their timely support, help and guidance. The authors are also thankful to the staff of INMAS-Mr. Kuntal Bhadra, Mr. Baig, and Mr. Satwir Singh for their assistance in various activities at screening, investigations and OPD setups.
REFERENCES
- V. Leoutsakos, A short history of the thyroid gland, Dept of Surgery Athens University School of Medicine, Athens, 115 27 Greece.
- Encyclopedia Homeopathica, Version 2.2.2
- RADAR 10, Apex Version.
- Thyroid gland development and defects, Kratzsch J, Pulzer F., Institute of Laboratory Medicine, Clinical Chemistry and Molecular Diagnostics, University Hospital, Paul-List-Str. 13-15, D-04103 Leipzig, Germany.
- Grant’s Atlas of Anatomy, Twelfth edition, Anne M. R. Agur
- Guyton & Hall Textbook Of Medical Physiology 11th_Edition
- Harrisons textbook of medicine, 17th edition.
- Organon of Medicine, Samuel Hahnemann, 5th edition, Publisher B. Jain.
10. http://www.ncbi.nlm.nih.gov/pubmed/15287432
11. http://www.ncbi.nlm.nih.gov/pubmed/14178448
13.




SIR
EXCELLEMT ARTICLE.
VERY INFORMATIVE AND EDUCARIVE.
MY DAUGHTER IS SUFFERING FROM HYPOTHYROIDISM SINCE 8 MONTHS.
Dr. Marchanda and other co-writers of the article on thyroid deserve appreciation for filling the knowledge of sea in a vessel. This is called practical approach that is useful for readers with special reference to students and practitioners. My congratulations.
Dr. Shiv Dua,
Author of book,’Manage and cure thyroid’.
Thanks to Dr Shiv Dua for your encouraging words.
Thyroid Clinic, SHMC & H.
As a nurse I find the information the most through, and along with the photos/graphics easier to understand for all concerned. I like how it includes prevention and a holistic approach. Homeopathy is much needed for women whose subclinical symptoms are ignores until illness or life-threatening thyroid conditions occur. This is because even tho it is women who predominately have thyroid disorders, are rudely dismissed by doctors as only hysterical, do not return for follow-up appointments.
It is a highly exhaustive article on the subject, covering all aspects of thyroid including its anatomy, functions, diagnosis of disorders, natural history, homeopathic approach et al. I particularly liked the candid admission made by the authors. They caution that while attempting to undertake the treatment we must ascertain the level of disease, as to what amount of damage has already been done. Once the destruction has set in, no medicine can revive the dead cells even well selected homeopathic remedies cannot undo the irreversible damage already done, however the remedies may stop the further damage and can save the rest of the gland. If we clearly perceive this concept, they say, we can avoid putting up false claims of cure. Homeopathy cannot go against the laws of nature. I must congratulate authors for compiling the most comprehensive article on the subject. It is an ‘all-in-one’ article worth saving on hard disc for future reference and consultation.
Dr. Kuldip Singh (Mohali)
1. AN EXCELLENT ARTICLE.
2. ADDING A BRIEF RESUME/REPERTORY FOR HOMEO MANAGEMENT OF THYROID DISORDERS MIGHT HAVE MADE THE ATICLE PERFECT ONE.
3. MOST OF THE THYROID DISORDERS OCCUR DUE TO PSYCHOLOGICAL REASONS, THEREFORE MORE EMPHASIS SHOULD BE PLACED ON THESE FACTORS WHILE REMEDY SELECTION.
4. PSYCHOTHERAPY IN SUCH CASES IS ALSO REQUIRED FOR CORRECTION OF THEIR BEHAVIOR DISORDERS, OTHERWISE THE PATIENT WILL KEEP ON HAVING REMISSIONS AND RELAPSES.
THENKS
On a homeopathy website, I was looking for homeopathic treatment and guidelines rather than exhaustive allopathic background that can be found easily on many other places on the net. The article would have been more useful to homeopaths if it can be revised providing concise allopathic/basic info about the illness with detail discussion and remedies to treat the illness homeopathically.
Very informative information, i never seen such a wonderfull information pls keep writting in future too
The most exhaustive, informative and wonderful article.
Thanks to HPathy. I found this article very informative, being a non-homeo background, I got so much information. I am a patient of Goitre since last 8 years, Now I am 18 year old female. My T3 and T4 is always with in the normal limit but TSH always fluctuate, Can u sugges me any thing ? I will be thankful to you.
Common symptoms of hypothyroidism are:
Fatigue or lack of energy
Weight gain
Feeling cold
Dry skin and hair
Heavy menstrual periods
Constipation
Slowed thinking
DIAGNOSIS of hypothyroidism is usually straightforward, once it is suspected.
Patients with hypothyroidism due to Hashimoto’s thyroiditis have an elevated level of serum TSH (thyroid stimulating hormone).
However, the rare patient with hypothyroidism due to a pituitary or hypothalamic condition may have a normal or low serum TSH.
In my experience for hypo/hyper thyroidism;
-thyroidinum 200 every week then after 1 month one dose of 1M
-Spongia 30(3 times a day)
-Fucus Q 4 times a day
– Iodium 30 (3 times a day)
These remedies gave excellent results, even specialist was surprised to see reports
regards
Left side goiter softy feel some time or hard feel t3 t4 & tsh report normal please advised me medicine in homeophathy
I am 44 year old, self employed. Always stressful business wise. I got thyroid nodule in right lower lobe, which is around one inch in shape. My TSH, T3, T4 are normal. There are multiple cystic small nodules in left lobe as well.
Can any one recommend any Homeopathic Remedy. Thanks
thyroid symptoms will be reflected in head classical homeopath consult book by ge dienst what to do for the head.hypo kalayan banerjea article advanced homeopathy best guidance.hyper arsenic iod lycopus spongia valuable.
Exhaustive studies, mostly copy paste type. Useless. Everything is found in any book of medicine ,viz: Davidson, Harrison etc.
No perfect light in the homoeopathic way of treatment of the disease.